Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Scott Barker and Dr Amanda Oakley, Hamilton, New Zealand, 2005. Reviewed and updated by Dr Amanda Oakley; Vanessa Ngan, Staff Writer; and Clare Morrison, Copy Editor; April 2014.
Eosinophilic pustular folliculitis is a recurrent skin disorder of unknown cause. It is also known as eosinophilic folliculitis and Ofuji disease. Skin biopsies of this disorder find eosinophils around hair follicles — hence its name.
There are several variants of eosinophilic pustular folliculitis. All of them present with itchy papules or pustules. Eosinophilic pustular folliculitis is rare and more often affects males than females. Variants include:
Eosinophilic pustular folliculitis presents with itchy red or skin-coloured dome-shaped papules and pustules. It may look like acne or other forms of folliculitis. The papules mostly appear on the face, scalp, neck and trunk and may persist for weeks or months. Less commonly, urticarial lesions are seen (these are larger red irritable weal-like patches similar to urticaria). Palms and soles may rarely develop similar papules and pustules, but in such cases, the condition should not be called folliculitis, as there are no follicles in these areas.
Longstanding cases may develop dermatitis or a form of prurigo, presumably because of the itching and scratching.
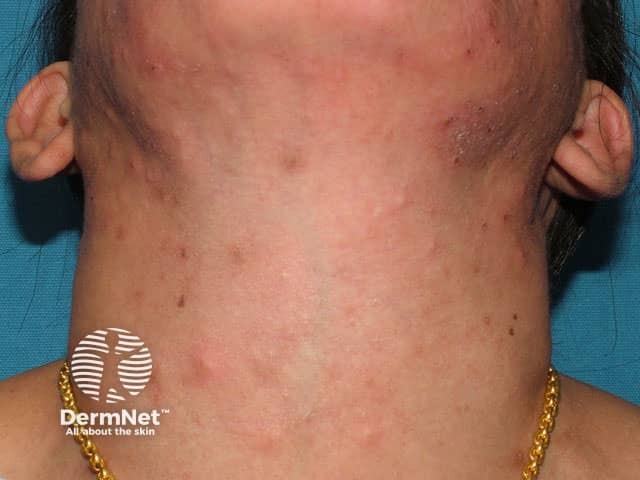
Eosinophilic folliculitis
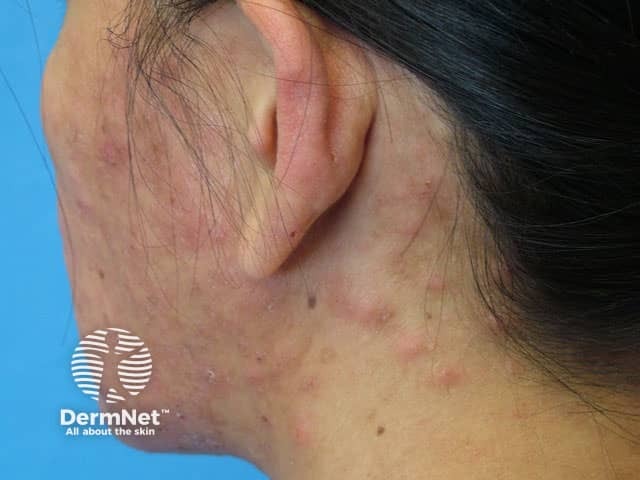
Eosinophilic folliculitis
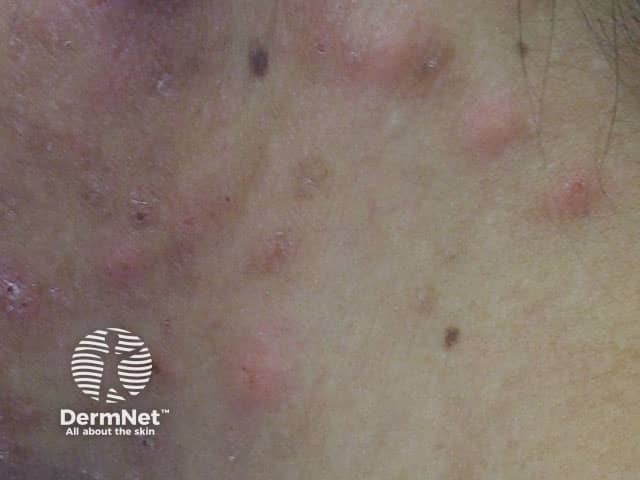
Eosinophilic folliculitis
See more images of eosinophilic pustular folliculitis
Skin biopsy reveals eosinophils under the skin surface and around the hair follicles and sebaceous glands (see eosinophilic folliculitis pathology). In many cases, blood tests show a mild rise in eosinophil cells and immunoglobulin-E (IgE), and reduced IgG and IgA levels.
Eosinophilic pustular folliculitis is often a feature of immunodeficiency. Eosinophilic pustular folliculitis associated with HIV infection presents when levels of CD4 lymphocyte cells drop below 300 cells/mm3, a level at which there is an increased risk of a secondary opportunistic infection. Cases of eosinophilic pustular folliculitis have also reported after bone marrow transplantation before the immune system is back to normal functioning, and in some individuals with inherited immune deficiencies.
The cause of eosinophilic pustular folliculitis of HIV is not known. Immunodeficiency appears to lead to increased risk of allergic-type skin diseases. There is no proof that bacterial, fungal or viral secondary infection is the cause, although some researchers have postulated overgrowth of Malassezia or Demodex (the hair follicle mite) might be involved. Another theory is that there is a change in the immune system causing eosinophils to attack the sebum produced by sebaceous gland cells.
In patients with HIV, eosinophilic pustular folliculitis is likely to improve or resolve with HAART (Highly Active Anti-Retroviral Treatment), as CD4 cell counts rise above 250/mm3.
Other treatments that may be effective include: