Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Introduction Causes Symptoms Clinical features Diagnosis Treatment
Balamuthia mandrillaris (B. mandrillaris) is an amoeba that lives in water and soil. B. mandrillaris was first discovered in 1990 and has been associated with more than 100 cases of disease since then. Infection with B. mandrillaris has been reported in South, Central, and North America, Asia, Australia, and Europe but remains a rare cause of amoebiasis.
B. mandrillaris can enter humans through the nasal mucosa, lungs, or breaks in the skin. As in cases of other free-living amoebae (eg, Naegleria and Acanthamoeba), a history of swimming in freshwater lakes, ponds, and heated swimming pools is common.
Weeks to years later (5–8 months on average) the infection spreads to the central nervous system causing amoebic encephalitis (inflammation of the brain).
Features of B. mandrillaris encephalitis include:
In 95% of patients, B. mandrillaris encephalitis is fatal.
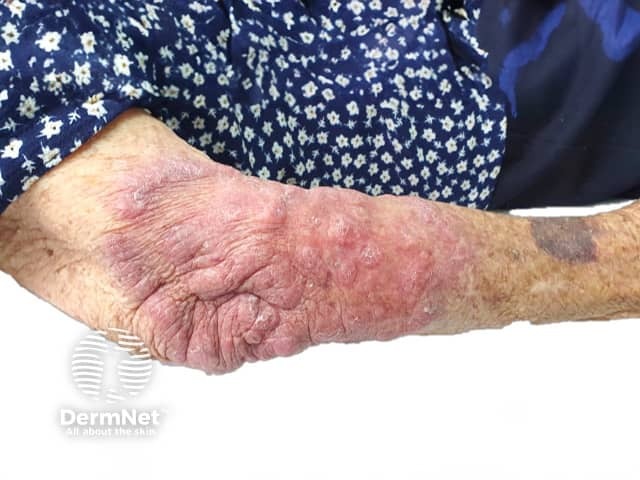
Following penetration through the skin, B. mandrillaris causes a skin lesion before the infection spreads to the central nervous system. The classical skin lesion is an asymptomatic granulomatous plaque (a nodule made of inflammatory cells), usually located on the central face. The plaque is often described as rubbery in consistency. Single or multiple lesions may be present,
The lesion may enlarge (to involve the entire face in some cases), and occasionally smaller satellite lesions appear. Ulceration occurs at a late stage. Occasionally the lesion may occur on the extremities.
As B. mandrillaris infection is very rare, diagnosis is often delayed. Diagnosis is made by finding the amoeba in the skin or other tissue. Biopsy shows a granulomatous infiltrate within dermis and subcutaneous tissues. Trophozoites and cysts are rarely seen.
B. mandrillaris is difficult to culture in the laboratory on normal culture media. The organism can be grown in specific mammalian cell culture lines or by inoculation of mice if there is clinical suspicion of Balamuthia infection. A polymerase chain reaction (PCR) test has been developed for research purposes but is available in some community laboratories.
Early treatment with a range of oral antifungal, anthelmintic, and antiprotozoal drugs (often in combination) may improve survival.