Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Last Reviewed: January, 2024
Author(s): Dr Sarah Seol, Waikato Hospital, New Zealand (2024)
Previous contributors: Vanessa Ngan, Staff Writer (2003)
Reviewing dermatologist: Dr Ian Coulson
Edited by the DermNet content department
Introduction
Demographics and risk factors
Causes
Clinical features
Variation in skin types
Complications
Diagnosis
Differential diagnosis
Treatment
Outcome
Cat scratch disease (CSD) is a bacterial infection that affects the lymph nodes. It is also known as cat scratch fever or subacute regional lymphadenitis.
Risk factors for acquiring cat scratch disease (CSD) include:
CSD can occur in people of all ages but is most common in children and adolescents. The majority (80%) of patients with cat scratch disease are less than 21 years old.
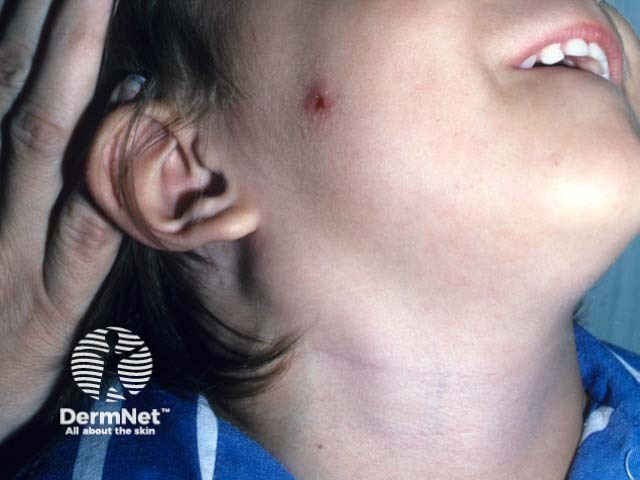
A primary lesion of cat scratch disease on the cheek - note the infra-auricular lymphadenopathy (CSD-patient2)
Click here for more images of cat scratch disease
Patients with CSD have usually suffered a scratch or bite from a cat or kitten which is infected with the bacteria Bartonella henselae, a common infection in young cats. It is also known as Rochalimaea henselae.
The bacteria is passed from cat to cat via fleas. In the absence of fleas, an infected cat cannot pass the infection to uninfected cats.
Once infected, the bacteria are present in saliva deposited in the cat’s fur and claws.
A small red raised spot develops at the site of contact with an infected cat’s saliva after 3–10 days. This changes into a fluid-filled blister that later forms a crusty sore. It is often mistaken for an insect bite. Most are found on the hands, arms, face, or neck as people often hold kittens close to their chest and face. The sore usually heals without scarring in several days or months.
The nearest lymph nodes become swollen and tender, most often those in the head, neck, and armpit. This is known as regional lymphadenopathy. The lymph nodes may swell to 10–12 cm in the first two weeks of the disease. On questioning, patients often recall being licked, bitten, or scratched by a cat in the previous 1–8 weeks.
About 50% of patients will experience additional signs and symptoms including:
Erythema of the initial spot may not be apparent in darker skin types. Instead, it could appear darker than the surrounding skin or violaceous/purple.
Less common problems occur in about 10% of patients. These may include:
Encephalopathy is an uncommon complication of CSD that occurs one to six weeks after the lymph glands swell up. The abrupt symptoms of fever, seizures, and coma can be frightening. With hospitalisation and high doses of antibiotics, most patients recover completely.
Immunocompromised patients (such as solid organ transplant recipients or people with HIV) can present with atypical manifestations such as thrombocytopaenic purpura, haemophagocytosis, and visceral disease resembling lymphoproliferative disorders.
There is no single established ‘gold standard’ test to diagnose cat scratch disease.
Previously, diagnosis was often based on the presence of three of the four following criteria:
Diagnostic testing is not routinely performed if characteristic clinical signs are present, although may be indicated in those with atypical signs, unresolving systemic symptoms, or diagnostic uncertainty:
See also: Laboratory tests for bacterial infections.
Pain and fever can be managed by increasing fluid intake and simple analgesics. Warm moist compresses to affected lymph glands may decrease swelling and tenderness.
Treatment of uncomplicated cat scratch disease remains controversial. As CSD is a benign and self-limiting condition, with most cases of regional lymphadenopathy resolving spontaneously in 2–4 months, no specific treatment is usually necessary.
However, some studies suggest that certain antibiotics including azithromycin, doxycycline, gentamicin, rifampicin, trimethoprim + sulfamethoxazole, or ciprofloxacin may significantly shorten the duration of lymphadenopathy. Antibiotics are warranted in patients with severe or persistent symptoms, disseminated disease, or immunodeficiency.
In rare cases, large pus-filled lymph nodes may persist for one to three years. The pus may need to be repeatedly drained using a needle.
Cat scratch disease spontaneously resolves in approximately 90–95% of children, and is managed symptomatically with pain relief, antipyretics, and warm compresses. In disseminated infection, the recovery process might take several months to a year, and the extent of complications varies depending on which organ systems are affected. CSD can be debilitating in immunocompromised patients.
Click here for images of cat scratch disease