Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author(s): Nataki Duncan MPH, MHS, Meharry Medical College, USA; Dr Libby Whittaker, DermNet Staff Writer, New Zealand (2023)
Previous contributors: Dr Amanda Oakley, Dermatologist (2002)
Reviewing dermatologist: Dr Ian Coulson
Edited by the DermNet content department
Introduction
Demographics
Causes
Clinical features
Variation in skin types
Complications
Diagnosis
Differential diagnoses
Prevention
Treatment
Outcome
E-lecture
Skin infections can be caused by bacteria (often Staphylococcal or Streptococcal) either invading normal skin, or affecting a compromised skin barrier (eg, skin affected by atopic dermatitis, or surgical wound sites).
The skin is our first line of protection against the environment. A local or systemic response is activated when this protective barrier is invaded. Microorganisms that invade the skin can be part of the external environment or the normal skin microbiome.

Honey-coloured crusts on the chin in impetigo

A swollen tender hot left leg due to Streptococcal cellulitis
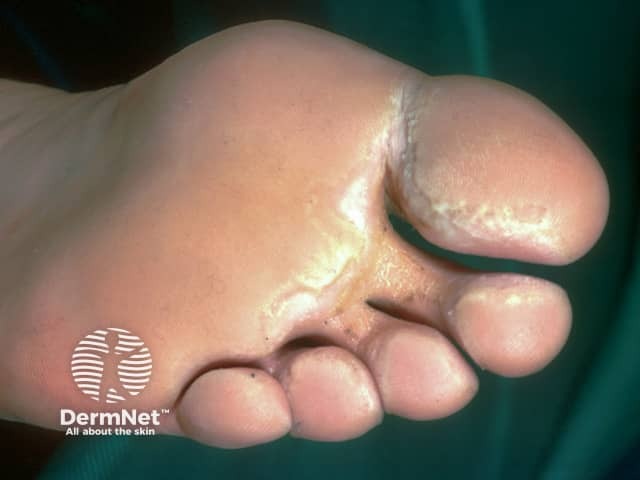
Interdigital and toe pitted keratolysis

Ecthyma gangrenosum due to Pseudomonas septicaemia

Palmar erythematous macules suggestive of secondary syphilis

Sporotrichoid spreading Mycobacterium marinum infection
More images of Staphylococcal skin infections
Bacterial skin infections are a common reason for emergency visits. Children under five years and adults over 65 years old are affected more often than other age groups. In 2005, the World Health Organisation (WHO) reported a high prevalence of skin disease in children from developing countries in sub-Saharan Africa.
Gender may also play a role; in one North American study, men comprised 60-70% of all cases of cellulitis.
Certain comorbid conditions increase susceptibility to bacterial skin infections, such as diabetes, vascular insufficiency, and being immunocompromised (eg, chemotherapy patients with neutropaenia). Some people, such as those who inject drugs, are at increased risk. Among hospitalised patients, skin infections are prevalent and often complicate the hospital course.
A variety of bacteria can cause skin infections, most commonly Staphylococcus and Streptococcus species.
Bacteria |
Mucocutaneous infections (or infections with skin signs) |
|---|---|
Staphylococcus aureus (common) |
|
Streptococcus pyogenes (common) |
|
Corynebacterium species |
|
Neisseria species |
|
Erysipelothrix insidiosa |
|
Haemophilus species |
|
Helicobacter pylori |
A cause of stomach infection; may be associated with: |
Klebsiella rhinoscleromatis |
|
Mycoplasma pneumoniae |
A cause of pneumonia; may be associated with:
|
Pseudomonas aeruginosa |
|
Calymmatobacterium granulomatis |
|
Bacillus anthracis |
|
Clostridium perfringens |
|
Listeria monocytogenes |
|
Treponema species |
|
Bartonella species |
|
Mycobacterium species |
|
Leptospira |
|
Nocardia |
|
Yersinia pestis |
|
Serratia marcescens (a facultative anaerobic gram-negative bacillus) |
|
Fusobacterium species (eg, Bacillus fusiformis, Treponema vincenti) |
|
Burkholderia species |
|
Actinomyces species |
|
Vibrio vulnificus |
|
Brucella species |
|
Salmonella species (eg, Salmonella typhi) |
|
Aeromonas species (found in water) |
|
Tick-borne bacterial infections |
|
Other conditions sometimes caused by or associated with bacterial infection include:
Bacterial skin infections can result in diverse clinical presentations. Generally, they will present with erythema, pain, warmth, swelling, and, depending on severity, dysfunction. Purulent discharge and lymphadenopathy may also be evident on examination.
In severe infections, the following signs may be present:
Erythema may be less evident in darker skin tones, and postinflammatory hyperpigmentation is more common.
Bacterial skin infection is commonly diagnosed clinically, although laboratory studies may be useful, such as:
Minor bacterial infections often resolve without treatment. Due to increasing antibiotic resistance, first-line use of topical antibiotics, such as fusidic acid, is generally discouraged; topical antiseptics are often used as an alternative for minor infections. More serious or persistent bacterial infections are treated with oral, intravenous, or sometimes intramuscular antibiotics.
It is best to take samples (eg, swabs or blood cultures) to test which organism is responsible for an infection before commencing antibiotics. If the infection is serious (eg, suspected meningococcal disease), do not delay treatment with a broad-spectrum antibiotic. As culture and sensitivities become available, change to an appropriate narrow-spectrum antibiotic.
Antibiotics should not be prescribed if they are not indicated or unlikely to be of benefit, for example, if the infection is viral in origin. Adverse reactions include cutaneous effects and gastrointestinal side effects. Antibiotic stewardship is also an important consideration.
Many bacterial skin infections resolve without treatment or without serious morbidity. However, skin infections can be severe and cause a significant burden of disease worldwide, sometimes resulting in sepsis and death, particularly in vulnerable patient groups such as the elderly, hospitalised, and immunocompromised.
Antibiotic resistance has increasing implications for the treatability and outcome of many bacterial skin infections moving forwards.