Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Marie Hartley, Staff Writer, 2010. Latest update by Dr Jannet Gomez, Postgraduate Student in Clinical Dermatology, Queen Mary University London, United Kingdom, July 2016.
Introduction Demographics Clinical features Complications Diagnosis Treatment Prevention
Acute rheumatic fever (ARF) is caused by a reaction to a bacterial infection with particular strains of group A streptococcus. It has long been thought that ARF only follows streptococcal pharyngitis (sore throat), however recent studies from Aboriginal populations in Australia have suggested streptococcal skin infection may precede some cases of ARF. Those who have experienced one episode of ARF are more likely to suffer recurrent attacks with subsequent group A streptococcal infections.
The skin sign of acute rheumatic fever is erythema marginatum.
ARF usually affects children aged 5–15 years. Most cases of ARF currently occur in developing countries. Worldwide there is an estimated 470 000 new cases of ARF annually (60% of whom eventually develop rheumatic heart disease). In most developed countries ARF is now rare, with a few notable exceptions; the highest documented rates of ARF in the world are in Maori and Pacific people in New Zealand, Aboriginal Australians, and those in Pacific Island nations.
Rheumatic fever is associated with poverty, overcrowding and poor sanitation facilities. It is suspected that there are genes that make some families more susceptible to the disease.
Symptoms of ARF generally develop several weeks after an episode of streptococcal pharyngitis. However, many patients do not recall having a sore throat. Non-specific symptoms include:
ARF causes a variety of more specific clinical features:
Skin signs in ARF may include:
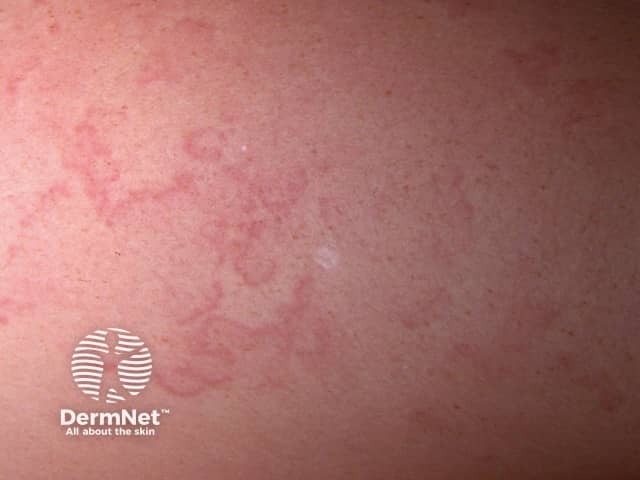
Erythema marginatum
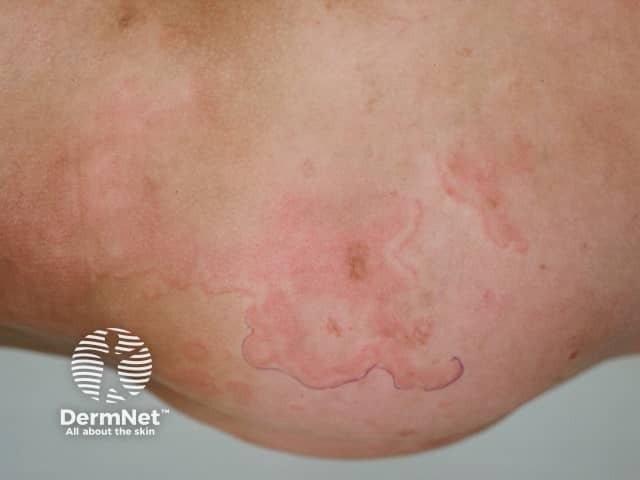
Erythema marginatum
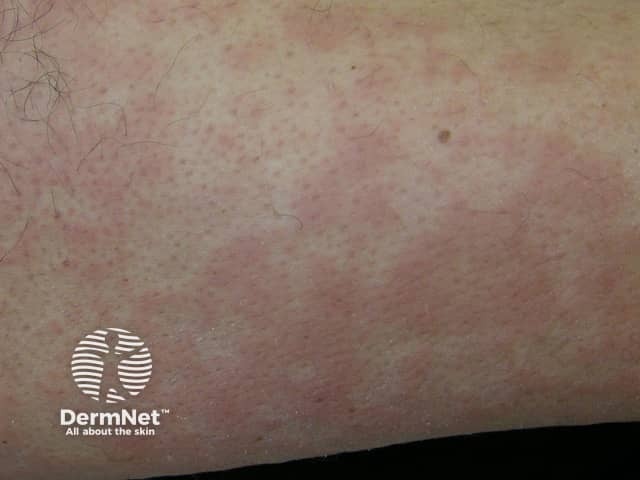
Erythema marginatum
The most severe complication of recurrent ARF is permanent damage to heart valves, known as rheumatic heart disease. The disease can result in permanent damage to:
The diagnosis of ARF is challenging, as there are no clinical features or diagnostic tests available to confirm or rule out this condition. Instead, the diagnosis is made using the Jones criteria. These criteria require evidence of a preceding group A streptococcus infection, and various combinations of the characteristic features above and other non-specific clinical features. A detailed explanation of these criteria (and modifications for the New Zealand environment) can be found on the National Heart Foundation of New Zealand website.
Tests to confirm evidence of a group A streptococcal infection include:
Other tests used in the assessment of a patient with suspected ARF include:
Following a diagnosis of rheumatic fever, it is standard practice to treat the group A streptococcal infection that led to the disease with oral penicillin (although this practice has not been proven to alter long-term outcomes).
Following the initial attack, patients are treated with continuous penicillin to prevent further streptococcal colonisation or infection and additional damage to the heart. Continuous penicillin is also recommended for people with established rheumatic heart disease. Continuous penicillin is generally given by injection every four weeks for a minimum of 10 years. Some patients, such as those with severe carditis, may require lifelong treatment.
Aspirin or naproxen are added to reduce inflammation, fever and pain. In extreme cases, a corticosteroid such as prednisone may be added.
Patients with rheumatic heart disease may occasionally require heart surgery to repair or replace damaged heart valves.
ARF can be prevented with timely treatment of group A streptococcal pharyngitis, particularly in people aged 5-15 years. People with sore throat and fever should see the doctor for advice. Vaccines are currently in development and are eagerly awaited.
Medscape Reference: