Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Created 2008.
Atopic dermatitis affects up to 20% of the childhood population and causes considerable distress and ill health. Its prevalence is greatest in childhood, generally starting in the first few months of life, becoming more severe in infancy and often improving in school years.
Diagnosis depends on clinical findings, which vary with the age and stage of the disease. The main features are:
A scoring index (SCORAD) combining extent, severity and subjective symptoms, is often used in clinical trials that assess the effectiveness of treatments.
Affected sites vary with age. Infantile eczema commonly affects the face, sparing around the mouth and later the hands, feet and elsewhere.
Atopic dermatitis Atopic dermatitis Atopic dermatitis 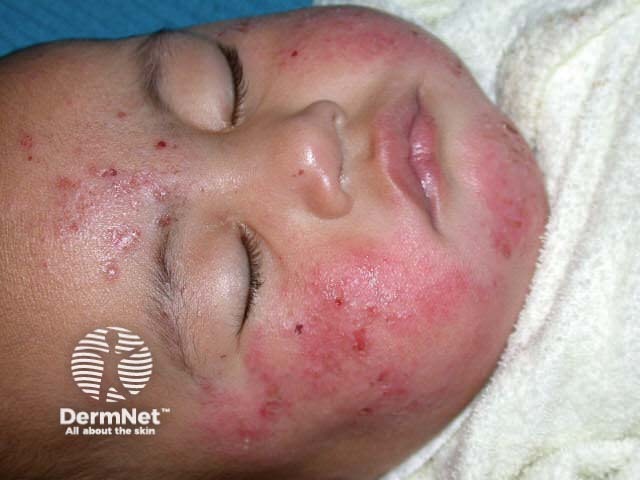
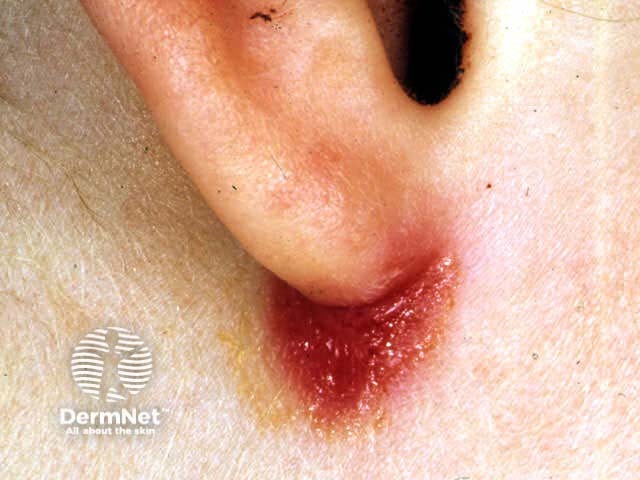
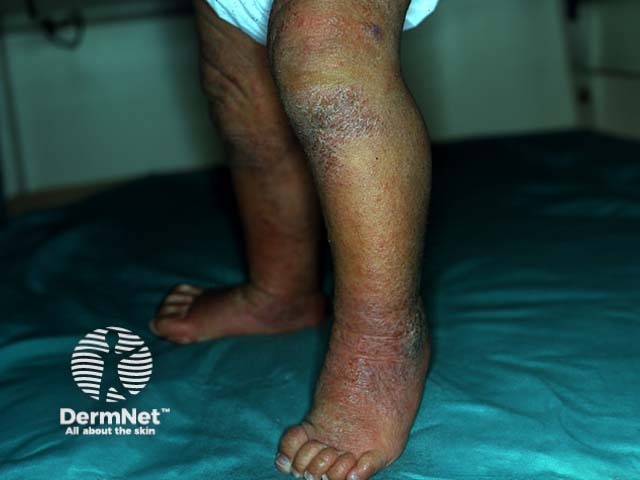
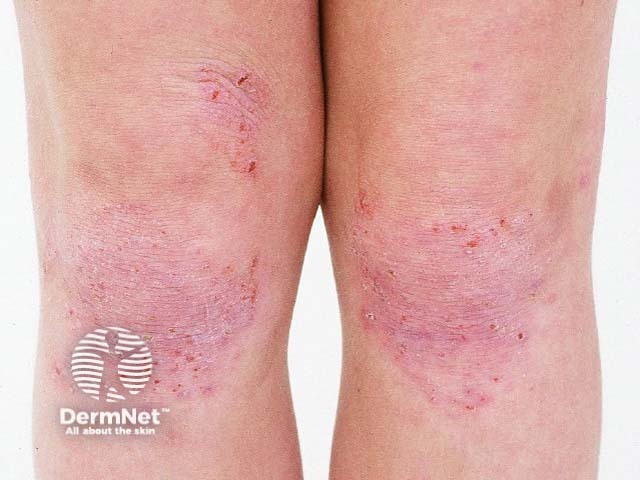
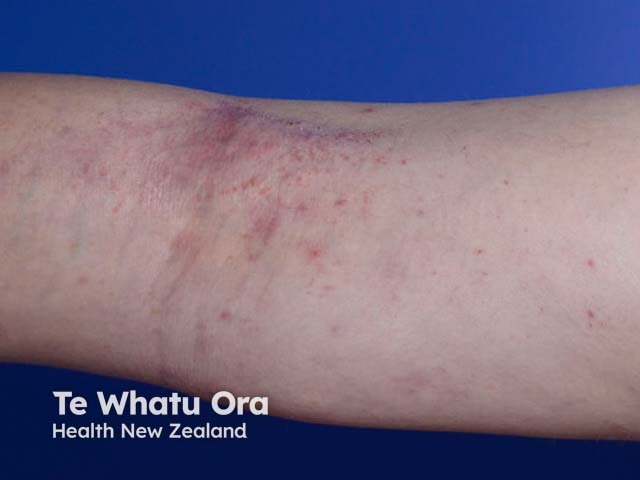
In older children, eczema tends to affect flexures, particularly antecubital and popliteal fossae.
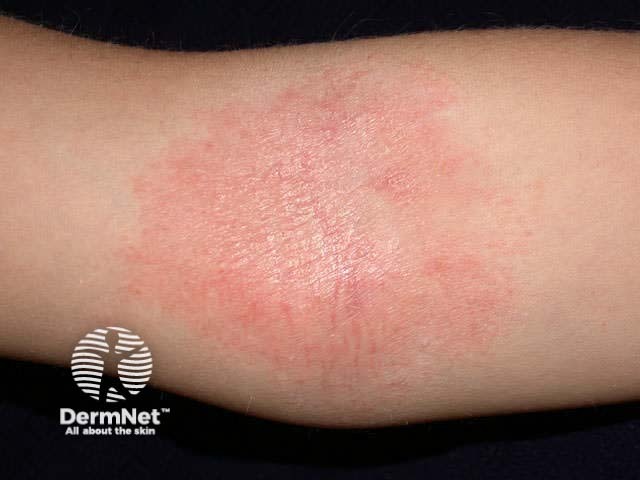
Atopic dermatitis
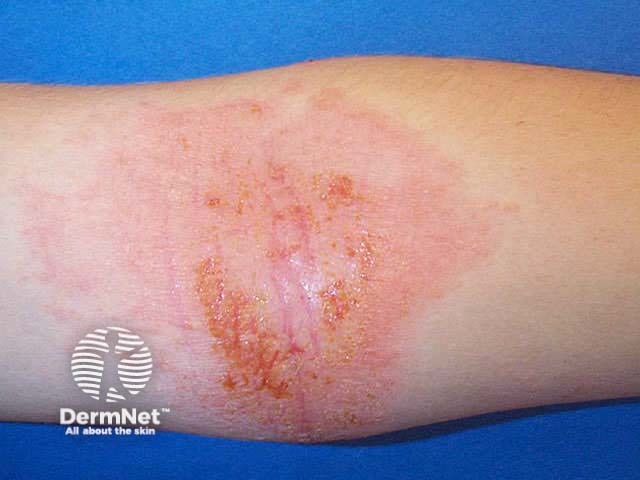
Atopic dermatitis
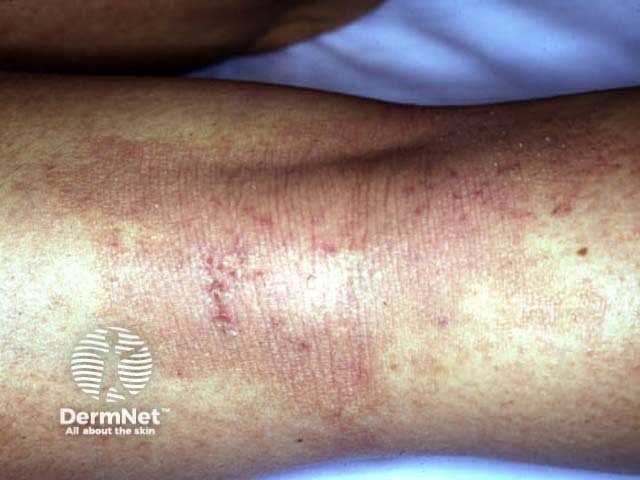
Atopic dermatitis
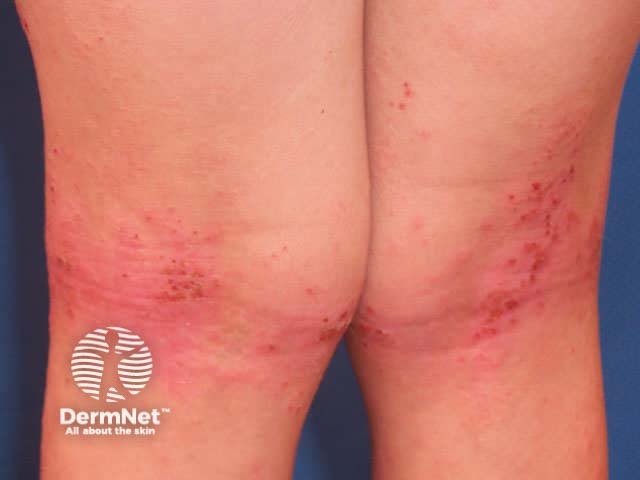
Atopic dermatitis
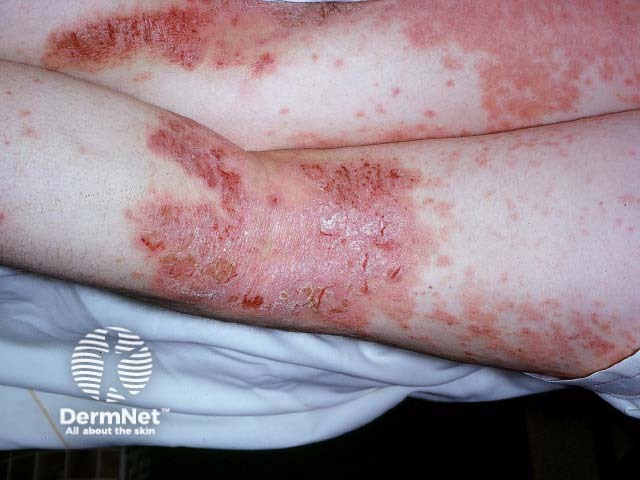
Atopic dermatitis
Atopic dermatitis
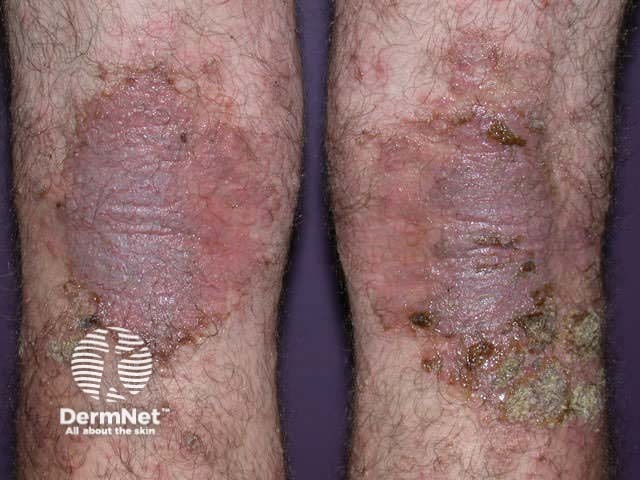
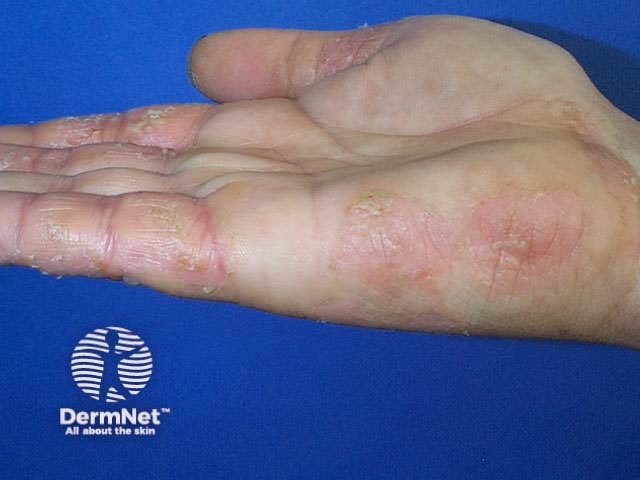
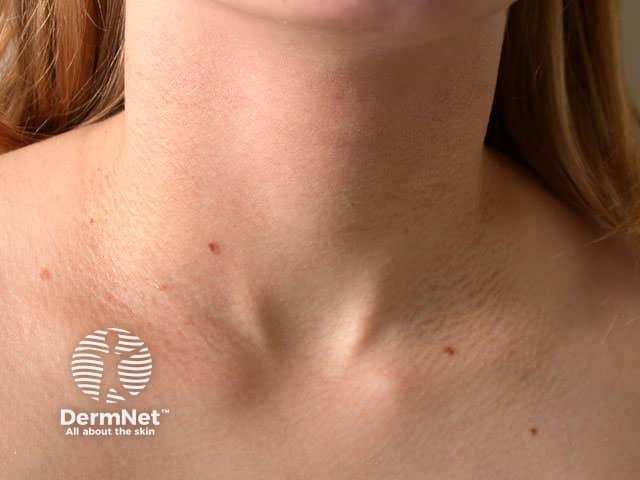
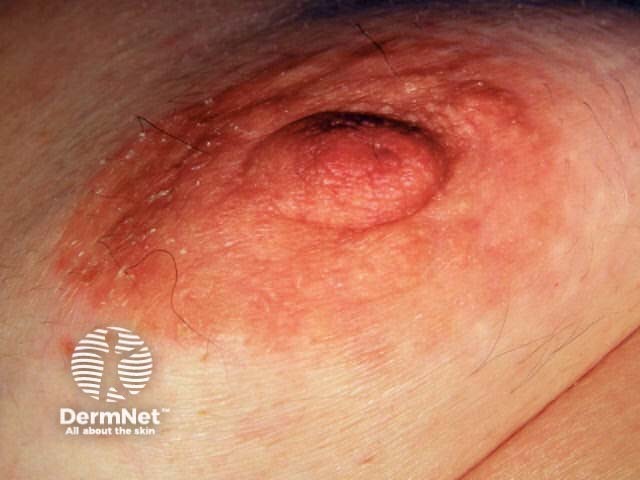
Flexural dermatitis often persists into adult life. Occasionally, a ‘dirty neck’ is observed in teenagers. Irritant hand eczema may be a problem for those who do wet work. Bilateral nipple eczema is not uncommon.
Atopic dermatitis
Atopic dermatitis
Atopic dermatitis
Atopic dermatitis
Atopic dermatitis
Atopic dermatitis
Erythrodermic eczema refers to involvement of the entire body at any age.
Flare-ups may be precipitated by:
Atopic eczema may be complicated by microbial colonisation or infection:
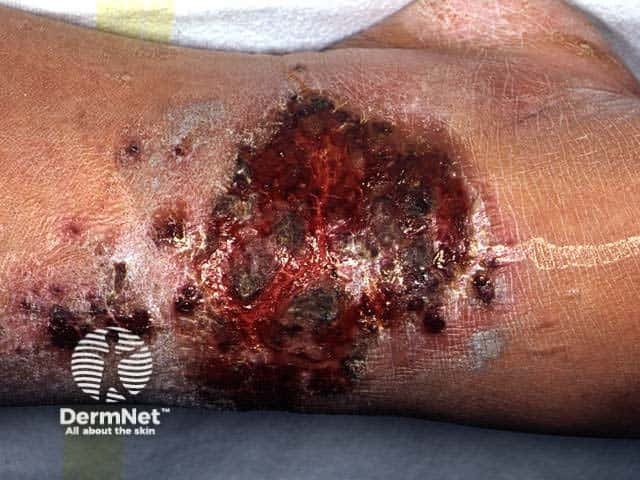
Impetiginised eczema
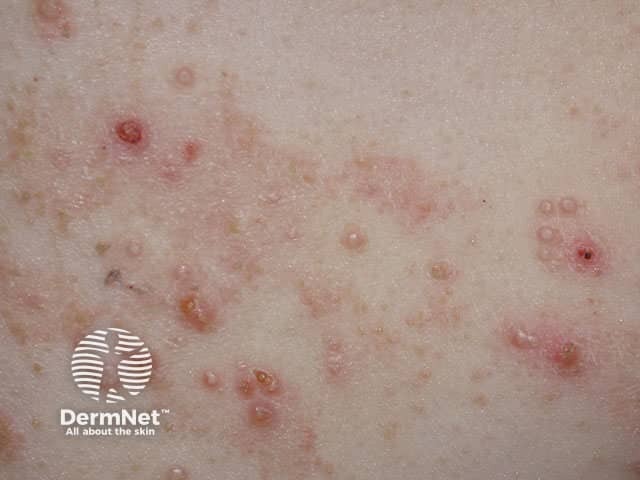
Molluscum contagiosum
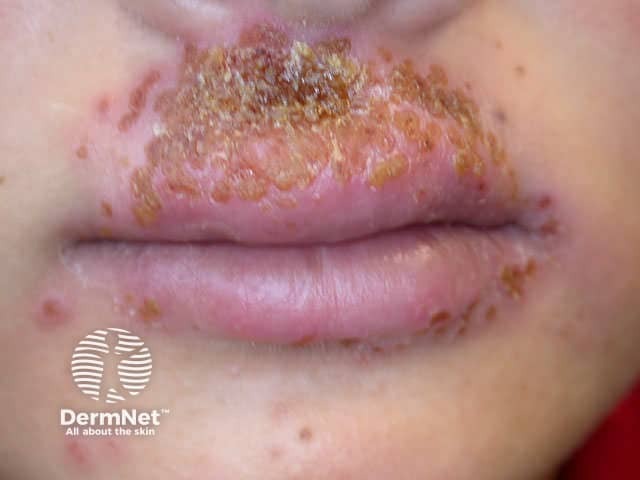
Eczema herpeticum
The pathogenesis appears involve release of vasoactive substances from mast cells and basophils as an IgE-mediated hypersensitivity reaction. There is a TH2 pattern of cytokine release from T helper lymphocytes in the epidermis and dermis with low levels of TH1 lymphocytes and gamma interferon. There is also a non-allergic or intrinsic type of atopic dermatitis. These patients have no associated respiratory diseases, show normal total serum IgE levels, no specific IgE, and have negative skin-prick tests to aeroallergens or foods.
It is not known why the incidence of atopic dermatitis appears to be increasing; theories include increased hygiene and decreased exposure to micro-organisms and greater exposure to house dust mite.
A proportion of patients have been found to be deficient in fillagrin, resulting in abnormal barrier function of the stratum corneum and increased susceptibility to the effect of contact irritants. These individuals have dry skin (ichthyosis vulgaris).
In most cases, no specific investigations are required. However, on occasion the following may be useful:
The best way to manage atopic dermatitis is unknown. At present, management of atopic eczema in patients of all ages involves:

Phototherapy
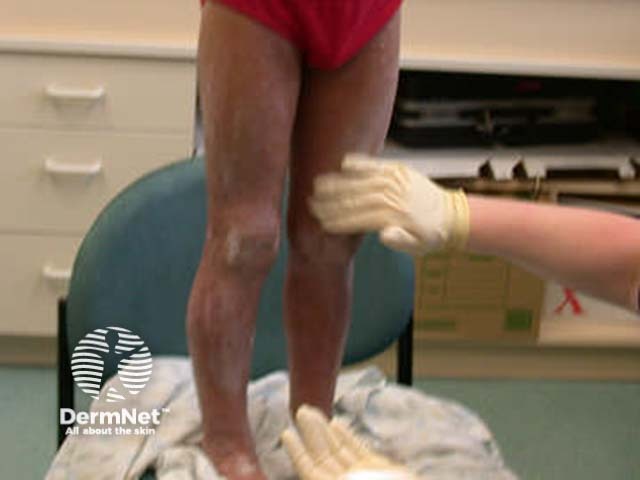
Applying cream
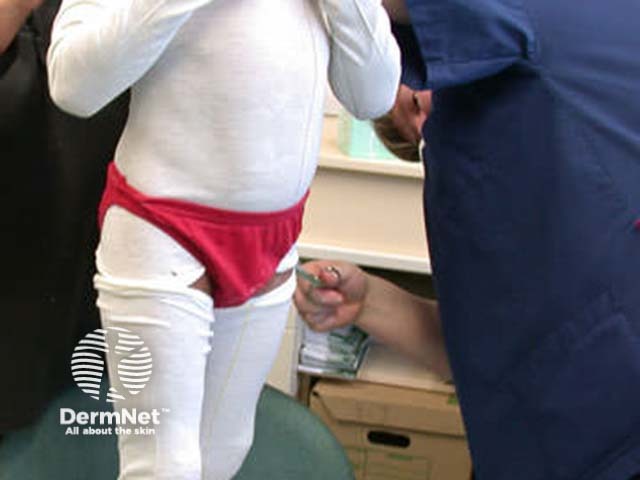
Tube gauze wet dressings

Shoulder detail
Potent topical steroids should be used with caution in infants because of their greater proportional absorption due to higher surface area to body weight ratio. Blistered or weeping eczema is brought under control most rapidly using wet dressings.
Oral corticosteroids are used for crisis intervention but may be followed by a severe rebound flare at discontinuation. It is important to taper the dose and begin intensified skin care with topical steroids and bathing followed by application of emollients.
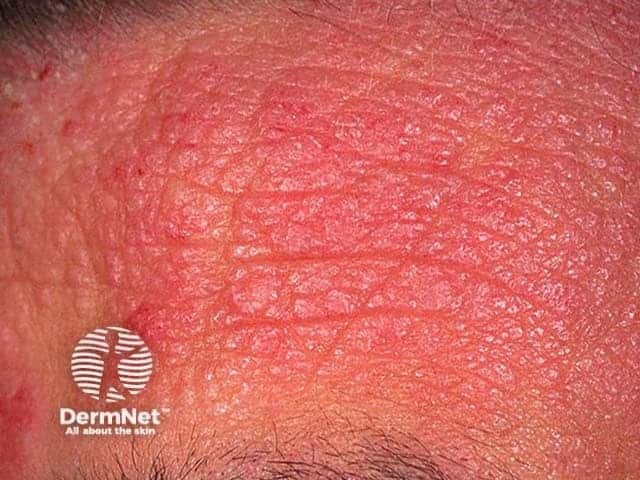
Facial eczema
Use light emollients in adolescents and adults to avoid provoking acne or perioral dermatitis. It is safe to use 0.5-2% hydrocortisone cream on active eczema indefinitely, although in time it is likely to lose its efficacy. Pimecrolimus cream can also be used as maintenance treatment. Severe eczema may require moderate potency topical steroids for a course of 5 to 10 days or as pulse therapy. A trial of antifungal agents may be warranted in adults with prominent facial eczema.
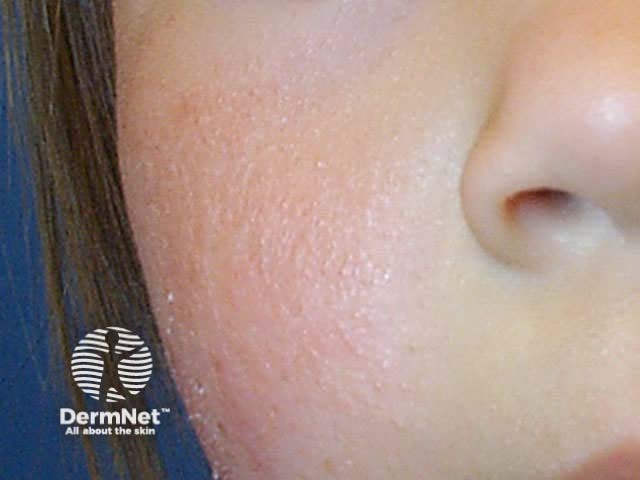
Atopic dermatitis
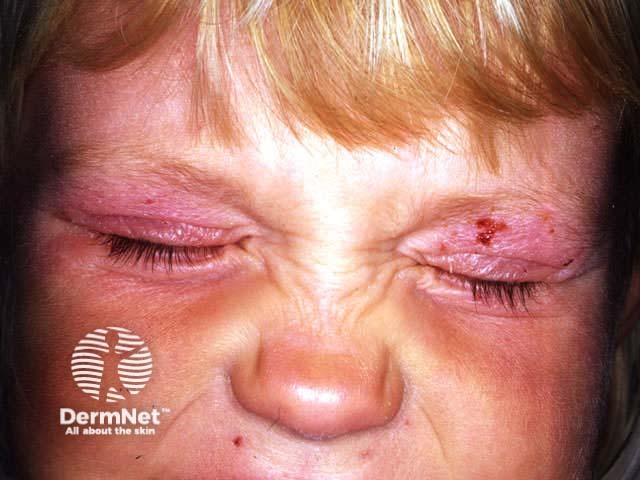
Atopic dermatitis
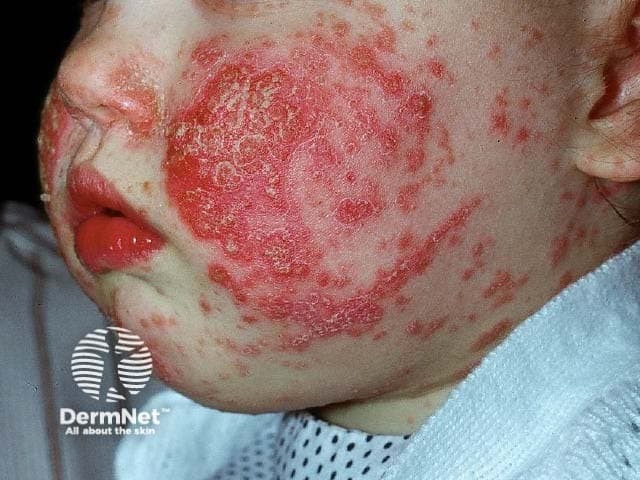
Atopic dermatitis
Trunk and limbs
These sites may require thicker emollients (sorbolene cream, white soft paraffin, emulsifying ointment, fatty cream) and moderate potency topical steroid fatty cream or ointment, with potent topical steroids for flare-ups. It is often useful to apply the potent preparation prophylactically on two consecutive days each week (pulse therapy). Ultrapotent products may be required for severe lichenification.
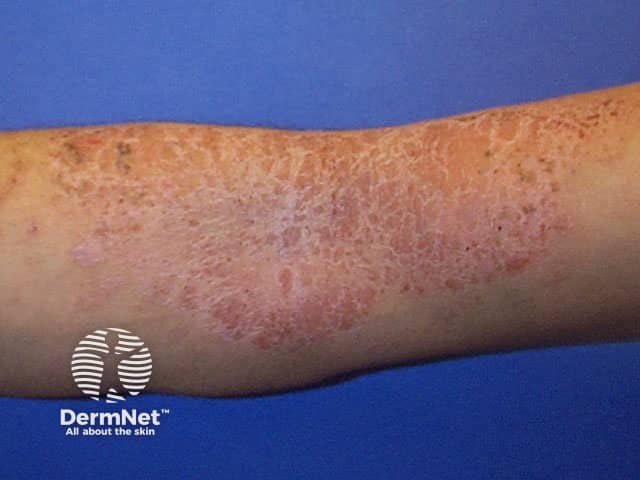
Atopic dermatitis
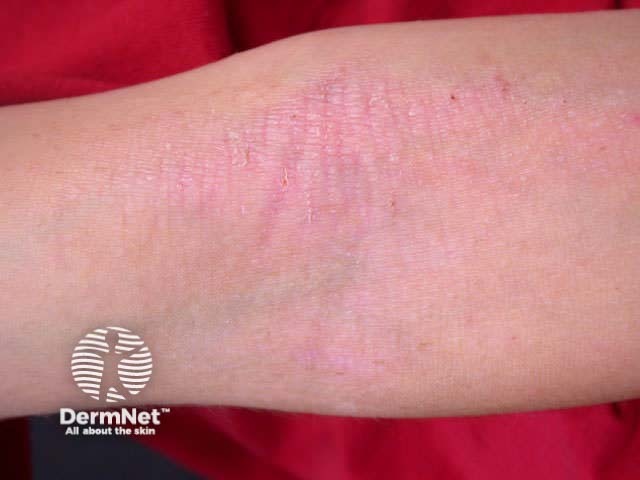
Atopic dermatitis
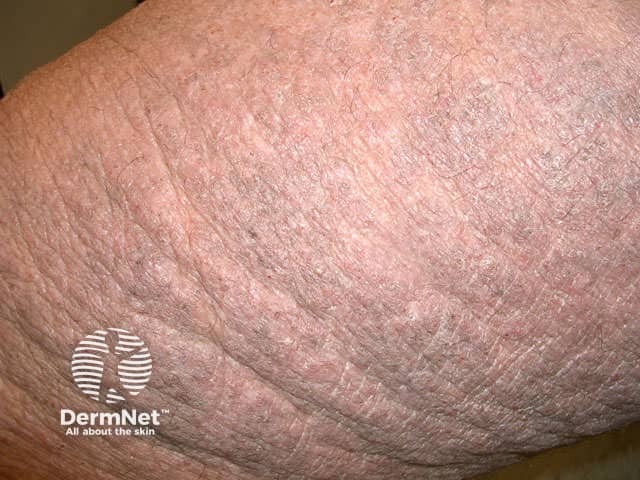
Atopic dermatitis
Hands and feet
The very thick stratum corneum of palmoplantar sites necessitates the use of ultrapotent topical steroids such as clobetasol propionate, generally in an ointment base, for two to four weeks. Advise frequent use of emollient barrier creams that contain dimethicone and/or petrolatum, and careful protection against irritants.
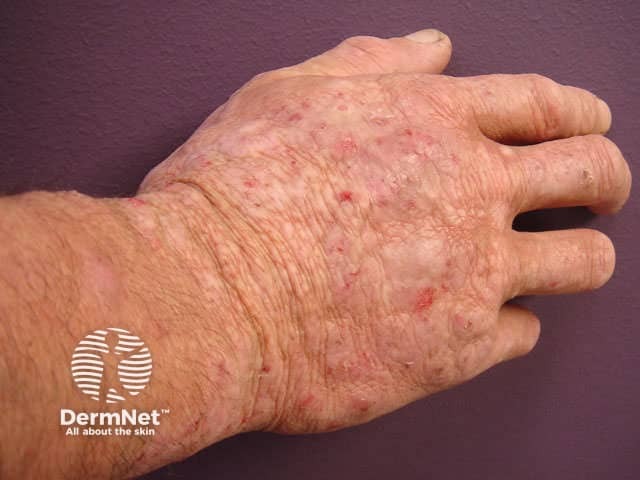
Atopic dermatitis
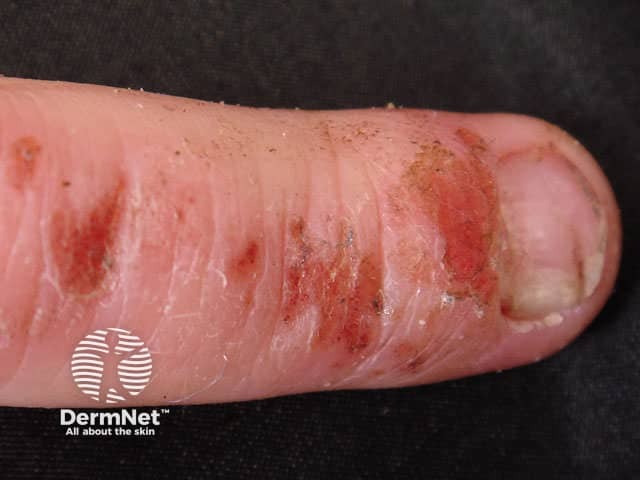
Atopic dermatitis
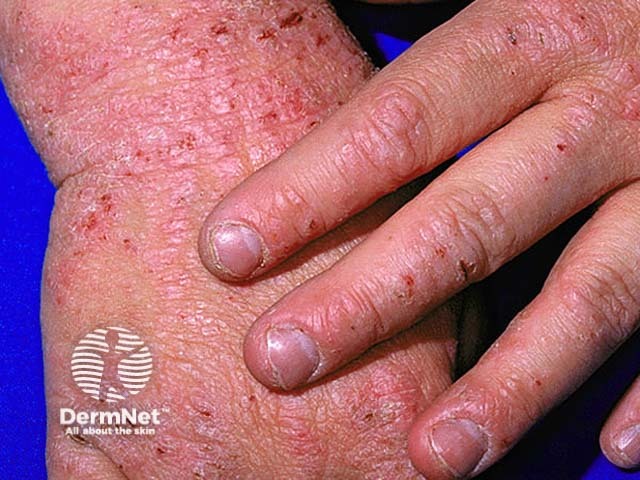
Atopic dermatitis
Axillae and groins
Flexures do not generally require emollients. Potent topical steroids are rarely required, and should only be used for a few days. Hydrocortisone cream or pimecrolimus cream is generally adequate.
Dermatologists rarely recommend dietary manipulation for atopic dermatitis because it is troublesome, expensive and not often helpful. However, about 30% of children with eczema also have food allergies causing urticaria and anaphylactic responses. In some of these, certain foods may consistently aggravate their eczema. The most well established food allergies associated with eczema are to egg, milk, peanut, wheat, and soy.
If there is a strong suspicion of food allergy, a specific RAST test reaction or positive prick test may be supportive but should be confirmed with controlled food challenges and a limited elimination diet that results in consistent clinical improvement. Extensive elimination diets can be nutritionally deficient and are useless. Most affected children outgrow their food hypersensitivity.
Extended avoidance of house dust mites in sensitised patients with atopic dermatitis is reported to be helpful but is difficult to achieve. Avoidance measures include use of house dust mite-proof encasings on pillows, mattresses, and duvets; washing bedding in hot water weekly; removal of bedroom carpets; and decreasing indoor humidity levels.
Immunotherapy has not been found to be useful.
Describe the evidence for and against the value of (a) breast feeding, and (b) probiotics, in the prevention of atopic dermatitis in infants.
Information for patients
See the DermNet bookstore