DermNet provides Google Translate, a free machine translation service. Note that this may not provide an exact translation in all languages
Home Fungal skin infections Tinea corporis CME
Fungal skin infections
Tinea corporis
Created 2009.
Learning objectives
- Identify and manage tinea corporis
Clinical features
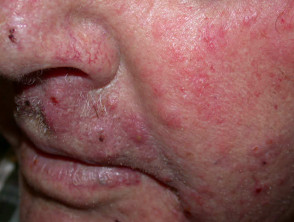
Tinea corporis presents as one or more round or oval erythematous scaly plaques that slowly enlarge. The appearance can be quite varied. The term ‘ringworm’ refers to the tendency for an annular raised edge and central healing. Any area can be involved including the face (tinea faciei).
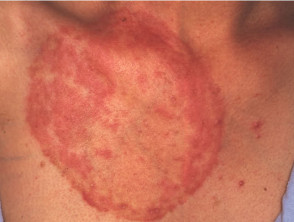
- M. canis (cat ringworm) is the most common cause of acute tinea corporis in New Zealand and arises from direct skin contact with an infected kitten. Most common sites are the chin, neck and forearms. It usually presents in children as an asymmetrical cluster of small (1 to 2 cm) erythematous itchy dry plaques.
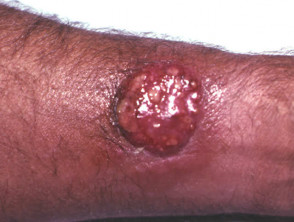
- T. verrucosum (cattle ringworm) also causes acute tinea corporis. One or a small number of plaques appear on exposed sites and are characterised by pustules or kerion.
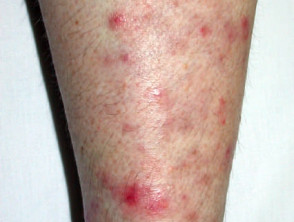
- T. rubrum is the most common cause of chronic tinea corporis in New Zealand. Infection often originates as tinea pedis or tinea unguium. The most common site is the lower leg but it may arise on any part of the body.
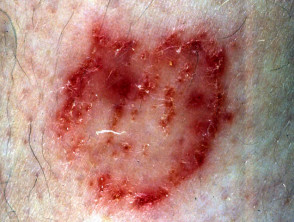
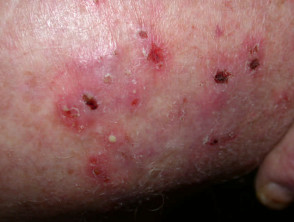
Kerion is the name given to markedly inflammatory tinea, presenting as an elevated exudative, eroded or pustular nodule or plaque.
Tinea incognita refers to tinea mistaken for a dermatitis and treated with topical steroids. The plaques are poorly demarcated and less inflamed, and may have pustules rather than scale.
Dermatophyte infections
Diagnosis
Obtaining scrapings from the active edge of the lesion for mycology. If you can't obtain a scraping, it probably isn't a fungal infection.
Look for other sites of infection (scalp, feet, nails).
Consider other reasons for scaly plaques:
- Discoid eczema (scattered dry or exudative round or oval plaques, sometimes with more pronounced edge, may or may not be itchy, may or may not be atopic)
- Psoriasis (red scaly plaques which may be annular, often signs elsewhere such as scalp, elbows, knees, flexures, nails)
- Pityriasis rosea (larger initial herald patch, symmetrical oval plaques on trunk with dry centre and trailing scale)
Consider other reasons for annular lesions:
- Granuloma annulare (dermal skin coloured or violaceous plaques, often over joints, slightly tender on knocking)
- Annular erythemas (slowly extending rings with trailing scale)
Consider other reasons for eroded nodules:
- Staphylococcal abscess
- Anaplastic skin cancer
Management
If tinea corporis persists despite topical imidazole creams, or is extensive, oral therapy is required for two to eight weeks, usually terbinafine or itraconazole. Oral azoles require specialist approval for PHARMAC subsidy. Griseofulvin may be more effective for M. canis infections but is no longer readily available in New Zealand.
Treatment should be continued until scaling has cleared up. If in doubt, repeat mycology and continue to observe.
Activity
Find out animal sources of dermatophyte infection. Are there specific clinical features that distinguish them?
Related information
References:
On DermNet NZ:
Information for patients
Other websites:
- Medscape Reference: Tinea corporis
- Merck Manual Professional: Dermatophytoses
Books about skin diseases:
See the DermNet NZ bookstore
Sign up to the newsletter
© 2024 DermNet.
DermNet does not provide an online consultation service. If you have any concerns with your skin or its treatment, see a dermatologist for advice.