DermNet provides Google Translate, a free machine translation service. Note that this may not provide an exact translation in all languages
Home Common skin lesions Benign keratinocytic and adnexal lesions CME
Common skin lesions
Benign keratinocytic and adnexal lesions
Created 2008.
Learning objectives
- Identify and describe acquired benign keratinocytic and adnexal lesions
Introduction
Acquired benign keratinocytic tumours to be discussed in this section include seborrhoeic keratoses, corns and calluses. They are extremely common and mainly of cosmetic concern. They may occasionally prove painful.
There are various benign tumours derived from adnexal structures. Various combinations of follicular, sebaceous, apocrine and eccrine differentiation occur commonly (mixed tumour or chondroid syringoma).
Seborrhoeic keratoses
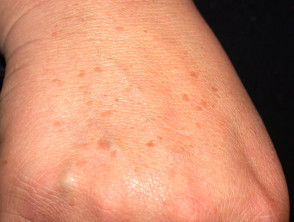
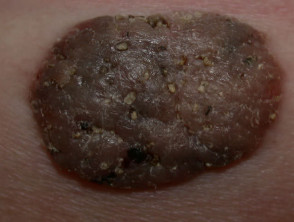
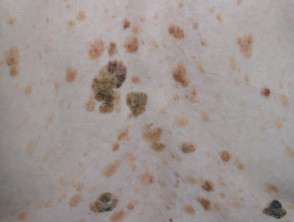
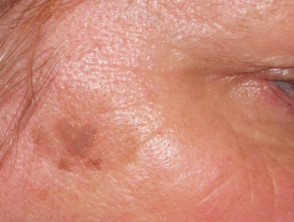
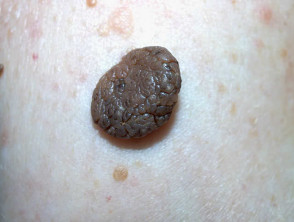
Seborrhoeic keratoses (basal cell papillomas) appear as stuck-on warty plaques and are very common on the face, neck and trunk in those over 40 years of age. The surface may be waxy or rough. They do not affect non-hair bearing areas such as the palms and soles. There is a familial predisposition in those with hundreds of lesions. They can present as macules, papules, plaques, verrucous, polypoid or pedunculated lesions. They can range in colour from white to black and may be confused with malignant melanoma; dermatoscopic features are often helpful to enable the distinction.
Some solar lentigines represent flat seborrhoeic warts.
Multiple eruptive lesions may arise when a patient is unwell, and is sometimes a sign of systemic malignancy (sign of Leser-Trélat. They may also appear after skin injury, including sun burn and dermatitis.
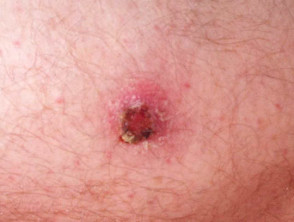
Irritated seborrhoeic keratosis is erythematous and crusty. It can resemble squamous cell carcinoma. These lesions may resolve spontaneously.
Seborrhoeic keratoses
Variants include:
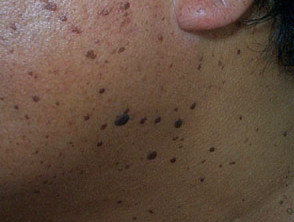
- Dermatitis papulosa nigra (black papules on face and neck of dark skinned individuals)
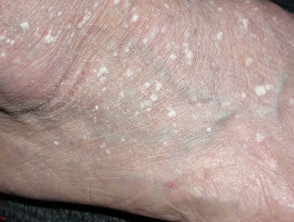
- Stucco keratoses (small scaly papules of lower legs and feet)
- Inverted follicular keratosis (solitary papule on face and neck
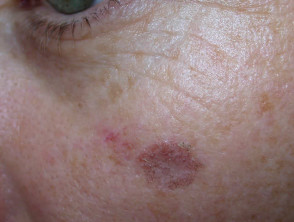
- Lichenoid keratosis (dry, pink or greyish-brown papules or plaques in which there is lichenoid inflammation)
Variants of seborrhoeic keratosis
Seborrhoeic keratoses are unsightly and often pruritic. They are readily removed by superficial destructive means such as shave excision, electrodessication or cryotherapy. However, if melanoma is considered in the differential diagnosis, the lesions should be fully excised for histology.
Corns and calluses
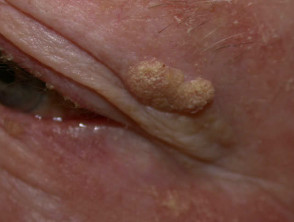
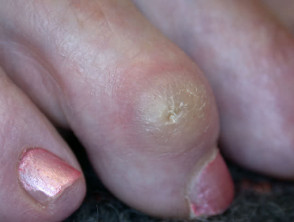
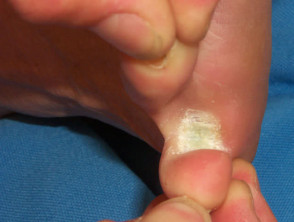
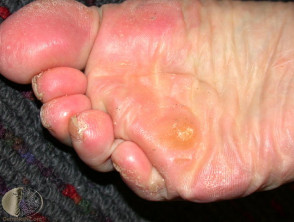
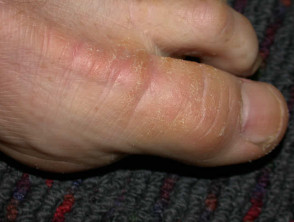
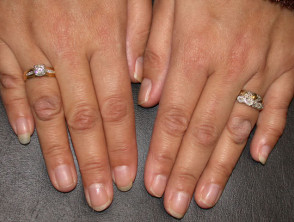
Corns and calluses represent localised hyperkeratosis induced by pressure, most often on hands and feet. Hard corns are firm papules with translucent central cores, found on the dorsolateral fifth toes and dorsal aspects of other toes. Soft corns are painful scaly plaques found between the toes. They often become macerated. Broad keratotic plaques, often under the metatarsal heads or over the metacarpals, are calluses.
Corns and calluses
Treatment involves paring down or filing the callosity. This is easier after soaking in warm water or applying a keratolytic such as salicylic acid or urea ointment, gel, paint or plaster. The pressure on the affected area should be relieved where possible using soft cushioning material or specific orthotic devices.
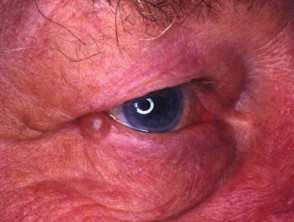
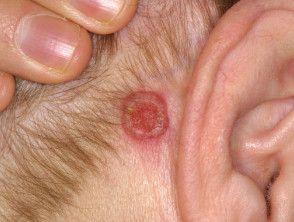
Chondrodermatitis nodularis helicis
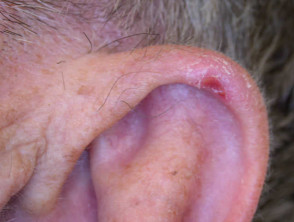
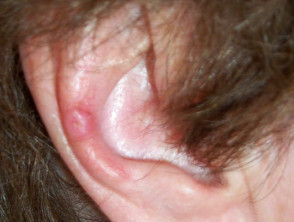
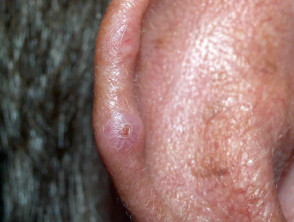
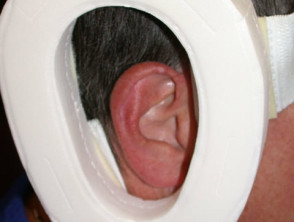
This condition, often referred to as ‘CNH’, presents as a tender papule on one or both ears, most often affecting the helix or antehelix. It is most common in men over 40 years, and probably represents ischaemic damage due to pressure on sun- and/or cold-damaged skin and cartilage, provoked by lying on it at night. Treatment involves relieving the pressure using a foam or silicone protector. Persistent lesions are usually excised but may recur.
Chondrodermatitis nodularis
Cysts
There are many types of cutaneous cyst.
Stratified squamous epithelial cysts
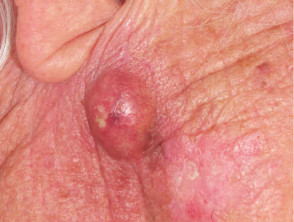
Epidermoid cysts are walled-off cavities filled with keratin and are derived from the hair follicle unit. Their contents can be expressed and have an unpleasant, cheesy odour. Epidermoid cysts are often found on the face and upper trunk and may be an inherited trait. If they rupture, they become inflamed (red and painful). Although this resembles infection, culture is generally sterile and antibiotics ineffective.
Stratified squamous epithelial cysts
Small superficial and often multiple cysts are known as milia, and occur on the face or as inclusion cysts in healing wounds, characteristically after subepidermal blistering.
Milia
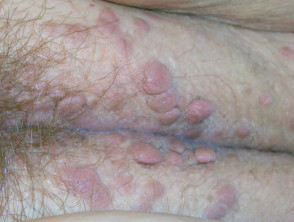
Multiple epidermoid cysts may accompany acne vulgaris. They are also a feature of Gardner syndrome, when they are associated with colonic polyps. Multiple scrotal or vulval cysts eventually calcify.
Multiple cysts
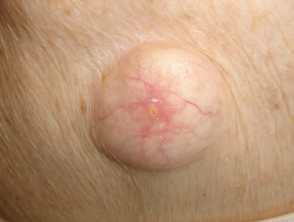
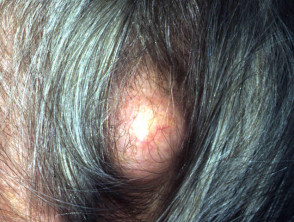
Trichilemmal or pilar cysts (scalp), vellus hair cysts (eruptive papules) and steatocystoma (oily lesions on chest) have characteristic histological features. The dermoid cyst occurs at the site of embryonic fusion planes, for example lateral eyebrow. A preauricular cyst is often called an ‘ear pit cyst’. The pilonidal cyst arises in the upper gluteal cleft, and may be associated with hidradenitis suppurativa.
Stratified squamous cell cysts
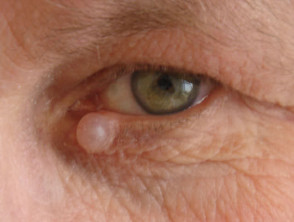
Non-stratified epithelial cysts
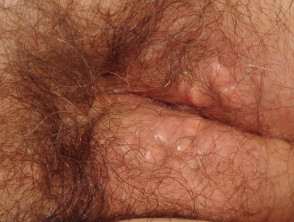
Cysts composed of non-stratified epithelium include hidrocystoma (eyelid margin) and others described by their embryonic origin, such as bronchogenic cyst (suprasternal notch), thyroglossal duct cyst (midline anterior neck), brachial cleft cyst (lateral neck and mandible).
Non-epithelial cysts
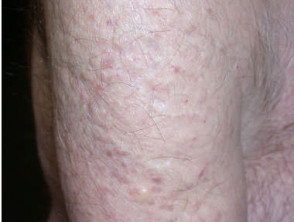
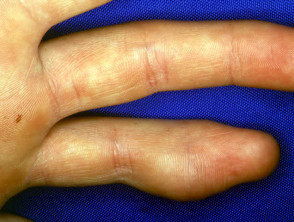
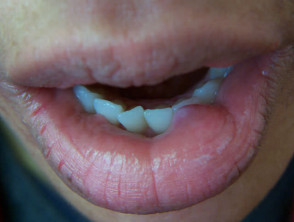
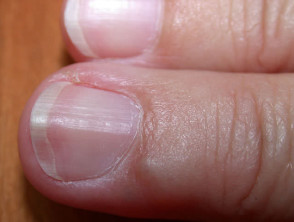
Non-epithelial cysts include the mucocoele (inner lip), mucous cyst (distal digit and nail bed), ganglion (wrist) pseudocysts of auricle (ear) and some traumatic cysts.
Non-stratified cysts
Follicular tumours
Lesions showing follicular differentiation contain basaloid cells resembling the follicular bulb, adjacent mesenchymal cells resembling the papilla, ‘shadow’ cells and trichilemmal (outer root sheath) cells, i.e. palisading pale cells with a thickened basement membrane.
Benign solitary or multiple follicular tumours include:
- Trichofolliculoma: vellus hairs seen within a skin coloured papule.
- Trichoepithelioma/trichoblastoma: follicular germinative differentiation (Brooke disease).
- Pilomatricoma (trichomatrioma, calcifying epithelioma of Malherbe): follicular matrical cornification. Often presenting as a hard, calcified papule or nodule in a child.
- Tricholemmoma: differentiation mostly toward the follicular outer sheath (Cowden syndrome).
- Trichodiscoma and fibrofolliculoma: multiple skin coloured papules in which histology shows stromal proliferation (Birt-Hogg-Dubé).
Follicular tumours
Tumours of sebaceous origin
Sebaceous differentiation results in cells with coarsely vacuolated cytoplasm and scalloped nuclei.
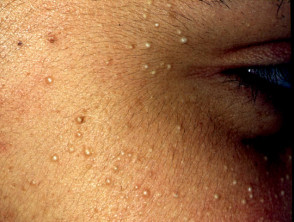
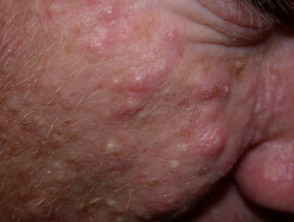
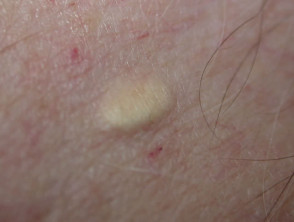
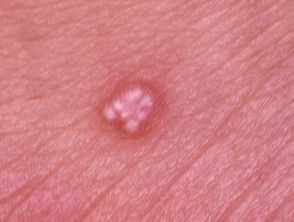
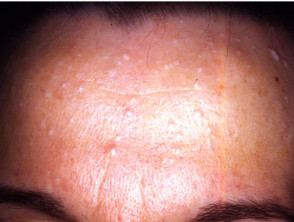
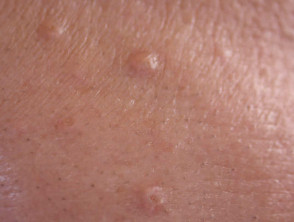
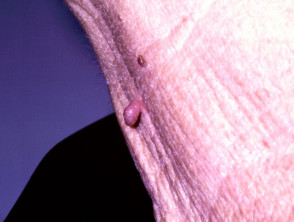
Sebaceous hyperplasia
Sebaceous hyperplasia represents benign enlargement of sebaceous lobules around the follicular infundibulum. Yellowish papules appear on the forehead or cheeks and have a characteristic central dimple.
Sebaceous hyperplasia
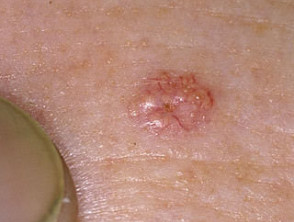
Sebaceous adenoma
These are solitary or multiple yellowish papules or nodules in which there is a proliferation of sebocytes and/or seboblasts (Muir-Torre syndrome)
Sweat gland tumours
It is difficult to determine whether sweat gland tumours are of eccrine or apocrine differentiation. The precise diagnosis of sweat gland lesions is most likely to be made histologically rather than clinically.
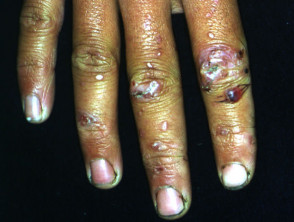
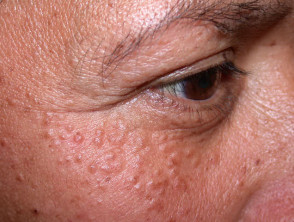
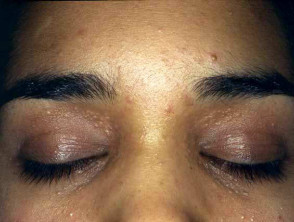
Syringoma
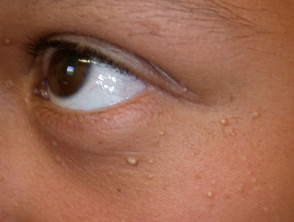
Syringomata are sweat duct tumours most often presenting as multiple skin-coloured papules on the eyelids. They may also develop on genital skin (apocrine). Eruptive syringomata sometimes affect hands and feet (eccrine).
Syringomata
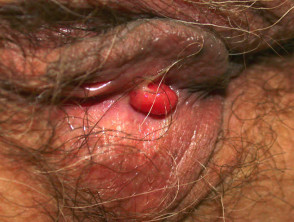
Poroma
Poromas have terminal ductal differentiation. They present as solitary papules most often on acral regions (eccrine origin) and are sometimes pigmented. Hidradenoma looks similar, but the cells have a greater amount of cytoplasm histologically. They most often appear in genital sites (apocrine origin). Papillary hidradenoma (hidradenoma papilliferum) is a variant with papillary pattern histologically, and may affect the nipple. Syringocystadenoma papilliferum tends to present as grouped keratotic papules, and may arise in a sebaceous naevus so presumably also has apocrine origin.
Eccrine tumours
Spiradenoma
Spiradenoma is the name given to an undifferentiated or poorly differentiated benign adnexal neoplasm that has some tubular features. They may be solitary or multiple and are often painful.
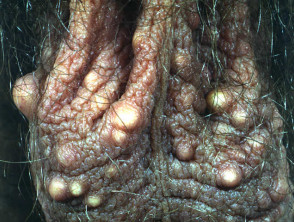
Cylindroma
Cylindroma describes an undifferentiated or poorly differentiated adnexal neoplasm with a mosaic pattern, presumably apocrine in origin. They may be solitary or multiple and are sometimes huge (turban tumour).
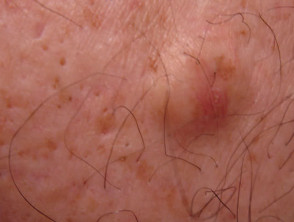
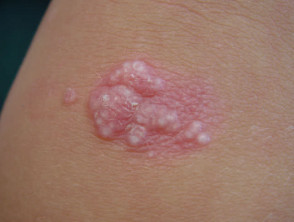
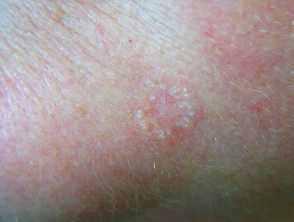
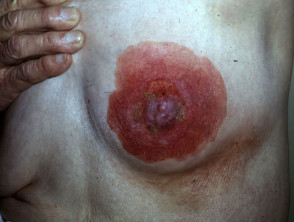
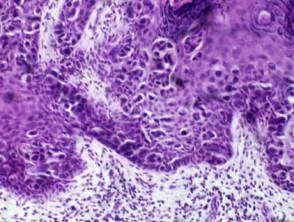
Paget disease
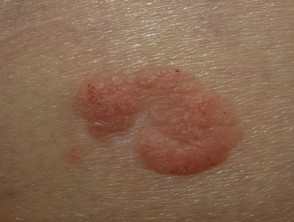
Paget disease presents as a dry red mildly irritable plaque. It is due to an intraepidermal malignant proliferation of clear cells and has characteristic histology.
Mammary Paget disease
Mammary Paget disease presents as a unilateral eczema-like plaque on the nipple or areola. It is associated with underlying in-situ ductal carcinoma or other underlying cancer. Investigation should include mammography and management should be by a breast surgeon.
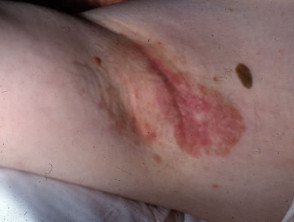
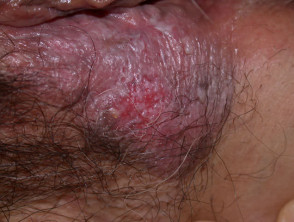
Extra-mammary Paget disease
Extra-mammary Paget disease presents as a dry red plaque in the axillae, or on genital or perianal skin. It is sometimes associated with underlying adenocarcinoma arising in adjacent but not necessarily contiguous tissue. If no such tumour is found, wide local excision is the usual management but recurrence is common. Alternative treatment may include fluorouracil cream, imiquimod cream, or photodynamic therapy.
Paget disease
Activity
Describe Birt-Hogg-Dubé syndrome.
Related information
References:
On DermNet NZ:
Information for patients
Other websites:
- Medscape Reference: Benign neoplasms
- Merck Medicus Best Practice of Medicine: Common cutaneous tumours
- American Family Physician: Minimal Excision Technique for Epidermoid (Sebaceous) Cysts 2002
Books about skin diseases:
See the DermNet NZ bookstore
Sign up to the newsletter
© 2024 DermNet.
DermNet does not provide an online consultation service. If you have any concerns with your skin or its treatment, see a dermatologist for advice.