DermNet provides Google Translate, a free machine translation service. Note that this may not provide an exact translation in all languages
Home Phototherapy Photodynamic therapy
Phototherapy
Photodynamic therapy
Created 2007.
Learning objectives
- Describe photodynamic therapy (PDT)
- List current indications for PDT
- List contraindications to PDT
- Name two photosensitisers used in topical PDT
- Describe the mechanism of action
- Describe the method of treatment for topical PDT
- Describe side effects of topical PDT
- Describe the results of PDT for:
- Actinic keratoses
- In-situ squamous cell carcinoma
- Superficial basal cell carcinoma
Introduction
Photodynamic therapy (PDT) has been under investigation for several years but is now entering a new phase as a routine non-surgical treatment for certain types of skin cancer.
It involves a non-invasive oxygen-dependent phototoxic reaction that can be used for multiple lesions at one time. The photosensitiser can given intravenously or can be applied to the target lesion topically. It is selectively localised in the target tissue and illuminated with visible light, resulting in photodamage and subsequent cell death.
There is minimal damage to surrounding normal tissue hence side effects are limited to the target area. As a rule, cosmetic results are good or excellent.
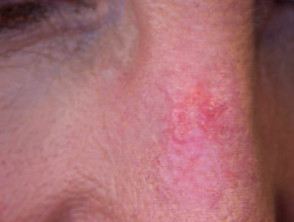
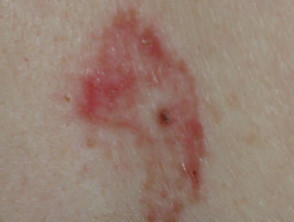
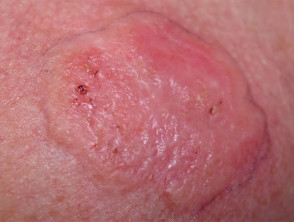
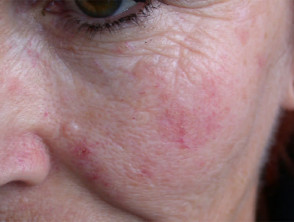
Effect of photodynamic therapy
Indications
The current indications for treatment are thin localised skin cancers:
- Superficial basal cell carcinoma
- Nodular basal cell carcinomas after removal of the bulk of the lesion, particularly those off the head and neck
- In-situ squamous cell carcinoma (Bowen disease)
- Actinic keratosis
PDT may also prove effective in a wide variety of other skin conditions in which there is rapid proliferation of cells. Some of those under investigation include:
- Actinic cheilitis
- Viral warts
- Cutaneous T-cell lymphoma
- Kaposi's sarcoma
- Extramammary Paget's disease
- Psoriasis
- Cutaneous vascular malformations
- Hair epilation
It is not effective in the treatment of:
- Morphoeic or sclerosing basal cell carcinoma
- Invasive squamous cell carcinoma
- Pigmented melanoma
- Metastatic lesions
There is insufficient evidence to support its use in amelanotic melanoma in situ.
Contraindications to treatment
Contraindications to systemic PDT include:
- A non-responsive tumour
- Porphyria
- Systemic lupus erythematosus
- Other photosensitivity dermatoses
- Allergy to the photosensitiser (very rare)
Photosensitisers
The photosensitisers in common use in dermatology are porphyrins but other chemicals are being used for cancers in other organs.
The drug must concentrate in the target cell quickly to allow a short drug-to-light interval. It should be inactive in non-target tissues. The absorption spectrum should involve wavelengths that penetrate at least a few millimetres into skin and that have sufficient energy for photochemical effect. Topical application of a photosensitiser limits the area of skin that reacts to light.
For skin cancer treatment, most published research reports the effect of topically applied aminolaevulinic acid (ALA), which is converted to protoporphyrin IX. This metabolism occurs physiologically in the haem cycle but the rate is limited by enzymatic conversion so that phototoxicity only arises in disease states (porphyrias). When ALA is applied topically to a tumour, the rate-limiting steps are bypassed so that protoporphyrin IX accumulates in the rapidly proliferating cells.
Mechanism of action
Tissue destruction (cytotoxicity) arises from a complex mixture of biochemical and molecular reactions in which there is direct killing of cells, vascular damage, inflammation and an immunological response.
Method of treatment
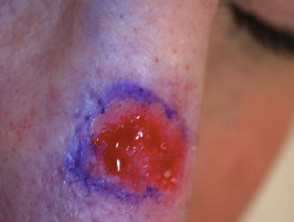
As with other skin cancer treatments, an experienced dermatologist should determine whether the lesion is appropriate for PDT. A skin biopsy will frequently be required. The tumour should be less than one millimetre in thickness and its margins should be carefully identified.
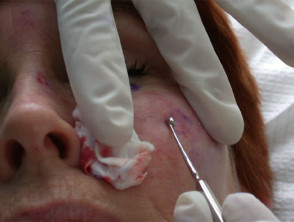
To enhance penetration of the photosensitiser through intact keratinised skin, the skin surface should be roughened or pricked using a sharp instrument such as a blade or curette.
Preparation of the lesion
An oil-in-water emulsion of 20% ALA may be used, or methyl aminolevulinate 160 mg/g in a cream base. The latter is retained more effectively at the site of application allowing more rapid treatment and less leakage of photosensitiser to surrounding skin.
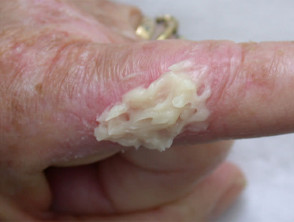
Application of Metvix® cream to keratoses
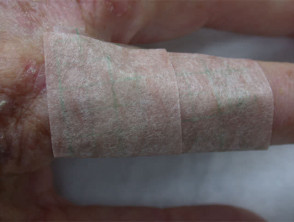
Visible light photodegrades the photoactive metabolites, so treated areas must be covered until deliberately exposed to the photoactive wavelength 630-635nm three to six hours later.
Protecting treated area from light
Reported effective doses vary from 30-540 J/cm2 depending on the light source used. These may be conventional incoherent sources, lasers or a portable diode system such as the Aktilite illustrated. This supplies a dose of 75 J/cm2 over about 8 minutes, with a continuous waveband of 570-670 nm.
Aktilite®
A second identical treatment is performed for most lesions 7 to 14 days after the first treatment.
Actinic keratoses
Response rates of 80-100% have been reported for single or repeated topical ALA or methyl aminolevulinate PDT. It is particularly useful for widespread lesions, except that larger areas require more drug so it may be a very costly option for treatment.
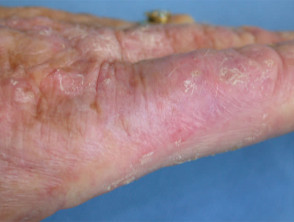
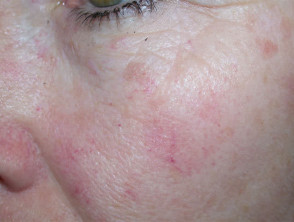
Effect of photodynamic therapy on actinic keratoses
Response rates are equal or better than with cryotherapy and chemical peels. Cosmetic results are excellent. However, hyperkeratotic lesions appear to respond poorly compared to less scaly lesions, probably because of poor penetration of the photosensitiser.
In-situ squamous cell carcinoma
In-situ squamous cell carcinoma (Bowen disease) is an excellent indication for topical PDT, which is more effective and better tolerated than vigorous cryotherapy. Multiple lesions have been reported to clear using a systemic photosensitiser (porfimer sodium).
Basal cell carcinoma
At present, basal cell carcinoma (BCC) is the most common skin lesion treated by PDT in New Zealand. It is especially useful for superficial basal cell carcinomas, which are frequently multiple and may be very large making surgery difficult and deforming. Two treatments are generally necessary. If lesions persist at 3 months, or recur later, PDT may be repeated.
Reported cure rates vary from 50 to 100%, with a variety of systemic or topical photosensitisers. Methyl aminolevulinate PDT has 80-100% histological cure rates with two treatments at 7-day intervals. Cosmetic outcomes are generally excellent and the treatment is popular with patients.
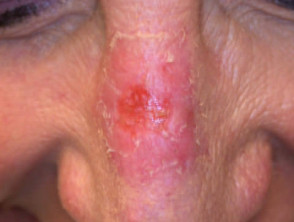
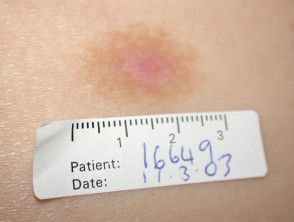
Effect of photodynamic therapy on basal cell carcinoma
Nodular BCCs may also respond well to treatment. However, as neither the ALA nor the light penetrates deeply, good results require debulking of the tumour by shave/curette so that it is less than one millimetre in thickness. Waiting up to 48 hours prior to exposure to light and repeated treatments may also be helpful.
Failure may arise if the true margin of the tumour is underestimated when the ALA is applied or if the light field exposure is too small.
Pigmented BCCs respond less well, presumably because melanin prevents the penetration of the light.
Morphoeic (sclerosing or fibrosing) tumours are resistant to PDT, probably because the excessive collagen matrix protects against it. They should be dealt with by adequate excision.
Cure rates with conventional surgery probably remain better than PDT, especially if it is compared to Mohs micrographic surgery, “the gold standard” for eradicating BCCs. However, PDT is an excellent alternative in the following circumstances:
- Multiple tumours
- Large tumours
- Recurrent lesions
- Cosmetically or functionally problematic sites such as the mid-face, where excision is considered inappropriate
- Medically unfit patients.
Side effects
PDT is a relatively easy option for patients because it has relatively insignificant side effects and these are transient in nature.
Preparation of the lesion to be treated may involve a minor surgical procedure including biopsy or curettage, often requiring local anaesthetic.
The treated area generally burns and stings to variable degree during exposure to light. Treatment can be interrupted and/or analgesics and local anaesthetic can be used but are rarely necessary. The discomfort settles most often immediately after PDT but may take a few hours to do so.
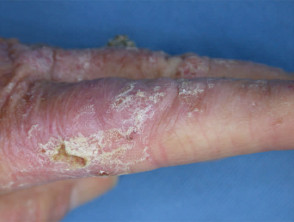
The lesion appears red and may be swollen (urticated) immediately after treatment and can be treated with a mild topical steroid if necessary. Over the next few days there is crusting, and scaling and there may be blistering, weeping and bleeding but this is not necessary to effect cure. The area should be covered for the expected duration of photosensitivity (usually 48 hours) or longer and simple emollients such as petroleum jelly used to soften crusts and reduce itch.
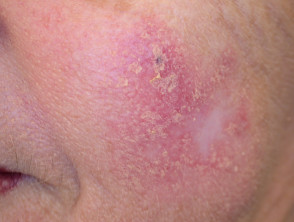
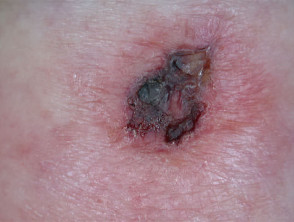
Adverse effects of photodynamic therapy
Cutaneous photosensitivity after systemic photosensitisers used for PDT may last weeks, depending on which drug is used, and is potentially dangerous. Sunscreens are not protective against the visible light wavelengths involved in the action spectrum for PDT. Patients' eyes and skin must be covered and sunlight and excessive indoor light strictly avoided. Low levels of indoor light are tolerated and help to inactivate residual drug in the skin.
Side effects from systemic PDT depend on the drug. ALA may result in nausea, vomiting, and transient liver function abnormalities. Neurovisceral symptoms experienced by patients with acute intermittent porphyria (AIP) have not been reported despite ALA plasma concentrations being up to 20-fold higher than in AIP.
Koebnerised psoriasis in treated areas has been reported.
Final results
One of the most desirable aspects of PDT is the excellent cosmetic outcome after treatment.
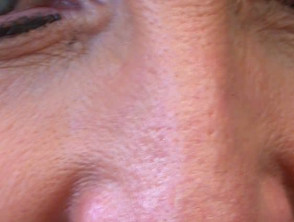
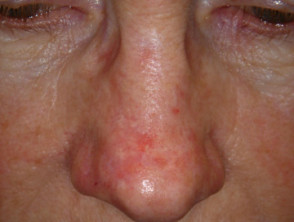
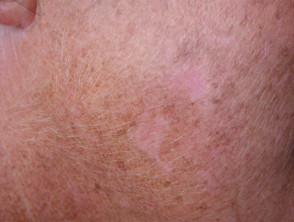
Cosmetic outcome
Often the treated area appears entirely normal within a month of treatment. However the following may arise after topical ALA PDT:
- Hyperpigmentation for up to several months
- Hypopigmentation for up to several months
- Scarring (extremely rare, but permanent)
- Persistent or recurrent tumour (treatment may be repeated or another modality selected).
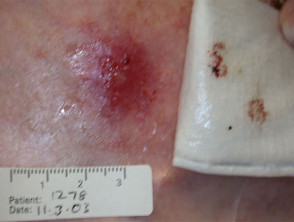
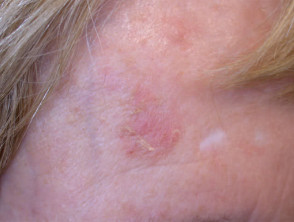
Pigmentary changes 1month, 3 month after PDT
Activity
Write an information sheet for patients having PDT treatment to basal cell carcinoma.
Take the Photodynamic therapy quiz
Related information
References
- Phototherapy resources
- BAD: Clinical Guidelines: Photodynamic therapy
- Medscape Reference: Photodynamic Therapy for the Dermatologist
On DermNet NZ
Information for patients
Books about skin diseases
Sign up to the newsletter
© 2024 DermNet.
DermNet does not provide an online consultation service. If you have any concerns with your skin or its treatment, see a dermatologist for advice.