DermNet provides Google Translate, a free machine translation service. Note that this may not provide an exact translation in all languages
Home Viral skin infections Herpes simplex CME
Viral skin infections
Herpes simplex
Created 2009.
Learning objectives
- Identify and manage herpes simplex infections
Clinical features
Herpes simplex virus (HSV) type 1 mainly affects the face and type 2 mainly affects genital skin, although in 10% of infections the reverse is true and any mucocutaneous site may be affected.
The virus is inoculated into the affected area and is more likely with minor injury, e.g. facial lesions contracted in rugby (‘scrum pox’).
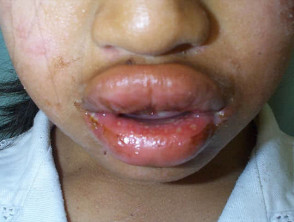
- Primary type 1 HSV infections occur mainly in infants and young children, and are usually mild or subclinical but may result in severe ulceration, oedema, regional lymphadenopathy and systemic symptoms.
- Type 2 infections occur mainly after puberty, often transmitted sexually.
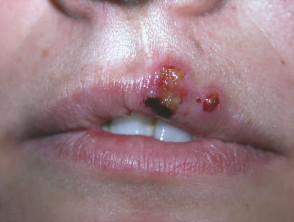
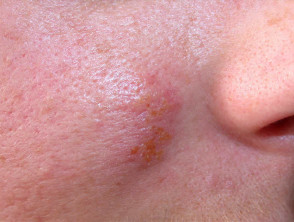
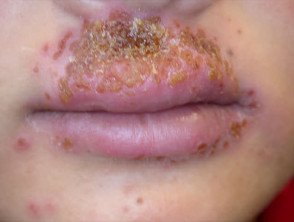
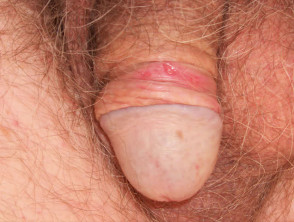
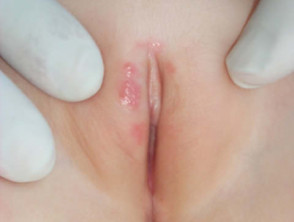
Both type 1 and type 2 herpes simplex viruses reside in a latent state in spinal anterior horn cells. Recurrences are due to proliferation of virus within the epidermis of the affected dermatome and present as clusters of 2-3mm umbilicated clear or haemorrhagic vesicles. These persist for 5 to 10 days and are typically preceded by localised tingling or burning. Mild fever and malaise may occur. Asymptomatic viral shedding is also common.
Following the initial infection immunity develops but does not fully protect against further attacks in the same or new sites. However where immunity is deficient, both initial and recurrent infections tend to recur more frequently and to be more severe.
Complications may include:
- Postinflammatory hypo- or hyperpigmentation or scarring
- Localised neuralgia and/or paresis
- Keratoconjunctivitis
- Eczema herpeticum (severe primary herpes in patient with atopic dermatitis
- Throat infections
- Meningoencephalitis
- Disseminated infection
- Neonatal herpes infection
Recurrent herpes infections can be triggered by:
- Localised trauma: dental procedure, injection, cosmetic treatment
- Upper respiratory tract infections
- Exposure to ultraviolet radiation
- Premenstrual tension
- Emotional stress and unknown factors
Investigations
The diagnosis may be confirmed by one of the following methods:
- Viral culture of swab from vesicle (reported in about 5 days)
- Immunofluorescence of basal cells collected from fresh vesicles onto slides for rapid identification (24 hours).
- 5ml plain tube blood or 500 µl serum for serology
Management
Topical therapy for mild herpetic infections may include:
- Aciclovir cream
- Penciclovir cream
- Idoxuridine solution
- Povidone iodine solution
Oral aciclovir is used for:
- Severe primary or recurrent infections, 200mg five times daily commenced within 48 hours
- Short-term prophylaxis, 400mg bd to cover facial surgery, cosmetic procedures or parturition
- Long term prophylaxis (3 months to life long) for those with frequent significant recurrences
Resistant cases, 23 April 2005in the presence of HIV infection, may be treated with foscarnet
There are no other systemic antiherpetic drugs available in New Zealand. However, twice daily dosing is more convenient and possible with famciclovir and valciclovir.
Activity
Find out the prevalence of herpes simplex type 1 and type 2 infections in New Zealand. How many patients are symptomatic?
Related information
References:
On DermNet NZ:
Information for patients
Other websites:
- Medscape Reference: Herpes simplex
- Medscape: Genital herpes Resource center
- Prodigy Guidance:
- Herpes simplex – oral July 2005
- Herpes simplex – genital 30 November 2005
- Merck Manual Professional: Herpes viruses
Books about skin diseases:
See the DermNet NZ bookstore
Sign up to the newsletter
© 2024 DermNet.
DermNet does not provide an online consultation service. If you have any concerns with your skin or its treatment, see a dermatologist for advice.