Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Vanessa Ngan, Staff Writer, 2005. Updated by A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand, December 2015.
Introduction Demographics Causes Clinical features Diagnosis Treatment
Postinflammatory pigmentation is temporary pigmentation that follows injury (eg, a thermal burn) or inflammatory disorder of the skin (eg, dermatitis, infection). It is mostly observed in darker skin types (see ethnic dermatology). Postinflammatory pigmentation is also called acquired melanosis.
More severe injury results in postinflammatory hypopigmentation, which is usually permanent.
Postinflammatory hyperpigmentation can occur in anyone but is more common in darker-skinned individuals, in whom the colour tends to be more intense and persist for a longer period than in lighter skin colours. Pigmentation tends to more pronounced in sun-induced skin conditions such as phytophotodermatitis and lichenoid dermatoses (skin conditions with lichen planus-like inflammation, such as erythema dyschromicum perstans).
Some medications may also darken postinflammatory pigmentation. These include antimalarial drugs, clofazimine, tetracycline, anticancer drugs such as bleomycin (flagellate erythema), doxorubicin, 5-fluorouracil and busulfan.
Postinflammatory hyperpigmentation follows damage to the epidermis and/or dermis with deposition of melanin within the keratinocytes (skin cells) and/or dermis.
Inflammation in the epidermis stimulates melanocytes to increase melanin synthesis and to transfer the pigment to surrounding keratinocytes (epidermal melanosis). If the basal layer is injured (e.g. lichen planus), melanin pigment is released and subsequently trapped by macrophages in the papillary dermis (dermal melanosis or pigment incontinence).
Postinflammatory hyperpigmented patches are located at the site of the original disease after it has healed. The lesions range from light brown to black in colour. The patches may become darker if exposed to sunlight (UV rays).
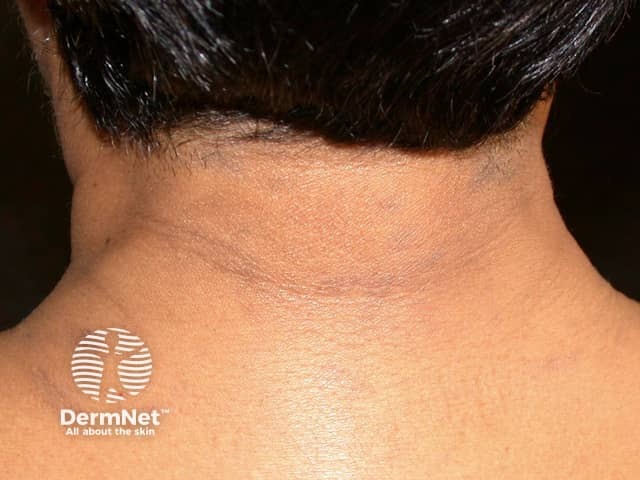
Lichen planus actinicus
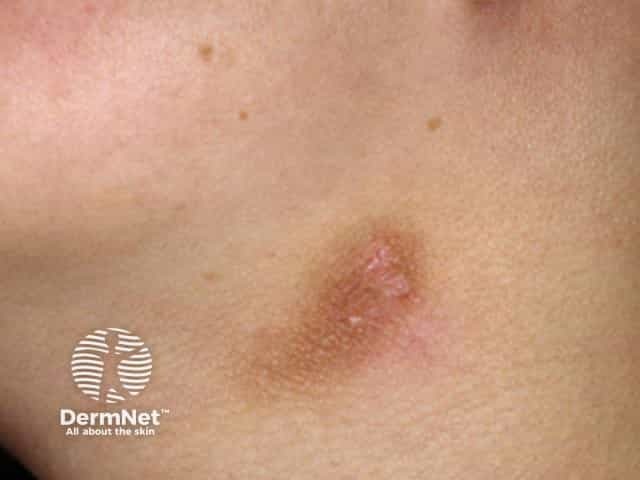
Violin playing (friction)

Irritant dermatitis
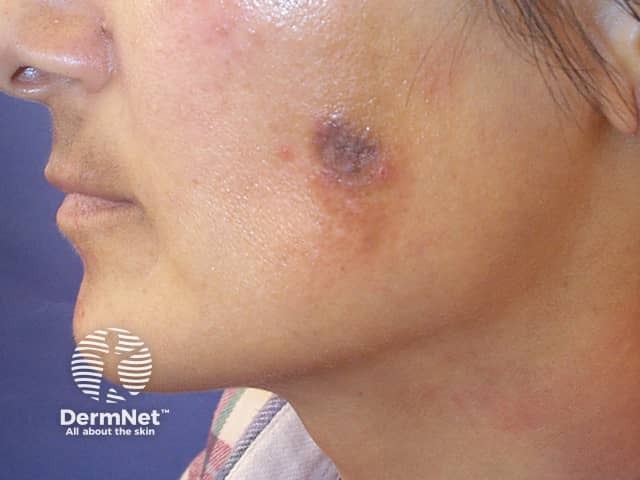
Postinflammatory hyperpigmentation (inflamed cyst)
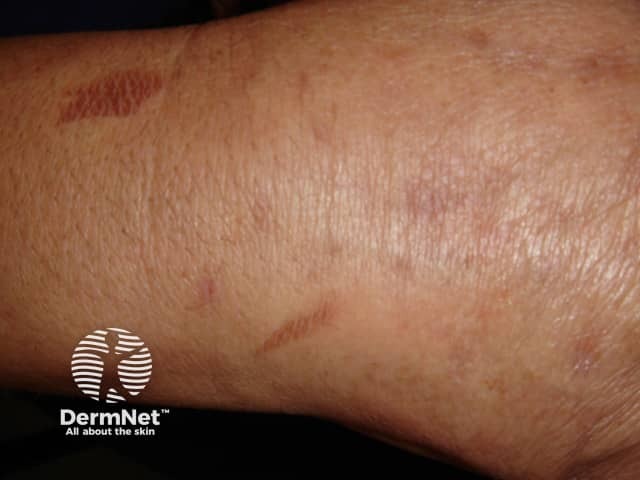
Oven burn
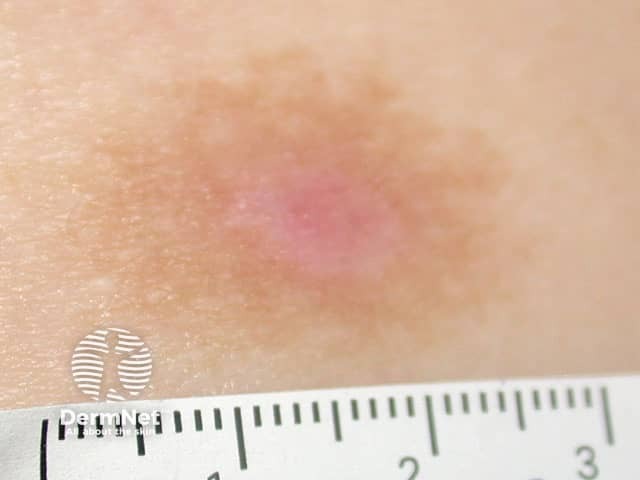
Photodynamic therapy
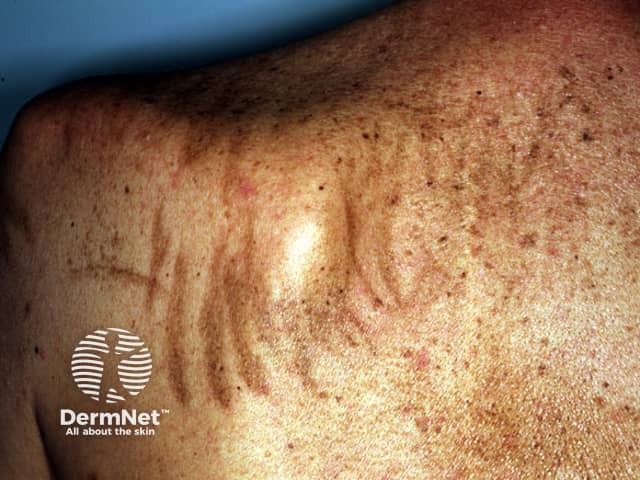
Flagellate reaction to bleomycin

Healed eczema
Postinflammatory hyperpigmentation is diagnosed by taking a careful history and examining the skin. Dermal melanosis gives a characteristic hue to the skin colour (grey-purple-brown).
Sometimes the diagnosis is only made after skin biopsy. Histopathology reveals patchy epidermal melanosis and/or dermal melanosis.
If pigmentation affects an exposed site, daily application of SPF 50+ broad-spectrum sunscreen is important to minimise darkening caused by UVR. Cosmetic camouflage can be used.
A variety of topical treatments are available to lighten/bleach hyperpigmented lesions in epidermal hypermelanosis. Varying degrees of success are achieved but combinations of the treatments below are usually required for significant improvement.
Chemical peels, laser treatments and intense pulsed light therapies (IPL) may be helpful for epidermal pigmentation, but physical treatments may also aggravate it by injuring the epidermis.
These treatments are not effective in dermal hypermelanosis.