Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Introduction
Demographics
Causes
Clinical features
Tests
Treatment
Napkin dermatitis and nappy rash are used to describe various skin conditions that affect the skin under a napkin or incontinence pad. The US term is diaper rash. Napkin dermatitis is most often a form of contact dermatitis.
Napkin dermatitis most often affects babies aged 3 to 15 months of age, especially those wearing traditional cloth nappies (50%). It is much less prevalent in babies wearing modern breathable and multilayered disposable nappies.
Napkin dermatitis can also affect older children and adults that are incontinent (see Incontinence-associated dermatitis).
Napkin dermatitis follows damage to the normal skin barrier and is primarily a form of irritant contact dermatitis.
Babies who are breastfed have a lower incidence of napkin dermatitis, as faeces in breastfed babies have a lower pH than in formula-fed babies. As babies start to eat solid foods, the stool frequency and pH start to increase and napkin dermatitis occurs more often.
Other causes of napkin rashes include:
Napkin dermatitis is not due to:
Napkin dermatitis presents as erythematous macules and papules in the genital area that can spread to involve the lower abdomen and thighs.
Napkin dermatitis may predispose the infant to urinary tract infection and, in females, to vaginal infection.
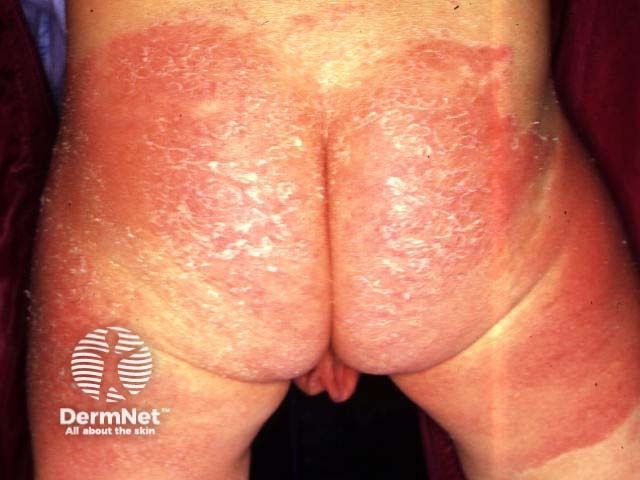
Napkin dermatitis
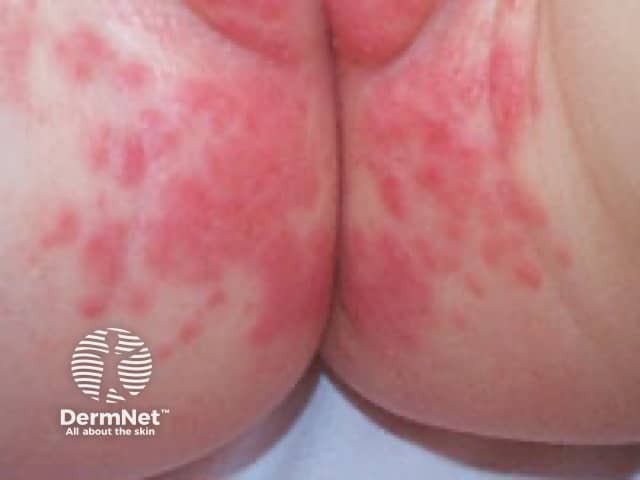
Napkin dermatitis thrush
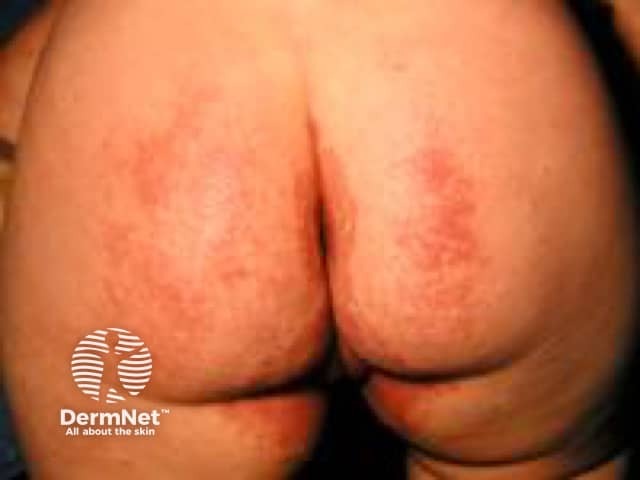
Napkin dermatitis
See more images of napkin dermatitis.
In most cases, no laboratory tests are necessary. Skin swabs may be useful to confirm Candida albicans or bacterial infection.
The need to keep baby dry and use barrier creams should be emphasised. The caregiver should always wash their hands before and after changing a nappy/diaper. Napkin dermatitis is much less common with modern disposable napkins than with cloth nappies.
Disposable nappies:
If using cloth nappies, nappy liners keep the skin dry. Avoid plastic overpants.
At napkin changes: