Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Created 2009.
Tinea pedis is most frequently due to Trichophyton rubrum, T. interdigitale (formerly known as T. mentagrophytes var. interdigitale) or Epidermophyton floccosum. Tinea pedis has various patterns and may affect one or both feet.
Tinea pedis is more common in adults than in children and frequently recurs after initially successful treatment with topical antifungal agents because of reinfection. Fungal spores can persist for months or years in bathrooms, changing rooms and around swimming pools.
Tinea pedis Tinea pedis Tinea pedis Athletes foot Athletes foot Tinea pedis 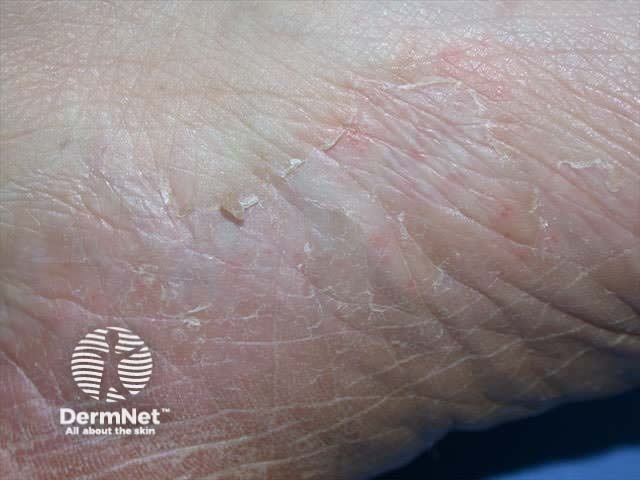
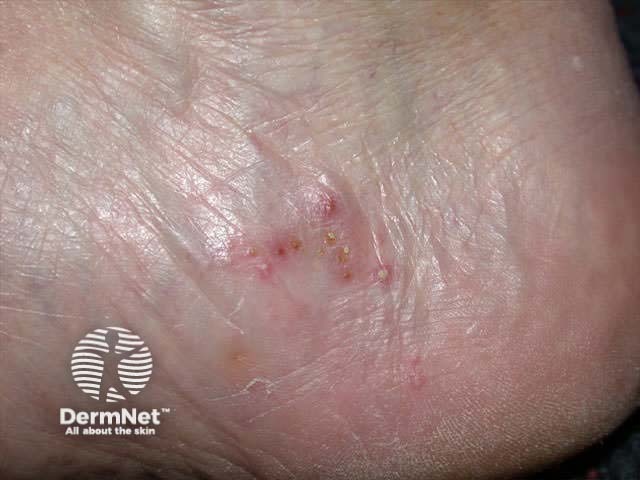
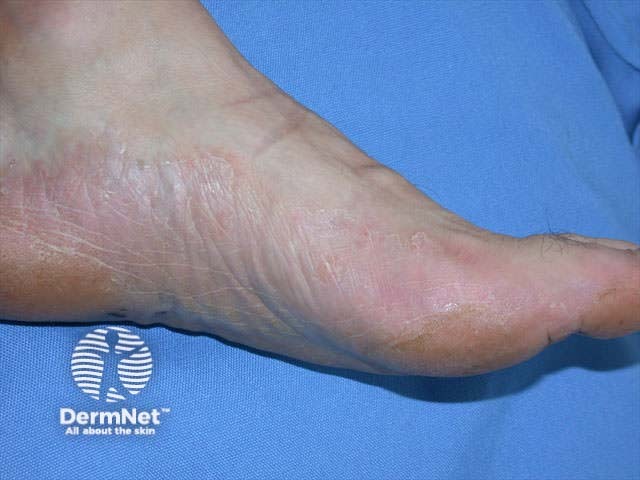
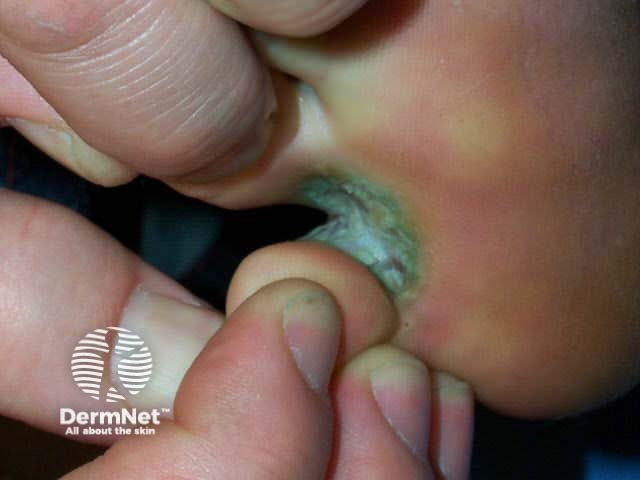
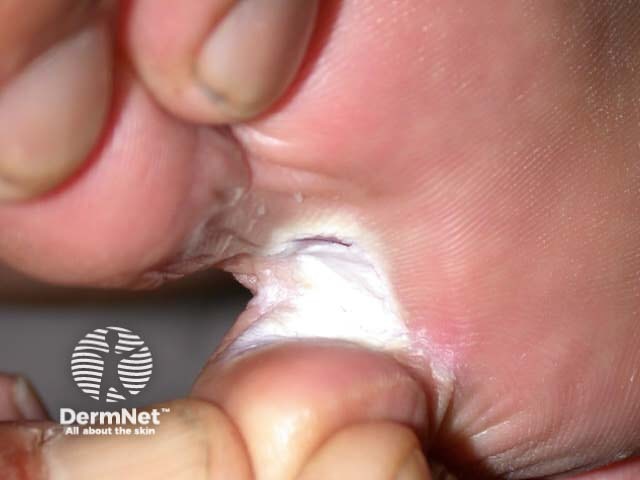
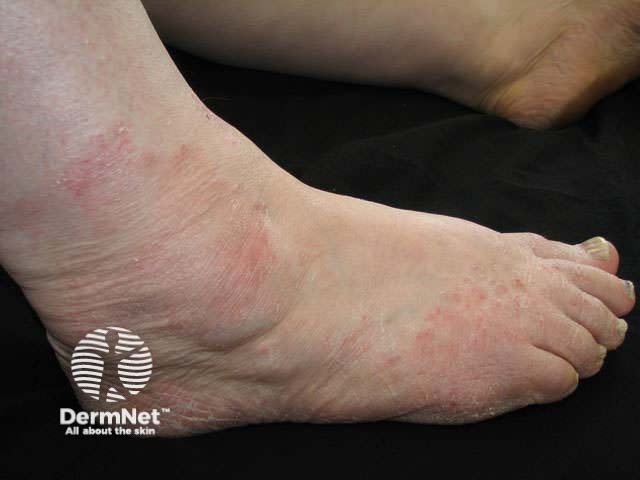
First confirm the diagnosis of tinea (scrapings and clippings) and look for other sites of infection (groin, nails). Consider alternative explanations including:
Mild and localised tinea pedis can be managed with education and topical antifungal agents. Tell the patient to hot wash socks and stockings, and to wipe out shoes with formalin or meths solution. They should be advised that the condition is mildly contagious, and to wear sandals in changing rooms and not to share towels and footwear. It is likely to recur, so suggest they dry carefully and apply an antifungal powder after bathing long term.
There are numerous topical antifungal agents, of which terbinafine cream (Lamisil™) is probably the most effective. Fully funded options in New Zealand (April 2005) are:
Whitfield ointment is also effective (benzoic acid 6%, salicyclic acid 3% in petrolatum).
Resistant and extensive culture-confirmed cases of tinea pedis will require oral therapy for one to four weeks, usually with terbinafine or itraconazole.
Confirmed tinea unguium may require oral antifungal agents for 3 months or longer if the infection is clinically significant and there are no contraindications to treatment. Cure rates depend on the severity of infection, the infecting organism, comorbidities and the age of the patient.
Find out how tinea manuum differs from tinea pedis.
Information for patients
See the DermNet bookstore.