Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Created 2008.
Basal cell carcinoma (BCC) is by far the most common cancer in humans. It may arise in habitually sun-exposed skin, especially on the face, or on areas that have been previously sunburned such as the back. Although most common in middle-aged and elderly, in New Zealand young adults also routinely present with basal cell carcinoma.
There is a strong association with both habitual sun exposure and a history of intermittent sunburn.
Somatic mutations are found in the PTCH, p53 and several other genes in sporadic basal cell carcinomas. There are specific ‘signature’ mutations that suggest that many or most of these are due to ultraviolet radiation.
Multiple and early onset BCCs are a feature of Gorlin syndrome (basal cell naevus syndrome). This very rare genodermatosis is also characterised by:
Palmar pits Multiple superficial BCCs Recurrent pigmented BCC Scars from treatment 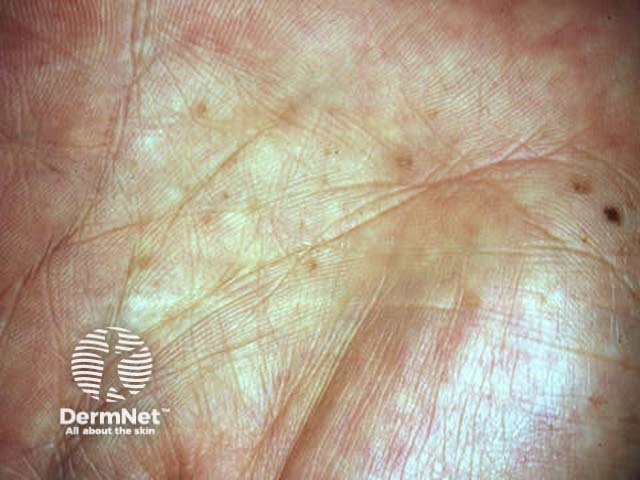
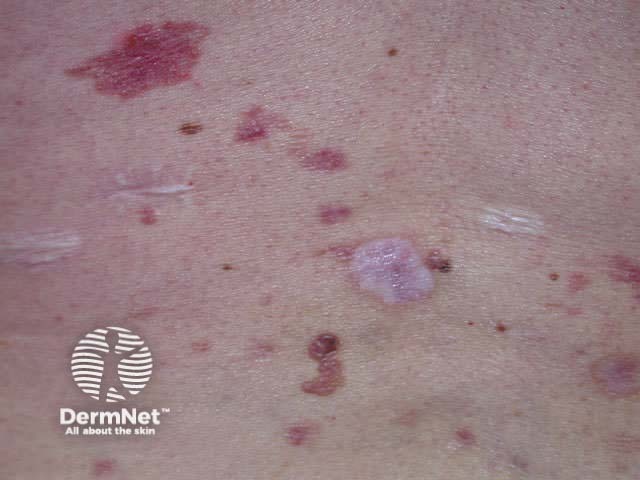
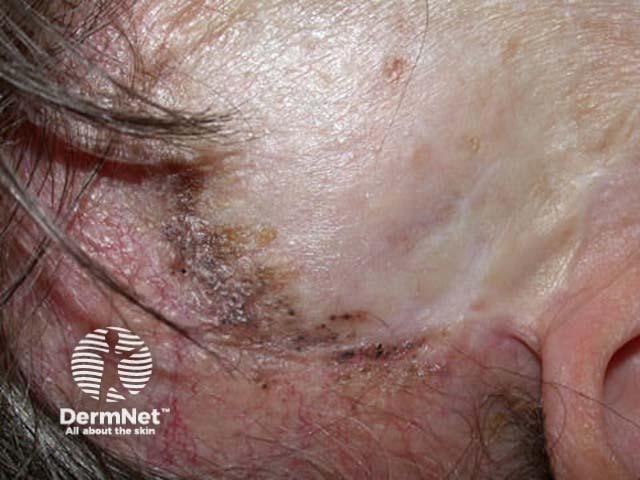
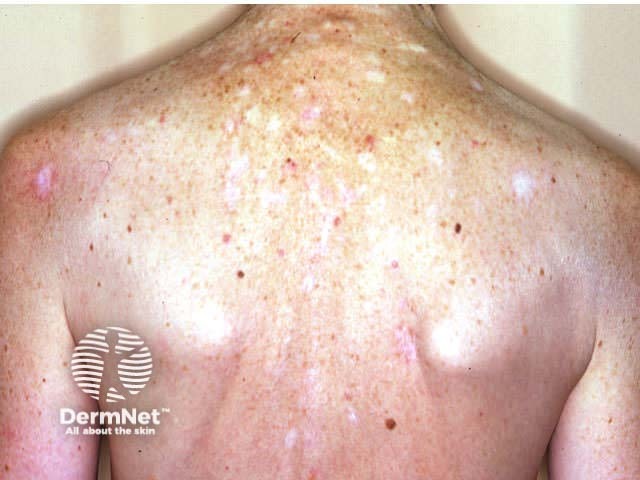
Multiple BCCs may also be related to excessive intake of arsenic, often in association with squamous cell carcinoma in situ (Bowen disease). Other individuals and families with multiple tumours may have other undetected genetic defects.
Basal cell carcinoma
Basal cell carcinoma
Basal cell carcinoma
Basal cell carcinoma
There are several clinical subtypes of basal cell carcinoma:
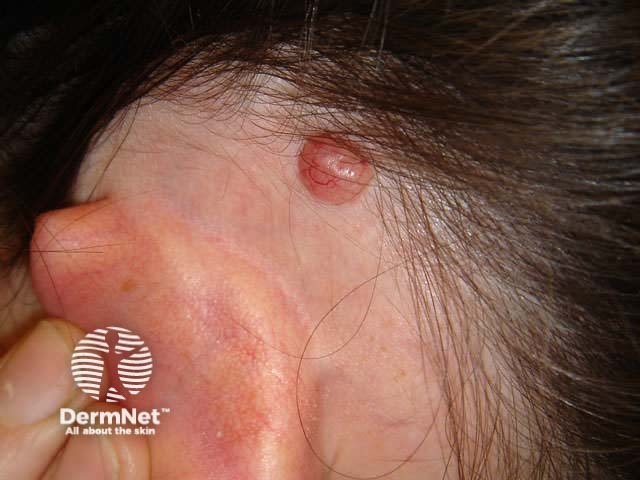
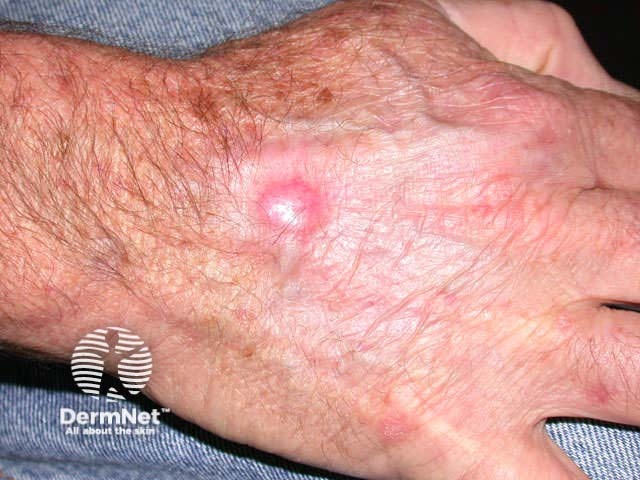
Nodular BCC presents as a slowly growing pearly nodule that may ulcerate. Linear telangiectasis may cross the lesion giving it a pink hue. There is frequently an elevated shiny border. It may be cystic; it is sometimes possible to express its gooey contents.
Nodular BCCs most often arise on the face, particularly on the forehead, temples, nose and upper lip. They are less common in sun-protected sites such as axillae, genitals and hair-bearing scalp. They rarely grow on mucosal surfaces.
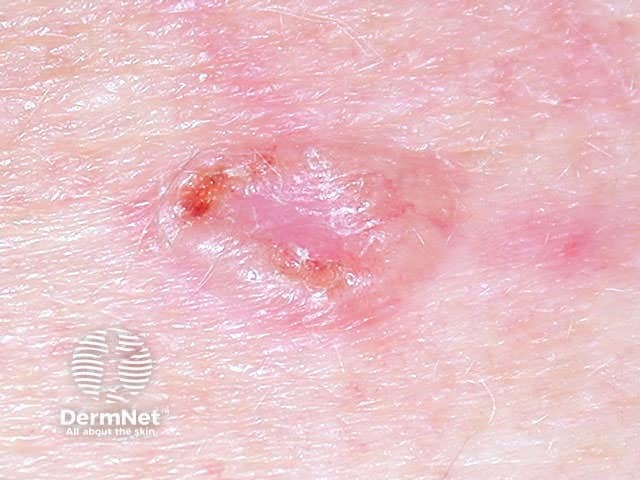
Basal cell carcinoma
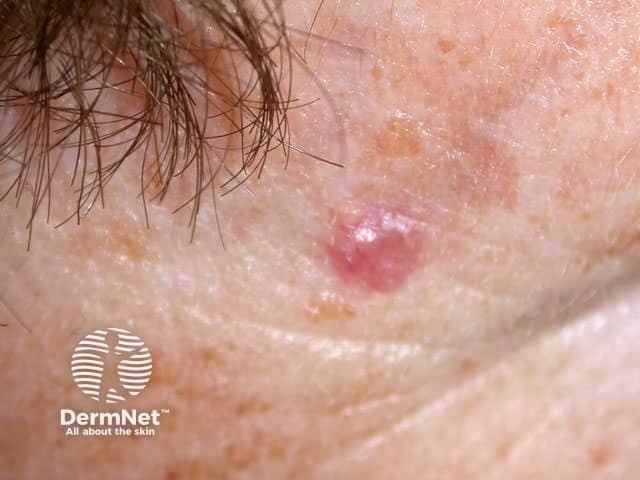
Basal cell carcinoma
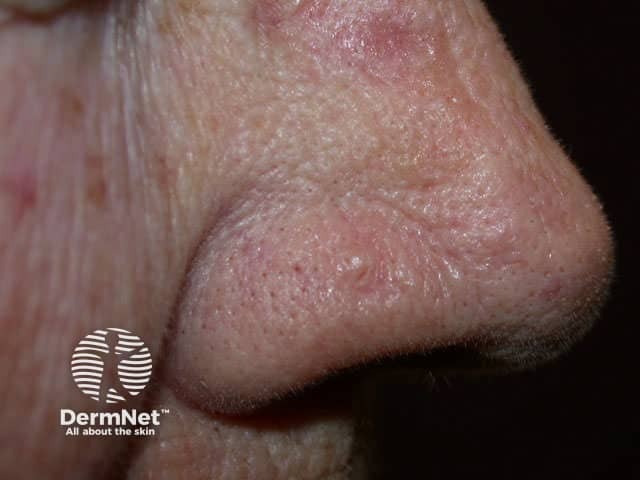
Basal cell carcinoma
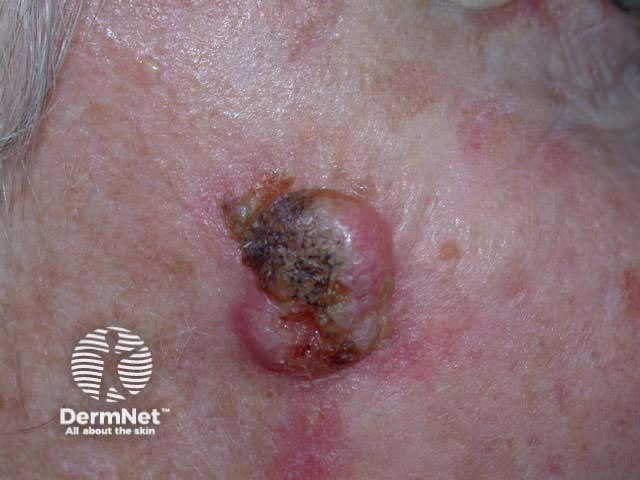
Basal cell carcinoma
Basal cell carcinoma
Basal cell carcinoma
Basal cell carcinoma
Basal cell carcinoma
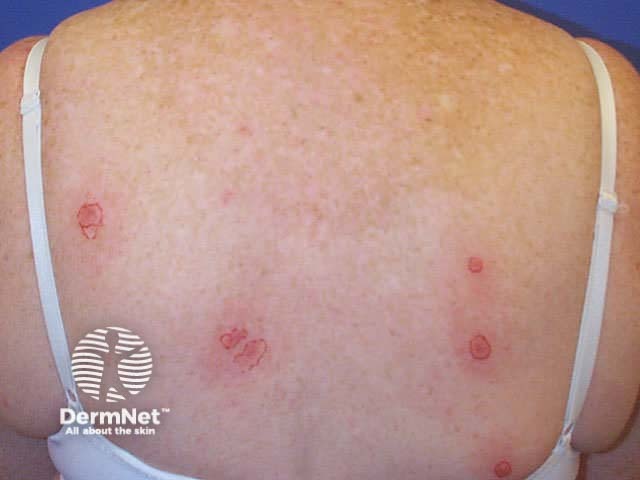
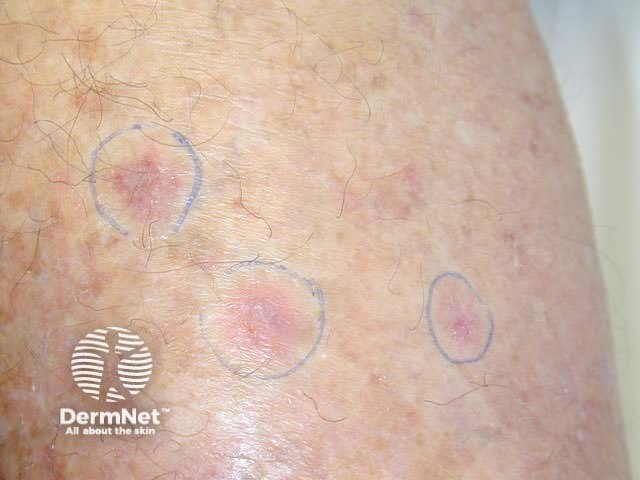
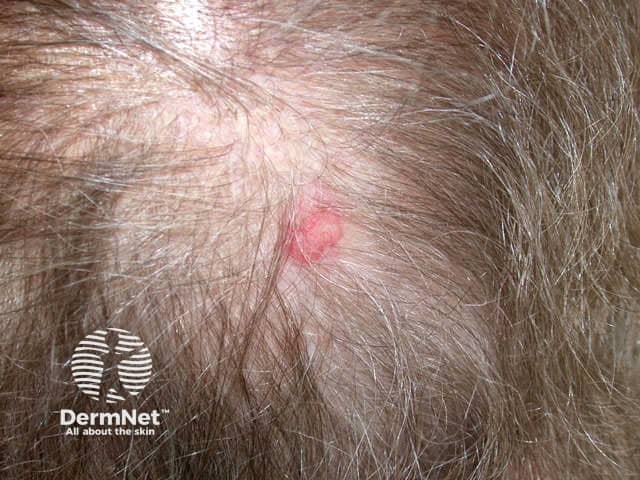
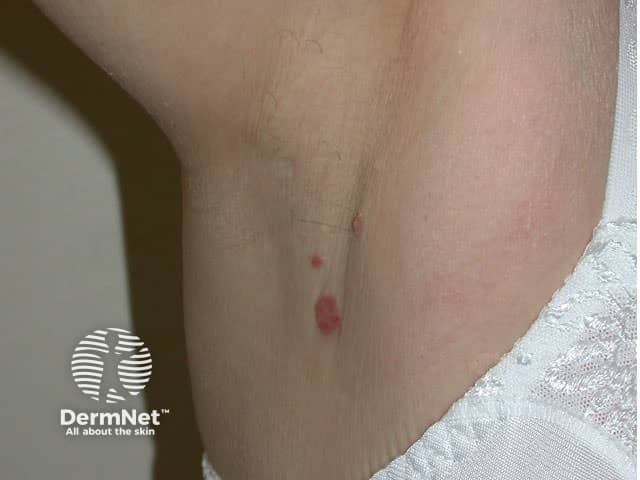
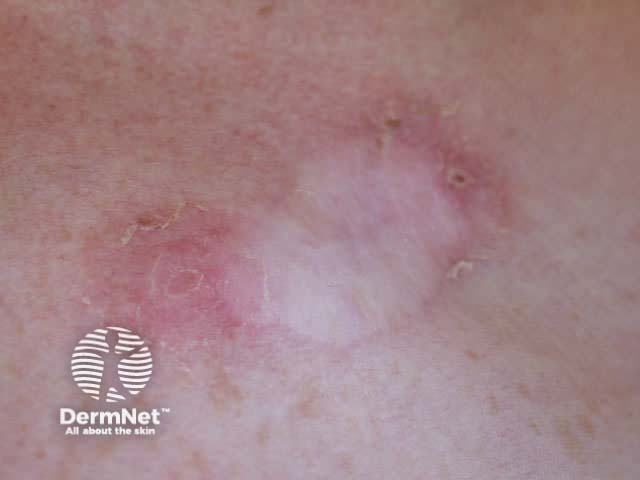
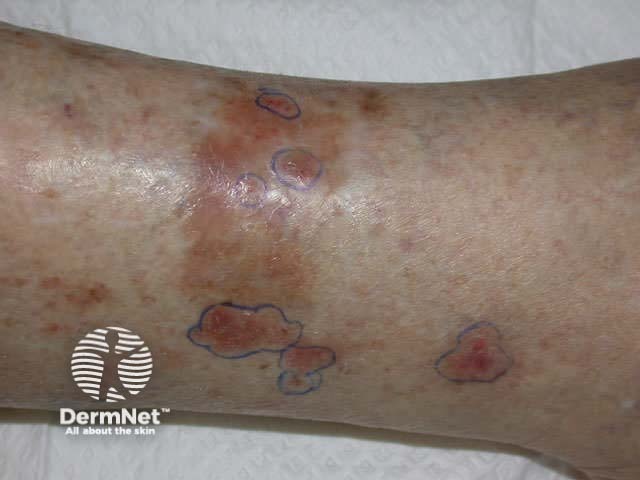
Superficial BCC presents as one or more often multiple, slowly growing thin erythematous plaques, with a slightly blue tinge. They are slightly dry or scaly and are often eroded and crusted. A shiny rim may be detected by stretching the affected skin. Pale or white areas are due to spontaneous regression. Superficial BCC may be difficult to distinguish from in situ SCC but the latter tends to be less blue and more dry or crusted.
Superficial BCC most often arise on the trunk and limbs. As they are usually asymptomatic and often unseen, patients frequently present with lesions that are several centimetres in diameter. They may be confused with dermatitis, psoriasis or tinea corporis. Sometimes, nodular BCC arises within superficial lesions.
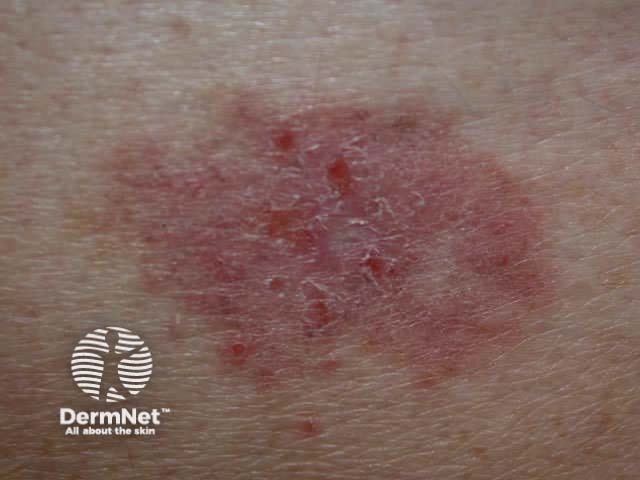
Basal cell carcinoma
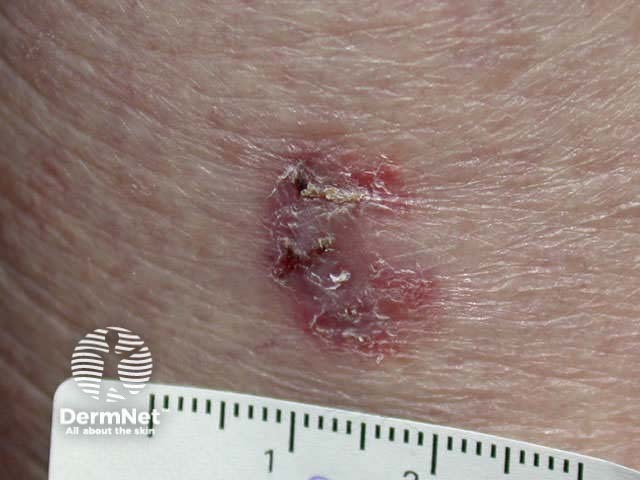
Basal cell carcinoma
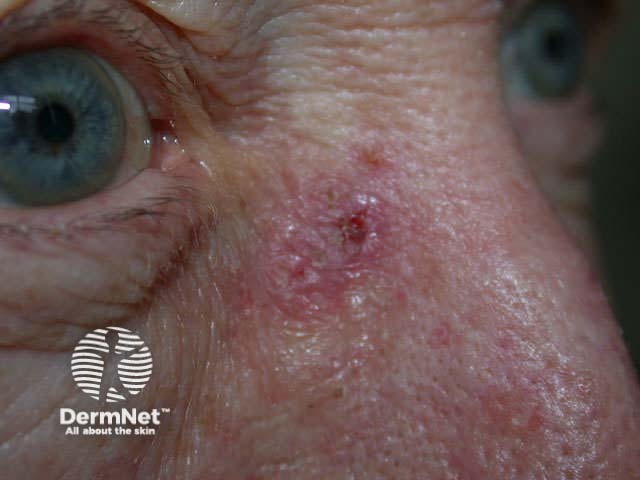
Basal cell carcinoma
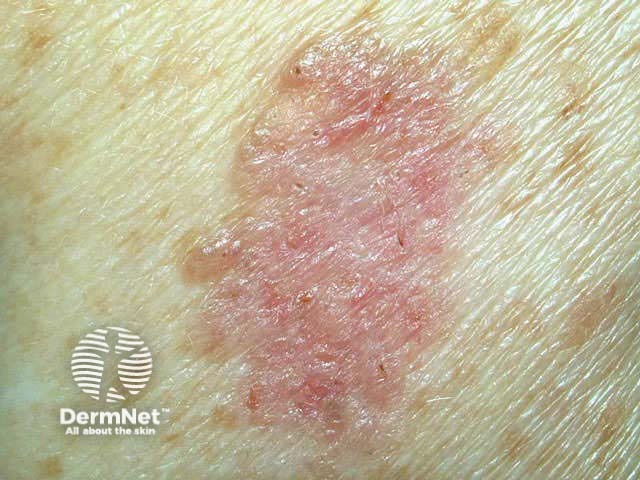
Basal cell carcinoma
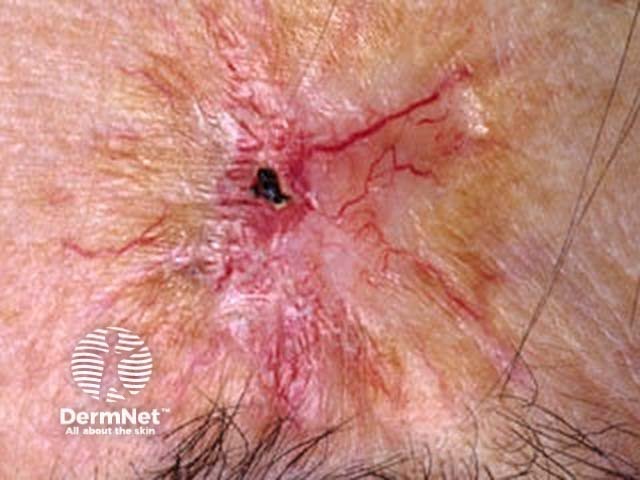
Morphoeic or sclerosing BCC is hard to identify (a scar-like plaque or dent) and often deeply invasive. It is most often found on the mid-face.
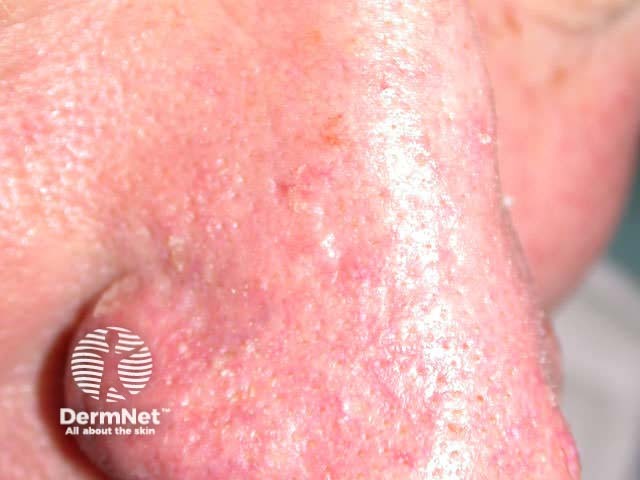
Basal cell carcinoma
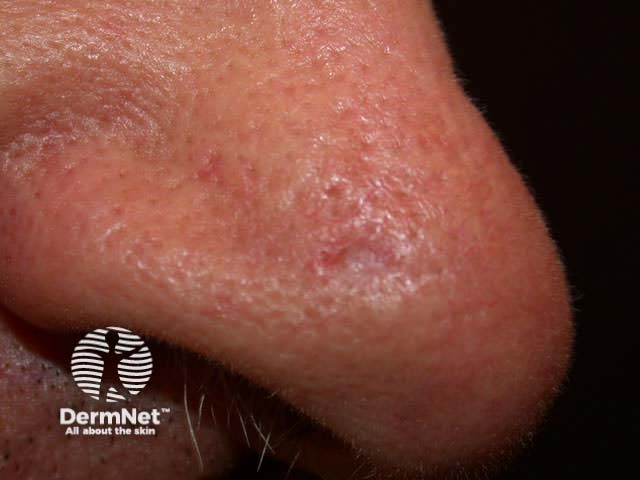
Basal cell carcinoma
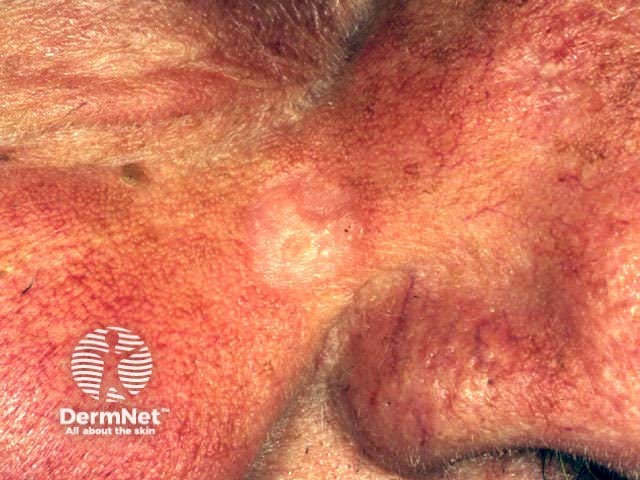
Basal cell carcinoma
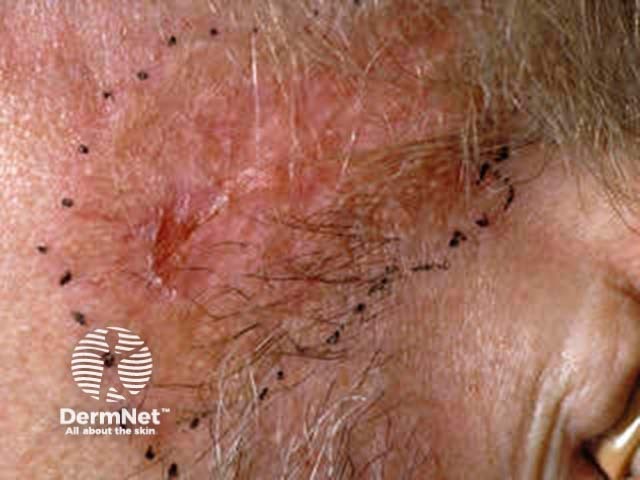
Basal cell carcinoma
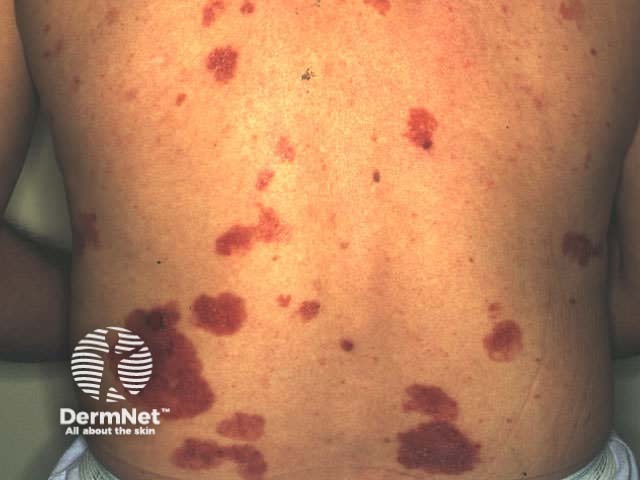
Pigmented BCC may appear similar to seborrhoeic keratosis or melanoma. It may be nodular or superficial in type. Dermoscopy is very useful to make a clinical diagnosis.
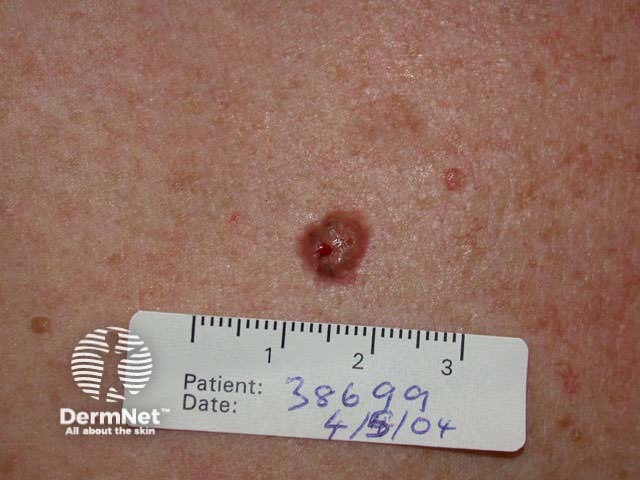
Basal cell carcinoma
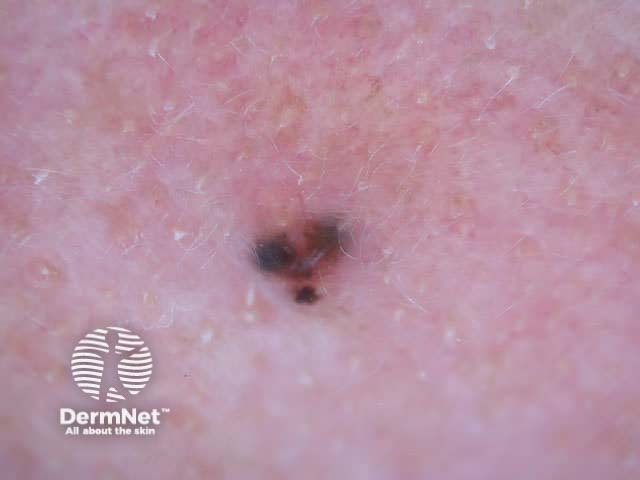
Basal cell carcinoma
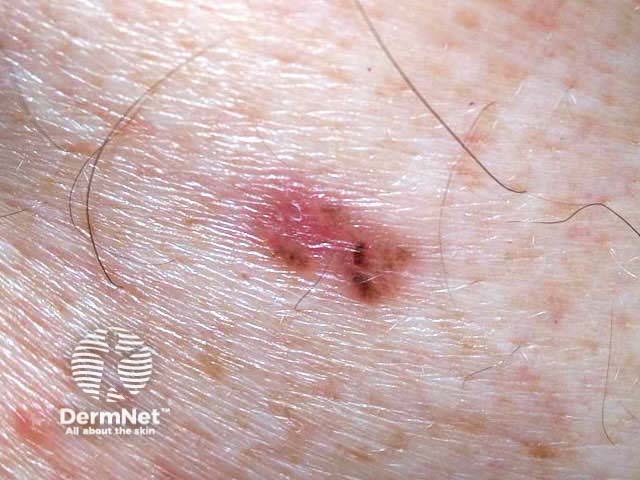
Basal cell carcinoma
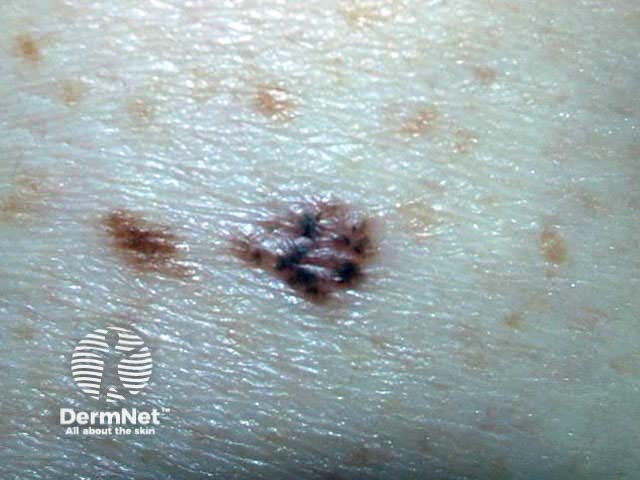
Basal cell carcinoma
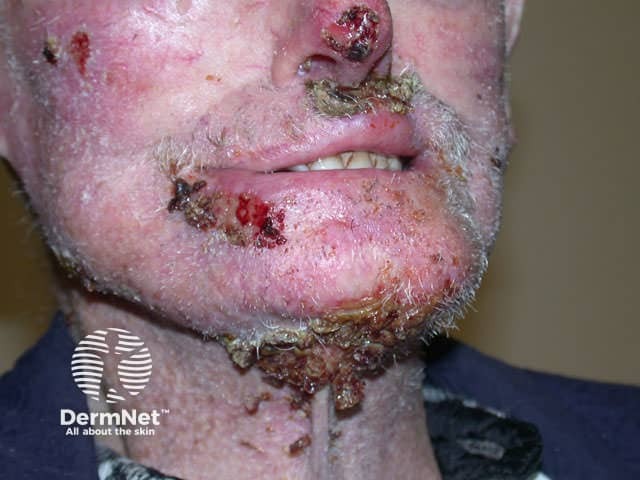
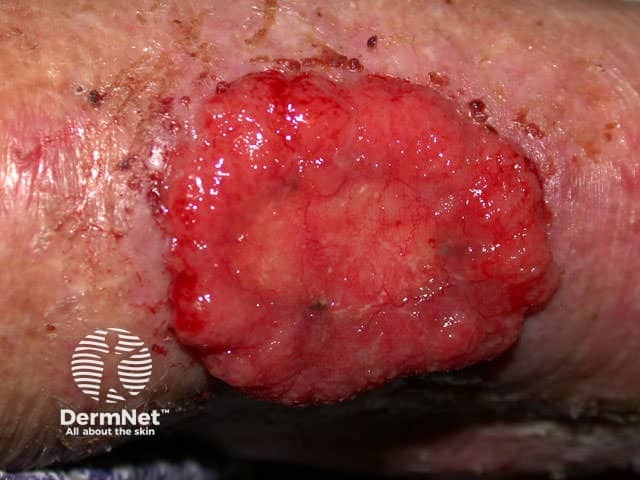
Any subtype of BCC may erode, when it may be called ‘rodent ulcer’.
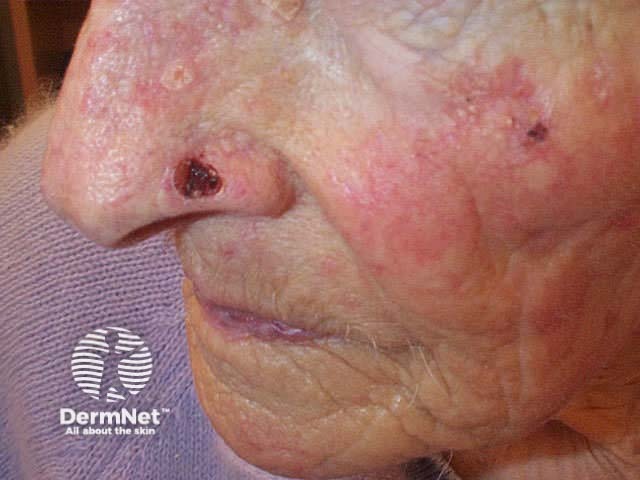
Basal cell carcinoma
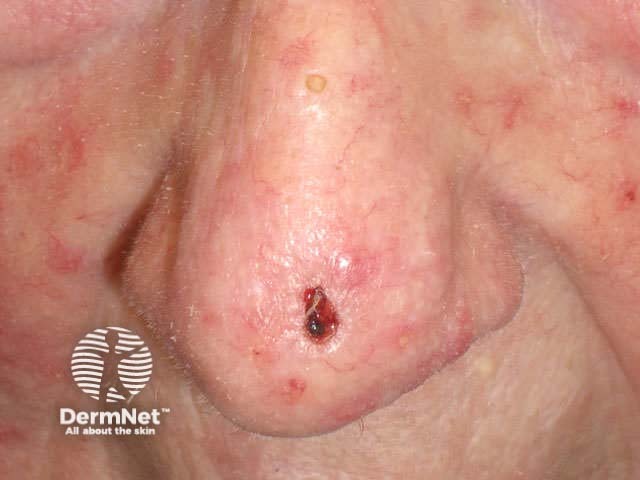
Basal cell carcinoma
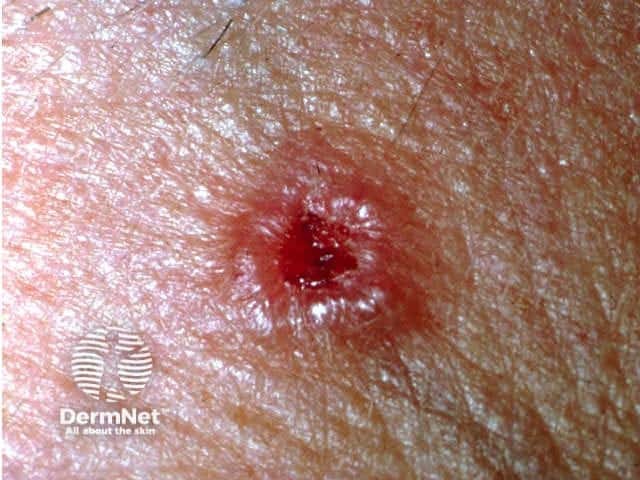
Basal cell carcinoma
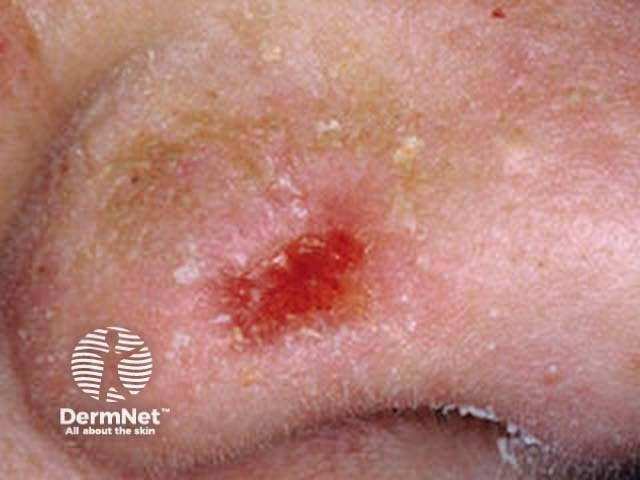
Basal cell carcinoma
Recurrent BCC presents late if arising from the base of the lesion, but marginal recurrence is usually visible within 6 to 12 months.
Basal cell carcinoma
Basal cell carcinoma
Basal cell carcinoma
Basal cell carcinoma
The features that distinguish BCC from other tumours include:
Histological subtypes also include:
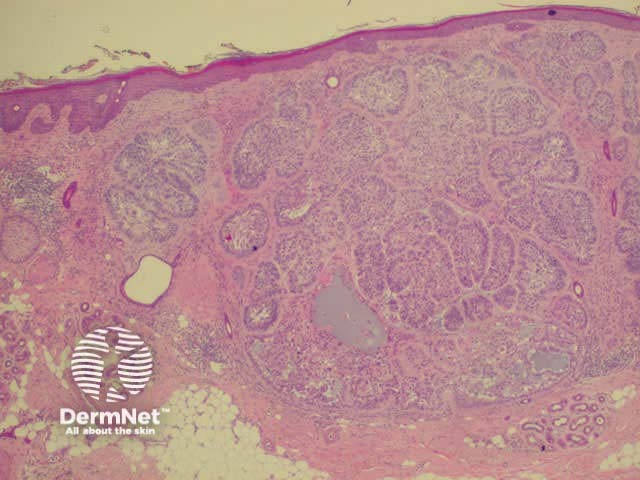
Histology of basal cell carcinoma
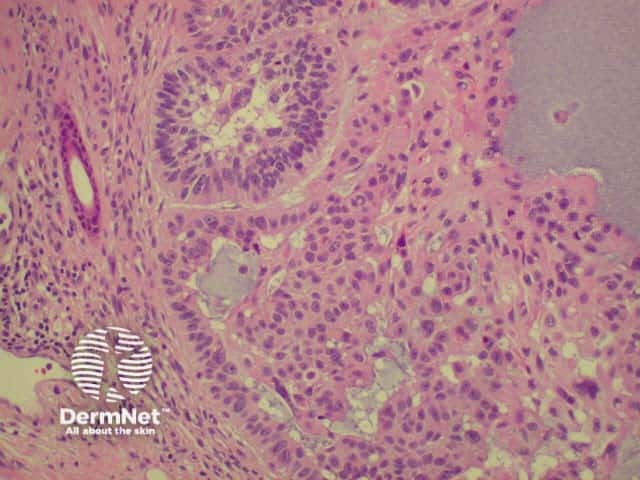
Histology of basal cell carcinoma
Management of basal cell carcinoma depends on:
The treatment may also depend on the convenience of the treatment; the age, finances and desire of the patient; and the training and expertise of the doctor.
Site of the lesion
Lesions affecting the mid-face or ears have an increased chance of recurrence because of clinical subtype, difficulty in determining margins and the tendency to narrow margins to reduce the deformity caused by surgery. The risk of recurrence is greatest on and around the eyelids, nose and mouth. A balance must be struck between the desire for excellent cosmesis and the risk of recurrence.
Healing is slow on the lower legs, where it is often difficult to obtain primary closure. Even small full thickness lesions may require skin grafting for repair. To avoid chronic leg ulceration, non-surgical options may be desirable.
Cosmesis is less important, and healing more straightforward, on the trunk and proximal limbs. Cost and convenience may be the deciding factor in these sites.
Clinical subtype
Morphoeic and micronodular subtypes are the most likely to recur after inadequate treatment as they are deeply infiltrating and margins are sometimes difficult to see clearly. A bright light and magnification is recommended. At present, excision with at least 3 to 4 mm margin is the recommended treatment for these lesions.
Well-demarcated nodulocystic and superficial BCC are readily treated by superficial treatment modalities.
Treatment suitable for BCC may include:
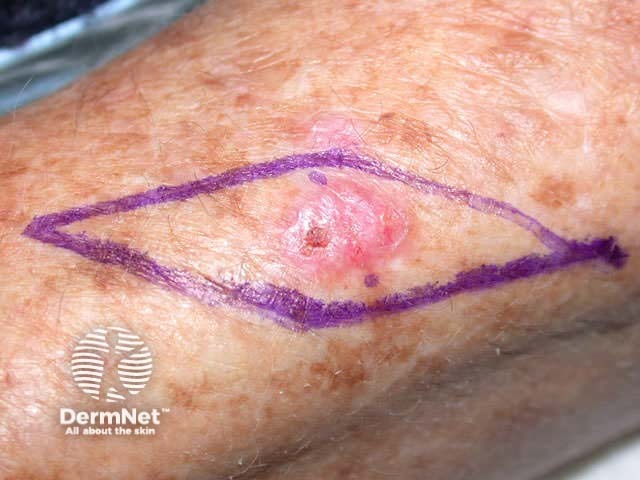
Excision
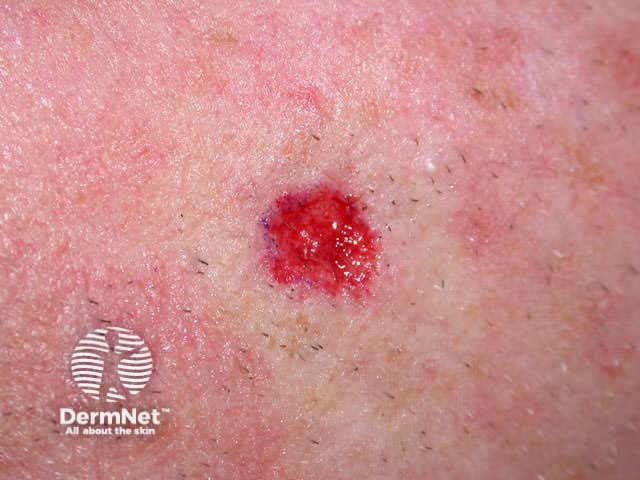
Curettage
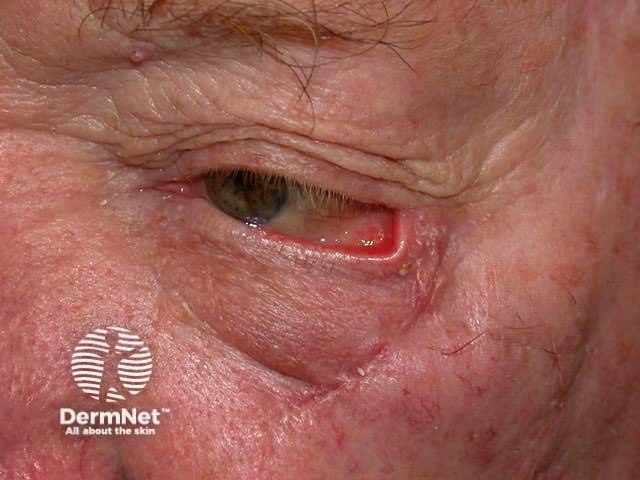
Ectropion due to excision
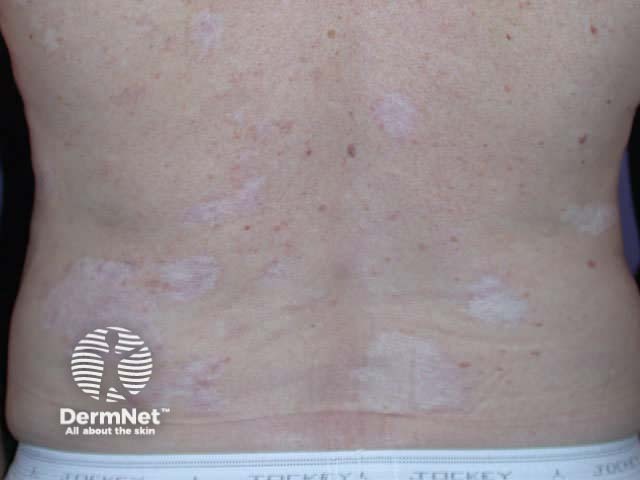
Cryotherapy marks
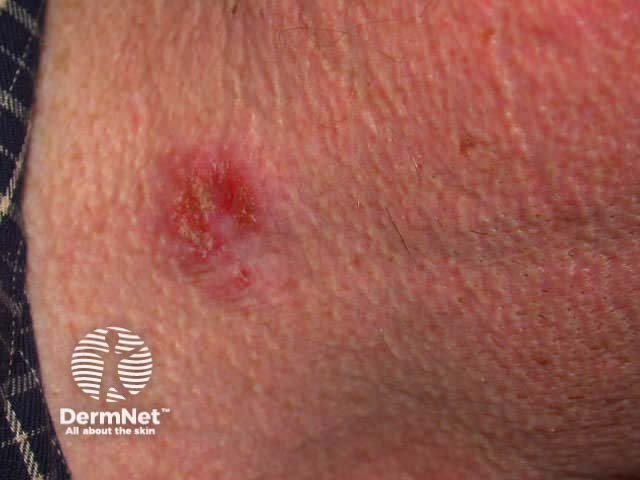
Erosion due to imiquimod
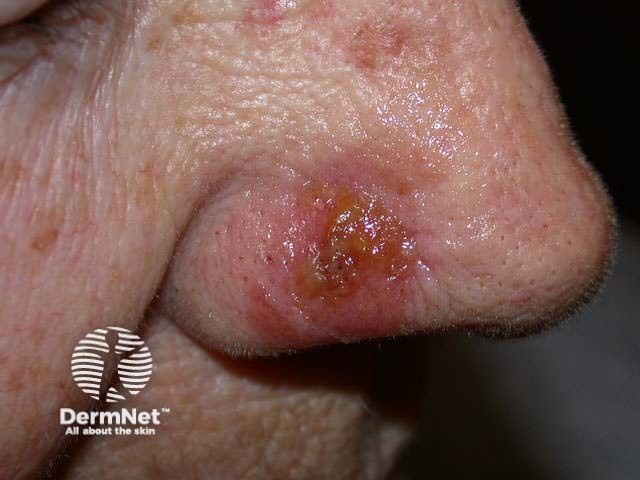
Crusting due to PDT
Fluorouracil cream results in low rates of cure but may sometimes be useful to control small superficial BCC.
The defect after removal of small or superficial lesions may be closed primarily and sutured, or left to heal by secondary intention (which results in a larger area of scarring). Larger lesions may require complex repair using flaps and grafts, by a specialist dermatologic or plastic surgeon.
What is the evidence that imiquimod is effective in the treatment of basal cell carcinoma? Through what mechanism?
Information for patients
See the DermNet bookstore.