Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Last Reviewed: April, 2025
Author: Dr Zoe Lee, MD, Flinders Medical Centre, Adelaide, Australia (2025)
Previous authors: Vanessa Ngan, Staff Writer, 2003; Hon Assoc Prof Amanda Oakley, Dermatologist, (2015)
Peer reviewed by: Dr Miranda Wallace, Department of Dermatology, Mater Hospital, Australia (2025)
Reviewing dermatologist: Dr Ian Coulson
Edited by the DermNet content department
Introduction
Demographics
Causes
Clinical features
Complications
Diagnosis
Differential diagnoses
Treatment
Outcome
Mucous membrane pemphigoid, also known as cicatricial pemphigoid, is an autoimmune blistering disease affecting mucous membranes (the oral cavity, ocular membranes, nasopharynx, and anogenital regions).
It may affect the skin in approximately 20–30% of patients. Blisters appear on the face, neck and scalp.
Brunsting Perry cicatricial pemphigoid is a rare variant affecting the head and neck. The blisters may burst resulting in blood-crusted plaques and scars.
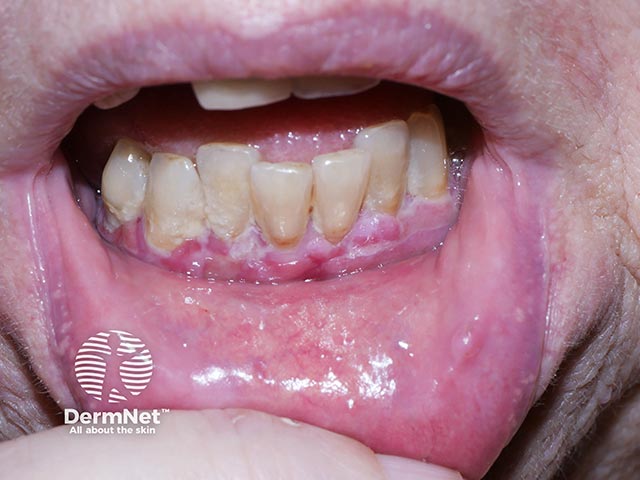
Gingival erosions due to MMP
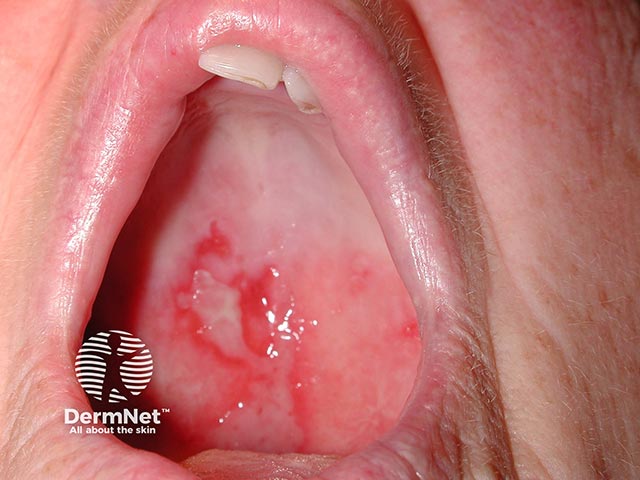
A palatal erosion due to MMP
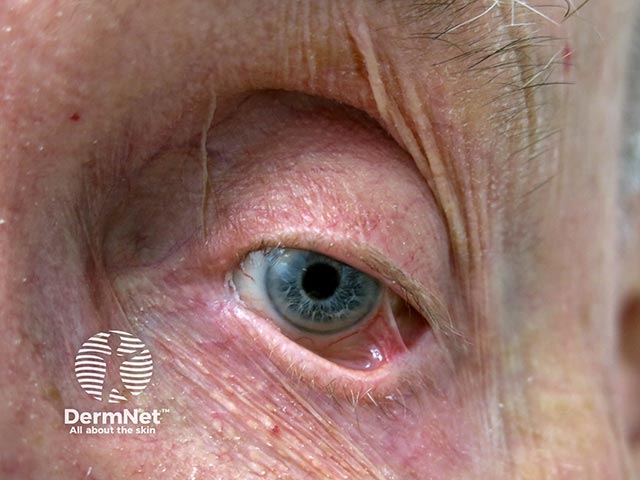
A synaechia of the conjunctiva due to MMP
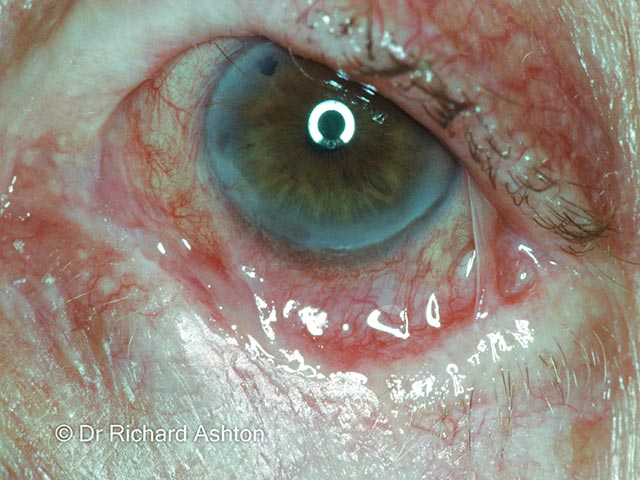
Conjunctival symblepharon due to MMP
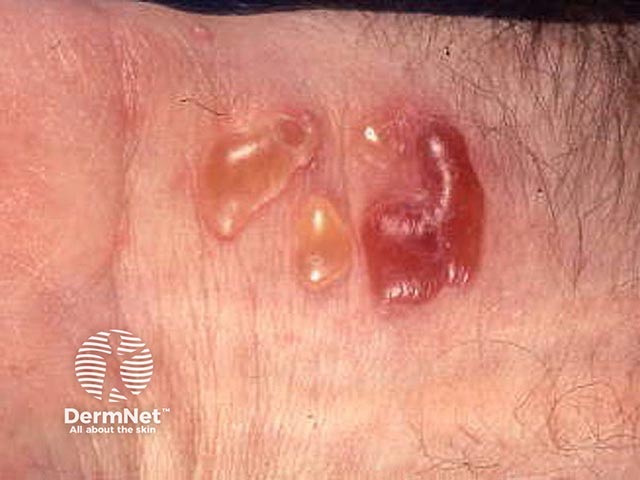
Cutaneous blisters in MMP - the mouth and eye were also affected
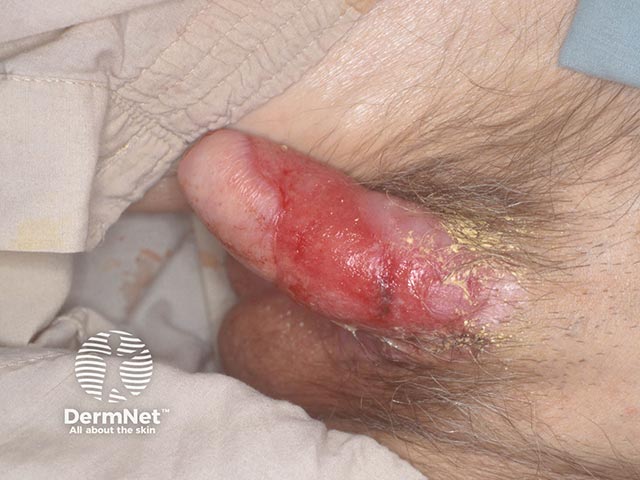
Penile erosions and scarring due to MMP
Mucous membrane pemphigoid has a reported incidence of approximately 1.3–2.0 cases per million people per year, with a larger incidence amongst females than males.
It is predominantly a disease of the elderly with a peak incidence at around 70 years of age. However, childhood cases have been reported.
MMP is an autoimmune blistering disease, involving an autoantibody attack of the basement membrane zone. Complement activation occurs, causing the migration of inflammatory cells into the upper lamina propria, resulting in degradation of the basement membrane. This results in subepidermal blisters.
The autoantibodies involved include collagen XVII, BP230, laminin 332, integrin α6/β4 and collagen VII. However, serological diagnosis is difficult as autoantibodies are usually in low titres and thus are not always revealed on testing.
Mucous membrane pemphigoid affects various mucosal sites with predilection for the oral cavity (85%) and ocular surfaces (65%) and may also affect the nasopharynx, larynx, oesophagus, genital regions and cutaneous sites.
Site |
Possible features |
|---|---|
Cutaneous (25–30% of patients) |
|
Oral (>85% of patients) |
|
Ocular (65% of patients) |
|
Nasal cavity (20–40%) |
|
Esophagus (5–15%) |
|
Anogenital (20% of patients) |
|
Severity of disease depends on site and extent of disease involvement. It can result in compromised airways due to tracheal strictures and threatened or complete vision loss due to conjunctival scarring. Risk-level stratification is often useful:
Severity of disease can be established through various scoring systems however, none currently available are validated. These scoring systems include the Mucous Membrane Pemphigoid Disease Area Index (MMPDAI), the Autoimmune Bullous Skin Disorder Intensity Score (ABSIS), the Oral Disease Severity Score (ODSS) and the Cicatrising Conjunctivitis Assessment Tool.
Sites |
Potential complications |
|---|---|
Ocular |
|
Oral |
|
Anogenital |
|
MMP is confirmed by biopsy of perilesional tissue by direct immunofluorescence (DIF) to detect IgG, IgA and complement C3 at the basement zone. Further blood analysis with indirect immunofluorescence and screening for laminin 332 autoantibodies may be performed.
Ocular mucous membrane pemphigoid is complex, with conjunctival DIF sensitivity ranging from 20% to 87%, lower than in extraocular sites due to lower autoantibody titres. Repeat biopsies of affected areas are recommended. In isolated ocular disease, diagnosis can be made even if DIF and serology are negative.
The primary aim of treatment is to stop blister formation, promote healing and prevent scarring. Mucous membrane pemphigoid is a particularly difficult disease to treat as it can affect so many different parts of the body.
Management often requires multidisciplinary input from multiple specialties depending on site and severity of symptoms.
Note: Topical treatment alone is appropriate in cases of mild, isolated oral mucous membrane pemphigoid. Consideration of short-term low-dose systemic corticosteroids may be considered as an adjuvant to topical treatments.
Mucous membrane pemphigoid is a chronic, progressive disease that responds slowly and often incompletely to treatment. Spontaneous remissions are rare. The condition may follow a relapsing and remitting course.
Appropriate follow-up is required to ensure management is optimised where possible.
Given the aggressive nature of ocular mucous membrane pemphigoid, the absence of treatment can result in complications such as visual impairment or complete blindness.