Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Amanda Saracino, Dermatologist, Alfred Health and Melbourne Dermatology Clinic, Melbourne, VIC, Australia. DermNet Editor-in-Chief A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. September 2017.
Introduction
Demographics
Causes
Clinical features
Morphology
Symptoms from morphoea
Diagnosis
Treatment
Monitoring treatment response
Natural history
Morphoea (American spelling, morphea) is characterised by an area of inflammation and fibrosis (thickening and hardening) of the skin due to increased collagen deposition. It is also known as localised scleroderma. The term 'scleroderma' covers various types of morphoea and systemic sclerosis.
Subtypes of morphoea vary according to the location of involved skin. Any subtype of morphoea can also result in deep or subdermal involvement of the underlying fat, fascia, muscle, or bone.
Unlike systemic sclerosis, morphoea does NOT cause:
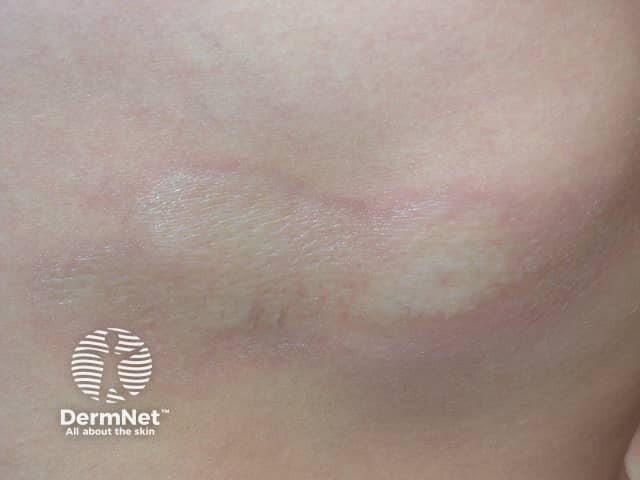
Morphoea
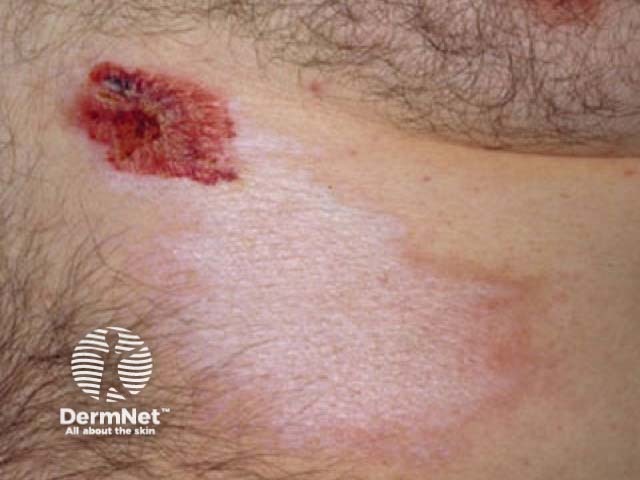
Morphoea
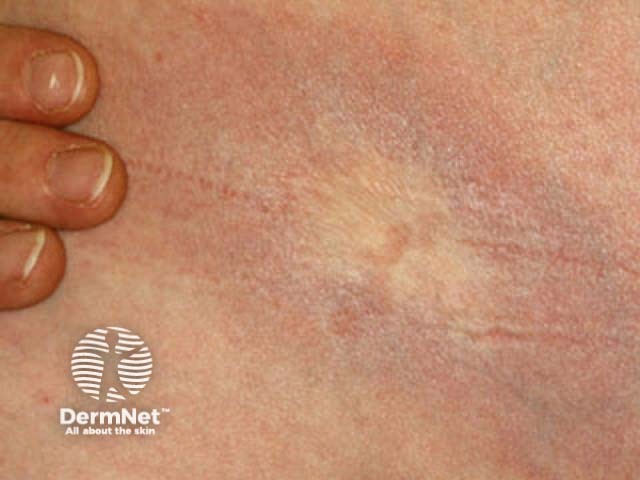
Morphoea
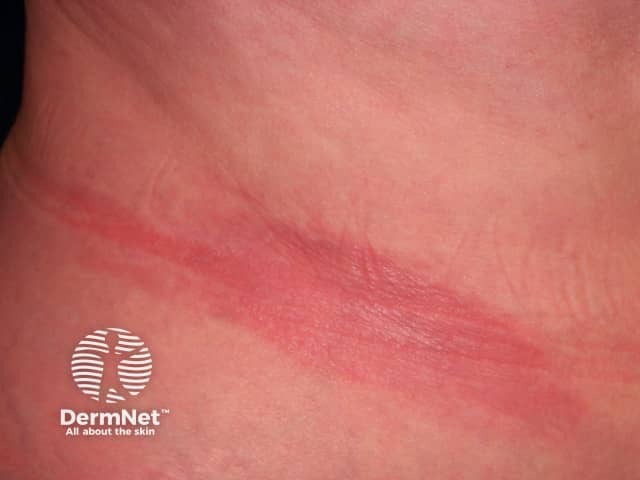
Morphoea
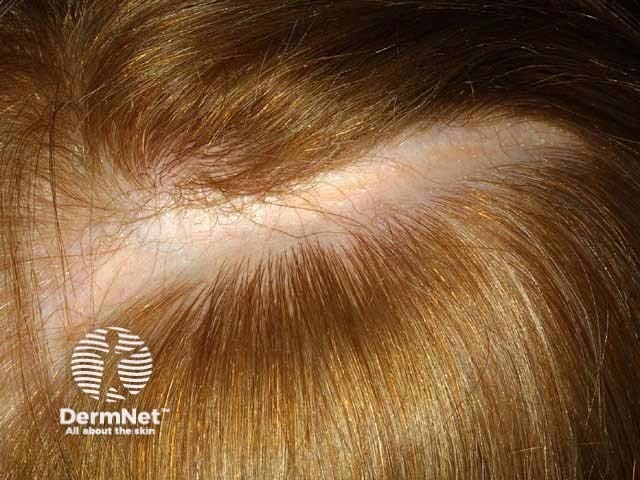
Morphoea
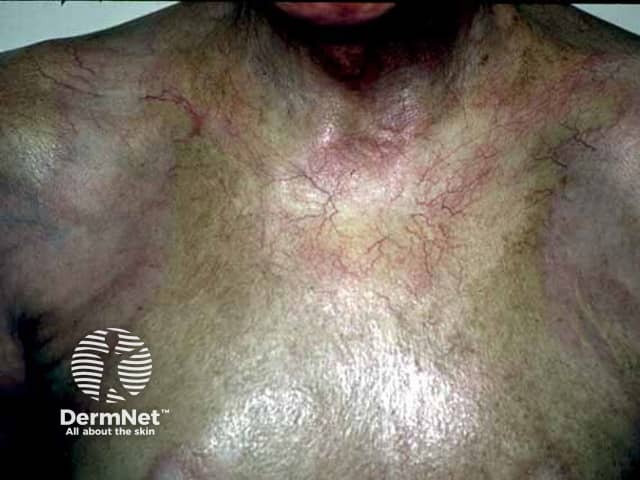
Morphoea
Morphoea is rare and is estimated to have an incidence of 1–3 per 100,000 children. It is three times more common in females compared to males and often begins in childhood. Although not an inherited disorder, certain HLA subtypes (HLA-DRB1*04:04 and HLA-B*37) are associated with an increased risk of morphoea.
The precise cause of morphoea is unknown.
For unknown reasons, morphoea often develops after an external trigger such as:
Trauma-related morphoea may occur at the affected site, or at unrelated distant sites.
When describing morphoea, consider three features.
Subtypes of morphoea are limited, linear, generalised or mixed.
Rare types of limited plaque morphoea include guttate morphoea and atrophoderma of Pasini and Pierini.

Morphoea

Morphoea

Morphoea
See more images of morphoea ...
Linear atrophoderma of Moulin is a rare subtype of atrophic and pigmented linear morphoea.
Craniofacial linear morphoea was previously sub-classified as:
These types of craniofacial linear morphoea occur together and vary based on morphology and depth of tissue involvement.

Morphoea
See more images of morphoea ...
Generalised morphoea affects three or more body sites. There are two major patterns;

Morphoea
See more images of morphoea ...
Mixed pattern morphoea
Limited morphoea is considered mild, while linear morphoea and generalised morphoea are more severe subtypes. The depth of tissue involvement is also important when assessing disease severity; subdermal involvement implies more severe disease.
The specific appearance of morphoea varies, and may include:
Morphoea classically passes through each of these morphological stages, this does not always occur.
Any subtype of morphoea can affect connective tissue under the skin, such as the fat, fascia, muscle, bone, joints, or rarely brain (in craniofacial linear morphoea). Deep tissue involvement is a marker of severe disease.
When the fascia (the connective tissue under the fat layer) is involved:
Involvement of bones or joints results in loss of bony tissue, pain and/or restricted joint movement (contractures).
Eosinophilic fasciitis is a form of pansclerotic morphoea with deep fascial involvement. Circumferential inflammation and sclerosis of the fascia (the connective tissue beneath the fat) frequently co-exists with overlying dermal sclerosis or other anatomical subtypes of morphoea indicating it is debatable whether it should be considered a separate condition.
Morphoea may be asymptomatic, or symptoms may arise from the skin or deeper tissues, or they may due to extracutaneous manifestations.
Up to 30% of patients with more severe types of linear or generalised morphoea can have extracutaneous non-specific inflammatory symptoms. These include:
These extracutaneous manifestations imply that morphoea is a systemic inflammatory condition. In contrast, systemic sclerosis results in direct damage and fibrosis of the lungs, heart, kidneys, and/or gastrointestinal tract — which do not occur in morphoea.
The diagnosis of morphoea is often made clinically, without the need for further tests. Biopsy, blood tests and imaging may be undertaken if the diagnosis or extent of disease is unclear.
A skin biopsy enables the skin, subcutaneous fat (and sometimes fascia) to be examined under the microscope. Classic findings in morphoea include:
Magnetic resonance imaging (MRI) may be performed to assess how deep the morphoea extends beyond the skin, for example in generalised morphoea, linear morphoea crossing joints, and craniofacial linear morphoea.
There is no cure for morphoea. Treatment is aimed at halting ongoing disease activity and progression.
Topical therapy may help limited and superficial forms of morphoea and can reduce the itch.
Phototherapy can soften morphoea and has anti-inflammatory effects.
Different wavelengths of ultraviolet radiation can be used.
Systemic treatment is intended to prevent progression and switch off the active disease process. It is usually needed for at least 2 to 4 years, but relapse can occur.
Specific treatment decisions in morphoea are guided by the subtype of morphoea and its severity.
Other options
Physiotherapy to improve joint mobility should be undertaken with caution in active morphoea, as the resultant trauma may potentially act as an ongoing disease trigger.
In some cases, surgery may be of benefit, such as autologous fat transfer, to improve atrophy.
Disease progression and treatment response can be monitored using photographs, the localized scleroderma cutaneous assessment tool(LoSCAT) and other highly specialised tests, such as infrared thermography.
LoSCAT is a validated tool used to assess disease activity and damage over time. It assesses 16 body sites and includes two LS domains.
Scoring for mLoSSI
Scoring for the LoSDI
Morphoea can follow a protracted course, which can be relapsing and remitting, or chronically active. Milder forms of the disease tend to become inactive within 3–5 years.
Relapse can occur after successful treatment, especially in morphoea that begins in childhood.
Extended courses of systemic treatments of 4 to 5 years or more may be required to minimise the risk of relapse.