Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Vanessa Ngan, Staff Writer, 2006. Updated by A/Prof Amanda Oakley, February 2016.
Introduction
Demographics
Causes
Clinical features
Diagnosis
Treatment
A lentigo is a pigmented flat or slightly raised lesion with a clearly defined edge. Unlike an ephelis (freckle), it does not fade in the winter months. There are several kinds of lentigo.
The name lentigo originally referred to its appearance resembling a small lentil. The plural of lentigo is lentigines, although “lentigos” is also in common use.
Lentigines can affect males and females of all ages and races. Solar lentigines are especially prevalent in fair skinned adults. Lentigines associated with syndromes are present at birth or arise during childhood.
Common forms of lentigo are due to exposure to ultraviolet radiation:
Ionising radiation, eg radiation therapy, can also cause lentigines.
Several familial syndromes associated with widespread lentigines originate from mutations in Ras-MAP kinase, mTOR signalling and PTEN pathways.
Lentigines have been classified into several different types depending on what they look like, where they appear on the body, causative factors, and whether they are associated to other diseases or conditions.
Lentigines may be solitary or more often, multiple. Most lentigines are smaller than 5 mm in diameter.
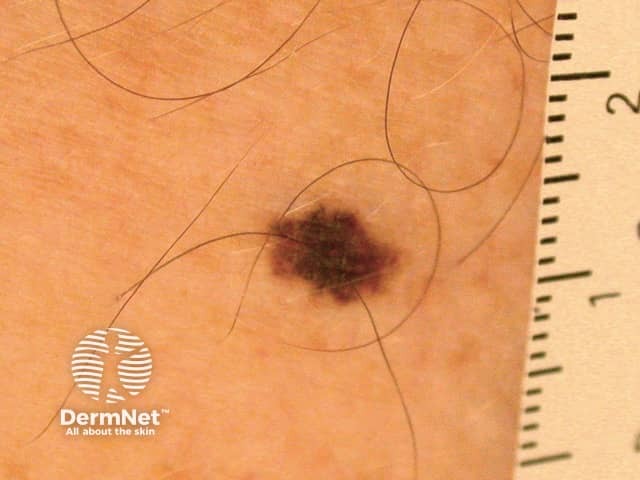
Lentigo simplex
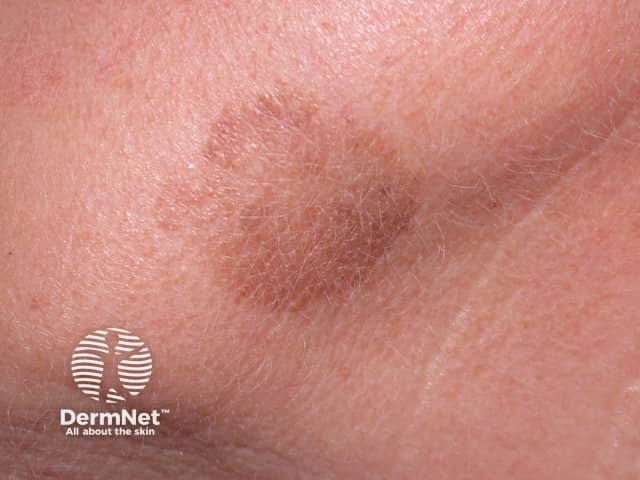
Solar lentigo

Ink spot lentigo
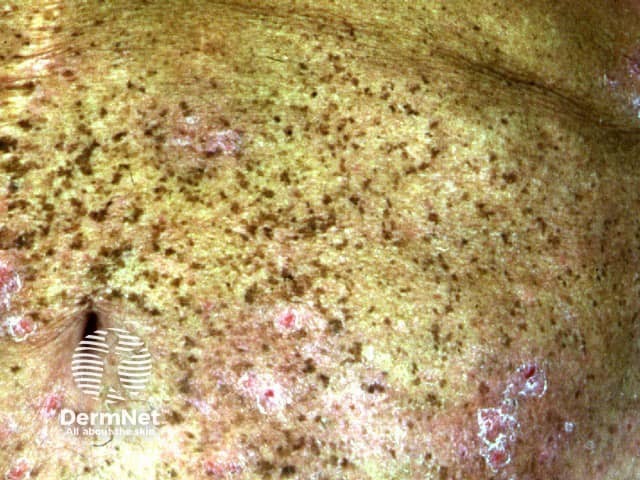
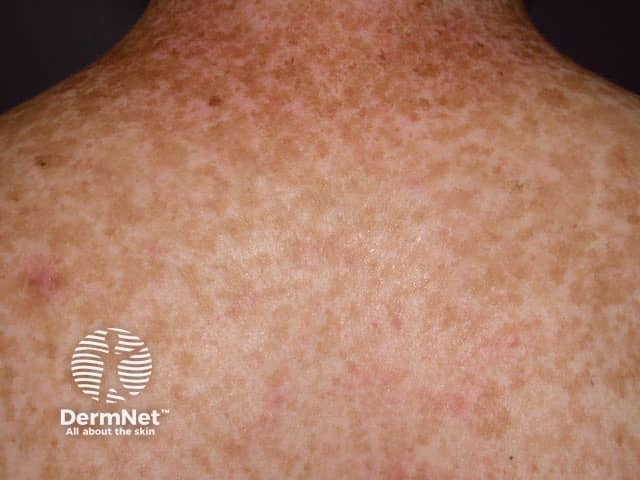
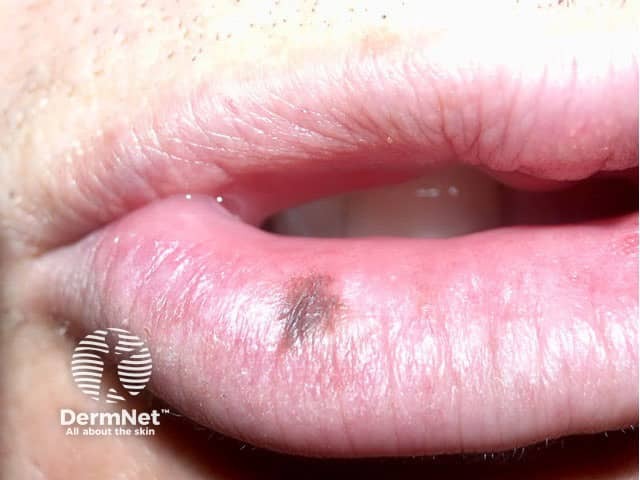
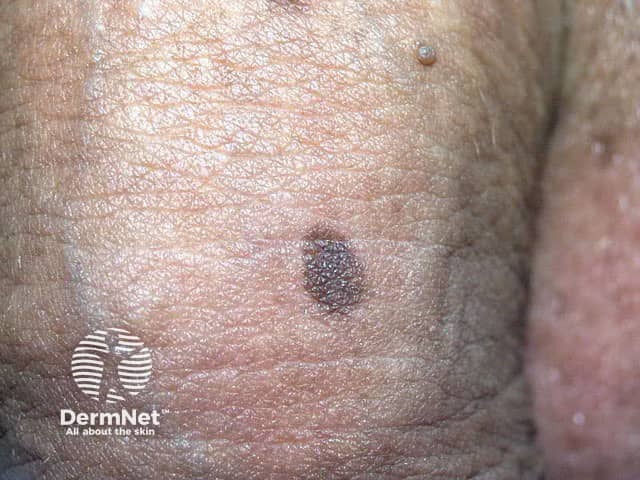
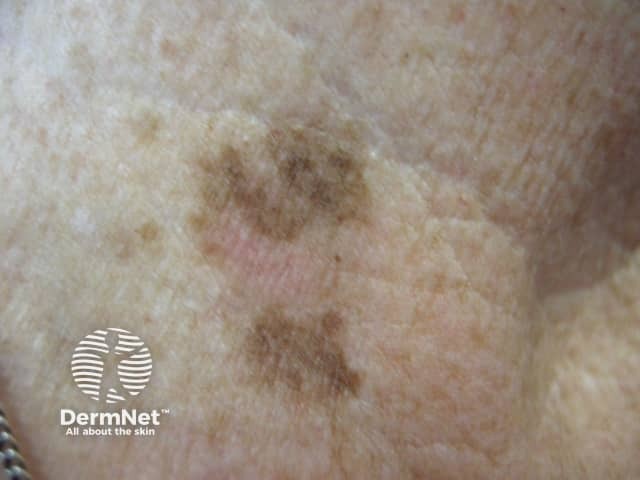
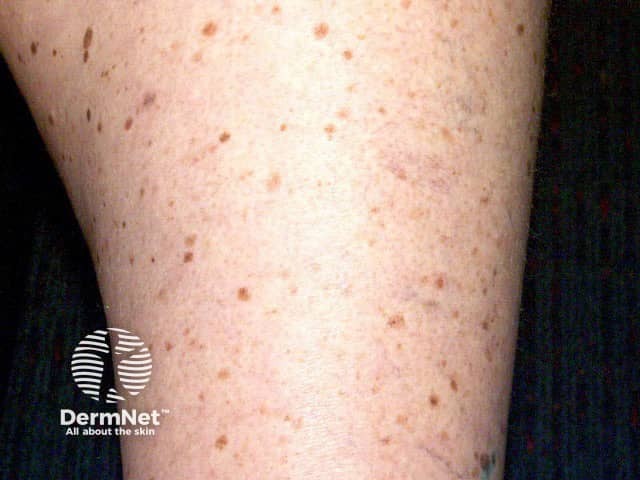
See more images of lentigines ...
Lentigines are usually diagnosed clinically by their typical appearance. Concern regarding possibility of melanoma may lead to:
Histopathology of a lentigo shows:
In contrast, an ephelis (freckle) shows sun-induced increased melanin within the keratinocytes, without an increase in number of cells.
Most lentigines are left alone. Attempts to lighten them may not be successful. The following approaches are used:
Individual lesions can be permanently removed using:
Lentigines associated with exposure ultraviolet radiation can be prevented by very careful sun protection. Clothing is more successful at preventing new lentigines than are sunscreens.
Lentigines usually persist. They may increase in number with age and sun exposure. Some in sun-protected sites may fade and disappear.