Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Amanda Oakley, Dermatologist, Hamilton New Zealand, in 1997. Updated in January 2016.
Credit: Many images have been supplied by MoleMap NZ.
Introduction
Demographics
Causes
Clinical features
Classification
Complications
Diagnosis
Treatment
Prevention
Outlook
A melanocytic naevus (American spelling ‘nevus’), or mole, is a common benign skin lesion due to a local proliferation of pigment cells (melanocytes). It is sometimes called a naevocytic naevus or just 'naevus' (but note that there are other types of naevi). A brown or black melanocytic naevus contains the pigment melanin, so may also be called a pigmented naevus.
A melanocytic naevus can be present at birth (a congenital melanocytic naevus) or appear later (an acquired naevus). There are various kinds of congenital and acquired melanocytic naevi (American spelling 'nevi').
Almost everyone has at least one melanocytic naevus.
Most white-skinned New Zealanders have 20–50 melanocytic naevi.
Although the exact reason for the local proliferation of naevus cells is unknown, it is clear that the number of melanocytic naevi a person has depends on genetic factors, on sun exposure, and on immune status.
Melanocytic naevi vary widely in clinical, dermatoscopic and histological appearance.
Congenital melanocytic naevi are classified according to their actual or predicted adult size in maximum dimension and on specific characteristics.
Small congenital naevus |
Medium congenital naevus |
Giant naevus |
Hairy congenital naevus |
|---|---|---|---|
Small congenital naevus is 1.5 cm diameter. |
Medium congenital naevi are 1.5–19.9 cm diameter. |
A large or giant congenital melanocytic naevus is ≥ 20 cm |
Hairy congenital naevi grow thick long hairs. |

|

|

|

|
Café au lait macule |
Speckled lentiginous naevus |
Naevus of Ota |
Mongolian spot |
|---|---|---|---|
Café au lait macule is a flat brown patch. |
Speckled lentiginous naevus is a flat brown patch with darker spots. |
Naevus of Ota is a bluish brown mark around forehead, eye and cheek. |
Mongolian spot is a large bluish mark most often seen on buttocks of a newborn. |

|

|

|
|
The pathological classification of melanocytic naevi relates to where naevus cells are found in the skin.
Junctional naevus |
Dermal naevus |
Compound naevus |
Combined naevus |
|---|---|---|---|
A junctional naevus has groups or nests of naevus cells at the junction of the epidermis and the dermis. A flat mole. |
A dermal or intradermal naevus has naevus cell nests in the dermis. A papule, plaque or nodule with a pedunculated, papillomatous (Unna naevus) or smooth surface (Miescher naevus). |
A compound naevus has nests of naevus cells at the epidermal-dermal junction as well as within the dermis. A central raised area surrounded by a flat patch. |
A combined naevus has two distinct types of mole within the same lesion – usually blue naevus and compound naevus. |

|

|

|

|
Dermatoscopy has given rise to a new classification based on the pigment patterns of melanocytic naevi. Examples include:
Reticular naevus |
Globular naevus |
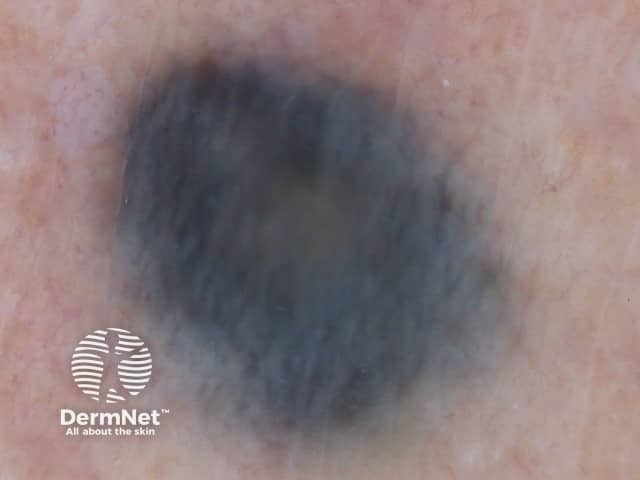
Blue naevus |
Starburst naevus |
|---|---|---|---|
Reticular naevus reveals a lattice of intersecting brown lines. |
Globular naevus characteristically shows aggregated brown oval structures. |
The blue naevus is a uniform structureless lesion, steel blue in colour. |
Starburst naevus reveals radial lines around the periphery of the lesion. |

|

|
|

|
Site-related naevus: facial |
Site-related naevus: acral |
Naevus with special features |
Unclassifiable naevus |
|---|---|---|---|
Facial naevi reveal pseudonetwork around hair follicles |
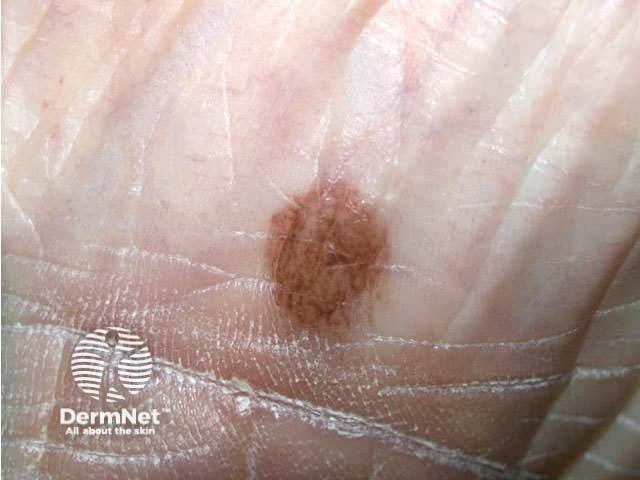
Acral naevi (these are on palms and soles) tend to be made up of parallel lines. |
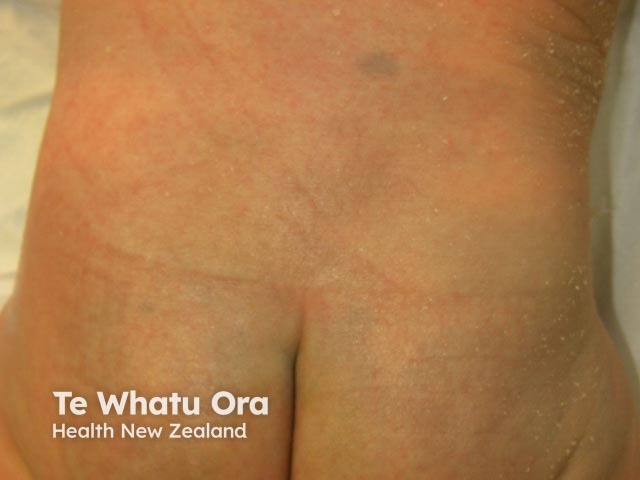
Naevi with special features include eczematised naevus (illustrated), irritated naevi and halo naevi. |
The unclassifiable naevus doesn't have any of the other patterns. |

|

|

|

|
Ordinary moles that appear after birth may be referred to as acquired naevi. Acquired melanocytic naevi are given a variety of names and there is considerable overlap of descriptions.
Signature naevi are the predominant group of naevi in an individual with multiple moles.
Solid brown naevus |
Solid pink naevus |
Eclipse naevus |
Cockade naevus |
|---|---|---|---|
Solid brown naevi have uniform brown pigmentation. |
Solid pink naevi are seen in fair-skinned individuals and lack melanin pigmentation. |
Eclipse naevus has a ring, or segment of a ring, of darker pigment around a tan or pink centre. Often found in the scalp. |
Cockade, or naevus en cocarde/cockade, has a central dark naevus surrounded by concentric circles of light and dark pigmentation like a rosette. |

|

|

|

|
Naevus with perifollicular hypopigmentation |
Fried-egg naevus |
Lentiginous naevus |
Naevus with eccentric pigmentation |
|---|---|---|---|
Naevi with perifollicular hypopigmentation have white spots around each hair. Easier to see by dermoscopy. |
Fried-egg naevus is a compound naevus with a flat rim of pigment around a bumpy central portion – the bump can be lighter or darker than the pigmented rim. |
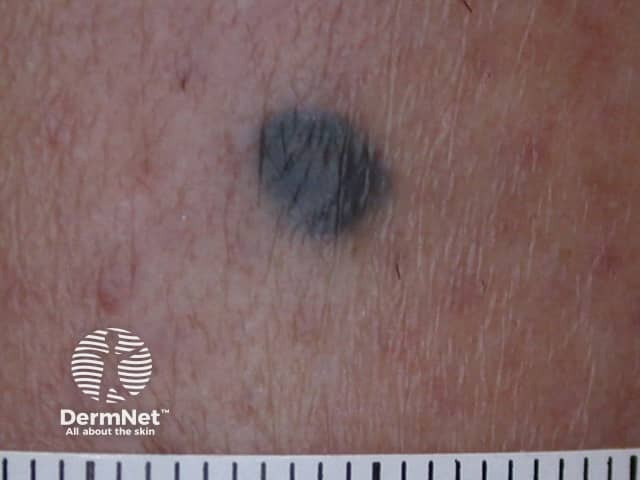
Lentiginous naevi are small, dark brown or black, flat lesions, often with a slightly paler rim – people with multiple lentiginous naevi have been said to have cheetah phenotype. |
The Bolognia sign refers to a harmless, small area of darker colour on one side of the naevus. |

|

|

|

|
Uncommon types of melanocytic naevi include:
The term atypical naevus may be used in several ways.
Atypical naevi usually occur in fair-skinned individuals and are due to sun exposure. They may be solitary or numerous. Pathology is reported as dysplastic junctional or compound naevus and has specific histological features (the Clark naevus).
Common naevus |
Naevus in dark skin |
Atypical naevus |
Dysplastic naevus |
|---|---|---|---|
A common naevus is a flat mole with a single uniform colour. |
In dark skin, naevi are often black in colour. |
People with multiple atypical naevi are at increased risk of melanoma (cancerous mole). |
Dysplastic naevus describes an atypical mole that has specific histological criteria. |

|

|

|

|
Blue naevus |
Cellular naevus |
Miescher naevus |
Unna naevus |
|---|---|---|---|
Blue naevus is a deeply pigmented type of dermal naevus. |
Cellular naevus is a non-pigmented dermal naevus. |
Miescher naevus is a dome-shaped smooth dermal naevus often found on the face. |
Unna naevus is a papillomatous dermal naevus that is in the shape of a raspberry. |
|

|

|

|
Meyerson naevus |
Halo naevus |
Spitz naevus |
Reed naevus |
|---|---|---|---|
Meyerson naevus is a naevus affected by a halo of eczema/dermatitis. |
Halo naevus or Sutton naevus has a white halo around the mole. The mole gradually fades away over several years. |
Spitz naevus or epithelioid cell naevus is a pink (classic Spitz) or brown (pigmented Spitz) dome-shaped mole that arises in children and young adults. |
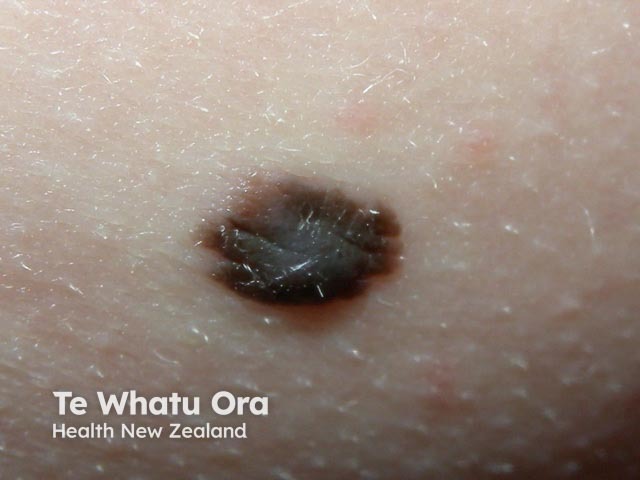
Reed or spindle cell naevus is a very dark-coloured mole with spindle-shaped dermal melanocytes, usually found on the limbs. |

|

|

|
|
Recurrent naevus |
Agminated naevus |
Acral naevus |
Nail unit naevus |
|---|---|---|---|
Recurrent naevus refers to the reappearance of pigment in a scar following surgical removal of a mole – this may have an odd shape. |
An agminated naevus is a cluster of similar moles or freckles. |
Acral naevus refers to one on the palm or sole. |
Nail unit naevus causes a uniform longitudinal band of pigment on a nail. |

|

|
|

|
See more images of atypical naevi.
People worry about their moles because they have heard about melanoma, a malignant proliferation of melanocytes that is the most common reason for death from skin cancer.
Melanocytic naevi sometimes change for other reasons than melanoma, for example following sun exposure or during pregnancy. They can enlarge, regress or involute (disappear).
Melanocytic naevi are usually diagnosed clinically by their typical appearance. If there is any doubt about the diagnosis, an expert may be consulted in person or with the help of clinical and dermatoscopic images. This is especially important if:
Most skin lesions with these characteristics are actually harmless when evaluated by an expert using dermatoscopy. Short-term digital dermatoscopic imaging may be used in equivocal flat lesions to check for change over time.
Naevi that remain suspicious for melanoma are excised for histopathology (diagnostic biopsy). A partial biopsy is not recommended, as it may miss an area of cancerous change.
Most melanocytic naevi are harmless and can be safely left alone. They may be removed in the following circumstances:
Surgical techniques include:
The number of melanocytic naevi can be minimised by strict protection from the sun, starting from birth. Sunscreen alone is not sufficient to prevent new naevi from appearing.
At any age, sun protection is important to reduce skin ageing and the risk of skin cancer.
Most melanocytic naevi that appear in childhood remain forever. Teenagers and young adults tend to have the greatest number of naevi. There are fewer in later life because some of them slowly fade away.
To increase the chance of spotting melanoma early, recommend: