Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Authors: Mr Jamie Banks, Plastic Surgery Core Trainee, St George’s Hospital, London, UK (2023)
Previous contributors: Vanessa Ngan, Staff Writer (2003); Dr Amanda Oakley, Dermatologist (2014)
Reviewing dermatologist: Dr Ian Coulson
Edited by the DermNet content department
Introduction Demographics Causes Clinical features Variation in skin types Complications Diagnosis Differential diagnosis Treatment Outcome
A nevus sebaceous is a common type of birthmark affecting 0.3% of live births. Present at birth and most often found on the scalp, it consists of overgrown epidermis, sebaceous glands, hair follicles, apocrine glands, and connective tissue.
A nevus sebaceous (also known as sebaceous naevus, naevus sebaceous of Jadasshon, and organoid naevus) is a type of epidermal naevus and is classified as a benign hair follicle tumour. It is also called an organoid naevus because it may include components of the entire skin. First described in 1895 by Jadassohn, recent work has significantly changed our understanding of this condition.
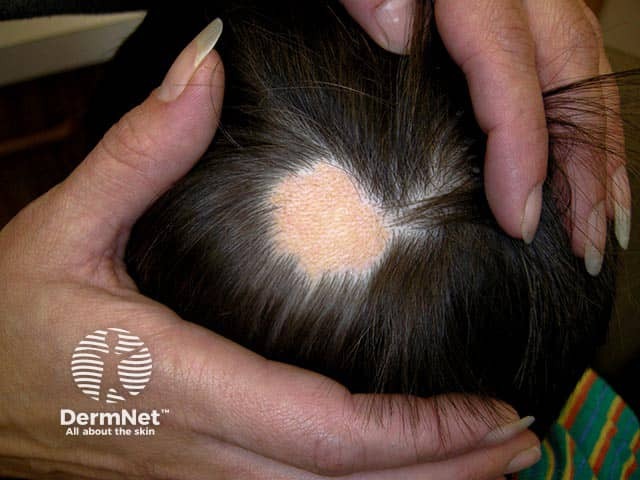
A hairless occipital patch in a child - the nevus sebaceous may become thicker and verrucous at puberty
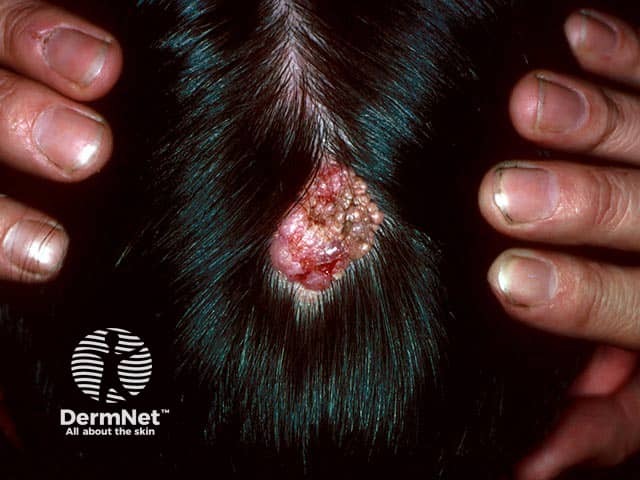
A nevus sebaceous on the occiput, which occasionally bleeds
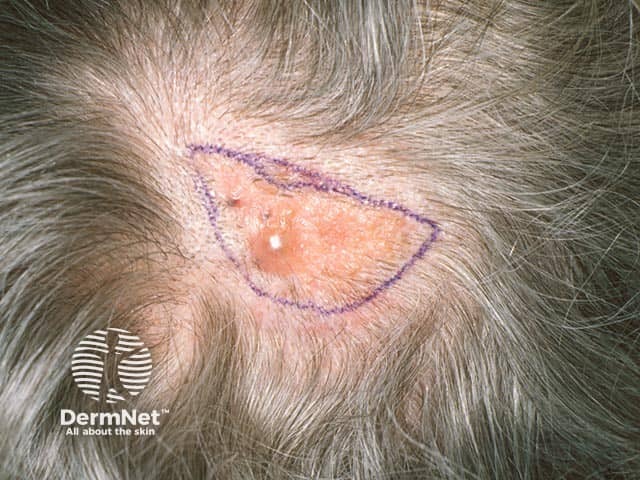
Nevus sebaceous, present since birth, slowly become rough and has developed a benign cyst within it
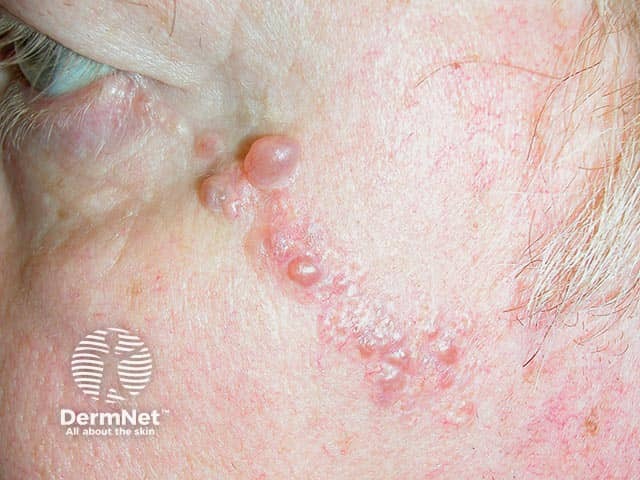
Apocrine hidrocystoma developing within a sebaceous nevus on the cheek
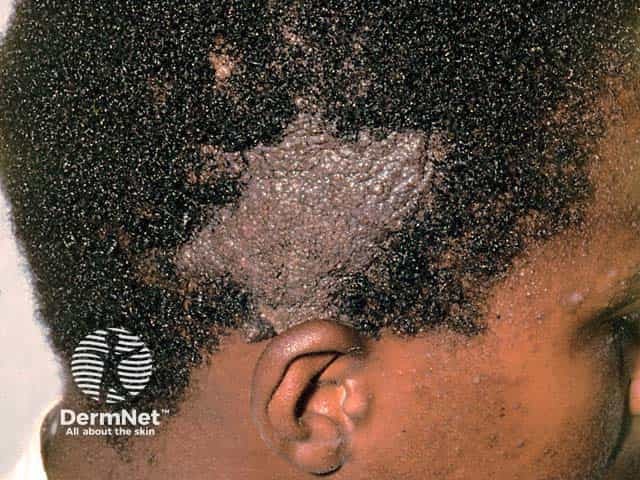
A nevus sebaceous in skin of colour - the typical yellow colour cannot be appreciated in darker skin types
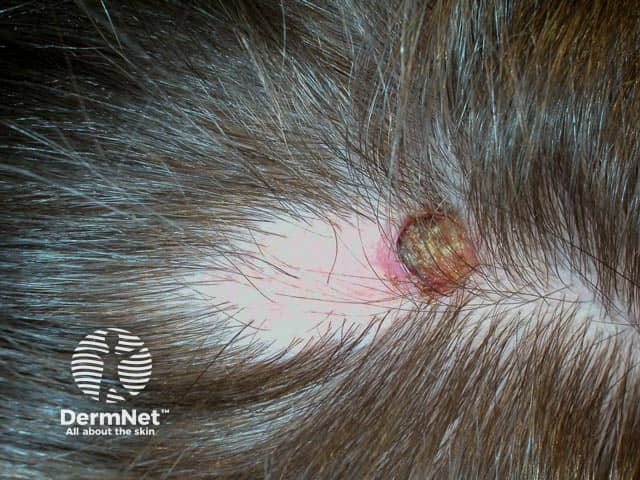
A crusted area has developed at the edge of this nevus sebaceous - biopsy is needed to exclude either a benign or malignant lesion arising within
A nevus sebaceous are associated with a number of congenital syndromes, such as epidermal nevus syndrome and Schimmelpenning-Feuerstein-Mims (SFM) syndrome. However, it is not considered an inherited disorder.
Males and females, and different skin types, are equally affected.
The abnormality resulting in nevus sebaceous arises from a defect in the ectoderm (the outer layer of the embryo that gives rise to epidermis and neural tissue).
A nevus sebaceous are thought to be due to a mosaic genetic abnormality (ie, a line of cells with a genetic error). Mutations in the RAS/MAP kinase pathway, which codes for growth factors, affect cellular growth, differentiation, and programmed cell death (apoptosis). Specifically, HRAS and KRAS mutations have been implicated as well as the fibroblast growth factor receptor FGFR2.
Changes during childhood are unlikely and should prompt biopsy if present. However, a nevus sebaceous may become more pronounced around adolescence with expected pubertal thickening, often appearing bumpy, warty, or scaly.
Different skin types are equally affected. There is some evidence that basal cell carcinoma may be misdiagnosed as nevus sebaceous in people with darker skin phototypes.
Most sebaceous nevi remain unchanged throughout life and do not cause any problems. However, in 10–20% of cases, another secondary tumour may grow within the lesion.
Secondary tumours in sebaceous nevi are:
Nevus sebaceous syndrome refers to the rare association of a large nevus sebaceous with disorders of the eye, brain, and skeleton.
Schimmelpenning-Feuerstein-Mims syndrome (or just Schimmelpenning syndrome) is a subtype.
Nevus sebaceous syndrome can result in eye tumours and the skull may be asymmetrical. Characteristic associated neurological features include:
For further information, see epidermal naevus syndromes.
Phakomatosis (or phacomatosis) pigmentokeratotica (PPK) is the association of a nevus sebaceous and a speckled lentiginous naevus. A speckled lentiginous naevus is a flat, light-brown birthmark with darker spots within it, classified as a type of congenital melanocytic naevus.
Neurological defects in PPK may include hemiatrophy (in which one side of the body under-developed), muscle weakness, sensory nerve abnormalities, and hyperhidrosis.
Nevus sebaceous (sebaceous nevus) has a characteristic clinical appearance and is often diagnosed clinically in childhood or adolescence. Sometimes the diagnosis is made by a pathologist after the lesion has been surgically removed.
A biopsy undertaken during childhood will show a hairless lesion with immature hair follicles and sebaceous glands. In adults, there is thickening of the epidermis with hyperkeratosis, acanthosis, mature hair follicles, and prominent sebaceous glands located at an abnormally high level within the dermis. Sometimes a secondary tumour is found in the specimen.
These can be difficult to differentiate due to significant overlap in both macro- and microscopic features. They are often associated with RAS mutations.
A nevus sebaceous (sebaceous naevus) should be monitored. If a lump or sore appears within a nevus sebaceous, arrange for it to be reviewed by a dermatologist. It may require a biopsy or excision. Typically, elective excision should be delayed until adolescence, however lesions demonstrating changes during childhood should be biopsied.
Full skin thickness excision may also be arranged for cosmetic reasons, but a scar is inevitable.
Lasers have been used to treat nevus sebaceous with varying success, but typically superficial procedures such as shave, dermabrasion, or laser resurfacing are not recommended as the lesion is not removed entirely.
New work suggests that topical 1% sirolimus flattens lesions in 4 out of 5 patients with nevus sebaceous.
Sebaceous nevi are common with a recognised small risk of developing a secondary malignant tumour within the original lesion, most commonly a locally invasive basal cell carcinoma. As these malignant changes occur almost exclusively in adults, there is greater time to decide on prophylactic or therapeutic excision (usually curative). This should reassure patients regarding long term outcomes.
Extensive nevi or evidence of nevus sebaceous syndrome should be discussed at a multidisciplinary team (MDT) meeting.