Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Harriet Cheng, Dermatology Registrar, Hamilton, New Zealand, 2012.
Introduction
Immediate complications
Bleeding during skin surgery
Damage to important structures
Adverse reactions
Delayed complications
Wound infection
Wound breakdown
Suture reactions
Incomplete excision of a skin cancer
Delayed healing
Persistent swelling
Late complications after skin surgery
Unsightly cosmetic result
Recurrent tumours
Unnecessary or inappropriate skin surgery
Skin surgery includes removal of skin lesions or sampling them (biopsy) to confirm a diagnosis. The sample will be sent to a pathologist who will examine the skin under a microscope.
The initial healing process occurs over 2-3 weeks. Remodelling and strengthening of the wound continues for 6 to 12 months following skin surgery. Complications such as bleeding and infection may delay the healing process, increase pain and discomfort and result in a larger scar.
This topic covers:
Complications quite commonly arise during or shortly after surgery, including:
There may also be difficulty in wound closure.
Risk factors for excessive bleeding include:
A small amount of bleeding and bruising can be expected. Your surgeon will try to minimise this as much as possible during the procedure by either clotting small vessels using electrosurgery (cautery) or tying off bleeding vessels with a stitch / suture.
Excessive bleeding:
If bleeding occurs, rest with the affected area elevated above the level of your heart, and apply firm, constant pressure on the wound for 20 minutes without removing the original dressing. If bleeding continues, urgent medical advice should be sought.
Skin surgery inevitably results in an injury to some components of the skin i.e. the epidermis (outer layer), dermis (structural layer) and subcutaneous tissue (fat layer).
However, important structures may also be damaged, particularly if the skin lesion for removal has grown deep into underlying structures or the lesion is in a site where important structures such as nerves or salivary glands lie close to the skin surface.
Surgical injury to nerves and salivary glands |
||
|---|---|---|
Sensory nerve damage |
|
|
Motor nerve damage |
|
|
Salivary gland damage |
These glands are responsible for production and secretion of saliva.
|
|
Medications used immediately before or during surgery include local anaesthetic and analgesics to reduce the pain of the procedure.
Local anaesthetics work by blocking sodium channels on nerve cell membranes. This results in blockage of pain impulses along the nerve. Adrenaline-containing local anaesthetic is administered in an acidic substance. This is essential to maintain the anaesthetic in a soluble form. It is also responsible for a stinging sensation on injection. There are two main types of local anaesthetic: esters and amides.
Local anaesthetics are generally safe. Adverse reactions may occur if a large volume is injected or if the anaesthetic is inadvertently injected into a blood vessel.
Local anaesthetics are often injected together with adrenaline (also called epinephrine). Adrenaline causes vasoconstriction resulting in less bleeding and less systemic absorption of the anaesthetic agent. Large volumes of adrenaline may result in:
Paracetamol (also called acetominophen) is available over the counter in pharmacies and supermarkets in New Zealand and elsewhere without the need for prescription.
Nonsteroidal anti-inflammatory drugs (NSAIDs) are a class of drugs which include ibuprofen, diclofenac, naproxen, meloxicam and indomethicin. These are marketed under a number of trade names in New Zealand and some are available without prescription.
Opioids include codeine, tramadol, morphine and oxycodone. Codeine is available without prescription in a combined form with paracetamol in pharmacies. Other opioid analgesics require a doctor's prescription.
Complications may arise hours, days or weeks after a surgical procedure, including:
Wound infection occurs in approximately 1% of skin surgeries, although this figure varies with the type of procedure, type and location of tumour, and patient factors. Signs of skin infection usually appear several days after surgery and include increasing redness, swelling, and pain around the wound +/- pus or discharge from the wound. If you develop these symptoms you should see your surgeon promptly and you may be prescribed a course of antibiotics.
Severe wound infection is rare after skin surgery and may lead to fever and severe illness due to spread of bacteria via the bloodstream (bacteraemia). Left untreated, severe infection could be fatal.
The type of bacteria causing infection differs depending on body site:
Factors that increase the risk of infection include:
If one or more of these risk factors are present, oral antibiotics may be prescribed for 7-10 days to prevent infection. It is important that the prescribed course is completed. Common antibiotic choices for skin infection include:
After stitches are removed the wound may reopen (dehisce), for example:
A clean reopened wound can be re-stitched but an infected wound is usually left to heal by secondary intention.
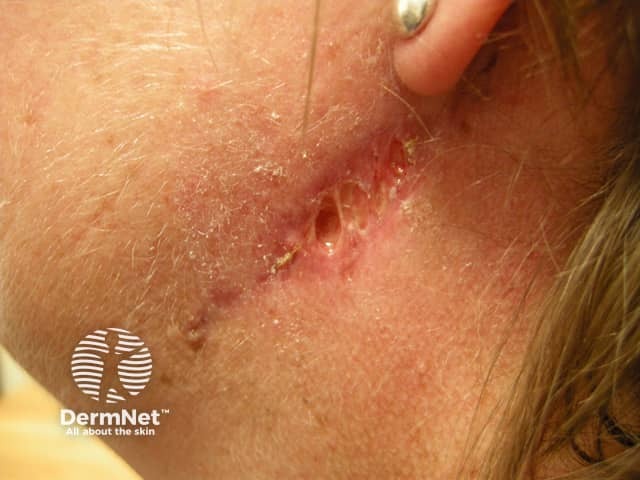
Surgical wound dehiscence
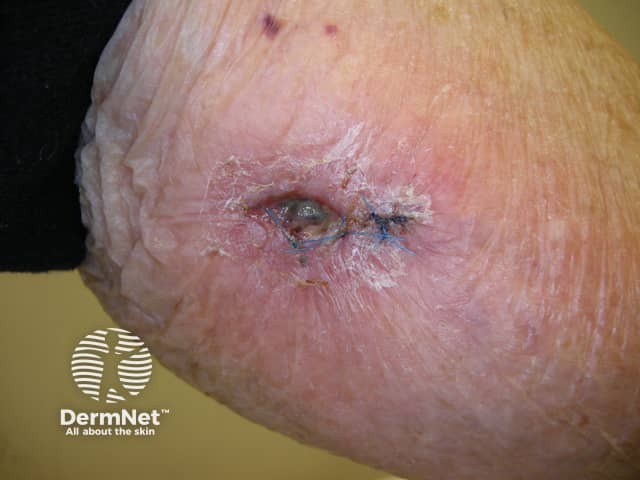
Surgical wound dehiscence
Wounds are usually closed with sutures made of synthetic (e.g. nylon) or natural materials (e.g. cotton, catgut, silk). Some sutures are absorbable and others will need to be removed once sufficient wound healing has occurred.
Suture material may elicit redness and swelling at the wound site, as they are foreign to the body. This is an expected reaction and does not represent allergy or infection. Factors associated with increased reaction include larger caliber sutures, delayed suture removal, natural materials and braided sutures.
Absorbable subcutaneous sutures may also occasionally extrude through the skin as they dissolve; this can occur weeks or months after the procedure.
True allergy to suture material is rare but has been reported with catgut, silk and nylon sutures.
A margin of healthy appearing skin is excised around a skin cancer to improve the chances of its complete removal. Once excised, the removed skin is sent to a pathologist for examination under a microscope. This gives a more reliable indication of whether the whole lesion has been removed. Skin cancers can occasionally recur even after careful surgery and when the pathologist has reported clear margins.
If a skin cancer is not completely excised, further surgical treatment may be required or a course of radiotherapy may be recommended.
Non-cancerous skin lesions may also recur. For example, epidermal cysts that have been drained or excised may reappear, requiring further surgery.
Factors that delay healing after skin surgery include:
Wounds on the legs that are left to heal by secondary intention are particularly at risk of delayed healing due to poor blood supply.
If a wound remains unhealed after several weeks it should be reviewed by your dermatologist or surgeon. Underlying factors contributing to delayed healing should be optimised or treated where possible. Special dressings may be used to assist wound healing.
Surgery may damage lymphatic channels and cause swelling that takes weeks or months to resolve. Common sites for persistent swelling after skin surgery are the Lower eyelid and lower Legs
Lymphatic damage may also cause increased risk of infection and ultimately delayed healing.
Late complications after skin surgery may include:
The appearance of the healed surgical site varies, depending on the type of surgery and its site. Some scar tissue always forms during surgery because the dermis (deep skin layer) is damaged.
Colour changes |
|
|
Stitch (suture) marks |
|
|
Hypertrophic scars |
|
|
Keloid scars |
|
|
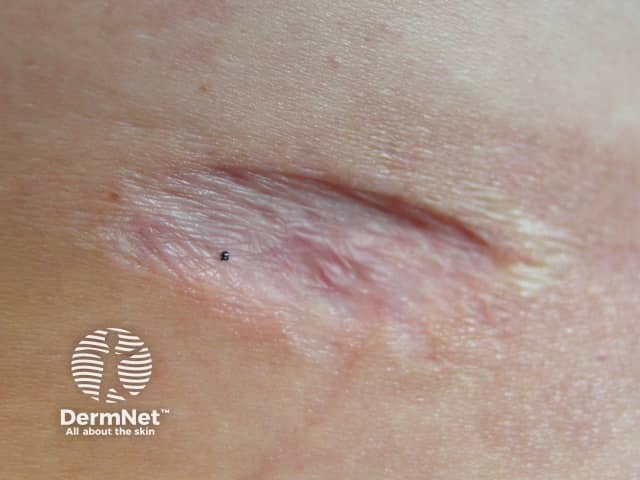
Atrophic scar
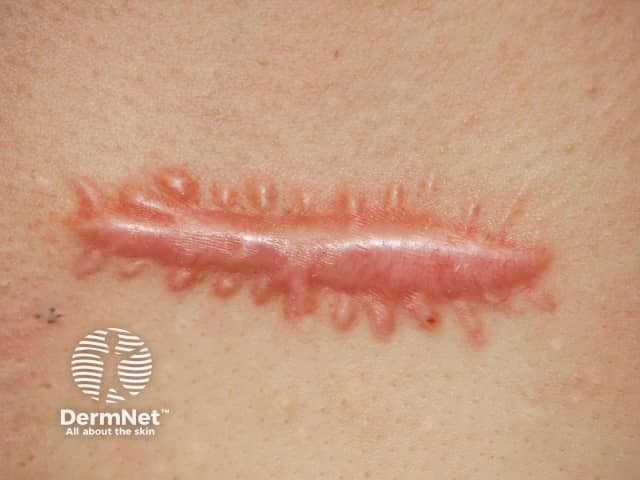
Hypertrophic scar
Tumour may recur at the excision site or a new tumour may develop. This usually requires repeated surgery to excise the new lesion. Depending on the tumour type, radiotherapy may be recommended as well or instead of further surgery.
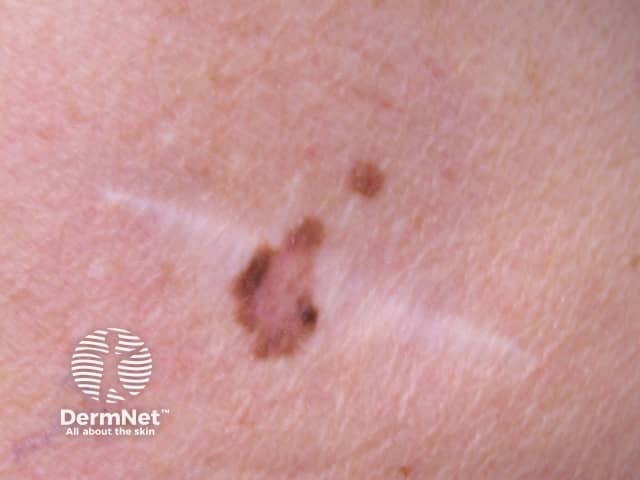
Recurring melanocytic naevus
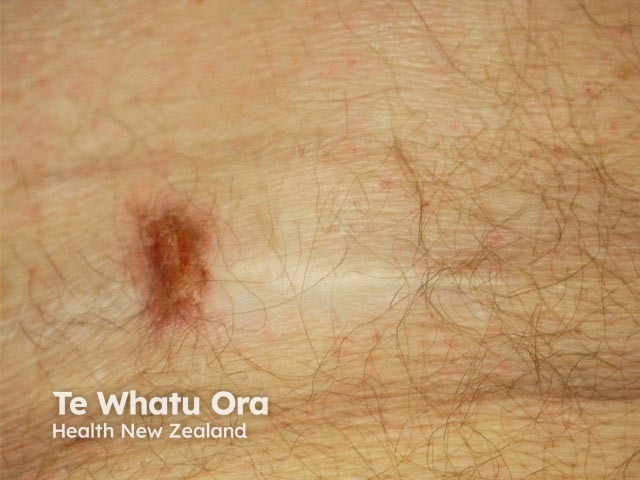
Recurring basisquamous cancer
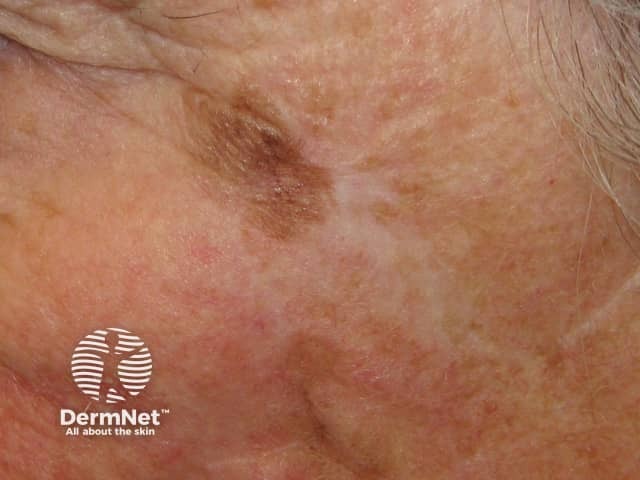
Recurring lentigo maligna
Sometimes a skin lesion suspected of being cancerous is benign when examined under the microscope. Therefore, surgical excision (and the associated risks) was undertaken unnecessarily.
It may be difficult to make a definitive diagnosis based on the lesion's clinical appearance. The potential risk of missing a skin cancer must be weighed against the risk associated with potentially unnecessary surgery. Assessment of the lesion by a specialist dermatologist prior to surgery will help reduce the number of unnecessary procedures. In many cases, a skin biopsy may be undertaken prior to a major skin surgical procedure. Of course skin surgery may be chosen to remove non-cancerous growths for functional or cosmetic reasons.
Other examples of inappropriate surgery include: