Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Claudia King, Medical Officer, Adelaide, Australia. Copy edited by Gus Mitchell. February 2022
Introduction
Demographics
Causes
Clinical features
Variation in skin types
Complications
Diagnosis
Differential diagnoses
Treatment
Outcome
Erythema multiforme is an immune-mediated, typically self-limiting, mucocutaneous condition characterised by ‘target’ lesions. Significant mucosal involvement distinguishes erythema multiforme major from multiforme minor. Episodes can be isolated, recurrent, or persistent.
In most cases, erythema multiforme is precipitated by herpes simplex virus (HSV) infection; alternative triggers include other infections, medications, and vaccinations. Classic ‘target’ lesions present as concentric rings of colour variation which develop symmetrically in an acral distribution, with or without involvement of mucous membranes.
Erythema multiforme is a distinct entity from Steven Johnson syndrome (SJS) and toxic epidermal necrolysis (TEN).
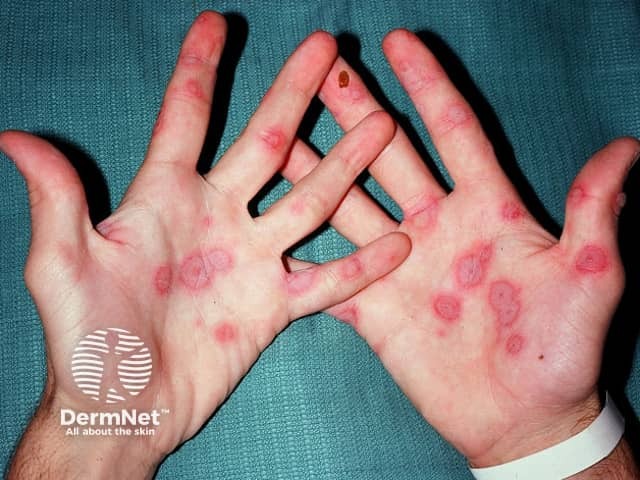
Cutaneous adverse reaction to anticonvulsant, erythema multiforme target lesions
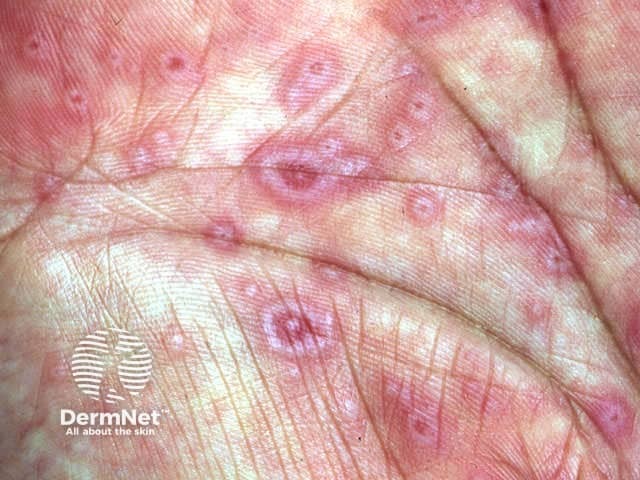
Erythema multiforme minor

Erythema multiforme
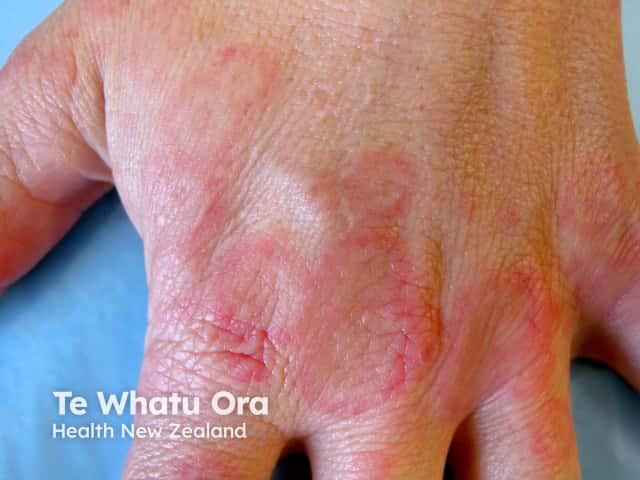
Erythema multiforme
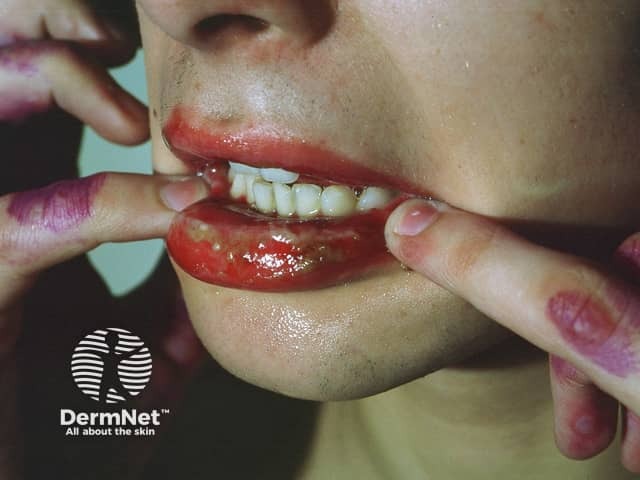
Lip involvement in erythema multiforme
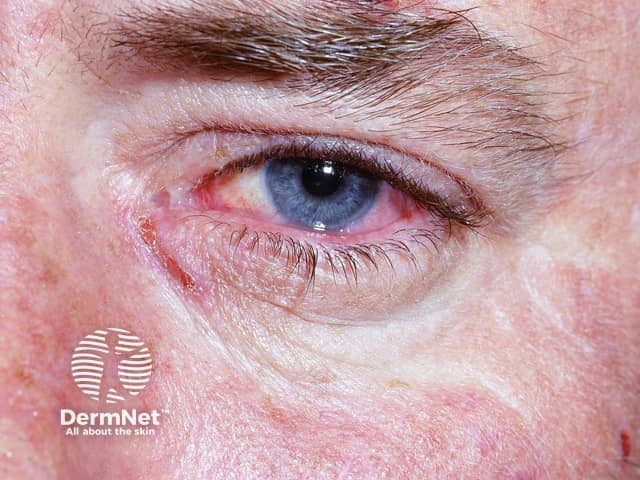
Erythema multiforme of eye
Erythema multiforme affects less than 1% of the population. It is most common in young adults (aged 20–40 years) with a modest predominance in males. There is no association with race.
There appears to be a genetic predisposition in people carrying the HLA-DQB1*0301 allele, which shares an even stronger association with herpes-related erythema multiforme. Multiple other alleles have been associated with its recurrent form.
Infection precipitates 90% of cases, with HSV type 1 being the predominant cause. Other infectious triggers include:
Mycoplasma pneumoniae infection is often listed as a trigger of erythema multiforme, however mucocutaneous manifestations associated with this infection have recently been classified as their own independent entity, reactive infectious mucocutaneous eruption (RIME).
Medications which may trigger erythema multiforme include:
Other conditions associated with erythema multiforme (usually in persistent disease) include:
In many cases, the inciting factor remains unknown.
Most research on the mechanism of disease has focused on the herpes-associated presentation. The herpes virus is phagocytosed by mononuclear cells which express cutaneous lymphocyte antigen (a skin-homing receptor). Engulfed viral DNA is then transferred to the epidermis and into keratinocytes. Within the keratinocyte layer, expression of viral DNA fragments induces a cell-mediated immune response, including the production of interferon-γ which upregulates the inflammatory process.
Many patients report prodromal symptoms including fatigue, malaise, myalgia, or fever. These likely represent the course of precipitating illness rather than true prodrome.
Symptoms are expected to self-resolve within 4 weeks from onset (or up to 6 weeks in severe disease).
Cutaneous lesions resolve without scarring, though hyperpigmentation may persist for several months.
Ocular involvement can lead to more serious complications including:
Diagnosis is often made based on history and clinical examination.
Where there is doubt about the diagnosis, consider:
Skin biopsy with histopathology and direct immunofluorescence can be non-specific but helps to distinguish erythema multiforme from other more serious differentials, such as autoimmune blistering diseases. Upper dermal oedema and individual epidermal keratinocyte necrosis are suggestive pathological features.
All patients with recurrent erythema multiforme should be tested for herpes simplex virus, including sampling of skin or mucosal lesions. In recurrent or persistent erythema multiforme without a clear precipitant, consider work up for solid organ or haematological malignancies.
Treatment is often not needed as episodes are typically self-limiting with no ongoing complications. However, ocular involvement should always prompt ophthalmology referral given the risk for more serious sequelae.
Treatment of symptomatic mild cases:
Other treatments are dependent on cause:
Severe mucosal disease:
Recurrent disease:
Erythema multiforme is self-limiting with little to no ongoing complication in most patients. Recurrent or persistent disease comes with additional treatment challenges, but remission can be achieved.