Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Introduction
Food allergy and the skin
Other food allergy symptoms
Causes
Diagnosis
Other reactions
Food deficiencies
Treatment
Prevention
Food allergy is an immunological reaction to a food protein that is either immediate (occurring seconds to minutes after eating or touching the food item) or delayed (occurring hours or days later). Allergic reactions may occur when the affected person eats or touches a tiny amount of the responsible protein.
Food allergy is most common in young babies (4%), who often outgrow their allergies. About 2% of adults also suffer from an allergy to one or more foods. The tendency to food allergy runs in families.
Skin conditions due to food allergy include:
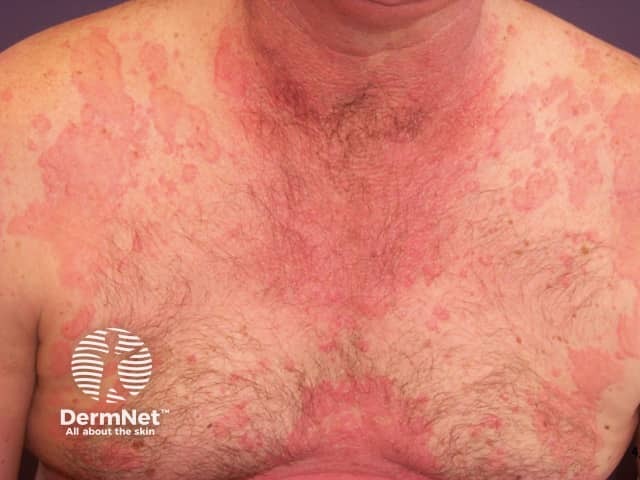
Urticaria
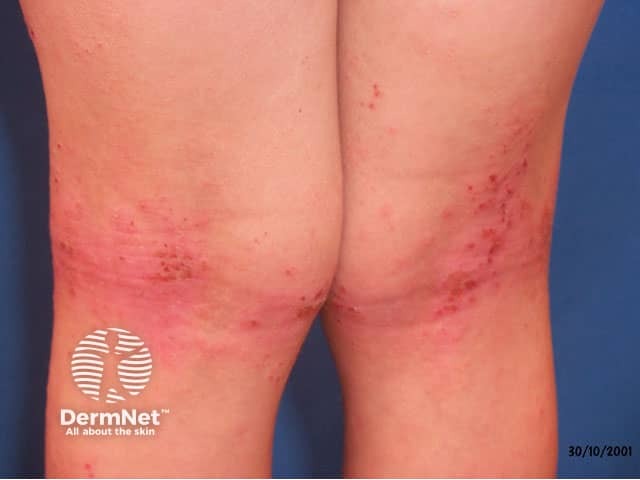
Atopic eczema

Dermatitis herpetiformis
Food allergy may result in the following symptoms.
Respiratory allergy
Gastrointestinal allergy
Circulatory allergy
About 90% of systemic allergic reactions are due to the following food items:
There are numerous other foods and plants that occasionally cause allergy. Some are listed here.
An allergy may also be provoked by preservatives such as parabens, sulphites, and flavouring agents or fragrances added to foods.
Food allergy is diagnosed by taking a careful history of the symptoms and their relationship to food, supported by examination findings and the results of tests. Unfortunately, neither history nor tests are entirely reliable in everyone.
The main tests for food allergy are:
Not all reactions to food are allergic in origin. Intolerance can cause similar symptoms to allergy, including urticaria and dermatitis. But the reaction often depends on how much is consumed. These reactions are classified as follows.
Skin conditions may also be due to deficiencies in the diet, sometimes because of attempts to reduce exposure to known or presumed allergens.
The mainstay of management is to identify which foods are responsible for reactions, and then to avoid them. Prescribed treatments depend on symptoms, and may include:
It is not known how to prevent all food allergy. Recommendations regarding the introduction of peanuts to the food of infants have recently changed.