Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Introduction Demographics Causes Clinical features Diagnosis Treatment
Hydroa vacciniforme is one of the rarest forms of photosensitivity dermatoses. It affects sun-exposed skin and is characterised by recurrent fluid-filled blisters (‘hydroa’) that heal with pox-like (‘vacciniform’) scars.
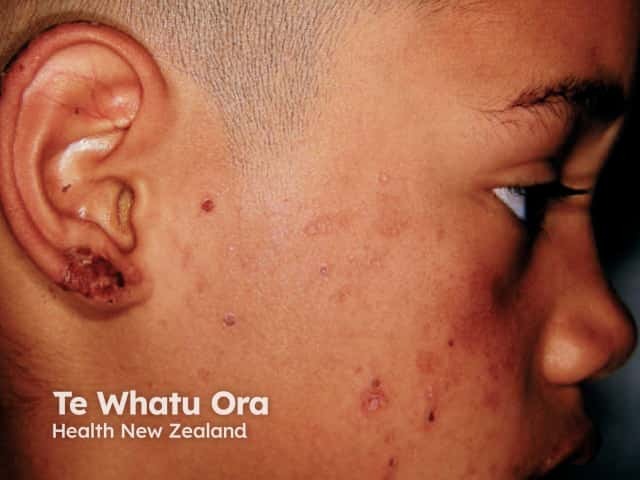
Hydroa vacciniforme
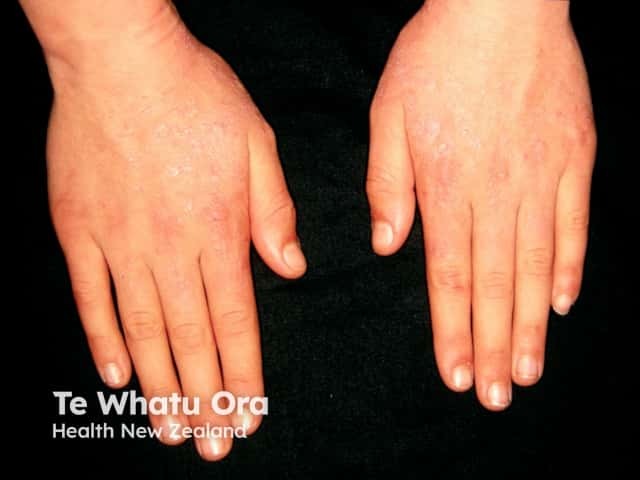
Hydroa vacciniforme
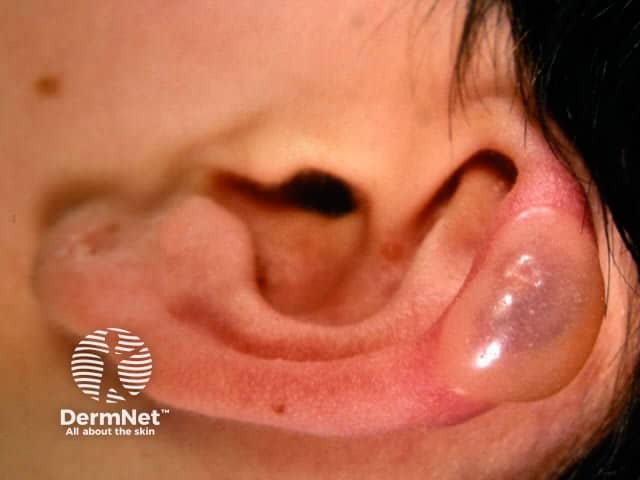
Hydroa vacciniforme
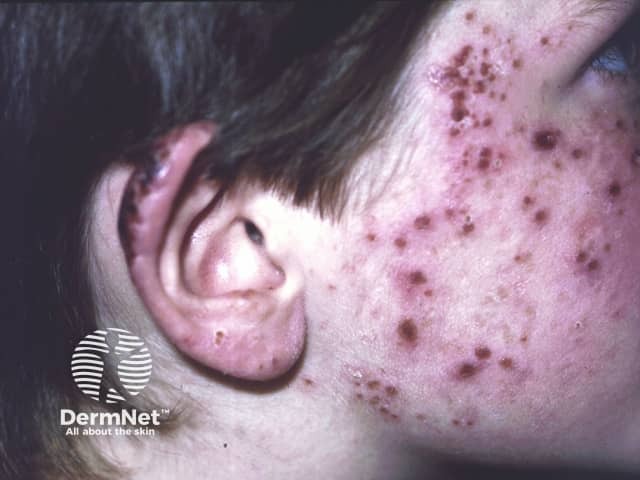
Hydroa vacciniforme
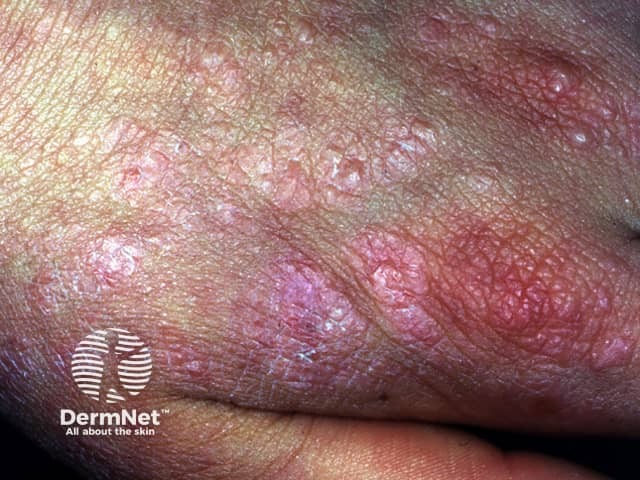
Hydroa vacciniforme
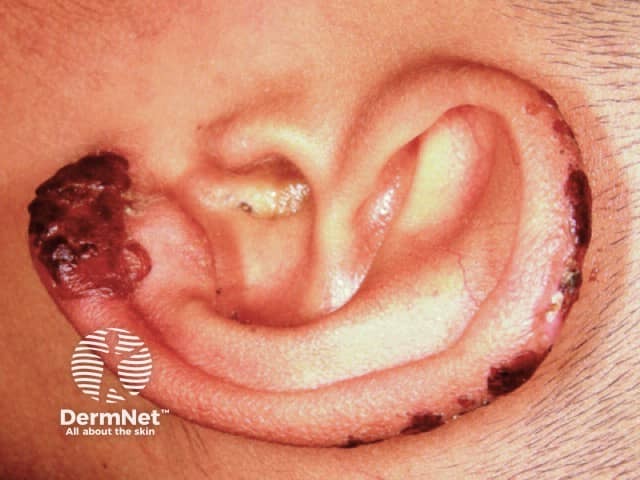
Hydroa vacciniforme
Hydroa vacciniforme mostly affects children aged 3–15 years. It is more commonly diagnosed in females than in males. The disease tends to have a later onset and run a longer course in males.
The cause of hydroa vacciniforme is usually unknown. Long wavelength ultraviolet radiation (UVA) is most often implicated.
In some cases, hydroa vacciniforme has been associated with Epstein-Barr virus (EBV) infection, which normally results in infectious mononucleosis (glandular fever). In these cases, the hydroa vacciniforme lesions may spread to involve areas that are not exposed to the sun.
Sun-exposed areas are affected most and include the face, ears, hands and lower limbs. In most cases signs and symptoms usually start to occur about 30 minutes to 2 hours after sun exposure and present as:
The rash usually first appears in spring with recurrences throughout the summer months.
Some patients may have other symptoms, including mild inflammation of the eyes (keratoconjunctivitis and photophobia), lifting of fingernails and toenails (photo-onycholysis) and rarely fever and malaise. Exaggerated reactions to insect bites are frequent and may result in skin necrosis and ulceration.
Severe EBV infection associated with hydroa vacciniforme has resulted in lymphoproliferative disorders (NK-cell non-Hodgkin lymphoma or leukaemia) and may have a fatal outcome.
Hydroa vacciniforme may be suspected clinically. A skin biopsy may show characteristic pathological features of hydroa vacciniforme.
The status of EBV should be evaluated.
In most patients, the condition disappears by the time they reach adolescence, although the scars are permanent. Patients with hydroa vacciniforme must take measures to avoid sun exposure by following sun protection strategies. This includes applying SPF 50+ sunscreens with UVA blocking agents and wearing protective clothing. This may prevent or reduce the number of recurrences of the condition.
Oral medication may be useful in reducing outbreaks but does not reliably prevent hydroa vacciniforme lesions.
Phototherapy with narrowband UVB or photochemotherapy (PUVA) has also been used to confer relative photoprotection and desensitisation.