Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Introduction
Classification
Demographics
Clinical features
Causes
Diagnosis
Treatment
Differential diagnosis
Outlook
Urticaria is characterised by very itchy weals (hives), with or without surrounding erythematous flares. The name urticaria is derived from the common European stinging nettle Urtica dioica. Urticaria can be acute or chronic, spontaneous or inducible.
A weal (or wheal) is a superficial skin-coloured or pale skin swelling, usually surrounded by erythema that lasts anything from a few minutes to 24 hours.
Urticaria can co-exist with angioedema which is a deeper swelling within the skin or mucous membranes.
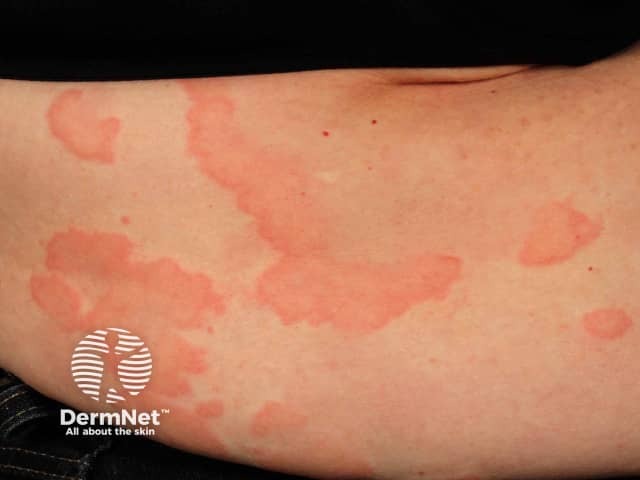
Urticaria
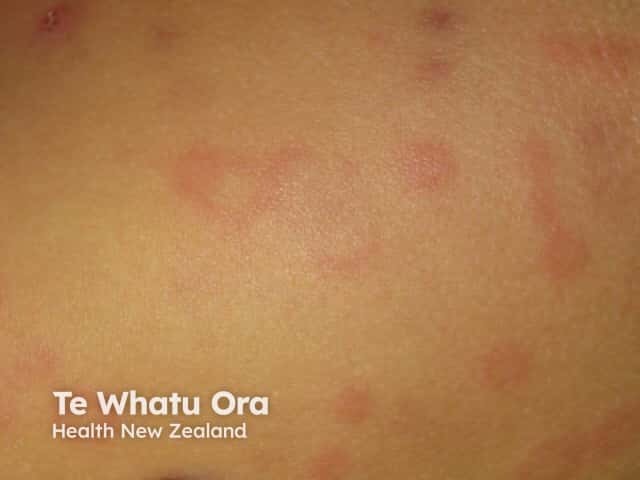
Spontaneous urticaria

Wheal in dark skin
Urticaria is classified according to its duration.
Chronic urticaria may be spontaneous or inducible. Both types may co-exist.
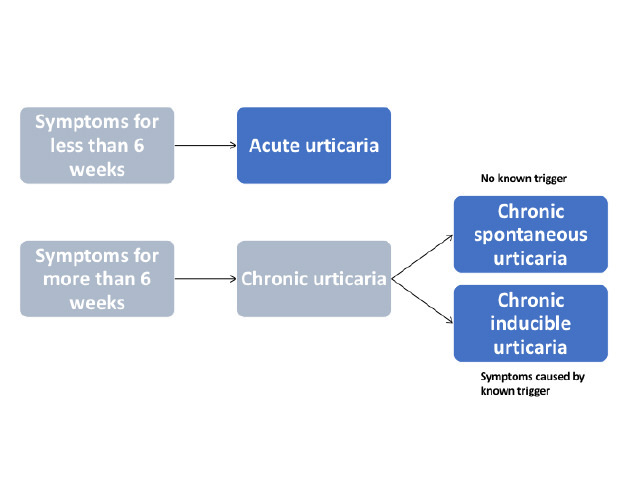
Figure 1 - Classification of urticaria
Chronic inducible urticaria includes:
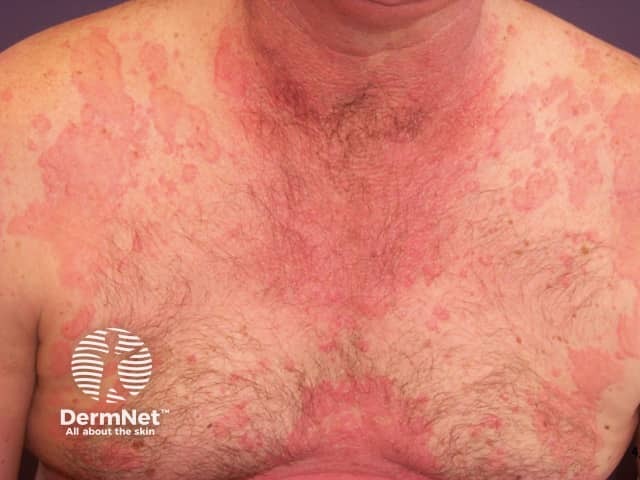
Urticaria
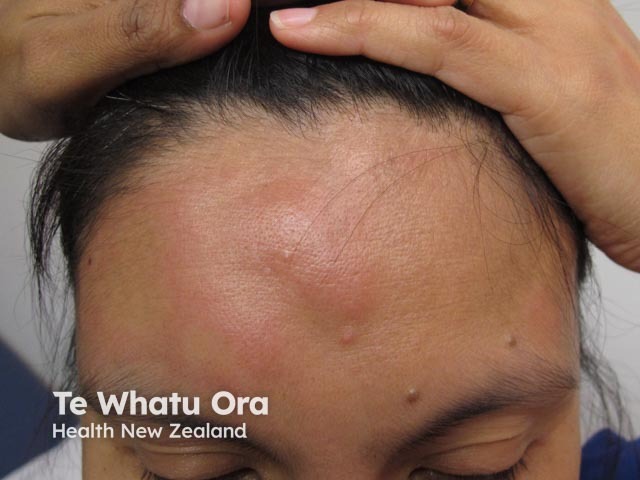
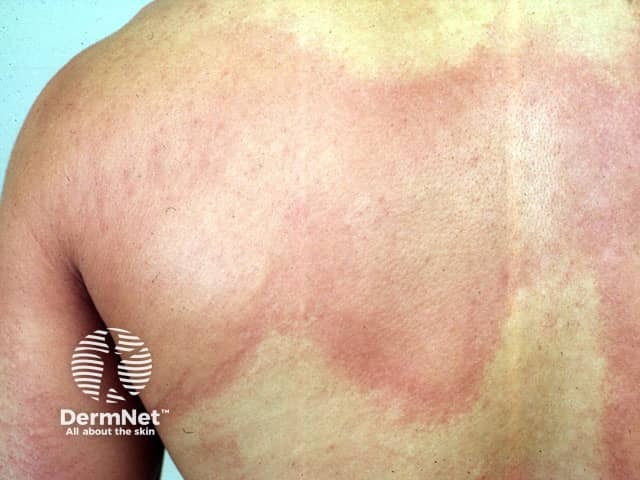
One in five children or adults has an episode of acute urticaria during their lifetime. It affects all races and both sexes.
Acute urticaria can occur in newborns and infants but is uncommon. Acute urticaria in children is usually caused by infection, even if afebrile. In older children food, medication, and inhaled allergens are also important causes. In adults urticaria is usually idiopathic and spontaneous.
Acute urticaria with fever can be the first sign of COVID-19 infection.
Chronic spontaneous urticaria affects 0.5–2% of the population; in some series, two-thirds are women. Chronic inducible urticaria is however more common. There are genetic and autoimmune associations.
Urticarial weals can be a few millimetres or several centimetres in diameter, coloured white or red, with or without a red flare. Each weal may last a few minutes or several hours and may change shape. Weals may be round, or form rings, a map-like pattern, or giant patches.
Urticaria can affect any site of the body and tends to be distributed widely.
Angioedema is more often localised. It commonly affects the face (especially eyelids and perioral sites), hands, feet, and genitalia. It may involve tongue, uvula, soft palate, or larynx.
Serum sickness due to blood transfusion and serum sickness-like reactions due to certain drugs cause acute urticaria leaving bruises, fever, swollen lymph glands, joint pain and swelling.
In chronic inducible urticaria, weals appear about 5 minutes after the stimulus and last a few minutes or up to one hour. Characteristically, weals are:
The weals are more persistent in chronic spontaneous urticaria, but each individual lesion will resolve within 24 hours. They may occur at certain times of the day.
Visual analogue scales can be used to record and compare the degree of itch.
The activity of chronic spontaneous urticaria can be assessed using the UAS7 scoring system. The daily weal/itch scores are added up for seven days; the maximum score is 42.
Score |
Weals/24 hours |
Itch |
|---|---|---|
0 |
None |
None |
1 |
20 |
Mild |
2 |
20–50 |
Moderate |
3 |
>50 |
Intense |
The emotional impact of urticaria and its effect on quality of life should also be assessed. The Dermatology Life Quality Index (DLQI) and CU-Q2oL, a specific questionnaire for chronic urticaria, have been validated for chronic urticaria, where sleep disruption is a particular problem.
Weals are due to release of chemical mediators from tissue mast cells and circulating basophils. These chemical mediators include histamine, platelet-activating factor and cytokines. The mediators activate sensory nerves and cause dilation of blood vessels and leakage of fluid into surrounding tissues. Bradykinin release causes angioedema.
Several hypotheses have been proposed to explain urticaria. The immune, arachidonic acid and coagulation systems are involved, and genetic mutations are under investigation.
Acute urticaria can be induced by the following factors, but the cause is not always identified.
Severe allergic urticaria may lead to anaphylactic shock (bronchospasm, collapse).
Immune complexes due to blood transfusion cause serum sickness and certain drugs cause serum sickness-like reactions.
A single episode or recurrent episodes of angioedema without urticaria can be due to an angiotensin-converting enzyme (ACE) inhibitor drug [see ACE inhibitor-induced angioedema].
Chronic spontaneous urticaria is mainly idiopathic (cause unknown). An autoimmune cause is likely. About half of investigated patients carry functional IgG autoantibodies to immunoglobulin IgE or high-affinity receptor FcεRIα.
Chronic spontaneous urticaria has also been associated with:
Weals in chronic spontaneous urticaria may be aggravated by:
Inducible urticaria is a response to a physical stimulus.
Type of inducible urticaria |
Examples of stimuli inducing wealing |
|---|---|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
Recurrent angioedema without urticaria can be due to inherited or acquired complement C1 esterase deficiency.
Urticaria is diagnosed in people with a history of weals that last less than 24 hours with or without angioedema. A medication and family history should be elicited. A thorough physical examination should be undertaken.
Skin prick tests and radioallergosorbent tests (RAST) or CAP fluoroimmunoassay may be requested if a drug, latex, or food allergy is suspected in acute urticaria.
There are no routine diagnostic tests in chronic spontaneous urticaria apart from blood count and C-reactive protein (CBC, CRP), but investigations may be undertaken if an underlying disorder is suspected.
The autologous serum skin test is sometimes carried out in chronic spontaneous urticaria, but its value is uncertain. It is positive if an injection of the patient's serum under the skin causes a red weal.
Inducible urticaria is often confirmed by inducing the reaction eg, scratching the skin in dermographism or applying an ice cube in suspected cold urticaria.
Investigations for a systemic condition or autoinflammatory disease should be undertaken in urticaria patients with fever, joint or bone pain, and malaise. Patients with angioedema without weals should be asked if they take ACE inhibitor drugs and tested for complement C4; C1-INH levels, function and antibodies; and C1q.
Biopsy of urticaria can be non-specific. The pathology shows oedema in the dermis and dilated blood vessels, with a variable mixed inflammatory infiltrate. Vessel-wall damage indicates urticarial vasculitis.
The main treatment of all forms of urticaria in adults and children is with an oral second-generation H1-antihistamine such as cetirizine or loratidine. If the standard dose (eg, 10 mg for cetirizine) is not effective, the dose can be increased up to fourfold (eg, 40 mg cetirizine daily). They are stopped when the acute urticaria has settled down. The addition of a second antihistamine is not thought to be helpful.
Terfenadine and astemizole should not be used, as they are cardiotoxic in combination with ketoconazole or erythromycin. They are no longer available in New Zealand.
Although systemic treatment is best avoided during pregnancy and breastfeeding, there have been no reports that second-generation antihistamines cause birth defects. If treatment is required, loratadine and cetirizine are currently preferred.
Conventional first-generation antihistamines such as promethazine or chlorpheniramine are no longer recommended for urticaria.
Identified triggers should be eliminated if possible (eg, drug or food allergy). Avoidance of relevant type 1 (IgE-mediated) allergens clears urticaria within 48 hours.
The physical triggers for inducible urticaria should be minimised; see examples below. However, symptoms often persist.
Some patients with inducible urticaria benefit from daily induction of symptoms to induce tolerance. Phototherapy may relieve the itch of symptomatic dermographism.
If non-sedating antihistamines are not effective, a 4 to 5-day course of oral prednisone (prednisolone) may be warranted in severe acute urticaria.
Intramuscular injection of adrenaline (epinephrine) is reserved for life-threatening anaphylaxis or swelling of the throat.
Patients with chronic urticaria that has failed to respond to maximum-dose second-generation oral antihistamines taken for four weeks should be referred to a dermatologist, immunologist or medical allergy specialist.
There is good evidence to support treatment with omalizumab or ciclosporin, which each have a 65% response rate in antihistamine-resistant patients.
Long-term systemic corticosteroids are not recommended, as high doses are required to reduce symptoms of urticaria and they have inevitable adverse effects that can be serious.
The effectiveness of treatment can be objectively monitored using urticaria control test. Patients are asked to score the physical symptoms of urticaria they have experienced in the previous four weeks, quality of life affected by urticaria, how often treatment was not enough to control symptoms, and overall control of urticaria.
Acute urticaria resolves in hours to days but is often recurrent. Although chronic urticaria clears up in most cases, 15% continue to have wealing at least twice weekly after two years.