Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Amy Stanway, Dermatology Registrar,Waikato Hospital, Hamilton, New Zealand, 2004.
Psoriasis is a common scaly skin condition resulting in red scaly and thickened patches of skin. Flexural psoriasis is sometimes called inverse psoriasis and describes psoriasis localised to the skin folds and genitals. Common sites of flexural psoriasis are:
Many patients have psoriasis affecting other sites, particularly inside the ear canal, behind the ears, through the scalp, and on elbows and knees.
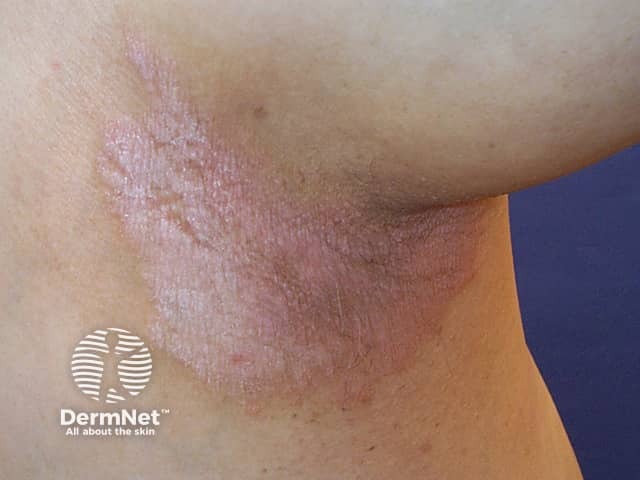
Flexural psoriasis

Flexural psoriasis
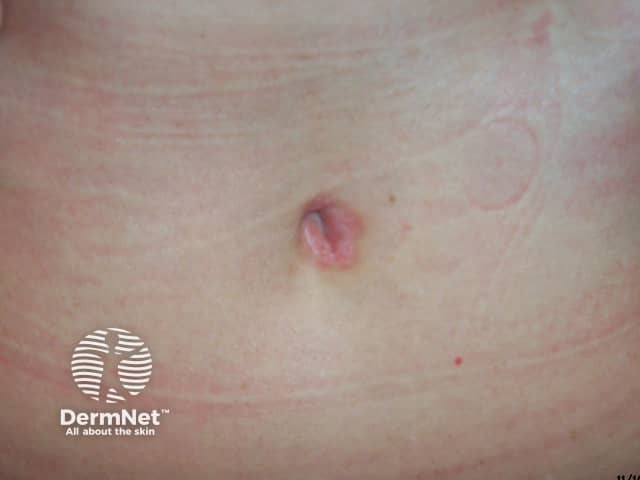
Flexural psoriasis
Due to the moist nature of the skin folds the appearance of the psoriasis is slightly different. It tends not to have silvery scale, but is shiny and smooth. There may be a crack (fissure) in the depth of the skin crease. The deep red colour and well-defined borders characteristic of psoriasis may still be obvious.
Scaly plaques may sometimes occur however, particularly on the circumcised penis.
Flexural psoriasis can be difficult to tell apart from seborrhoeic dermatitis, or may co-exist. Seborrhoeic dermatitis in skin folds tends to present as thin salmon-pink patches that are less well defined than psoriasis. If there is any doubt which is responsible, or there is thought to be overlap of the two conditions, the term sebopsoriasis may be used.
Complications of flexural psoriasis include:
Flexural psoriasis responds quite well to topical treatment but often recurs.
Weak topical steroids (often in combination with an antifungal agent to combat thrush) may clear flexural psoriasis but it will usually recur sometime after discontinuing treatment. Stronger topical steroids need to be used with care and only for a few days, thinly and very accurately applied to the psoriasis. If the psoriasis has cleared, stop the steroid cream. The steroid cream may be used again short-term when the condition recurs.
Overuse of topical steroids in the thin-skinned body folds may cause stretch marks, marked thinning of the skin and can result in long term aggravation of psoriasis (tachyphylaxis).
Calcipotriol cream is an effective and safe treatment for psoriasis in the flexures and should be applied twice daily. If it irritates, it can be applied once daily and hydrocortisone cream 12 hours later.
The topical calcineurin inhibitors, tacrolimus ointment and pimecrolimus cream may be effective and do not cause skin thinning.
Combinations of the treatments listed above may be used, together with emollients. Antiseptics and topical antifungal agents are often recommended as flexural psoriasis may be complicated by bacteria and yeasts, including Candida albicans and Malassezia.
Treatments that are tolerated in other sites are often too irritating to use in skin folds, e.g., dithranol, salicylic acid and coal tar. However, it may be possible to use them by diluting in emollients, or by applying them for short periods and washing off.
The topical phosphodiesterase-4 topical inhibitor, roflumilast, is approved for the treatment of plaque psoriasis (2022). Off-label use of another phosphodiesterase-4 topical inhibitor crisaborole has been shown to be effective for flexural psoriasis.
Systemic agents are rarely required for limited flexural psoriasis.
Phototherapy is relatively ineffective because the folds are hidden from light exposure.