What is pityriasis lichenoides?
Pityriasis lichenoides (PL) is an uncommon cutaneous rash of uncertain aetiology. The acute form, pityriasis lichenoides et varioliformis acuta (PLEVA), and the chronic form, pityriasis lichenoides chronica (PLC), sit at either end of a disease spectrum with many patients showing overlapping features.
The eponym Mucha–Habermann disease is sometimes applied to the entire spectrum of PL but is often reserved for the particularly severe ulcero-necrotic variant of PLEVA.
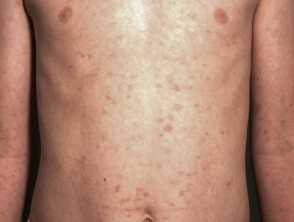
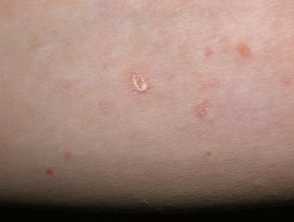
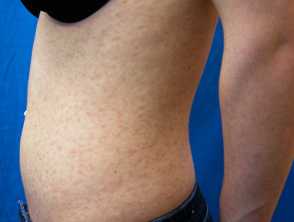
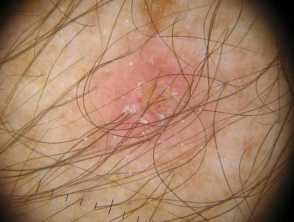
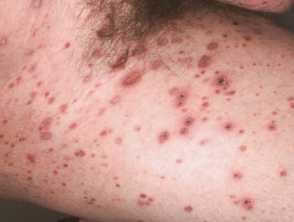
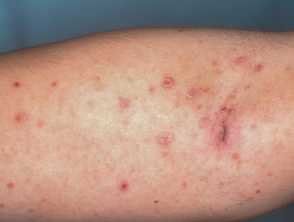
Pityriasis lichenoides chronica images
Click for more images of pityriasis lichenoides
Who gets pityriasis lichenoides?
The incidence of PL is unknown, but the disease is rare. It is most common in children and young adults under age 30 but can present at any age. There is a slight male predominance. All races are affected.
What causes pityriasis lichenoides?
The cause of PL is unknown. The main hypotheses are that it may be:
- A hypersensitivity reaction to an infection, such as:
- Viruses (Epstein-Barr Virus, cytomegalovirus, human immunodeficiency virus)
- Bacteria (Staphylococcus, Streptococcus)
- Parasites (Toxoplasma gondii).
- An inflammatory reaction to medication, such as anti-TNF agents, statins, antidepressants, vaccines, and radiocontrast dye.
- A low-grade lymphoproliferative disorder.
What are the clinical features of pityriasis lichenoides?
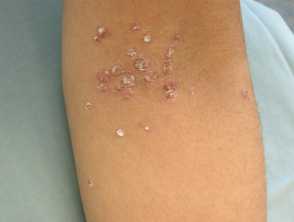
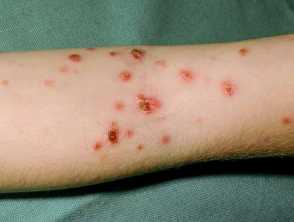
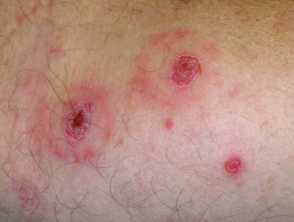
PLEVA presents abruptly with a rapidly progressive rash:
- 10-50 reddish brown, erythematous, ovoid papules, 5-15mm in diameter
- Mainly on the trunk and proximal extremities
- Evolution into vesicles, pustules, haemorrhagic crusts, and ulcers
- Pruritus or burning sensation
- Most cutaneous lesions heal with transient or persistent hyper- or hypo-pigmentation.
- Constitutional symptoms are usually mild (see complications below).
PLC presents more slowly over several days with:
- Larger numbers of small erythematous papules with a brown hue visible on diascopy
- Mica-like scale on more established lesions
- Lesions at various stages of evolution
- Patients often experience periods of relapse and exacerbation.
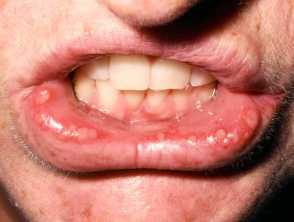
Patients often show features of both PLEVA and PLC, and PLEVA may evolve into PLC. Mucosal lesions have been reported.
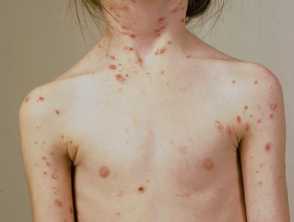
Pityriasis lichenoides acuta
How do clinical features vary in differing types of skin?
Dark-skinned patients, particularly children, may present with widespread hypopigmentation and prominent facial involvement. The definitive signs of pityriasis lichenoides may be very subtle.
What are the complications of pityriasis lichenoides?
- Ulceronecrotic lesions may heal with varioliform scarring.
- A rare severe form of PLEVA (Febrile Ulceronecrotic Mucha–Habermann Disease) has systemic features of malaise, fever, lymphadenopathy, arthritis, and/or bacteraemia. There may be mucosal, gastrointestinal, and pulmonary involvement. Mortality up to 25% is reported.
- The psychological impact should not be overlooked, particularly when skin lesions appear on more easily visible areas such as the face and upper arms.
How is pityriasis lichenoides diagnosed?
The diagnosis can often be made on clinical grounds but is usually confirmed with a skin biopsy, which helps to exclude other important differential diagnoses.
Histological features of PLEVA include:
- A wedge-shaped deep dermal and superficial lymphohistiocytic infiltrate
- Parakeratotic scale and crust, with thinning of the granular layer
- Interface dermatitis with basal cell necrosis and vacuolation
- Epidermal spongiosis and necrosis in more developed lesions
- Extravasated erythrocytes.
In PLC there is usually:
- A superficial dermal infiltrate
- Focal parakeratosis
- Preservation of the granular layer
- Focal loss of the dermo-epidermal interface.
Dermoscopy may be useful, particularly to distinguish PLC from guttate psoriasis or pityriasis rosea.
Other tests, such as screening for viral, bacterial, and toxoplasma infection may be considered, depending on the severity of the presentation.
What is the differential diagnosis for pityriasis lichenoides?
- Lymphomatoid papulosis
- Guttate psoriasis
- Varicella
- Pityriasis rosea
- Arthropod bite reactions
- Lichen planus
- Papular acrodermatitis (Gianotti-Crosti syndrome)
- Hypopigmented mycosis fungoides
What is the treatment for pityriasis lichenoides?
It is important to recognise that there have been no randomised controlled trials regarding treatment, and the natural history of pityriasis lichenoides makes interpretation of anecdotal reports difficult.
- PLEVA is most commonly treated with prolonged courses of erythromycin (in young children) or doxycycline. They are used for their anti-inflammatory effects rather than their antibacterial properties.
- Topical corticosteroids are of little value.
- Antihistamines may reduce itch.
- Phototherapy, usually narrowband UVB, is often the preferred treatment for pityriasis lichenoides chronica.
- Methotrexate and other immunosuppressive agents may be considered for refractory or very severe cases.
What is the outcome for pityriasis lichenoides?
Pityriasis lichenoides et varioliformis acuta typically resolves within a few weeks. However, this can be variable and PLEVA may evolve into PLC or a scar. Pityriasis lichenoides chronica typically lasts several months, but some cases can wax and wane for several years.