Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Vanessa Ngan, Staff Writer, 2003. Updated by A/Prof Amanda Oakley, Chief Editor, January 2016. DermNet Revision April 2021
Introduction Demographics Causes Clinical features Diagnosis Differential diagnoses Treatment Outcome
An aphthous ulcer is the most common ulcerative condition of the oral mucosa, and presents as a painful punched-out sore on oral or genital mucous membranes. They are also called aphthae, aphthosis, aphthous stomatitis and canker sores.
Anyone can get an aphthous ulcer; 20% of the population have one or more, at least occasionally. They usually first appear in childhood or adolescence, and more commonly affect females than males.
Aphthous ulcers can be an early manifestation of a systemic disease such as Behçet disease, or gastrointestinal disorders including coeliac disease, Crohn disease, and ulcerative colitis. Aphthous stomatitis is a feature of the recurrent fever syndrome PFAPA syndrome.
Interestingly, smoking may be protective against aphthae, even though smoking makes many oral and skin conditions worse.
The exact reason why aphthous ulcer develops is not yet clearly defined. Approximately 40% of people who get aphthous ulcers have a family history of aphthous ulcers. Current thinking is that the immune system is disturbed by some external factor and reacts abnormally against a protein in mucosal tissue.
Factors that seem to trigger outbreaks of ulcers include:
An aphthous ulcer is typically a solitary round or oval punched-out sore or ulcer inside the mouth on an area where the mucosa is not tightly bound to the underlying bone, such as on the inside of the lips and cheeks or underneath the tongue. Aphthous ulcers can also affect the genitalia in males and females.
Recurrent aphthous ulcer usually begins as a round yellowish elevated spot surrounded by a red halo. This then breaks down into a punched-out ulcer, which is covered with a loosely attached white, yellow, or greyish membrane. Surrounding tissue is healthy and unaffected. The ulcer can be painful, particularly if irritated by movement or eating certain types of food such as citrus fruit.
People may experience a single ulcer or multiple ulcers. Multiple ulcers tend to be widely distributed throughout a person's mouth.
Aphthous ulceration is classified into three types.
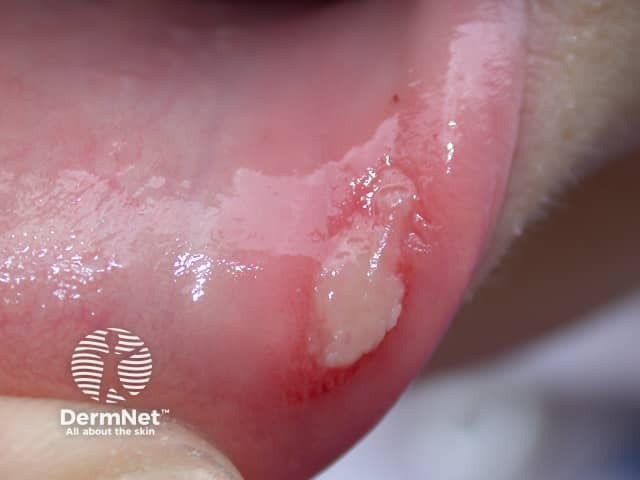
Aphthous ulcer

Aphthous ulceration

Aphthous ulceration
Aphthous ulcers are usually diagnosed clinically. Investigations are rarely required, but are undertaken if there are recurrent attacks of multiple or severe oral ulcers or complex aphthosis.
Blood tests may include:
Swabs for microbiology evaluate the presence of Candida albicans, Herpes simplex virus and Vincent's organisms.
Other causes of mouth ulcer should be considered, including:

Hand foot and mouth disease

Fixed drug eruption

Herpangina
There is no cure for an aphthous ulcer and the ulcers heal spontaneously. The main goal of treatment is to lessen pain and discomfort and promote healing.
Topical prescription medicines are rarely required:
In severe cases, particularly if there are systemic symptoms, oral medications with anti-inflammatory activity may be considered (off-label use):
Most recurrent minor aphthous ulcers heal within 1–2 weeks without scarring without any treatment. Minor aphthous ulcers commonly recur intermittently.
Recurrent aphthous ulcers are mostly a minor nuisance, but they are associated with significant health problems in some people.
Major aphthous ulcer heals with scarring.