What is hand, foot, and mouth disease?
Hand, foot, and mouth disease (HFMD or HFM) is a common, self-limiting, viral infection that causes blisters on the hands, feet, and inside or around the mouth. It mainly affects children under the age of 5 years.
HFMD, also called enteroviral vesicular stomatitis, occurs sporadically worldwide. Epidemics are most common during warm weather, usually in the late summer or early autumn.
It is important to note that HFMD is NOT related to foot and mouth disease of animals.
Who gets hand, foot, and mouth disease?
HFMD mostly occurs in children under 10 years of age with 95% of the cases occurring in toddlers aged under 5 years. However, it can also affect older children/adolescents. Adults, especially those who are immunocompromised, may also be affected. However, HFMD only rarely affects healthy adults.
Hand, foot, and mouth disease is very common. The average annual incidence of HFMD has been reported as 90–2400 cases per 100,000 people in some countries.
What causes hand, foot, and mouth disease?
Enteroviral vesicular stomatitis (HFMD) is usually caused by the Coxsackie virus, most commonly the A16 subtype. It may also be caused by other viruses such as:
- Coxsackie A virus (5, 6, 7, 9, 10)
- Coxsackie B virus (2, 5)
- Enterovirus 71
- Echoviruses.
Enterovirus 71 infection is associated with more severe infections that may involve the heart, lungs, and can also cause inflammation of the lining of the brain (meningitis).
Transmission occurs via direct contact with blister fluid or droplets spread from the mouth. It can spread very rapidly among family members or within a school. The virus can be shed in faeces and saliva for several weeks.
What are the clinical features of hand, foot, and mouth disease?
The illness usually begins with one or all of the following: fever, sore throat, loss of appetite, and lethargy. However, many children remain well in themselves despite the rash. The blisters usually appear 1–2 days following the fever.
The incubation period is typically 3–6 days and children remain infectious until the blisters have ruptured and healed (usually 7–10 days).
Skin findings typically include:
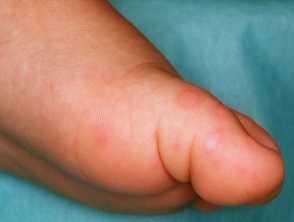
- Blisters on the tops of the hands, feet and/or palms, and soles. Lesions usually:
- Feel tender
- Evolve over time from flat pink macules to small, elongated, red-greyish blisters
- Are often oval rather than round
- Peel off within a week, without leaving a scar.
- Small blisters (vesicles) and ulcers may develop in and/or around the lips and mouth and the back of the throat. These can sometimes be very painful. Oral intake may be significantly impacted, especially in infants and younger children.
- In children with eczema, or past eczema, blisters, flat red macules and papules may develop over other areas of the skin, especially the buttocks and sometimes on the arms, legs, and genital skin.
Atypical HFMD can result in a more widespread rash and blistering. Features may include:
- Red, crusted macules and papules without blistering
- Large blisters (bulla)
- Targetoid (bulls-eye, or target-shaped) lesions
- Nail shedding
- Involvement of atypical or unusual sites such as the ears.
Hand, foot, and mouth disease
How do clinical features vary in differing types of skin?
In children with pre-existing eczema (atopic dermatitis), HFMD lesions may be localised in eczematous areas (eczema coxsackium).
What are the complications of hand, foot, and mouth disease?
Severe complications are very uncommon in people that are otherwise healthy. They include:
- Dehydration due to inadequate fluid intake. This can cause significant problems in younger children.
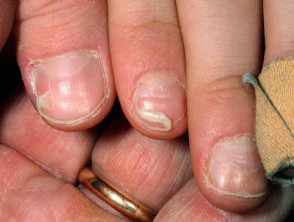
- Fingernail and toenail changes are often noted about two months after HFMD infections due to coxsackie A6 infection.
- Transverse lines in the nail plate that slowly move outwards
- Onychomadesis (nail shedding) may occur about 2 months after the illness, however, eventually the nails return to normal.
Serious enteroviral infection can lead to:
- Widespread blistering
- Enteritis
- Myocarditis
- Inflammation of the brain and or the lining of the brain (meningoencephalitis)
- Loss of nerve function in a limb (acute flaccid paralysis)
- Pulmonary oedema and pneumonia
- Haemorrhagic conjunctivitis
- In pregnancy, viruses that cause HFMD can cause first trimester spontaneous miscarriage or intrauterine growth restriction
- Meningoencephalitis, thrombocytopenia, disseminated intravascular coagulopathy, cardiomyopathy and hepatitis in the newborn have rarely been described.
How is hand, foot, and mouth disease diagnosed?
HFMD is usually diagnosed clinically. Cutaneous lesions are typically distributed symmetrically over common sites of the skin such as the hands, feet, and in and around the mouth in a child.
Other diagnostic tools include:
- Polymerase chain reaction (PCR) testing
- Viral DNA may be detected from nasopharyngeal, (throat or nose), swabs and stool specimens.
- Analysis of blood, cerebrospinal fluid (CSF), and faeces samples can confirm the diagnosis, but are rarely needed except in atypical or severe cases.
- Skin biopsy of a blister
- Very rarely indicated.
- Shows acral skin with lymphocytic infiltrates at the epidermis.
- The infiltrate is associated with keratinocyte apoptosis in early lesions.
See hand, foot, and mouth disease pathology for more information.
What is the differential diagnosis for hand, foot, and mouth disease?
- Bacterial infections: such as Group A Streptococcus and Staphylococcus aureus, may cause similar blistering skin lesions, eg, bullous impetigo.
- Other viral infections such as human parechoviruses, herpes simplex virus, adenoviruses, varicella zoster virus, Epstein-Barr virus, and human herpesvirus 6 and 7.
- Bullous insect bite reactions may also present on the hands and feet in children.
- Pompholyx eczema.
What is the treatment for hand, foot, and mouth disease?
Specific treatment is not usually required for HFMD, and the focus is symptomatic care. HFMD rarely causes serious complications. Antibiotics do not work and should not be given to children with HFMD.
No vaccines or specific antiviral medications are available.
General measures
Pain relief
- Simple analgesia such as paracetamol or ibuprofen as needed.
- Antiseptic mouthwashes or topical soothing agents (eg, lignocaine) can be used in children with painful oral/palatal ulcers.
- Aspirin should not be used routinely due to the risk of Reye syndrome.
Hydration
- Constantly offer the child sips of water/juice to prevent dehydration.
- If oral intake is poor, nasogastric or intravenous fluids may be indicated.
Blister care
- Leave blisters to dry naturally.
- Do not pierce/rupture the blisters to reduce contagion.
- Keep the blisters clean and apply non-adherent dressings to erosions.
Should children with hand, foot, and mouth disease stay home from school?
In the vast majority of cases, HFMD is a mild illness and there is no need to keep children from school once they are well enough to attend.
The blisters remain infective until they have dried, which is usually within a few days. However, the virus sheds through faecal stools and these remain infective for up to a month after the illness. Therefore, it is impractical to keep children who are well away from school.
General preventative measures include:
- Thorough hand hygiene especially after coming into contact with one’s bodily fluid.
- This includes touching their blisters, helping them to blow their nose and changing nappies or helping with toileting.
- Minimise sharing personal items such as cutlery, drinking cups, towels, toothbrushes, and clothing.
What is the outcome for hand, foot, and mouth disease?
HFMD infection is usually mild and complete resolution is seen within 7–10 days. Infection often results in long-term immunity to the specific virus, however a second episode can occur following infection with a different member of the enterovirus group.