Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Hon A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand, 2003. Updated by Dr Sara de Menezes, Basic Physician Trainee, Alfred Health, Melbourne, Australia. December 2016.
Introduction
Clinical features
Demographics
Underlying mechanisms
Causes
Diagnosis
Treatment
Outcome
Pruritus is the medical term for itch. Itch is an unpleasant sensation on the skin that provokes the desire to rub or scratch the area to obtain relief. Itch can cause discomfort and frustration; in severe cases it can lead to disturbed sleep, anxiety and depression. Constant scratching to obtain relief can damage the skin (excoriation, lichenification) and reduce its effectiveness as a major protective barrier.
Pruritus is often a symptom of an underlying disease process such as a skin problem, a systemic disease, or abnormal nerve impulses.
There are no specific skin signs associated with pruritus, apart from scratch marks (excoriations) and signs of the underlying condition.
Persistent scratching over a period of time may lead to:
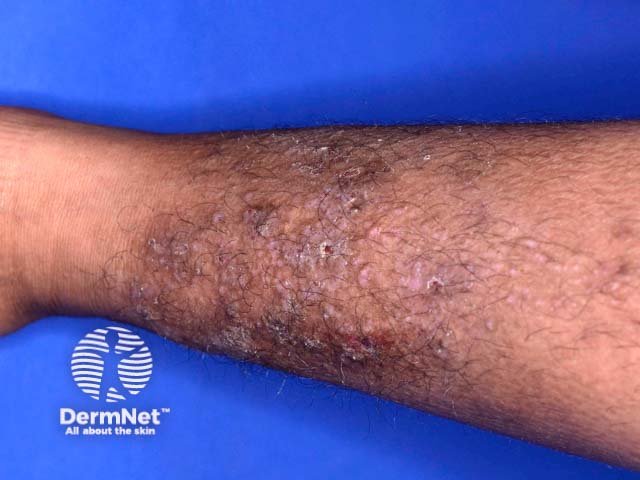
Lichen simplex
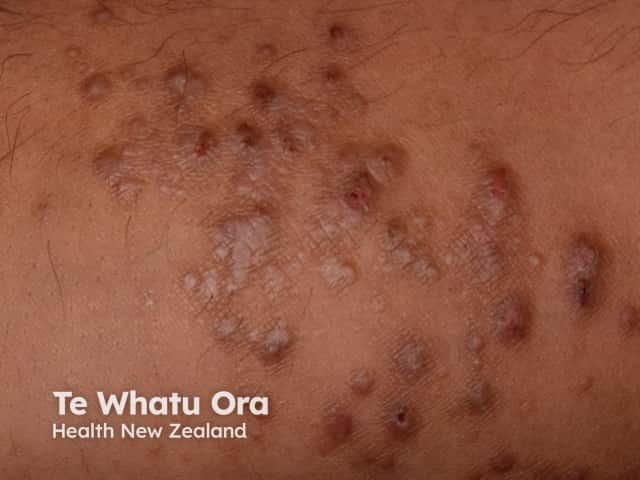
Nodular prurigo

Excoriations and bruises
The epidemiology of pruritus depends on its underlying cause or causes. However, in general, the incidence of chronic pruritus increases with age, it is more common in women, and in those of Asian background.
Itch, like pain, can originate anywhere along the neural itch pathway, from the central nervous system (brain and spinal cord) to the peripheral nervous system and the skin.
Mechanisms underlying pruritus are complex.
The way scratching stops itching has been explained by an interaction with pain pathways within the dorsal horn of the spinal cord.
Causes of pruritus can be classified under 5 main headings.
Localised pruritus is pruritus that is confined to a certain part of the body. It can occur in association with a primary rash (eg dermatitis) or may occur because of hypersensitive nerves in the skin (neuropathic pruritus). Neuropathic pruritus is due to compression or degeneration of nerves in the skin, on route to the spine or in the spine itself. Neuropathic itch is sometimes associated with reduced or absent sweating in the affected area of skin.
Typical causes of localised itchy rashes
Neuropathic causes of localised pruritus without primary rash (cutaneous dysaesthesia)
Scratching a localised itch may lead to lichen simplex, prurigo or prurigo nodularis.
Systemic diseases may cause generalised pruritus. This is sometimes called metabolic itch. There is nothing wrong with the skin itself, at least until it's been scratched.
Metabolic disorders include chronic renal failure (dialysis) and liver disease (with or without cholestasis).
Haematological disorders include iron deficiency anaemia and polycythaemia vera.
Endocrine disorders include thyroid disease and diabetes mellitus.
Paraneoplastic itch is associated with lymphoma, especially Hodgkin lymphoma, leukaemia or a solid organ tumour (eg lung, colon, brain).
Infections causing itch include human immunodeficiency virus infection (HIV) and hepatitis C virus.
Pruritus is often a symptom of many skin diseases. Some of these are included in the following list.
Pruritus may arise as a result of exposure to certain external factors.
About 2% of pregnant women have pruritus without any obvious dermatological cause. In some cases the itch is due to cholestasis (pooling of bile in the gall bladder and liver). It usually occurs in the 3rd trimester and is relieved after giving birth.
Generalised itch is also a common symptom of menopause.
The first steps of evaluation of an itchy patient are medical history and examination.
A thorough history can identify constitutional symptoms that may point towards an underlying systemic disease. Drug triggers such as opioids may be identified, especially if the commencement of the drug relates to the itch.
A careful examination can identify dermatological causes for the itch (eg scabies, lichen simplex, pemphigoid) or evidence of chronic skin changes related to the itch. In dermatological causes of pruritus, primary skin lesions will usually suggest the diagnosis. Patients without primary skin lesions and little evidence of chronic scratching should be investigated for systemic, neuropathic and psychogenic causes.
The panel of investigations could include:
The management of pruritus relies on establishing the cause and then either removing or treating the cause to prevent further itching. In many cases, tests are necessary to determine the cause; while these are in progress, treatment to provide symptomatic relief of pruritus may be given.
In addition to specific therapy for any underlying skin or internal disease, topical treatment may include:
Other measures that can be useful in preventing pruritus include avoiding precipitating factors such as rough clothing or fabrics, overheating, and vasodilators if they provoke itching (eg, caffeine, alcohol, spices). Fingernails should be kept short and clean. If the urge to scratch is irresistible then rub the area with your palm.
Topical antihistamines should not be used for chronic itch, as they may sensitise the skin and result in allergic contact dermatitis.
If pruritus is severe and sleep is disturbed treatment with oral medication may be necessary. Some drugs may help to relieve the itch whilst others are given solely for their sedative effects.
Ultraviolet B (UVB) phototherapy alone, or in conjunction with UVA, has been shown to be helpful for pruritus associated with chronic kidney disease, psoriasis, atopic eczema and cutaneous T-cell lymphoma.
Behavioural therapy may be used in conjunction with pharmacotherapy to modify behaviours such as coping mechanisms and stress reduction, which help interrupt the itch-scratch cycle. One randomised controlled trial showed short-term benefits with a reduction in itch frequency and scratching as well as improvement in coping mechanisms.
The management of chronic severe itch is difficult and often requires the use of combination therapy over a long period of time. Identification and treatment of underlying conditions causing pruritus may help in this process. The symptom may quickly disappear or persist for long periods of time.