Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Nicole A. Seebacher, Department of Oncology, University of Oxford, United Kingdom, U.K. (2022)
Previous contributors: Dr Amanda Oakley, Dermatologist (1997)
Reviewing dermatologist: Dr Ian Coulson
Edited by the DermNet content department
Introduction
Demographics
Causes
Classification
Clinical features
Variation in skin types
Complications
Diagnosis
Differential diagnoses
Treatment
Lymph node removal
Follow-up
Prevention
Outcome
Melanoma, also referred to as malignant melanoma, is a potentially very serious skin cancer in which there is an uncontrolled growth of melanocytes (pigment cells).
Normal melanocytes are found in the basal layer of the epidermis (outer layer of skin). Melanocytes produce a protein called melanin, which protects skin cells by absorbing ultraviolet (UV) radiation.
Non-cancerous growth of melanocytes results in moles (benign melanocytic naevi) and freckles (ephelides and lentigines). In contrast, the cancerous growth of melanocytes results in melanoma. Melanoma is described as:
Management of melanoma is rapidly evolving. For up-to-date recommendations for the diagnosis and management of melanoma, refer to local guidelines such as the Australian Cancer Council clinical practice guidelines.
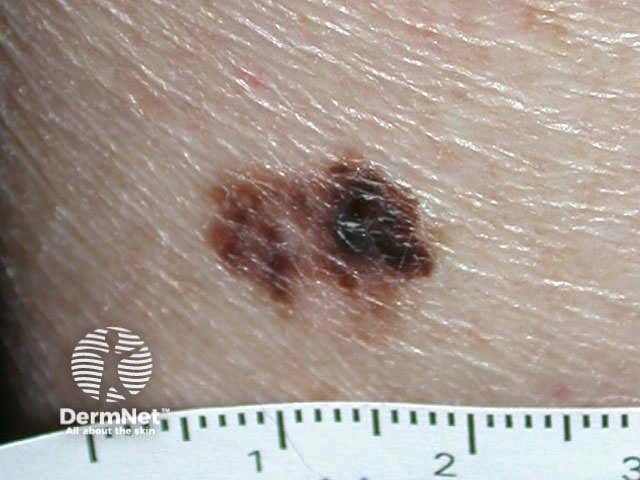
Superficial spreading malignant melanoma - irregular border, variable pigmentation, and areas of clinical regression

Superficial spreading malignant melanoma - an enlarging pigmented lesion with variable pigmentation, irregular edge, and asymmetry
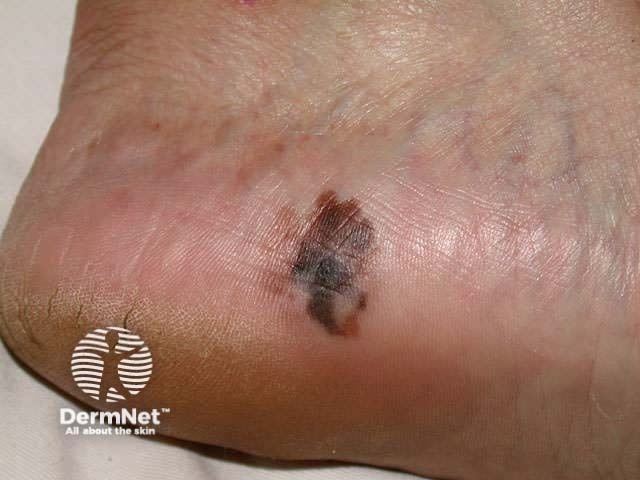
Acral lentiginous malignant melanoma - irregular edge, with variable pigmentation, asymmetry and areas of regression on the heel
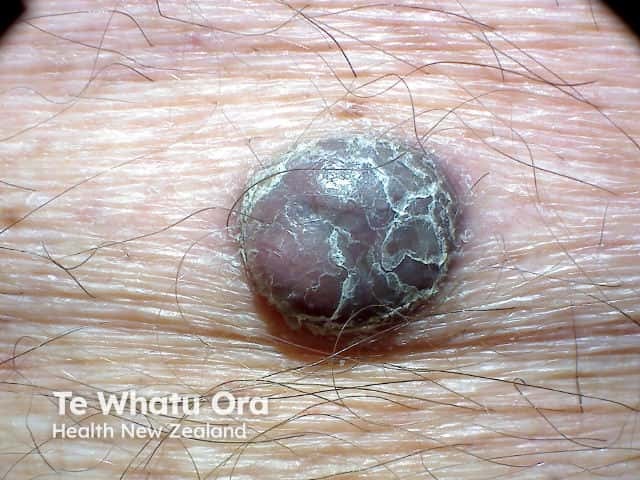
Nodular malignant melanoma in a vertical growth phase - rapidly enlarging scaly pigmented nodule
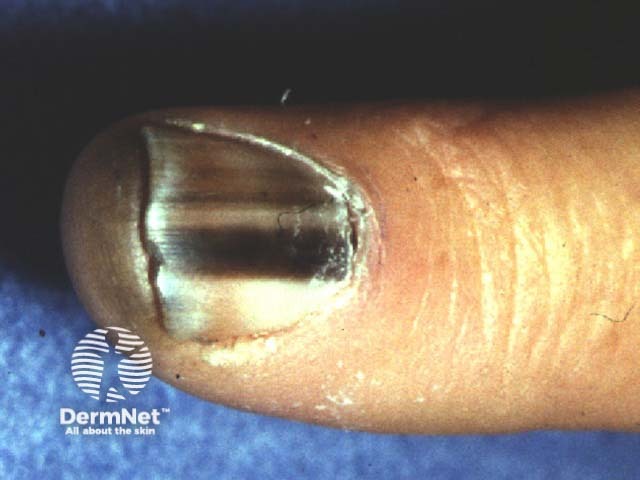
Irregular pigmented longitudinal bands in melanoma of the nail unit
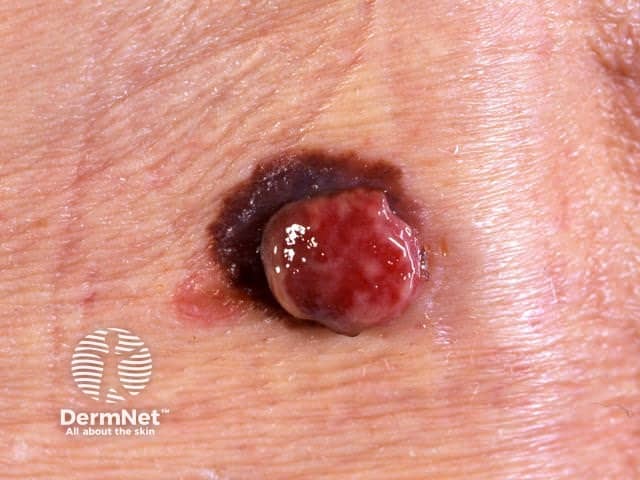
Amelanotic melanoma arising within pigmented melanoma
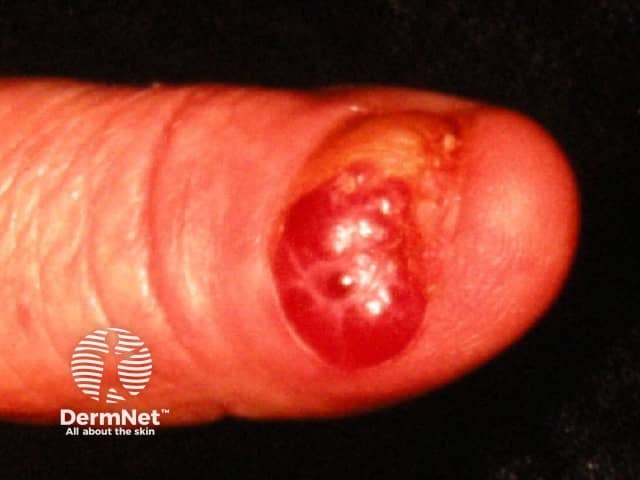
Amelanotic subungal melanoma - a red lesion arising from the nail fold that has produced destruction of the nail plate
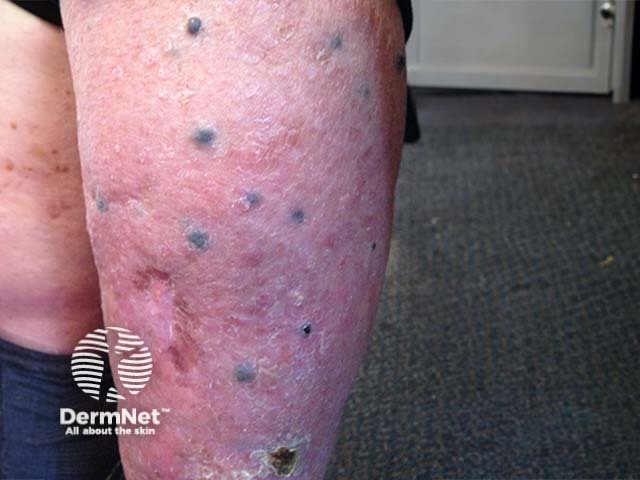
Multiple blue nodules of cutaneous metastatic malignant melanoma
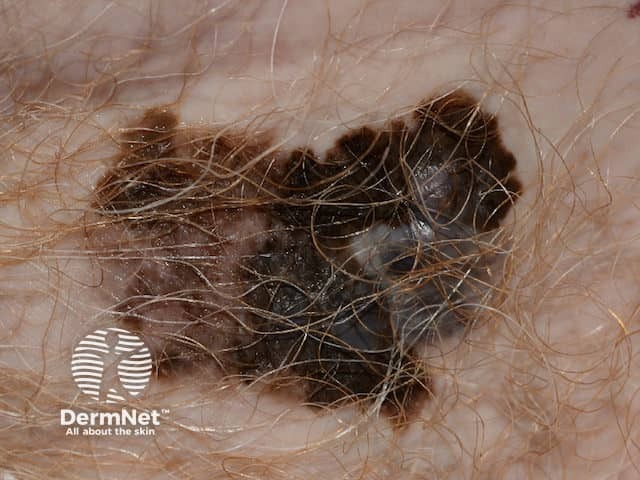
A superficial malignant melanoma - irregular and notched margin, variable and irregular pigmentation in an itchy and enlarging pigmented lesion
For more images, please see links at the bottom of the page.
Australia and New Zealand have the highest reported incidence and mortality of melanoma globally. About 1 in 15-18 white-skinned Australians and New Zealanders are expected to develop melanoma in their lifetime. Melanoma is the third most common cancer in Australia and New Zealand.
In 2019, there were 2,727 melanoma registrations in New Zealand. There were 362 deaths from melanoma in 2016.
Melanoma can occur in adults of any age but is very rare in children. According to the Australian Institute of Health and Welfare, in 2021:
The mean age for melanoma diagnosis is 65.7 years among men and 62.4 years among women. Melanoma is the most common cancer diagnosed in young Australians aged 15–29 years, accounting for 15% of all cancers in this age group.
The main risk factors for developing the more common type of melanoma (eg, superficial spreading melanoma) include:
These risk factors are not as relevant to rarer types of melanoma.
Although the presence of a large number of common nevi is a strong risk factor for cutaneous melanoma, the majority of melanomas arise de novo. A 2017 meta-analysis of 38 studies including over 20,000 melanomas found that only 29 percent were nevus-associated, with the rest arising de novo.
Melanoma is thought to begin as an uncontrolled proliferation of melanin-producing cells (melanocytic stem cells) that have undergone a genetic transformation.
The cause of these cell mutations can be acquired or inherited.
Cutaneous melanoma can arise from otherwise normal-appearing skin (in about 75% of melanomas) or from within a pre-existing mole or freckle, which starts to grow larger and change in appearance. Precursor lesions include:
Melanomas have two growth phases, radial and vertical. Most melanomas arise as superficial tumours confined to the epidermis (ie, they have a horizontal growth phase; in situ). These generally grow slowly, but at any time, further genetic changes may cause the tumour to progress to the vertical growth phase, in which the malignant cells breach the basement membrane, invading deeper tissues, resulting in invasive melanoma.
Once the melanoma cells have reached the dermis, they may spread to other tissues via the lymphatic system to the local lymph nodes or via the bloodstream to other organs such as the lungs or brain. This is known as metastatic disease or secondary spread. The chance of this happening mainly depends on how deep the cells have penetrated the skin.
In 2018, the World Health Organization (WHO) revised the classification of melanoma, distinguishing them by their cumulative solar damage (CSD), anatomic site, epidemiology and mutation signatures. These now include low and high CSD melanomas, desmoplastic melanoma, Spitz melanomas, acral melanomas, mucosal melanomas, melanomas in congenital nevus, melanomas in blue nevus, and uveal melanomas.
The more traditional morphologic classification by histopathology of melanoma, includes the subtypes:
Less common variants include:
Combinations may also occur, for example, nodular melanoma arising within a superficial spreading melanoma.
Melanoma is usually epithelial in origin ie, starting in the skin or, less often, mucous membranes. However, very rarely, melanoma can start in an internal tissue such as the brain (primary CNS melanoma) or the back of the eye.
Melanoma can also be classified according to its relationship with age.
Melanomas can occur anywhere on the body, not only in areas that get a lot of sun. In New Zealand, the most common site in men is the back (around 40% of melanomas in men), and the most common site in women is the leg (around 35% of melanomas in women).
Although melanoma usually starts as a skin lesion, it can also grow on mucous membranes (mucosal melanoma), such as the lips or genitals. Occasionally it occurs in other parts of the body such as the eye, brain, mouth or vagina.
The first sign of a melanoma is usually an unusual looking freckle or mole and may itch or bleed. Melanomas may grow across the skin (known as the radial growth phase) or grow in depth (known as the vertical growth phase).
Melanoma may be detected at an early stage when it is only a few millimetres in diameter, but it may grow to several centimetres in diameter before it is diagnosed.
A melanoma may have a variety of colours including:
During its horizontal phase of growth, a melanoma is normally flat. As the vertical phase develops, the melanoma becomes thickened, raised, and palpable.
Some melanomas are itchy or tender. More advanced lesions may bleed easily or crust over.
Most melanomas have characteristics described by the ABCDE+EFG melanoma criteria or the Glasgow 7-point checklist.
For superficial melanomas — ABCDE signs
A: Asymmetry of shape and colour
B: Border irregularity, including smudgy or ill-defined margin
C: Colour variation and change
D: Different (formerly diameter)
E: Evolving (enlarging, changing)
Melanomas may not conform to the 'ABCD' rule alone. For nodular melanomas, also consider the EFG signs
E: Elevated
F: Firm to touch
G: Growing
See ABCDE+EFG criteria.
Taking a thorough history is important, and any lesion that changes in size, shape, colour, or elevation for more than one month should be reviewed by a dermatologist or biopsied.
Major features
Minor features
White or pale skin colour is an independent but significant risk factor for melanoma across diverse ethnic groups. However, people of all skin colours with a family history of melanoma are at increased risk of developing melanoma due to a genetic predisposition.
In skin of colour, it can be harder to identify melanomas, their growth phase, and their pattern as the surrounding skin may mask or match the colour of the melanoma.
People with skin of colour tend to have:
This topic is further discussed on the melanoma of skin colour page.
Complications due to surgery:
Melanoma may be suspected because of a lesion's clinical features or a history of change.
A thorough history and skin examination will be performed using the "ugly duckling" sign, ABCDE rule, and the Glasgow revised seven-point checklist (described above). This may be supported by dermoscopy, confocal microscopy, total body photography (mole mapping), and adhesive patch genomic analysis, among other methods.
Histopathology is required for the definitive diagnosis of melanoma.
Where possible, suspicious lesions should be surgically removed by diagnostic excision with a 2 mm clinical margin and upper subcutis for pathological examination. A partial (incisional) biopsy is best avoided but may be considered where complete excision is not feasible, eg, large lesions. Nail biopsy for suspected melanoma of the nail is discussed elsewhere.
The pathological diagnosis of melanoma can be very difficult. Immunohistochemical stains may help confirm melanoma and include S-100, SOX10, MART-1, HMB-45, MITF, tyrosinase and PRAME. Also, molecular techniques such as gene expression profiling and fluorescence in situ hybridisation (FISH), may aid in diagnosis.
If there is invasive melanoma, the pathologist will comment on:
The report may also include comments about the cell type, growth pattern, invasion of blood vessels or nerves, inflammatory response, regression, associated in-situ disease and any associated naevus (original mole).
Melanoma staging means finding out if the melanoma has spread from its original site in the skin. Most melanoma specialists refer to the American Joint Committee on Cancer (AJCC) cutaneous melanoma staging guidelines (8th edition, 2018). In summary, the stages are:
Stage |
Characteristics |
|
|---|---|---|
Stage 0 |
In situ melanoma |
|
Stage 1 |
Thin melanoma 2 mm in thickness |
|
Stage 2 |
Thick melanoma > 2 mm in thickness, or > 1mm thickness with ulceration |
|
Stage 3 |
Melanoma spread to involve local lymph nodes |
|
Stage 4 |
Distant metastases have been detected |
|
A dermatologist and oncologist may both be involved to provide a recommended treatment option based on the melanoma stage and other factors such as age and general health.
Surgery is the most common treatment for early-stage (Stage 0, I or II) melanoma. If caught early, 90% of melanomas can be cured with simple surgery alone.
More advanced melanomas (Stage III or IV) may require a combination of treatments, including surgery, drug therapy, and radiation therapy. All melanoma patients with distant metastases should be reviewed by a multidisciplinary team to ensure an optimal treatment combination.
Melanoma therapy is rapidly evolving with the frequent availability of new and more effective treatments. Access to these new treatments is dependent on the results of clinical trials and approval by government bodies. For an up-to-date summary of therapies available, please refer to your local guideline such as the Australian Cancer Council clinical practice guidelines for the diagnosis and management of melanoma.
Following confirmation of the diagnosis, wide local excision is carried out at the primary melanoma site. The extent of surgery depends on the thickness of the melanoma and its site.
Margins recommended in New Zealand (2013):
Australian Clinical Practice Guidelines for the diagnosis and management of melanoma (updated 2018), recommend, where possible:
If the melanoma is widespread, surgical treatment is not always successful in eradicating cancer. Some patients may be offered new or experimental treatments. Currently, there are two main types of drug therapy used to treat melanoma:
Immunotherapy/immune-modulating therapy
For a more detailed summary of the immunotherapy agents currently available, see the Cancer Research Institute website.
Chemotherapy is rarely used in Australia and New Zealand for melanoma management.
Radiation therapy is a localised treatment that uses high-energy radiation to kill cancer cells. It may be given on its own (when the patient has a melanoma too widespread for surgery or is unfit for surgery), after surgery (particularly when there is a high risk of recurrence) or as a combination therapy.
Radiation therapy should be considered in patients with a single or small number of brain metastases, painful bone metastases, problematic skin, soft tissue or nodal metastases that have not responded to systemic therapy. This may help relieve symptoms from the metastases.
In Australia and New Zealand, it is recommended that lymphatic mapping with a sentinel node biopsy is performed for melanomas thicker than 1 mm or where the melanoma is greater than 0.75 mm with other high-risk pathological features. However, while the biopsy may help in staging cancer and directing the use of adjuvant therapies, it does not offer any survival advantage.
When the sentinel node is removed it is assessed for the presence of malignant cells, which may indicate melanoma spread to other body parts. In the past, a positive sentinel node biopsy required a lymph node dissection to remove all the lymph nodes in the area. However, this is no longer the preferred treatment. Patients may choose to have the procedure to reduce the risk of lymph node field relapse.
Follow-up after a melanoma diagnosis is required to:
The current Cancer Council Australia and Melanoma Institute Australia (2022) Clinical Guidelines make the following recommendations for follow-up for patients with invasive melanoma:
The follow-up appointments may be undertaken by the patient's general practitioner and specialist. Follow-up appointments may include:
In those with more advanced primary disease, follow-up may include:
Most tests are not worthwhile for patients with stage 1 or 2 melanoma unless there are signs or symptoms of disease recurrence or metastasis. No tests are necessary for healthy patients who have remained well for five years or longer after the removal of their melanoma.
Preventative measures involve addressing risk factors such as exposure to UV radiation, eg, wearing protective clothing, using sunscreen (SPF 50), and avoiding tanning beds. For more information, see skin cancer.
Melanoma in situ is cured by excision because it has no potential to spread around the body.
The risk of spread and ultimate death from invasive melanoma depends on several factors, including anatomic location, pathologic factors, and mutation status. However, the main factor is the Breslow thickness of the melanoma at the time it was surgically removed.
Metastases are rare for melanomas < 0.75 mm in size, and the risk associated with tumours 0.75–1 mm thick is about 5%. The risk steadily increases with thickness so that melanomas > 4 mm have a risk of metastasis of about 40%.
For images, see the following links:
Superficial spreading melanoma images