What is mycetoma?
Mycetoma is a chronic infection of the skin and the subcutaneous tissue. It can sometimes also affect muscles, bones, tendons and joints.
Mycetoma is characterised by nodules and sinus tracts that discharge watery fluid or pus containing grains [1].
Mycetoma is classified as:
- Eumycetoma — when it is caused by a fungus;
- Actinomycetoma— when it is caused by filamentous bacteria from the order, actinomycetes.
Mycetoma
Who gets mycetoma?
The bacteria and fungi causing mycetoma have a worldwide distribution in the soil and plant material, but mycetoma is mostly found in tropical areas in south and south-east Asia, Latin America and Africa. Most cases are reported in the ‘Trans-African mycetoma belt” from western Africa, including Senegal and Sierra Leone, to eastern Africa, including Somalia and Sudan [2,3].
Infection usually occurs after local trauma.
- Eumycetoma mainly affects middle-aged men that work as herdsmen or farmers, especially when walking barefoot.
- Mycetoma can also affect younger men and females.
- Actinomycetoma can also be related to oral infections, teeth or gum disease.
Mycetoma has no known vector or animal reservoir, and there are no reports of infections transmitted from person to person [1,3].
What causes mycetoma?
The causative agent can be suspected from the colour of the grains.
Eumycetoma
Dark or black grains
- Madurella mycetomatis
- Trematosphaeria grisea (formerly Madurella grisea)
- Exophiala jeanselmei
- Medicopsis romeroi (formerly Pyrenochaeta romeroi)
- Falciformispora senegalensis (formerly Leptosphaeria senegalensis)
- Falciformispora thompkinsii
- Curvularia lunata
White, pail or unstained grains
- Acremonium spp.
- Fusarium spp
- Neotestudina rosatii
- Aspergillus nidulans
- Aspergillus flavus
- Microsporum ferrugineum
- Microsporum audouinii
- Microsporum langeronii
- Scedosporium apiospermum
- Scedosporium boydii (formerly Pseudallescheria boydii)
Actinomycetoma
White to yellow grains
- Nocardia brasiliensis
- Nocardia otitidiscaviarum (formerly Nocardia caviae)
- Actinomadura madurae
- Pleurostomophora ochracea
Brown grains
- Streptomcyes somaliensis
Red to pink grains
- Actinomadura pelletieri
What are the clinical features of mycetoma?
The incubation time after inoculation of the microorganism until mycetoma is diagnosed ranges from months to years [2].
Actinomycetoma and eumycetoma have similar clinical features. However, actinomycetomas tend to be more aggressive and destructive, invading bones earlier.
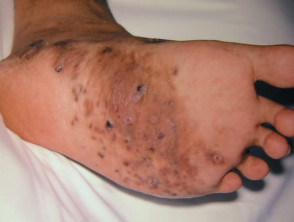
- Mycetoma starts as a localised swelling on an exposed site; two thirds arise on the foot.
- The affected area has normal skin temperature and is often hyperpigmented.
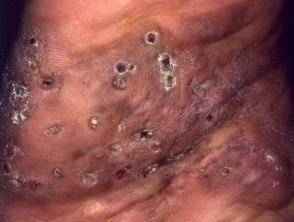
- Multiple firm nodules appear and start to drain spontaneously or following pressure.
- The fluid discharged from sinus tract can contain the characteristic granular grains.
- Local pain is mild or absent, and it worsens only in later stages with more subcutaneous tissue damage or with secondary bacterial infection.
Mycetoma has little effect on the general condition of the affected patient and fever is rare [2].
Actinomycetoma
What are the complications of mycetoma?
Complications of mycetoma include:
- Secondary bacterial infection
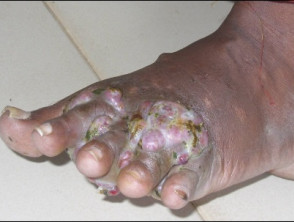
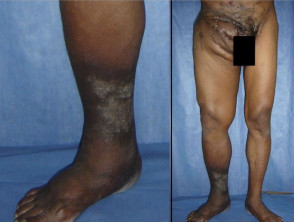
- Bizarre massive swelling with deformity
- Joint ankylosis and loss of function
- Chronic oedema
- Atrophy of the disused limb (reduction in size and strength)
- Pain.
These can be prevented by early diagnosis and proper treatment [4].
How is mycetoma diagnosed?
Mycetoma is suspected when there is a typical triad of symptoms and signs:
- A painless firm subcutaneous mass
- Multiple sinus tracts
- A purulent or sero-purulent discharge that contains grains.
Dermoscopy may be useful for early stages of the disease detecting grains within skin lesions [5]. Grains are conglomerates of fungi or bacteria disposed radially (like sun rays).
Tissue for microscopy and culture is collected by:
- Making a small incision and expressing the secretions;
- Using a needle and syringe to withdraw fluid.
The colour of the grains can narrow the options of the causative bacterium or fungus. The grains are treated with potassium hydroxide (KOH) and then stained with Gram and PAS stains. On microscopy:
- Actinomycotic grains have very fine filaments
- Eumycotic grains contain thicker, branched filaments.
As some are slow-growing organisms, cultures at 25–30°C and 37°C are set for up to 6 weeks for both bacteria and fungi [1,6]. When it is difficult to identify the responsible organism, molecular techniques such as PCR (polymerase chain reaction) can be used [2].
Skin biopsy may show typical histopathological features of mycetoma.
Imaging can be used to assess the depth of infection [6].
-
- Plain X-ray
- Ultrasound scan
- Computed tomography (CT)
- Nuclear magnetic resonance imaging (MRI).
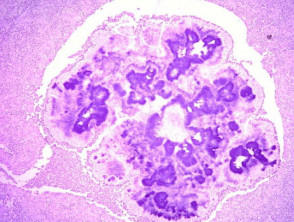
H&E stain of actinomycosis grains
What is the differential diagnosis for mycetoma?
Infectious diseases
- Bacterial infection: leprosy, cutaneous tuberculosis, non-tuberculous mycobacterial infections, botryomycosis (non-actinomycetic bacteria causing skin infection with grain-like structures), syphilis, osteomyelitis
- Fungal infection: chromoblastomycosis, sporotrichosis, and dermatophyte pseudomycetomas
Non-infectious diseases
- Podoconiosis or other forms of mossy foot due to lymphoedema
- Certain cancers: sarcoma of the skin, soft tissue or bones, Kaposi sarcoma
- Foreign-body reactions
What is the treatment for mycetoma?
Mycetoma cannot be cured without active treatment. It requires antibiotics (for actinomycetomas) or oral antifungals (for eumycetomas) for weeks, months or years. Damage to subcutaneous tissues (muscle, bones, joints or tendons) often persists, so local surgery (including amputation) and physiotherapy may be required [1,2].
Actinomycetoma (single or in combination)
- Trimethoprim + sulphamethoxazole
- Amoxicillin + clavulanic acid
- Amikacin or gentamicin
- Doxycycline or minocycline
- Penicillin
- Dapsone
- Streptomycin
- Rifampicin
Eumycetoma (only one usually used)
What is the outcome for mycetoma?
Despite the need for prolonged treatment, prognosis is usually good with proper therapy. The longer the infection has been present prior to treatment, the more likely complications and disability will occur [4].