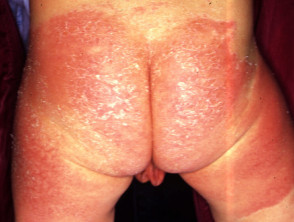
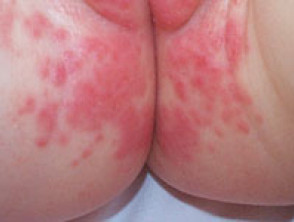
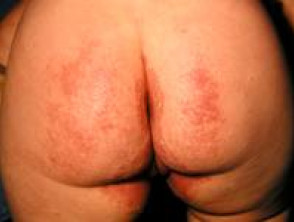
What is napkin dermatitis?
Napkin dermatitis and nappy rash are used to describe various skin conditions that affect the skin under a napkin or incontinence pad. The US term is diaper rash. Napkin dermatitis is most often a form of contact dermatitis.
Who gets napkin dermatitis?
Napkin dermatitis most often affects babies aged 3 to 15 months of age, especially those wearing traditional cloth nappies (50%). It is much less prevalent in babies wearing modern breathable and multilayered disposable nappies.
Napkin dermatitis can also affect older children and adults that are incontinent (see Incontinence-associated dermatitis).
What is the cause of napkin dermatitis?
Napkin dermatitis follows damage to the normal skin barrier and is primarily a form of irritant contact dermatitis.
- Urine and occlusion lead to overhydration and skin maceration.
- Faecal bile salts and enzymes break down stratum corneum lipids and proteins.
- A mixture of urine and faeces creates ammonium hydroxide, raising pH.
- The wet skin is colonised by micro-organisms, particularly candida.
- Mechanical friction from limb movement may increase discomfort.
- Pre-existing skin conditions such as atopic dermatitis or seborrheic dermatitis predispose a baby to napkin dermatitis.
Babies who are breastfed have a lower incidence of napkin dermatitis, as faeces in breastfed babies have a lower pH than in formula-fed babies. As babies start to eat solid foods, the stool frequency and pH start to increase and napkin dermatitis occurs more often.
Other causes of napkin rashes include:
- Candida albicans
- Impetigo
- Infantile seborrhoeic dermatitis
- Atopic eczema
- Psoriasis
- Miliaria
- Acrodermatitis enteropathica
- Acrodermatitis enteropathica-like conditions
- Biotin responsive dermatosis
- Rare disorders.
Napkin dermatitis is not due to:
- Allergy to the napkins
- Toxins in the napkins
- Washing powders (unless these are not thoroughly removed by rinsing)
- Dermatophyte fungal infections (tinea).
What are the clinical features of napkin dermatitis?
Napkin dermatitis presents as erythematous macules and papules in the genital area that can spread to involve the lower abdomen and thighs.
- Irritant napkin dermatitis: well-demarcated variable erythema, oedema, dryness and scaling. Affected skin is in contact with the wet napkin and tends to spare the skin folds.
- Chafing: erythema and erosions where the napkin rubs, usually on waistband or thighs.
- Granuloma gluteale infantum: red or purple nodules
- Candida albicans: erythematous papules and plaques with small satellite spots or superficial pustules.
- Impetigo (Staphylococcus aureus and Streptococcus pyogenes): irregular blisters and pustules.
- Infantile seborrhoeic dermatitis: cradle cap and bilateral salmon pink patches, often desquamating, in skin folds.
- Atopic dermatitis: bilateral scratched, dry plaques anywhere, but uncommon in the nappy area and family history is common.
- Psoriasis: persistent, well-circumscribed, symmetrical, shiny, red, scaly or macerated plaques; other sites may be involved; family history common.
- Disseminated secondary eczema or autoeczematisation: rash in distal sites associated with severe napkin rash.
Napkin dermatitis may predispose the infant to urinary tract infection and, in females, to vaginal infection.
Napkin dermatitis
See more images of napkin dermatitis.
What tests should be done?
In most cases, no laboratory tests are necessary. Skin swabs may be useful to confirm Candida albicans or bacterial infection.
What is the treatment for napkin dermatitis?
General measures
The need to keep baby dry and use barrier creams should be emphasised. The caregiver should always wash their hands before and after changing a nappy/diaper. Napkin dermatitis is much less common with modern disposable napkins than with cloth nappies.
Disposable nappies:
- Are available in different shapes and sizes depending on age and sex
- May be selected in a larger size to reduce contact and friction between the napkin and skin
- Keep the skin dry and clean
- Maintain optimal skin pH
- Should be changed when wet or soiled
- Contain cellulose pulp and superabsorbent polymers
- May include petrolatum-based moisturising lotion to support the skin barrier
- Fasteners, backsheets and stretch reduce leakage
- Are non-toxic and biologically inert
- Do not contain allergens such as natural rubber latex or disperse dyes
- Lead to less household exposure to faecal matter.
If using cloth nappies, nappy liners keep the skin dry. Avoid plastic overpants.
At napkin changes:
- Gently clean the baby’s skin with water and a soft cloth
- Wet wipes are convenient but expensive and can lead to contact allergy to preservatives used to stop them going mouldy
- Aqueous cream or another non-soap cleanser can be used if necessary
- Pat dry gently and allow to air dry
- Apply a protective emollient ointment containing petrolatum and zinc oxide.
Other suggestions
- Give evening fluids early to reduce wetting at night.
- Observe whether certain foods are related to the rash by increasing stool acidity (eg, orange juice) or frequency. If this is the case, discontinue the responsible food, at least temporarily.
- Allow nappy-free times.
Prescription treatments
- Mild topical steroid such as hydrocortisone cream applied to inflamed skin once or twice daily for 1–2 weeks.
- Topical antifungal cream (eg, clotrimazole, ketoconazole, ciclopirox, sertaconazole) once or twice a day if suspicious of Candida albicans infection.
- Strong steroid creams should not be applied to a baby's bottom due to potential side effects of striae, tachyphylaxis, and skin thinning.
- Non-prescription topical products containing Aloe vera and Calendula officinalis are reportedly effective for napkin dermatitis.