What is oral candidiasis?
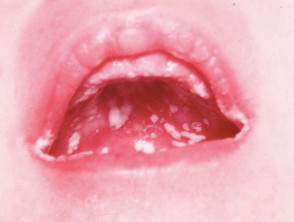
Oral candidiasis is a fungal infection of the mouth often called 'thrush' because its white spots resemble the breast of the bird with the same name.
Although candida is present in 50% of the normal flora of healthy mouths, it causes infection (candidiasis) when increased numbers of yeast cells invade the mucosa.
Who gets oral candidiasis?
Risk factors for developing oral candidiasis include:
- Infancy or old age
- In a newborn baby, maternal vaginal yeast infection
- Serious underlying diseases, such as cancer, primary immunodeficiency or infection with human immunodeficiency virus
- Candida infection elsewhere eg, in an infant, napkin dermatitis
- Dry mouth due to disease of the salivary glands or medications, eg antihistamines, diuretics
- Dentures, especially if they are not regularly cleaned or fit badly
- Smoking
- Injury to the mouth
- Broad-spectrum antibiotics
- Nutritional deficiency, for example, iron or B-vitamin deficiency
- Inhaled corticosteroids used to treat asthma, such as beclometasone, budesonide, fluticasone.
Oropharyngeal candidiasis is reported in hospitalised and asymptomatic COVID-19 patients.
What causes oral candidiasis?
The usual organism is Candida albicans, but at least seven other species of Candida can also cause oral candidiasis including C. tropicalis, C. glabrata, C. kruesi, and others. C. dubliniensis is also reported in HIV patients. See Non-albicans candida infections.
Oral candidiasis
More images of oral candidiasis.
What are the clinical features of oral candidiasis?
Candida may arise suddenly as an acute infection or persist for long periods as a chronic infection.
- Acute pseudomembranous candidiasis.
- There are white patches on gums, tongue and inside the mouth that can be peeled off leaving a raw area.
- Acute atrophic candidiasis.
- There are smooth red shiny patches on the tongue. The mouth is very sore.
- Chronic atrophic candidiasis.
- This is common in those with dentures. The underlying mucosa is red and swollen.
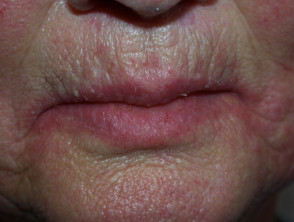
- Angular cheilitis.
- There are sore red splits at each side of the mouth, more likely if there is an overhang of the upper lip over the lower lip causing a moist deep furrow. Angular cheilitis due to candida and/or Staphylococcus aureus arises frequently in those taking the medication isotretinoin for acne; this medication dries the lips.
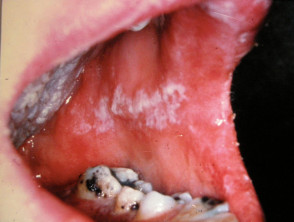
- Chronic hyperplastic candidiasis.
- This is a type of oral leukoplakia (white patch) inside the cheeks or on the tongue with persistent nodules or lumps. It usually affects smokers and is pre-malignant. Red patches (erythroplakia), as well as white patches, may indicate malignant change.
- Chronic mucocutaneous candidiasis
- Presents as a chronic pseudomembranous oral infection. The skin and nails are also affected.
- Median rhomboid glossitis
- Diamond-shaped inflammation at the back of the tongue.
- Candida can cause a secondary infection of other oral mucosal conditions such as lichen planus or geographic tongue.
Severe infections may extend down the throat (oesophageal infection) and cause difficulty with swallowing.
How is oral candidiasis diagnosed?
Microscopy and culture of skin swabs and scrapings aid in the diagnosis of candidal infections. However, as candida can live on a mucosal surface quite harmlessly, clinical correlation is required. It may also secondarily infect an underlying disorder.
In extensive oral candidiasis, endoscopy is performed to see the extent of the lesions into the gastrointestinal tract.
How is oral candidiasis treated?
General measures including prevention
Practice good oral hygiene.
- Brush teeth regularly.
- Use warm saline water as a mouth wash.
- Avoid use/overuse of antiseptic mouthwashes, as they alter the flora of the mouth.
- If using a steroid inhaler for asthma, drink water and rinse mouth after inhalation.
Denture wearers:
- Clean dentures with an anti-candidal preparation, such as 1% sodium hypochlorite solution.
- Remove dentures overnight.
Specific measures
Mouthwashes with anti-candidal activity include:
- Triclosan
- Chlorhexidine gluconate
- Essential oil formulations.
Topical antifungal products for oral candidiasis include:
- Oral nystatin suspension (1 ml 4 times daily), or pastilles (for denture stomatitis)
- Amphotericin B (5 ml or 1 10-mg lozenge 4 times daily)
- Miconazole gel (2.5 ml after food 4 times daily).
Treatment should be continued for 1–4 weeks or until symptoms have been clear for 7 days.
Systemic treatments include:
- Fluconazole 100–150 mg daily for 10 days (especially for pseudomembranous infection)
- Itraconazole
- Voriconazole
- Amphotericin B