What is tinea pedis?
Tinea pedis is a foot infection due to a dermatophyte fungus. It is the most common dermatophyte infection and is particularly prevalent in hot, tropical, urban environments.
- Interdigital involvement is most commonly seen (this presentation is also known as athlete’s foot, although some people use the term for any kind of tinea pedis).
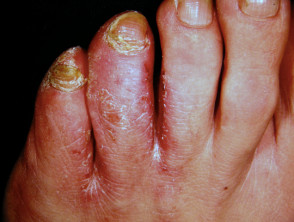
- Tinea pedis may be accompanied by tinea cruris, tinea manuum or tinea unguium.
What causes tinea pedis?
The three most common dermatophyte fungi causing tinea pedis are:
- Trichophyton (T.) rubrum
- T. interdigitale, previously called T. mentagrophytes var. interdigitale
- Epidermophyton floccosum
Tinea pedis
See more images of tinea pedis ...
Who gets tinea pedis?
Tinea pedis usually occurs in males and adolescents/young adults, but can also affect females, children and older people. Infection is usually acquired by direct contact with the causative organism, for example using a shared towel, or by walking barefoot in a public change room.
Other risk factors include:
- Occlusive footwear (for example, heavy industrial boots)
- Excessive sweating (hyperhidrosis)
- Underlying immunodeficiency or diabetes mellitus
- Systemic corticosteroids or immune suppressive medications
- Poor peripheral circulation or lymphoedema.
What are the clinical features of tinea pedis?
Tinea pedis tends to be asymmetrical, and may be unilateral. It usually presents in one of three ways:
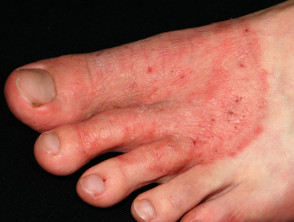
- Itchy erosions and/or scales between the toes, especially between 4th and 5th toes
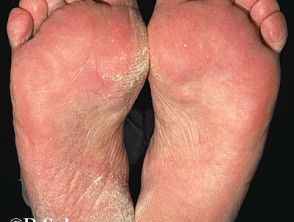
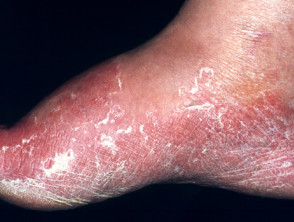
- Scale covering the sole and sides of the feet (hyperkeratotic/moccasin type, usually caused by T. rubrum)
- Small to medium-sized blisters, usually affecting the inner aspect of the foot (vesiculobullous type).
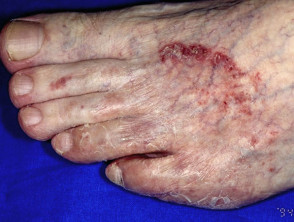
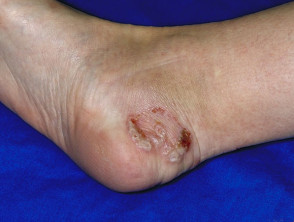
It can also uncommonly cause oozing and ulceration between the toes (ulcerative type), or pustules (these are more common in tinea pedis due to T. interdigitale than that due to T. rubrum).
How is the diagnosis of tinea pedis made?
The diagnosis of tinea pedis can be made clinically in most cases, based on the characteristic clinical features. Other typical sites, such as toenails, groin, and palms of the hands, should be examined for fungal infection, which may support a diagnosis of tinea pedis.
Diagnosis is confirmed by skin scrapings, which are sent for microscopy in potassium hydroxide (when segmented hyphae may be observed) and culture (mycology). Culture may not be necessary if typical fungal elements are observed on microscopy.
What is the differential diagnosis of tinea pedis?
The differential diagnosis of tinea pedis includes:
- Foot eczema — especially pompholyx (pedopompholyx), or irritant contact dermatitis due to persistent moisture between closely adherent toes
- Contact allergic dermatitis to a component of footwear (such as a rubber accelerant, shoe adhesive, potassium dichromate used as leather tanning agent, or fabric dye)
- Psoriasis (plantar psoriasis)
- Plantar pustulosis
- Plantar keratoderma.
These inflammatory disorders are more likely to be symmetrical and bilateral. Mycology is negative.
What is the treatment for tinea pedis?
General measures should be first-line, including meticulous drying of feet, especially between the toes, avoidance of occlusive footwear, and the use of barrier protection (sandals) in communal facilities.
Topical antifungal therapy once or twice daily is usually sufficient. These include azoles, allylamines, butenafine, ciclopirox, and tolnaftate. A typical course is 2 to 4 weeks, but single dose regimes can be successful for mild infection [1,2].
For those who do not respond to topical therapy, an oral antifungal agent may be needed for a few weeks. These include:
- Terbinafine
- Itraconazole
- Fluconazole
- Griseofulvin (this may be inferior to other oral agents and may not be available in some countries) [3,4].
Patients with the hyperkeratotic variant of tinea pedis may benefit from the addition of a topical keratolytic cream containing salicylic acid or urea [5].
How can recurrence of tinea pedis be prevented?
To minimise recurrence of tinea pedis:
- Dry feet and toes meticulously after bathing
- Use desiccating foot powder once or twice daily
- Avoid wearing occlusive footwear for long periods
- Thoroughly dry shoes and boots
- Clean the shower and bathroom floors using a product containing bleach
- Treat shoes with antifungal powder.
If treatment of tinea pedis is unsuccessful, consider reinfection, coexistent untreated fungal nail infection, reinfection due to untreated family member, or an alternative diagnosis.