Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Autoimmune/autoinflammatory Blood vessel problems
Author: Vanessa Ngan, Staff Writer, 2003. Updated by Dr Ebtisam Elghblawi, Tripoli, Libya, April 2017.
Introduction Causes Demographics Signs and symptoms Diagnosis Treatment
Antiphospholipid syndrome is an acquired autoimmune disorder characterised by recurrent arterial or venous thrombosis and/or pregnancy losses, in the presence of persistently elevated levels of anticardiolipin antibodies and/or evidence of circulating lupus anticoagulant (these abnormalities are detected by blood tests). Antiphospholipid syndrome can be primary or secondary.
Seronegative antiphospholipid-like syndrome is a similar disease where antiphospholipid antibodies are not detected.
The mechanisms resulting in a hypercoagulable state and recurrent thrombosis are not yet defined. Complement activation is involved. The 'two-hit' theory has associated the onset of thrombosis with increasing age, hypertension, diabetes, obesity, smoking, pregnancy, surgery, and other genetic hypercoagulable states.
Antiphospholipid syndrome is generally diagnosed in young to middle-aged adults. However, it can affect children and adults of all ages.
Secondary antiphospholipid syndrome is more common in females than in males, most likely because systemic lupus erythematosus and other connective tissue disorders have a female predominance.
Patients have a history of spontaneous miscarriage, deep vein thrombosis (DVT), pulmonary embolism, myocardial infarction, or stroke.
To classify as antiphospholipid syndrome a patient must have at least one of the two following clinical manifestations in addition to the presence of certain laboratory abnormalities.
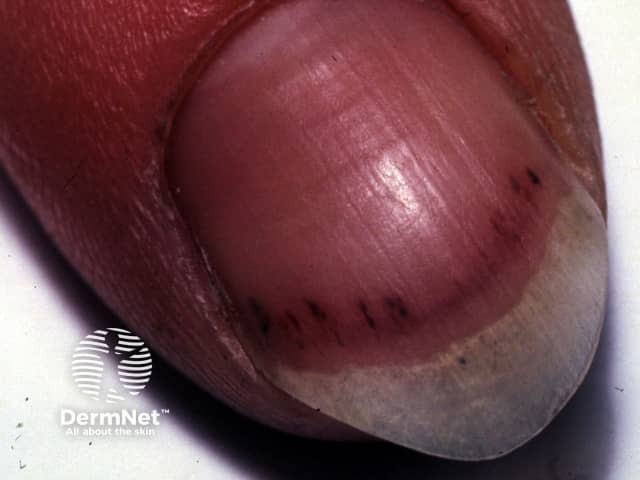
Splinter haemorrhages
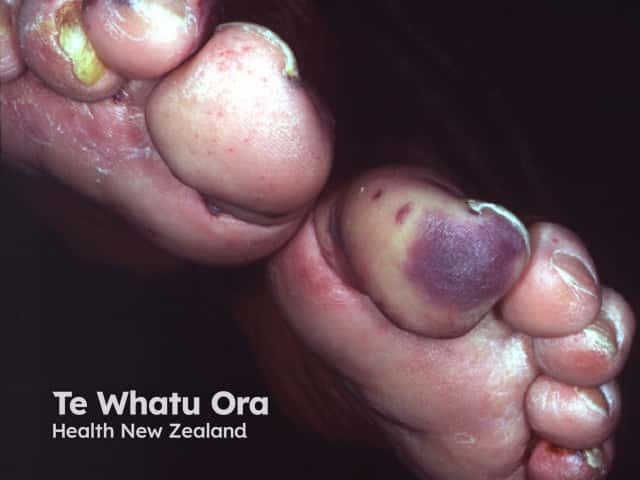
Cholesterol emboli
Other symptoms are not part of the classification criteria.
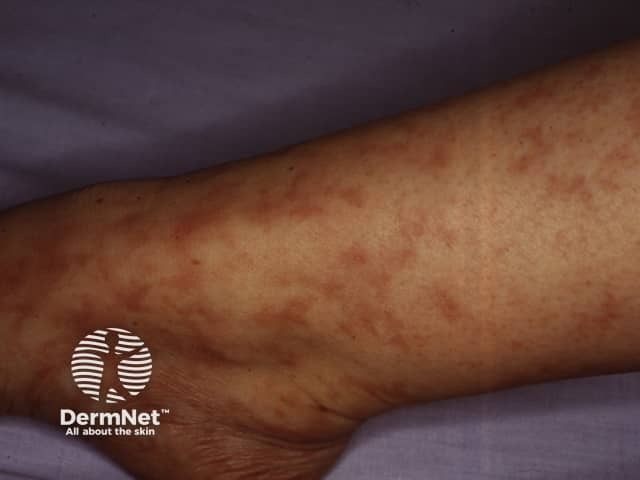
Livedo reticularis affects up to 80% of people with antiphospholipid antibodies. Other features include:
Catastrophic antiphospholipid syndrome refers to blockage of blood vessels in multiple organs, which may occur over days or weeks. The condition is serious and often lethal.
The antiphospholipid syndrome has various clinical manifestations and is associated with a range of autoantibodies. In 2006, revised criteria for the diagnosis of antiphospholipid syndrome stated that at least one clinical criterion and one laboratory criterion must be present [1]. The name 'lupus anticoagulant' is misleading because not all patients with a positive result have systemic lupus erythematosus, and the antiphospholipid syndrome is associated with increased blood clotting rather than increased bleeding.
Laboratory tests detect antiphospholipid antibodies or abnormalities in phospholipid-dependent tests of blood clotting (coagulation). Patients with suspected antiphospholipid syndrome should be tested for the following:
The main aim of treatment is to prevent the clinical manifestations of antiphospholipid syndrome. Risk factors for thrombosis should be identified and removed or corrected:
Antiplatelet drugs such as low-dose aspirin may be useful.
There is no specific treatment for antiphospholipid syndrome. Signs and symptoms are treated as they occur. For example, thrombosis or embolism is treated with the anticoagulants heparin and warfarin.