Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Marius Rademaker, Dermatologist, Hamilton, New Zealand, 2008.
A glomus tumour is a nodule that arises from glomus cells in the arterial portion of the glomus body, or the Sucquet-Hoyer canal. The tumour is usually found on the nail bed or palm of a young adult and can be extremely painful, particularly following change in temperature or pressure.
Extracutaneous glomus tumours have been reported rarely in the gastrointestinal tract, mediastinum, trachea, mesentery, cervix and vagina.
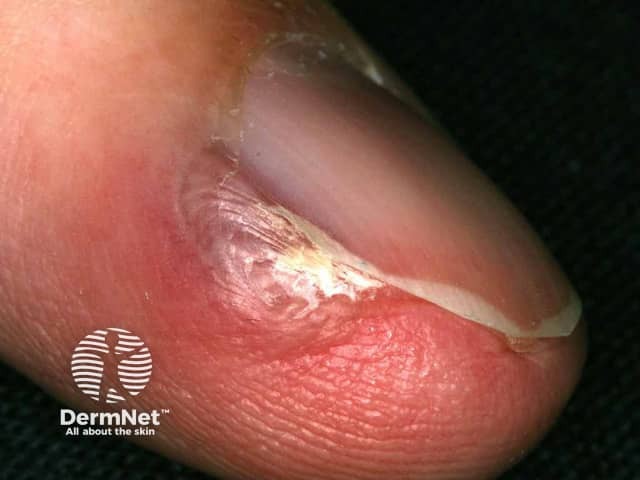
Glomus tumour
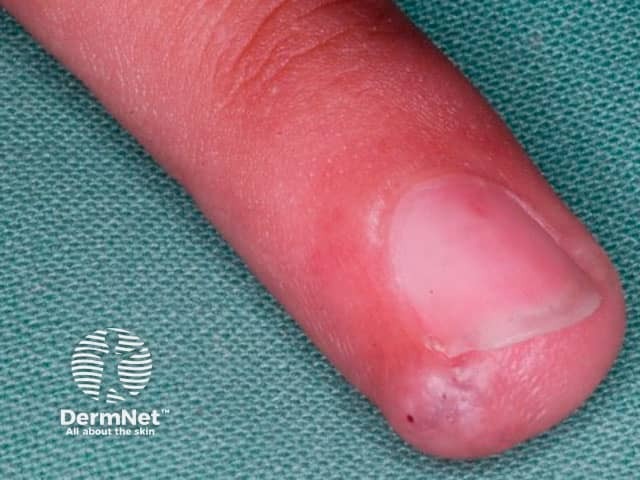
Glomus tumour
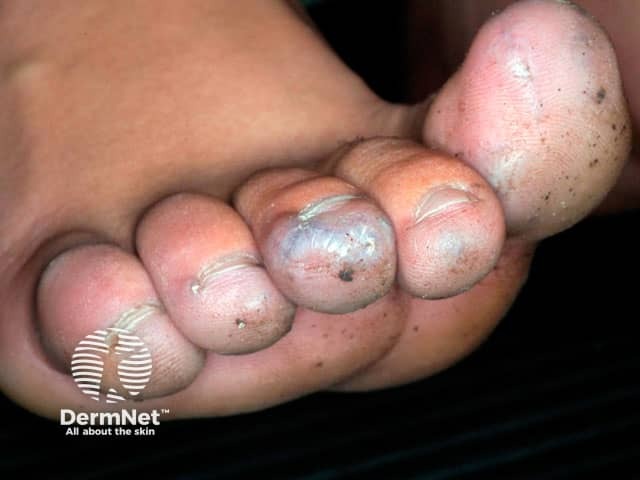
Glomus tumour
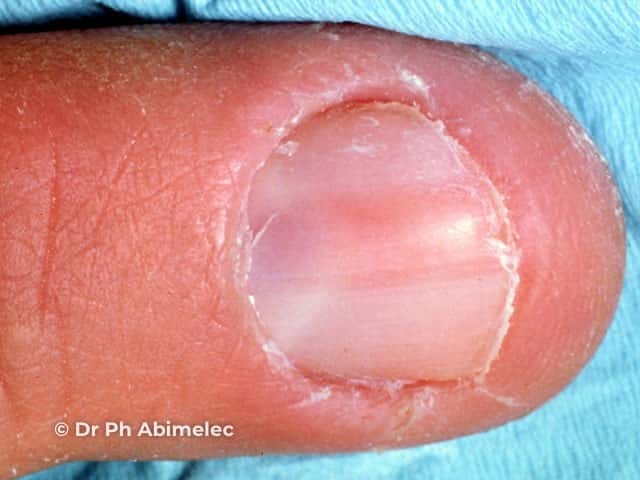
Glomus tumour
The glomus body is a temperature-sensitive organ of modified perivascular smooth muscle cells, which is involved in the vascular regulation of skin temperature; arterioles contract with cold, whereas glomus bodies dilate, thereby maintaining blood flow to the nail bed.
Glomus tumour may be suspected clinically, as it is typically a solitary, painful, 1–2 cm reddish-blue papule or nodule on or around a nail bed. It usually undergoes biopsy. The histology of a glomus tumour reveals solid sheets of glomus cells around small blood vessels. Immunohistochemical studies may be helpful in diagnosis.
Solitary glomus tumours can be surgically excised.