Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Vanessa Ngan, Staff Writer, 2003. Updated by Dr Sara de Menezes, Basic Physician Trainee, Alfred Health, Melbourne, Australia; Chief Editor, Dr Amanda Oakley, Dermatologist, Hamilton, New Zealand, September 2016.
Introduction Causes Demographics Complications Diagnosis Treatment Outlook
Livedo reticularis refers to various conditions in which there is mottled discolouration of the skin. It is described as being reticular (net-like, lace-like), as cyanotic discolouration surrounds pale central skin.
The terminology of livedo reticularis may include:
Livedo reticularis results from a disturbance of blood flow to the skin, causing low blood flow and reduced oxygen tension to the skin. Cutaneous vasculature is comprised of a series of 1–3 cm cones. The apex of each cone is located deep within the dermis at the site of an ascending arteriole. At the margin of each cone, the density of the arterial bed is decreased, and the superficial venous plexus is more prominent. Any pathological or physiological process which impairs blood flow to the skin results in higher amounts of deoxygenated haemoglobin, leading to a livid discolouration.
Physiological arteriolar vasospasm in response to cold, produces reversible skin discolouration, such as in cutis marmorata. Prolonged vasospasm, thrombosis or hyperviscosity can cause the pathological skin changes of livedo racemosa.
A unilateral form of livedo reticularis due to local heat injury is known as erythema ab igne.
Cutis marmorata causes temporary or physiological livedo in about 50% of healthy infants and many adults, particularly young women when exposed to the cold.
Cutis marmorata telangiectatica congenita is a rare condition in which pronounced livedo is present at birth or soon after. It often improves with age. There are several congenital abnormalities associated with cutis marmorata telangiectatica.
Primary livedo reticularis is the idiopathic form in adults and can be persistent. The diagnosis is usually made once other more severe causes of livedo reticularis have been ruled out.
Secondary livedo, or livedo racemosa, is associated with a range of systemic diseases.
Occlusion of vessels may occur because of a hypercoagulable state. This may present as blue toe syndrome.
Small, medium and large vessel vasculitis is associated with livedo racemosa.
Amantadine (dopamine agonist used to treat Parkinson disease, multiple sclerosis, and attention deficit hyperactivity disorder) causes livedo through arteriolar vasospasm associated with depletion of catecholamines. Drug-associated livedo has also been reported with:
Livedo reticularis is characterised by:
In cutis marmorata, mottling is diffuse, mild and usually symptomless. The livedo commonly occurs on the legs and gradually resolves on rewarming. Cutis marmorata telangiectatica congenita is more pronounced than cutis marmorata. Primary livedo reticularis in adults is intermittent, and the changes in skin colour are less influenced by ambient temperature.
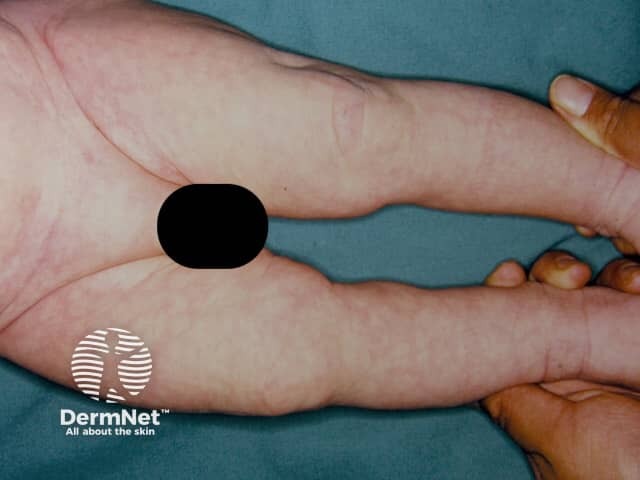
Cutis marmorata
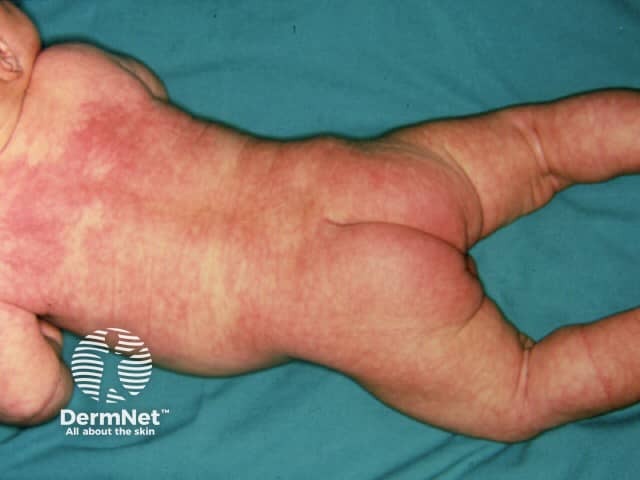
Cutis marmorata
Livedo racemosa often affects the trunk and buttocks as well as legs. The net-like violaceous pattern tends to be composed of irregular, broken macules with an annular pattern.
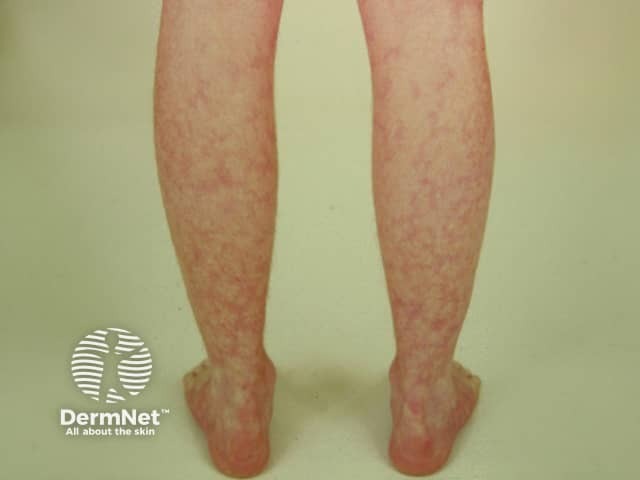
Livedo reticularis
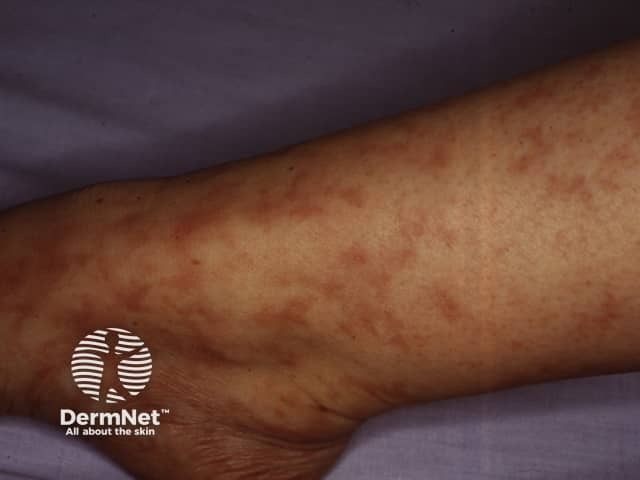
Livedo reticularis itself is relatively benign. However, thromboembolic disease due to associated conditions such as antiphospholipid syndrome may lead to serious arterial events, including the death of the patient.
Livedo reticularis/racemosa is diagnosed by its clinical appearance. Investigations are undertaken to seek for an underlying cause (see above) based on careful history and examination, as extensive screening studies are unlikely to be helpful. The lupus anticoagulant panel should be ordered in acquired livedo that is not induced by the cold.
If required, it is best to take at least two biopsies from red/blue and white areas of the livedo and to ask for serial sections to be performed. A palpable site is ideal for a biopsy if present. The red area may just show non-diagnostic telangiectasia. The central white, ischaemic area may reveal an occluded vessel. Even a large skin biopsy of the centre of livedo racemosa ring may be reported as normal. Multiple biopsies may increase the diagnostic yield. The goal of a biopsy is to obtain samples of the medium vessel found in the deep reticular dermis and subcutaneous fat, which may require a wedge or large punch biopsy for increased yield.
Early signs of vasculopathy in livedo racemosa are lymphocytes and histiocytes attaching to endothelial cells. The cells join with fibrin to occlude the lumen of capillaries (lymphocytic thrombophilic arteritis).
This should be distinguished from medium vessel neutrophilic vasculitis occurring in cutaneous polyarteritis nodosa. Other capillaries may be dilated, or replaced by scar tissue (fibrosis).
There is no specific treatment for livedo reticularis, except for cold avoidance.
In some patients, the symptoms may improve spontaneously with age. Rewarming the area in idiopathic cases or treatment of the underlying cause of secondary livedo may reverse the discolouration. Treatment should be directed at treating the underlying disorder causing the livedo reticularis if known. Treatment with low-dose aspirin, pentoxifylline and other anticoagulants may be recommended in patients with a confirmed occlusive vasculopathy.
Smoking cessation is essential to reduce the risk of associated arterial events such as stroke.
Livedo reticularis itself is relatively benign. However, thromboembolic disease due to associated conditions such as antiphospholipid syndrome may lead to serious arterial events, including the death of the patient.
Cutis marmorata is usually less evident with age. Over time, in primary livedo reticularis and livedo racemosa, the vessels become permanently dilated, and livedo reticularis becomes permanent regardless of the surrounding temperature.