Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Amanda Oakley, Dermatologist, Hamilton, New Zealand, 2002. Updated by Dr Jannet Gomez, October 2016. Updated October 2020
Introduction
Causes
Prevalence
Transmission
Demographics
Signs and symptoms
Diagnosis
Treatment
Complications
Prevention
Do you have confirmed measles? Send DermNet your pictures.
Measles, also known as English measles, rubeola or morbilli, is a highly contagious viral infection causing fever and a rash.
Measles is a notifiable disease.
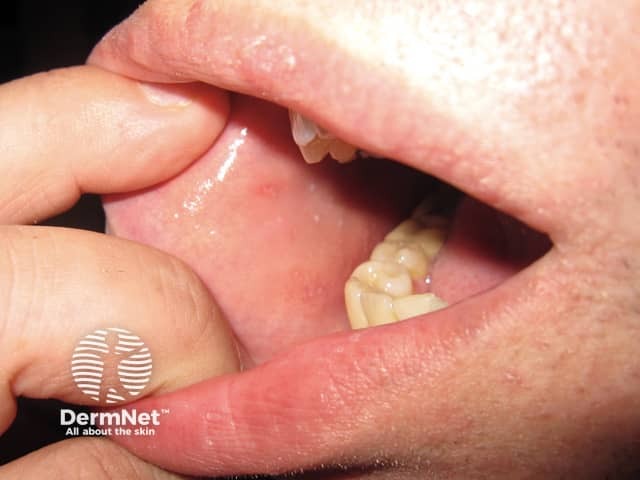
Koplik spots Day 1
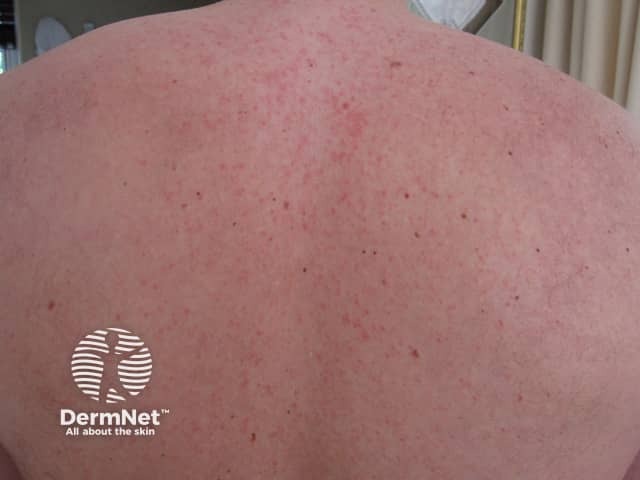
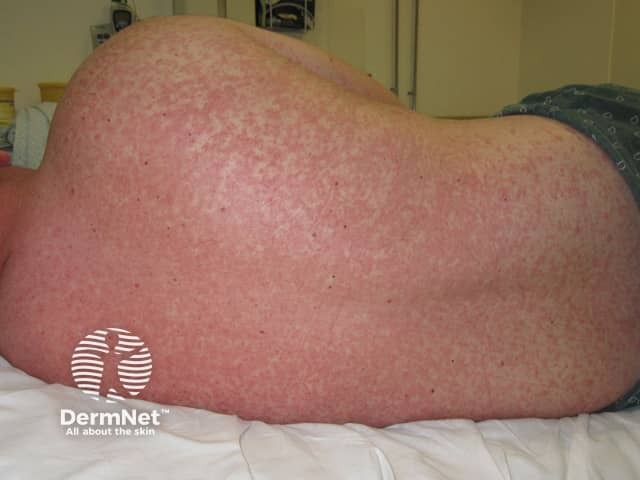
Rash Day 3
Measles is caused by the measles virus, which belongs to the morbillivirus family.
Before widespread immunisation against measles in industrialised countries, measles was a very common childhood disease that carried a high death rate. Nowadays in countries where measles is part of an immunisation programme, the risk of exposure and incidence of actual disease cases is low. A recent trend by some parents not to immunise their children has led to an increase in the number of cases of measles, and its complications.
In developing countries, measles still occurs frequently and is associated with a high rate of complications and death. It remains a common disease even in some developed countries of Europe and Asia.
WHO reported a surge in cases worldwide in 2018, with nearly 10 million cases, and more than 140,000 deaths mostly in children under 5 years of age. The highest incidence rates were in Ukraine, Somalia, Democratic Republic of Congo, Liberia and Madagascar. The US reported its highest rate of infection in 25 years, and four countries in Europe lost their 'measles elimination' status.
Measles is highly contagious and is easily spread from person to person by breathing in airborne respiratory droplets from an infected person's coughing or sneezing.
An infected person is contagious 2 days before any symptoms show, and remains infectious for at least 5 days after the onset of rash.
An acute infection of measles almost always gives lifelong immunity.
Individuals at particular risk of measles infection include:
The greatest risk for severe measles and its complications is seen in:
Measles develops through distinct clinical stages.
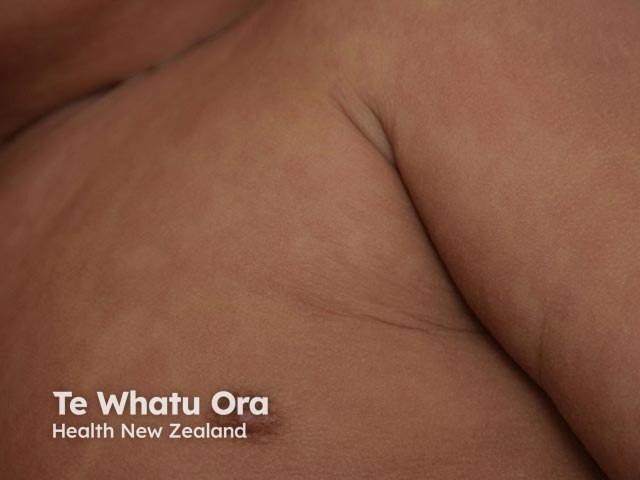
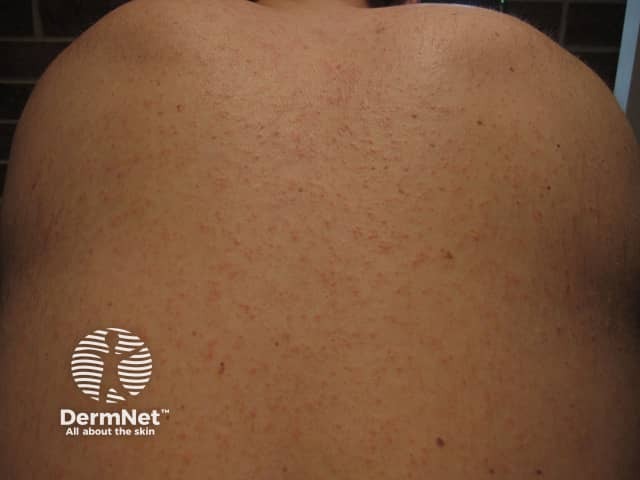
Diagnosis of measles is based on the characteristic history and physical examination. Because the disease is now so rarely seen in developed countries, any suspected cases require laboratory confirmation. This is particularly useful in the following situations:
Acute measles is usually confirmed on a viral nasopharyngeal or throat swab analysed by polymerase chain reaction (PCR). Blood and urine samples can also be used. This should be done within 5 days of onset of rash, however, positive results are sometimes obtained up to 10–14 days after the rash has resolved.
Blood is also taken for measles IgM and IgG antibodies (serology). Levels of specific IgM become elevated during the active infection phase and IgG antibody appears during the recovery phase.
Viral culture of the throat and nasopharyngeal swabs is preferred in immunocompromised patients where serological evidence might be absent due to decreased immune response. An immunofluorescence test for measles antigen can also be considered in patients with poor immunity.
There is no specific treatment for measles, which is why immunisation is so important. Treatment for mild cases of measles is supportive. Bed rest is vital, as it prevents complications and prevents the spread of the virus.
Patients with drowsiness, dehydration, or discomfort breathing require hospitalisation for supportive care.
Antibiotics are only needed to treat secondary bacterial infections such as otitis media, infectious diarrhoea, pneumonia, and sepsis.
Ribavirin (antiviral) is used to treat measles infection in immunocompromised patients and in those affected with subacute sclerosing panencephalitis.
Approximately 30% of reported measles cases have one or more complications.
Rarely, subacute sclerosing panencephalitis—a fatal condition—develops decades after a measles infection due to persistence of the measles virus in the central nervous system.
Measles can be prevented by vaccination with live attenuated measles vaccine. It is available as a single antigen preparation or combined with live attenuated mumps and/or rubella vaccines. Combined measles, mumps and rubella (MMR) vaccine is currently part of routine immunisation programmes in most industrialised countries, including New Zealand.
Measles vaccine induces long-term (probably life-long) immunity in most individuals. Vaccination schedules recommend a two-dose immunisation strategy; the first dose at 12–15 months of age, followed by a second dose at 4–6 years.
Measles vaccine should not be given during pregnancy. Women not previously immunised against measles should avoid pregnancy for one month (28 days) after receiving the MMR vaccine.
Immune globulin does not prevent measles, but it is helpful in decreasing the severity of illness in those exposed to the virus. It is recommended for:
Individuals vaccinated prior to 1968 may require revaccination, as vaccines used before this time may not have conferred life-long immunity.