Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Introduction Spread Signs and symptoms Diagnosis Differential diagnoses Treatment Complications Prevention Adverse effects
Smallpox is a highly contagious and sometimes deadly disease that is caused by infection with the variola virus. It has been around for thousands of years and has been associated with many deadly epidemics. Widespread vaccination between 1940 and 1970 has led to the global eradication of the virus and in 1980 the World Health Organization (WHO) officially declared smallpox eradicated. The last naturally occurring case of smallpox was in Somalia in 1977. The only remaining known variola virus isolates are stored at the Centers for Disease Control and Prevention (CDC) in the US and at the Vektor Institute in Russia. Renewed interest in smallpox is taking place, as there is concern that the variola virus may be used as an agent of bioterrorism.
There are 2 clinical types of smallpox, variola major and variola minor. Variola major is the most common and severe form and has a death rate of about 30%. Variola minor is a much less common form with an estimated death rate of less than 1%.
Vaccinia
The variola virus emerged in human populations thousands of years ago and humans are the only natural host. Smallpox is most efficiently spread from one person to another by breathing in airborne respiratory droplets from an infected person. This generally requires direct and fairly prolonged face-to-face contact. It can also be spread by touching the skin rash, sores and scabs of an infected person, or by sharing contaminated clothing, towels or bedding.
Infection with the variola virus begins with an incubation period that can be from 7-17 days (on average 12-14 days). During this time most people experience no symptoms whatsoever and they are not contagious. The first sign of smallpox disease is the prodromal phase, which lasts 2-4 days and is characterised by:
A characteristic rash appears after the prodromal phase and goes through several stages, lasting for up to 20 days or longer. The most contagious stage is the early rash, which lasts for about 4 days. Characteristics of this stage include:
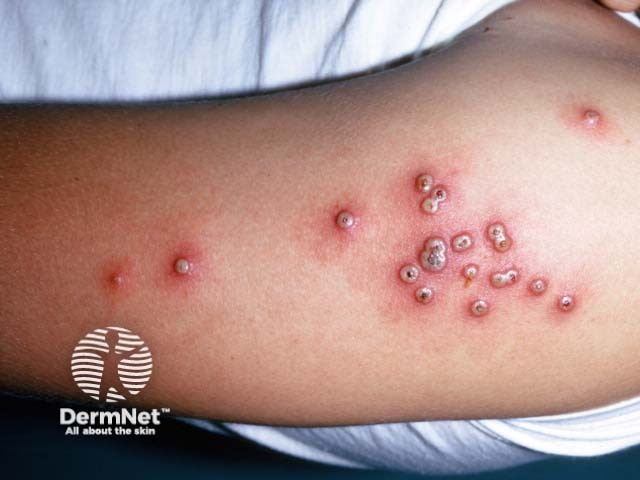
The bumps turn into pustules that are raised, round and firm to touch. Pustules may reach between 4 and 6 mm in diameter. After about 5 days pustules begin to form a crust and then scab. By about 3 weeks after the first signs of the rash appearing, scabs fall off leaving marks on the skin that eventually become pitted scars. A person is contagious until all the scabs have fallen off.
Smallpox can be diagnosed clinically by the presence of fever and typical skin lesions. It is supported by isolation of the virus in the blood or skin lesions or the detection of antibodies to the variola virus in a bloodstream. These tests must be undertaken in specialised laboratories.
Smallpox could be confused with several other diseases, especially:
There is no cure for smallpox. The aim of keeping smallpox under control is to prevent it from occurring. If smallpox is suspected in an individual, state health officials must be notified immediately and containment of the virus a major priority. This would include strict respiratory and contact isolation for at least 17 days and vaccination of all contacts.
Treatment for an already ill smallpox patient should be supportive care consisting of adequate hydration and nutrition, eye care and antibiotics as needed for secondary skin infections. Vaccination within the incubation period, particularly if given within 3 days of exposure to the virus, has been shown to prevent or significantly lessen the severity of smallpox disease in most people.
The patient should be isolated. Very strict adherence to hygiene and personal protective equipment (N95 mask, eye protection, gloves, and gown) must be worn by carers to reduce the chance of contagion.
Most patients who survive smallpox have extensive scarring of the skin. Other complications may include:
Routine vaccination against smallpox among the general population was stopped soon after the WHO declared smallpox had been eradicated from the world. However, the last manufactured batches of smallpox vaccine (Vaccinia virus vaccine) are kept at the CDC, ready for use in the event of a smallpox outbreak. The United States has recently begun a vaccination programme for its military forces (February 2003).
Immunity is most effective during the first 10 years after vaccination and decreases thereafter. Historically, the vaccine has been effective in preventing smallpox infection in 95% of those vaccinated. The level of protection, in people who received the last routine smallpox vaccination over 30 years ago, is unclear.
Vaccination involves pricking the vaccine into a 5-mm area of the upper arm. The vaccination should be kept covered and should not be scratched, to avoid transmitting vaccinia virus to someone else. Within a few days, a papule appears that turns into a blister. It forms a pustule within a week, scabbing over in 2 weeks and healing with a scar within 3 weeks.
Unless recently exposed to smallpox, the following people should avoid vaccination as they are at greater risk of severe adverse effects.
The complications of vaccination include:
Severe adverse reactions to vaccination include:
Severe adverse reactions require treatment with Vaccinia Immune Globulin (VIG). A new intravenous form is likely to replace an intramuscular form used during the 1960s.