DermNet provides Google Translate, a free machine translation service. Note that this may not provide an exact translation in all languages
Home Arthropod infestations Pediculosis CME
Arthropod infestations CME
Pediculosis
Created 2008.
Learning objectives
- Identify and manage pediculosis
Introduction
The three species of louse that infest humans are:
- Pediculus humanus var. capitis - The head louse
- Pediculus humanus var. humanus - The body louse.
- Phthirus pubis - The pubic louse.
Lice are wingless insects with six legs on which are attached strong claws, which they use to grasp on tightly to hair shafts or clothing fibres.
Head lice, the most common infestation in humans, are colloquially known as cooties and their eggs are called nits. Pubic lice are smaller with a short body resembling a crab.
Head lice
Despite excellent hygiene, head lice (pediculosis capitis) are very prevalent especially in school children in most societies (one study in the Uk found 57% primary school children were infested). The usual organism is Pediculus humanus capitis, but there is some evidence that interbreeding between body and head lice has facilitated adaptation to the curly hair of people with black skin.
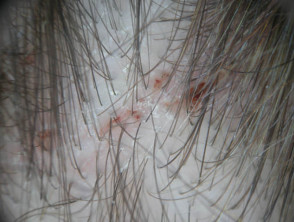
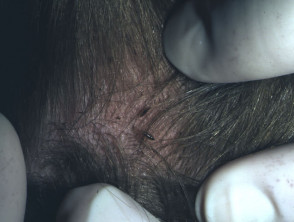
Scurrying mature live lice are 3 mm in length and are most easily found on the occiput or behind the ears. Black specks of louse dung, and tiny haemorrhagic papules (bites) are often visible.
Lice result in irritable crusted papules and sometimes, secondary dermatitis, impetiginisation and cervical lymphadenopathy.
The egg cases (‘nits’) are flask-shaped and 1 mm in length. They are found firmly attached to hair shafts. Empty egg cases are easier to see because they are white and further away from the scalp than grey nits containing live eggs.
Head lice
Identification
Scurrying mites are not always readily seen. Occasionally, it is difficult to distinguish egg cases from hair casts. Hair casts generally slide up the hair shaft, whereas egg cases are glued to the hair. Microscopy and dermoscopy may be helpful.
Other conditions to consider:
- Seborrhoeic dermatitis
- Psoriasis
- Irritant dermatitis from insecticide use
- Acne necrotica
Management
Children should be taught not to share hats, scarves, headbands, combs and brushes, as adult lice can survive up to three days away from a host. However, lice usually are spread through direct head-to-head contact.
Treatment of infestation should include:
- Application of insecticide foam, shampoo or liquid, repeated in one week
- Wet hair with vinegar to loosen nits
- Vigorous and repeated combing using a fine-toothed comb
- Regular scalp inspections
- Hot wash towels, sheets, pillowcases, clothing, brushes
- Isolate stuffed toys and other non-washable fomites for one week
Topical insecticides are neurotoxic and are not effective against young nits. They include:
- Gamma benzene hexachloride: neurotoxic, increasing levels of resistance
- Pyrethroids: safe, may irritate
- Permethrin: if necessary, extend time of application to overnight treatment under a shower cap
- Malathion: flammable.
Resistant cases may benefit from oral trimethoprim/sulphamethoxazole. Oral ivermectin is not registered for head lice treatment but is thought to be safe and effective. It is available under Section 29.
Preparations listed by MIMS NZ:
- ParaPlus aerosol spray: contains malathion, permethrin, piperonyl butoxide.
- Pyrifoam shampoo: contains permethrin.
Pubic lice
Pubic lice or crabs are easily transmitted sexually. The pubic hair is most common site but lice can spread to other hairy parts of the body including armpit, beard, chest hair and thigh hair. Eyelashes can also be affected. Infestation presents as itching, but blood specks on underclothes and live lice moving in the pubic hair are occasionally noted.
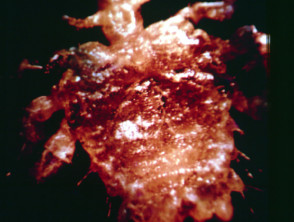
Pubic louse
Treatment
An insecticide such as Prioderm Cream Shampoo (maldison 1%) should be applied to all hairy parts of the body apart from the eyelids and scalp. It is washed off after 5 to 10 minutes and any remaining nits should be removed by using a fine toothed comb. A repeat application is advisable 7 days later.
Lice and nits can be removed from eyelashes by using a pair of fine forceps. Alternatively petroleum jelly, such as Vaseline can be smeared on the eyelashes twice a day for at least 3 weeks.
Underwear and bed linen should be washed thoroughly in hot water to prevent recurrences. Sexual partners need to be treated even if they deny itching and do not appear to be infected.
Body lice
Body lice tend to infest people in extreme states of poverty or personal neglect. The eggs of body lice are laid and glued to cloth fibres instead of hair, and the lice feed off the skin. Regular hot washing of clothes and bathing has lead to a decrease in incidence of body lice but during wartime and in some undeveloped countries the condition can still occur.
Body lice in the past have been responsible for spreading diseases such as typhus. However because of the decline in numbers of people infested with body lice this is no longer a significant problem.
Similar insecticides used in the treatment of head lice are used in the treatment of body lice. Hot washing of clothes and bathing should be emphasised.
Activity
Discuss the evidence that head lice are resistant to currently available insecticides.
Related information
References:
On DermNet NZ:
Information for patients
Other websites:
- Medscape Reference: Lice
- Medscape: Medline Abstracts: Head Lice
- Cochrane review: Interventions for treating head lice
- Clinical Evidence (BMJ): Head lice
- Auckland Sexual Health Service
- Merck Medicus Best Practice of Medicine: Lice, scabies and bed bugs
Books about skin diseases:
See the DermNet NZ bookstore
Sign up to the newsletter
© 2024 DermNet.
DermNet does not provide an online consultation service. If you have any concerns with your skin or its treatment, see a dermatologist for advice.