Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Created 2008.
Scabies is common in all communities and is responsible for a great deal of misery because of intractable pruritus and secondary bacterial pyoderma. The human mite Sarcoptes scabiei is responsible, and resides only in the stratum corneum. Animal mites (mange) may cause papular urticaria but do not infest humans.
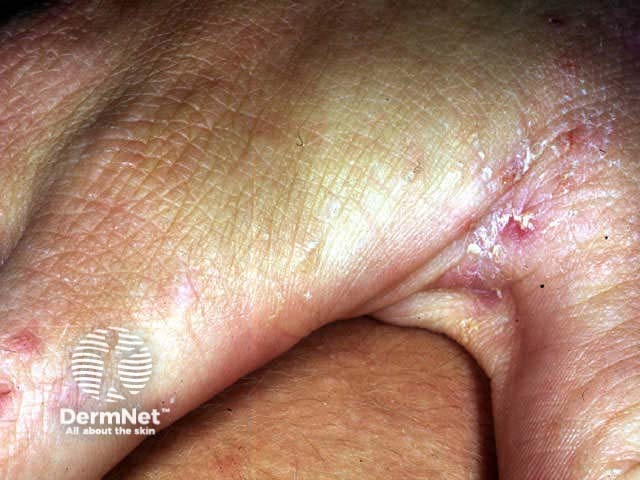
In most cases the infestation predominantly affects hands, wrists and genitals. Fine grey irregular 5-10 mm burrows are most easily identified on the sides of the fingers or volar aspects of the wrist. Using magnification, the mites can be extracted from the distal end of their burrows using a fine needle and examined under low power light microscopy to confirm the diagnosis.
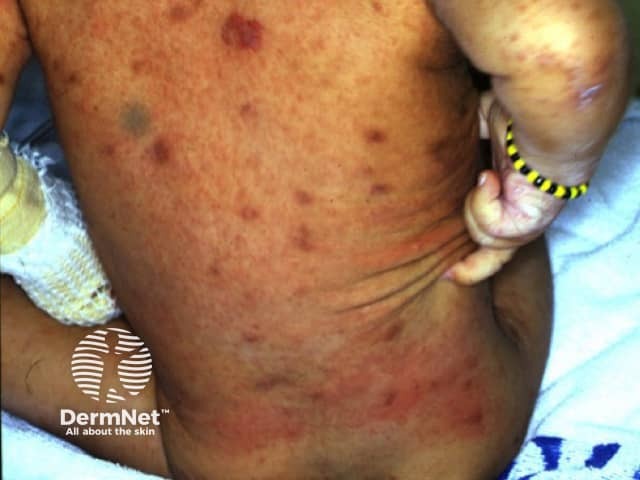
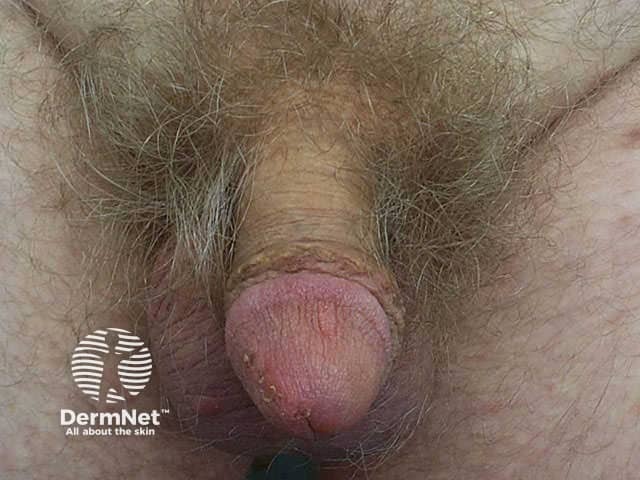
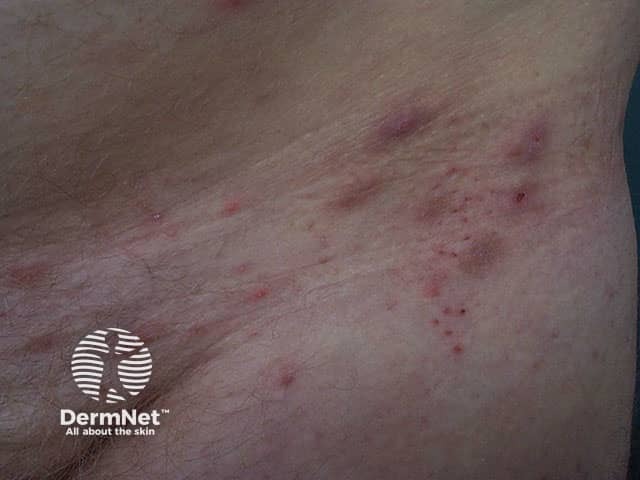
Within days to weeks of infestation an allergic erythematous non-specific papular rash and/or generalised pruritus may appear, sparing the head and neck. Frequently the rash is masked by numerous excoriations due to intense pruritus, particularly at night. Later, papules may be found on the shaft of the penis and dermal nodules in the axillae and/or inguinal regions.
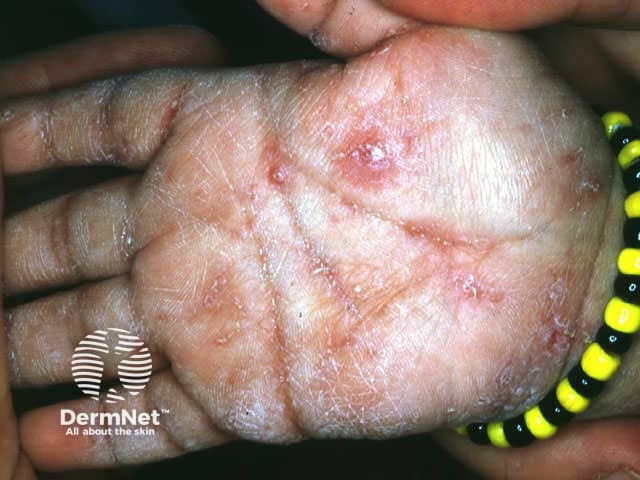
Scabies in infants is characterised by vesicles and pustules on the palms and soles. If they are too young to effectively scratch, burrows may be numerous. Palmoplantar vesicopustules may persist for some weeks or months after effective antiscabetic treatment (acropustulosis).
Scabies mite Interdigital burrows Scabies hypersensitivity Penile and scrotal papules pathognomonic of scabies longstanding scabies Palm of infant 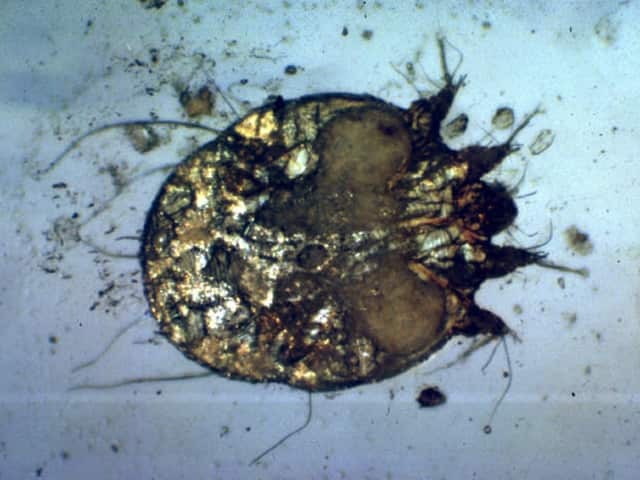
Severe infestation resulting in psoriasis-like hyperkeratosis and scalp involvement (Norwegian scabies) is most likely in immunosuppressed or debilitated elderly patients who are unable to scratch out the arthropods. This form of scabies is highly infectious due to the large number of mites and can infest hundreds of individuals living or working in affected rest homes or hospitals.
 Innumerable burrows |
 Crusting |
 Psoriasis-like plaque |
Scabies may also cause hypersensitivity reactions including urticaria, nummular dermatitis and vasculitis. These may persist after eradication of the responsible mite.
Diagnosis of scabies is based on patient history, physical examination, and demonstration of mites, eggs, or scybala (black or brown football-shaped masses of faeces of scabies) on microscopic examination.
Skin scrapings for microscopy are taken from the closed end of a burrow. Identification of the pinhead-sized mite is easier applying ink to the burrow (wipe off excess ink). Use magnification or dermoscopy. Extract the mite using a blade or non-hypodermic needle (the mite is supposed to cling to it). Scrape the entire length of the burrow several times. Place the scrapings on a glass slide and promptly examine under a light microscope at low power. Live mites may be missed as they often walk off the slide.
In infants, use a dull curette to scrape debris from under the fingernails.
Skin biopsy may show a burrow containing a female mite and ova within the stratum corneum. There is spongiosis and a mixed inflammatory infiltrate in the deep and superficial dermis.
Available topical scabicides include:
The insecticide should be applied to the entire body surface below the hairline and chin, including under the nails and genitals. In infants and bedridden patients it should also be applied to the scalp and face, avoiding eyelids.
Oral ivermectin is available for resistant disease, as 3 mg tablets. The dose is 200-400 µg/kg, repeated in 7 to 14 days. It is particularly useful for institutional outbreaks.
Unfortunately, treatment failure is common. Reasons may include:
All household contacts should be treated at the same time. It is generally wise to advise retreatment once weekly for two or three weeks. In addition, pruritus and eczematisation should be actively managed with emollients, topical steroids and oral antihistamines.
Describe the control of epidemics of institutional scabies.
Information for patients
See the DermNet bookstore