DermNet provides Google Translate, a free machine translation service. Note that this may not provide an exact translation in all languages
Home Bacterial skin infections Mycobacteria CME
Bacterial skin infections CME
Mycobacteria
Created 2008.
Learning objectives
- Recognise possible cutaneous myobacterial infections
Introduction
Mycobacterial infections are uncommonly diagnosed in New Zealand. The responsible acid-fast bacilli are slow-growing opportunistic pathogens but may invade the skin of immunocompetent individuals causing indolent granulomatous disease. If you suspect any of these infections, seek help from a clinical microbiologist or infectious diseases specialist for specific diagnosis and management.
Cutaneous tuberculosis
Direct infection of the skin or mucous membranes with Mycobacterium tuberculosis results in a tuberculous chancre within 2-4 weeks. Lesions most often occur on the knees, elbows, hands, feet and buttocks. The immune response of the patient and the virulence of the mycobacteria determine the type and severity of cutaneous TB.
Cutaneous TB
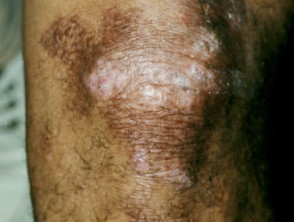
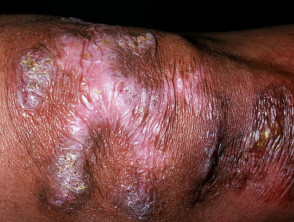
TB verrucosa cutis
TB verrucosa cutis is a solitary brownish-red warty nodule arising after direct inoculation in an immune subject that has had a previous tuberculous infection.
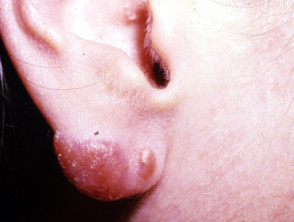
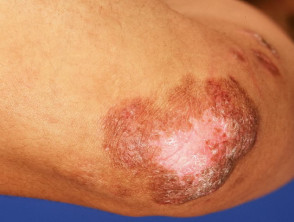
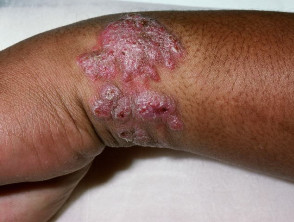
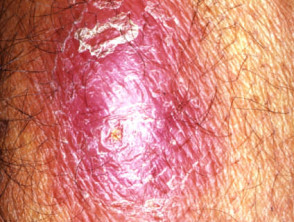
Lupus vulgaris
Lupus vulgaris results in persistent, progressive reddish-brown ‘apple-jelly’ nodules with a gelatinous consistency. Lesions persist for years, leading to disfigurement and sometimes squamous cell carcinoma.
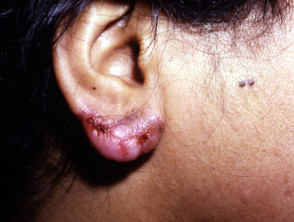
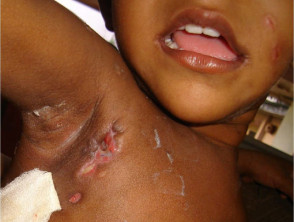
Scrofuloderma
Scrofuloderma presents as firm, painless nodules and may ulcerate. It is due to direct extension from underlying infected lymph nodes, bone or joints.
Miliary TB
Miliary TB results in diffuse small (millet-sized) red papules, ulcers and abscesses. Nowadays it most often arises in immunocompromised patients and has a poor prognosis.
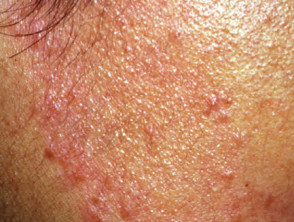
Tuberculid
A tuberculid is a generalised exanthem in patients with moderate or high degree of immunity to TB because of previous infection, which may have cleared up.
- Erythema induratum (Bazin disease) presents as recurring subcutaneous nodules on the back of the legs (mostly women) that may ulcerate and scar.
- Papulonecrotic tuberculid results in crops of recurrent crusted skin papules on knees, elbows, buttocks or lower trunk that heal with scarring after about 6 weeks.
- Lichen scrofulosorum is an extending eruption of small follicular papules in young persons with underlying TB.
Diagnosis of TB
The diagnosis of cutaneous tuberculosis is usually made or confirmed by skin biopsy. Typical tubercles are caseating epithelioid granulomas that contain acid-fast bacilli. Tuberculin skin test, sputum culture and chest X-ray and other relevant radiological tests should be performed. Polymerase chain reaction (PCR) is an emerging diagnostic tool.
Treatment of TB
A combination of antibiotics (isoniazid, rifampicin, pyrazinamide and ethambutol) are generally given over a period of several months and sometimes years.
Occasionally surgical excision of localised cutaneous TB is recommended. Some lesions resolve spontaneously.
Leprosy
Leprosy is a chronic bacterial infection with Mycobacterium leprae. It primarily affects the skin, mucous membranes (e.g. nose), peripheral nervous system (nerve function), eyes and testes. The form the disease takes depends on the immune response to the infection.
Depending on clinical features, leprosy is classified as:
- Indeterminate leprosy (IL)
- Tuberculoid leprosy (TT)
- Borderline tuberculoid leprosy (BT)
- Borderline borderline leprosy (BB)
- Borderline lepromatous leprosy (BL)
- Lepromatous leprosy (LL)
Patients with indeterminate leprosy, may either be cured or progress to one of the other forms of leprosy depending on their immune status. Within each type of leprosy, a patient may remain in that stage, improve to a less debilitating form or worsen to a more debilitating form depending on their immune state. Lepromatous leprosy is the only form that never reverts to a less severe form.
Leprosy is most common in warm, wet areas in the tropics and subtropics. Worldwide prevalence is reported to be around 5.5 million, with 80% of these cases found in 5 countries: India, Indonesia, Myanmar, Brazil and Nigeria. The average incubation period is two to three years, but it can range from 6 months to 40 years or longer. In 90% of patients the first sign of the disease is a feeling of numbness, which may precede skin lesions by a number of years. Temperature is the first sensation lost, followed by light touch, pain and then deep pressure. Sensory loss usually begins in the extremities (toes and fingertips).
The first skin lesion is usually the indeterminate type, which causes one or a few hypopigmented (pale) spots before evolving into the borderline, tuberculoid or lepromatous types.
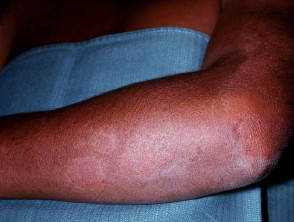
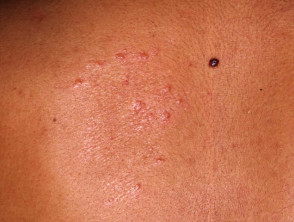
Tuberculoid leprosy
- Can be either one large red patch with well-defined raised borders or a large hypopigmented asymmetrical spot
- Lesions become dry and hairless
- Loss of sensation may occur at site of some lesions
- Tender, thickened nerves with subsequent loss of function are common
- Spontaneous resolution may occur in a few years or it may progress to borderline or rarely lepromatous types
Tuberculoid leprosy
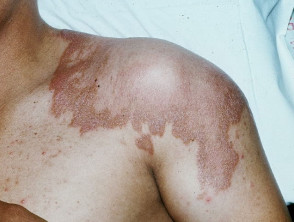
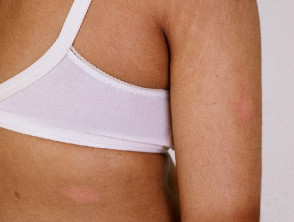
Borderline tuberculoid leprosy
- Similar to tuberculoid type except that lesions are smaller and more numerous
- Disease may stay in this stage or convert back to tuberculoid form, or progress
Borderline tuberculoid leprosy
Borderline borderline leprosy
- Numerous, red, irregularly shaped plaques
- Sensory loss is moderate
- Disease may stay in this stage, improve or worsen
Borderline lepromatous leprosy
- Numerous lesions of all kinds, plaques, macules, papules and nodules. Lesions looking like inverted saucers are common
- Hair growth and sensation are usually not impaired over the lesions
Lepromatous leprosy
- Early nerve involvement may go unnoticed
- Numerous lesions of all kinds, plaques, macules, papules and nodules
- Early symptoms include nasal stuffiness, discharge and bleeding, and swelling of the legs and ankles
- Left untreated, the following problems may occur:
- Skin thickens over forehead (leonine facies), eyebrows and eyelashes are lost, nose becomes misshapen or collapses, ear lobes thicken, upper incisor teeth fall out
- Eye involvement causing photophobia (light sensitivity), glaucoma and blindness
- Skin on legs thickens and forms ulcers when nodules break down
- Testicles shrivel causing sterility and enlarged breasts (males)
- Internal organ infection causing enlarged liver and lymph nodes
- Voice becomes hoarse due to involvement of the larynx
- Slow scarring of peripheral nerves resulting in nerve thickening and sensory loss. Fingers and toes become deformed due to painless repeated trauma.
Diagnosis of leprosy
Leprosy has very characteristic clinical features but the diagnosis must be confirmed because of the need for prolonged treatment with antibiotics. A skin biopsy may show characteristic granulomas (mixed inflammatory cell infiltrate in the deeper layers of the skin, the dermis) and involvement of the nerves. Special staining of the tissue may show acid fast bacilli, the number visible depending on the type of leprosy.
The bacteria may also be found in lepromatous leprosy on smears taken from skin slits made in the ear lobes, but the smears will be negative in the tuberculoid or borderline forms of the disease.
Treatment of leprosy
Antibiotics used first-line to eliminate organisms include dapsone, rifampicin and clofazimine. Varying regimens are used depending on the type of leprosy and the severity of infection. This may be a combination of two or three antibiotics given over varying lengths of time (up to years). Other antibiotics include minocycline, ofloxacin and clarithromycin.
Oral corticosteroids and thalidomide are helpful in preventing nerve damage by reducing swelling. Long courses are necessary to decrease severity of deformities and disabilities.
Surgery may sometimes be used to drain abscesses to restore nerve function, reconstruct collapsed nose, or to improve function or appearance of affected areas.
Patient education is paramount. Leprosy can be cured but it is essential to take the full course of medication. It is no longer infectious once treatment has begun. Patients should be instructed how to deal with existing nerve damage for example protecting numb feet from injury. Physical, social and psychological rehabilitation is a necessary for those in whom neglected disease has caused havoc.
Atypical mycobacteria
Cutaneous atypical mycobacterial infections are caused by:
- Mycobacterium marinum
- Mycobacterium ulcerans
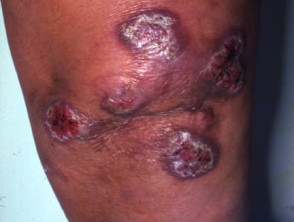
Mycobacterium marinum infection (fishtank granulomas) occurs most often in people with recreational or occupational exposure to contaminated freshwater or saltwater. It presents as one or more papules or pustules on an elbow, knee, foot, knuckle or finger. These that break down to form a crusted nodule or abscess. Sporotrichoid spread along the lines of lymphatic drainage may occur.
Mycobacterium ulcerans (Buruli ulcers) is not seen in New Zealand, but has been reported in Australia and Central and West Africa around areas of lush vegetation and swamps. A solitary nodule of 1-2 cm develops about 7-14 days after infection through broken skin. Over one to two months the nodule may break down to form a shallow ulcer that spreads rapidly and may involve up to 15% of the patient's skin surface. Severe infections may destroy blood vessels, nerves, and invade bone.
Mycobacterium marinum infection
Treatment of atypical mycobacterial infections
Treatment of atypical mycobacterial infections in most cases requires oral antibiotics for 2 to 3 months. Suitable drugs include rifampicin, minocycline, ciprofloxacin, clarithromycin, azithromycin and trimethoprim + sulphamethoxazole.
Antibiotics are usually ineffective in treating large skin lesions caused by Mycobacterium ulcerans. Most lesions eventually spontaneously heal after 6-9 months but may leave behind extensive scarring and disfigurement. Surgical removal of infected lymph nodes and skin lesions is sometimes appropriate.
Activity
Describe adverse reactions to antimycobacterial drugs.
Related information
On DermNet NZ:
Information for patients
Other websites:
- Medscape Reference:
- Clinical Evidence (BMJ): Tuberculosis
- Medline: Moschella SL. An update on the diagnosis and treatment of leprosy. J Am Acad Dermatol. 2005 Sep;51(3):417-26.
Books about skin diseases:
See the DermNet NZ bookstore
Sign up to the newsletter
© 2024 DermNet.
DermNet does not provide an online consultation service. If you have any concerns with your skin or its treatment, see a dermatologist for advice.