DermNet provides Google Translate, a free machine translation service. Note that this may not provide an exact translation in all languages
Home Hand dermatitis CME
Dermatitis
Hand dermatitis
Created 2008.
Learning objectives
- Identify, classify and manage hand dermatitis
Introduction
Hand dermatitis (or eczema) may be classified as being of constitutional, contact or mixed origin. It may or may not be associated with dermatitis at other sites.
- Constitutional origin: atopic dermatitis, pompholyx, nummular dermatitis
- Contact dermatitis: irritant dermatitis, allergic dermatitis
Occupational factors may be important, and having hand dermatitis may prevent the patient from working. Hand dermatitis is particularly common in industries involving cleaning, catering, metalwork, hairdressing, healthcare and mechanical work.
Clinical features
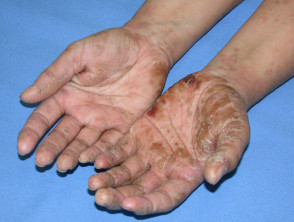
Hand dermatitis may affect palms, dorsum or both. Often it starts as a mild intermittent complaint, but it can become increasingly severe and persistent. It can present acutely (with blisters and oedema) or persist as a chronic condition characterised by dry skin and fissures.
Mostly hand dermatitis is bilateral and fairly symmetrical, but some forms of contact dermatitis may be unilateral or asymmetrical, tending to favour the dominant hand.
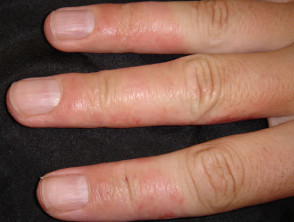
Atopic dermatitis Atopics may develop non-specific hand dermatitis at any age. They are also more prone to contact irritant dermatitis than non-atopics because of defective skin barrier function. Various clinical patterns may arise.
Atopic hand dermatitis
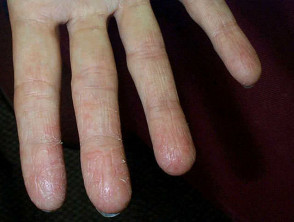
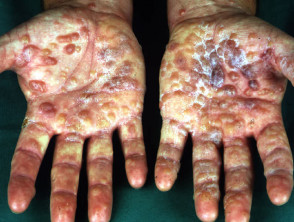
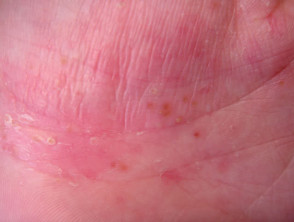
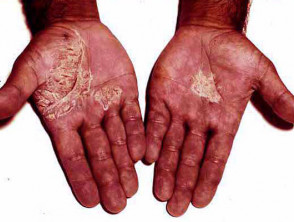
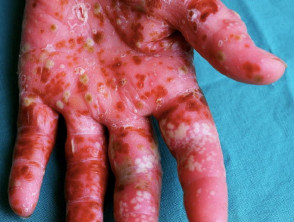
Pompholyx Pompholyx, also known as dyshidrotic or vesicular palmar eczema, refers to acute, chronic or relapsing blistering of the fingers, palms and/or soles. Crops of irritable deep-seated vesicles are followed by scaling and fissuring of the affected areas and may be complicated by Staphylococcus aureus infection. Sweating in response to emotional stress or heat may precipitate vesicles in some individuals. Pompholyx sometimes presents as an id reaction to tinea pedis (‘one foot, two hands’ syndrome) or as an expression of contact dermatitis to nickel.
Pompholyx
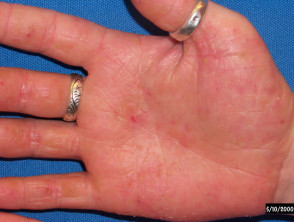
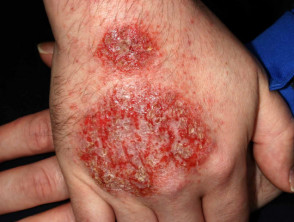
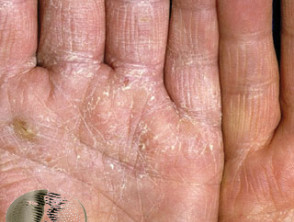
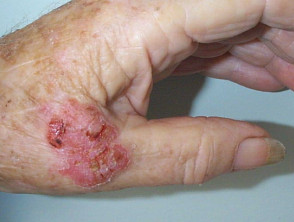
Nummular dermatitis Nummular dermatitis may affect any site including the hands, resulting in round or oval, dry or exudative plaques; surrounding skin may appear entirely normal. Contact factors may or may not play a part as affected plaques can arise in areas of skin that have been injured in some way. In most cases, typical nummular (discoid) plaques are found elsewhere, particularly the forearms and lower legs.
Nummular pattern hand dermatitis
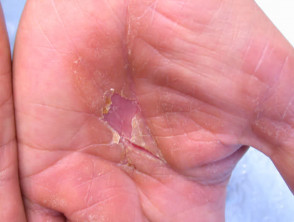
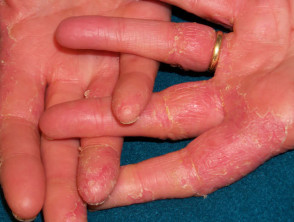
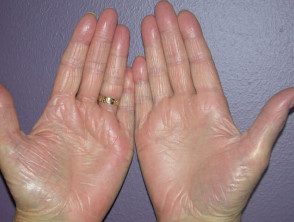
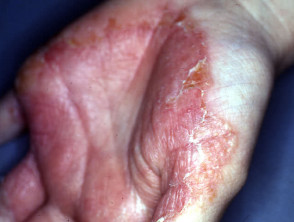
Contact irritant dermatitis
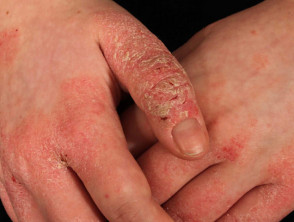
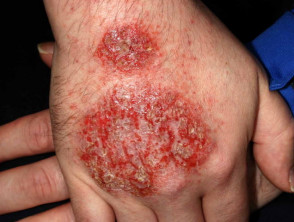
The most common occupational factor leading to dermatitis is frequent immersion of the hands in water especially in combination with detergents and solvents. These injure surface keratinocytes reducing the effectiveness of the stratum corneum as a barrier. Friction and repetitive injury also damage the skin. Irritants result in much more damage once dermatitis has become established; a few minutes carelessness can result in a flare-up that can last for several months.
Contact irritant dermatitis
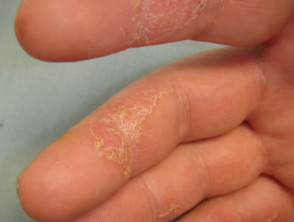
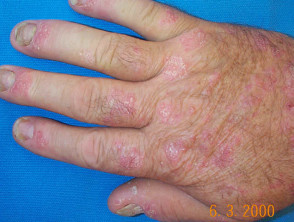
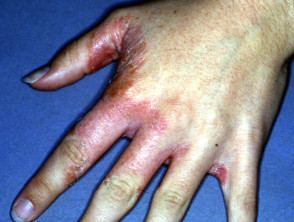
Contact allergic dermatitis
Specific immunological hypersensitivity can result in immediate or delayed reactions.
Immediate contact urticaria is most frequently caused by latex gloves; itchy weals last for about 20 minutes. Other causes include paraphenylenediamine (permanent hair dye), fragrances, plants and fish. Contact urticaria is usually localised but can rarely precipitate generalised anaphylaxis.
Allergic contact dermatitis is delayed for hours to days after the contact has occurred, so it can be difficult to identify the cause. There are a huge number of items that can cause allergic contact dermatitis, including nickel and other metals, fragrances, rubber accelerators, hair dye, adhesives and preservatives.
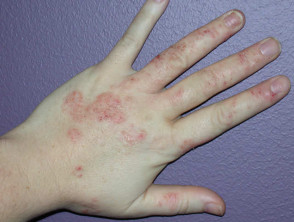
Once a specific allergy has been identified and confirmed by patch testing, contact with the causative material must be strictly avoided long term to clear up the dermatitis and to prevent its recurrence.
Contact allergic dermatitis
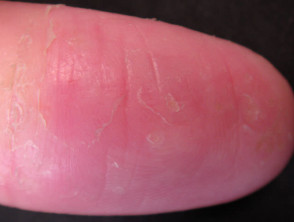
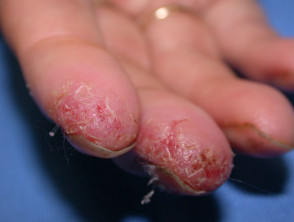
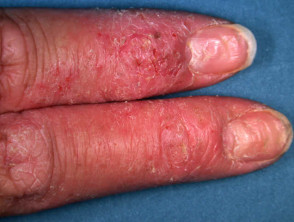
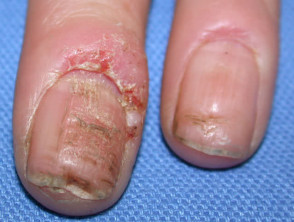
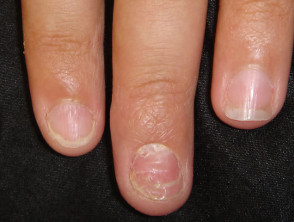
Nail dystrophy Nails are involved when hand dermatitis affects the distal phalanx, particularly when the dermatitis is predominantly palmar but sometimes when it is dorsal. Chronic paronychia may be a variant of dermatitis especially when culture negative for candida.
Nail dystrophy due to dermatitis
Investigations
Skin swabs for Staphylococcus aureus are sometimes required if antibiotic treatment is not proving effective in apparently infected hand dermatitis.
Skin scrapings for microscopy and fungal culture may be necessary to rule out dermatophyte infection.
Patch testing should be carried out in chronic cases or if there is suspicion of specific contact allergy.
Differential diagnosis
Hand dermatitis is most commonly confused with the following skin disorders:
- Psoriasis: well demarcated erythematous, scaly plaques on the palm of dorsum, sometimes associated with typical nail psoriasis. Psoriasis is not particularly itchy but may result in painful fissures.
- Palmoplantar pustulosis (localised pustular psoriasis): persistent pustulosis usually on an erythematous base, affecting central palm and instep.
- Tinea manuum: gradually enlarging unilateral patch with a scaly or pustular edge and positive mycology. Acute tinea is usually due to a zoophilic organism such as Trichophyton verrucosum (cattle ringworm) or Microsporum canis (cat ringworm). Chronic tinea sometimes accompanies tinea pedis and presents with increased skin markings accompanied by mild dryness and peeling. It is most often due to Trichophyton rubrum.
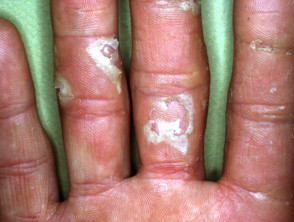
- Keratolysis exfoliativa, also known as ‘exfoliative keratolysis: recurrent focal peeling on fingers, palms and soles.
- Squamous cell carcinoma in situ (Bowen disease) may present as a persistent red scaly patch resembling chronic dermatitis. It is usually asymptomatic.
Skin conditions affecting the hands
Many other inflammatory skin diseases may also affect hands.
Management
Management of hand dermatitis involves:
- Avoidance and/or protection from wet-work and irritants (vinyl and cotton gloves are least likely to sensitise). Rubber and plastic gloves should not be used for prolonged periods because sweating tends to aggravate dermatitis; a cotton or silk lining or extra pair of gloves can be helpful. Dirt or allergens inside the gloves can also be harmful.
- Thick emollient ‘barrier’ creams and ointments as often as desired. A thin smear should be applied to all affected areas before work, and reapplied after washing and whenever the skin dries out. They cannot be used by in some industries for example where oil would prevent fine hand control or stain paint-work.
- Topical corticosteroids: ultra potent creams or ointments for palms, potent creams or ointments for dorsum of hands for 2 to 4 weeks then pulsed at weekends if necessary. Prolonged use may result in tachyphylaxis, atrophy and other adverse effects.
- Oral anti-staphylococcal antibiotics for secondary infection (recognised by pustules, crusting, pain and spreading erythema).
- Wet dressings may be required for the early vesicular phase of pompholyx, using 3% acetic acid or 1:10 000 potassium permanganate compresses.
- If hand dermatitis is severe and preventing function, prescribe oral corticosteroids for 2 to 4 weeks, slowly reducing the dose and discontinuing within another 4-6 weeks.
- Patients with severe recurrent acute dermatitis or chronic hand dermatitis should be referred to a dermatologist. Management will usually include patch testing.
- Resistant and severe cases may require photochemotherapy or immunosuppressive medications, most often azathioprine and ciclosporin. Pompholyx may also respond to dapsone or colchicine.
With careful management, hand dermatitis usually recovers completely. It may be necessary to discontinue work for days, weeks or months; compensation from ACC sometimes applies. Occasionally a change of occupation is necessary.
Activity
Describe the aetiology and management of hand dermatitis in nurses.
Related information
References:
On DermNet NZ:
Information for patients
Other websites:
- Medscape Reference:
Books about skin diseases:
See the DermNet NZ bookstore
Sign up to the newsletter
© 2024 DermNet.
DermNet does not provide an online consultation service. If you have any concerns with your skin or its treatment, see a dermatologist for advice.