DermNet provides Google Translate, a free machine translation service. Note that this may not provide an exact translation in all languages
Home Seborrhoeic dermatitis CME
Dermatitis
Seborrhoeic dermatitis
Created 2008.
Learning objectives
- Identify and manage seborrhoeic dermatitis
Clinical features
Infantile seborrhoeic dermatitis
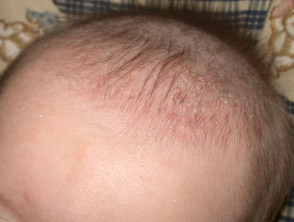
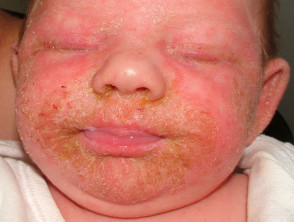
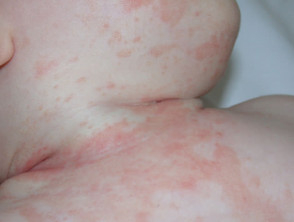
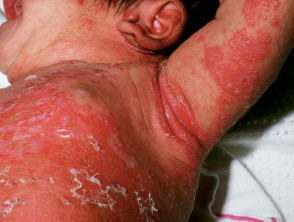
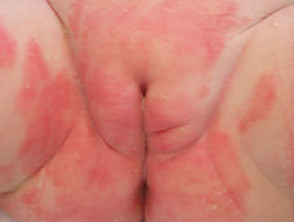
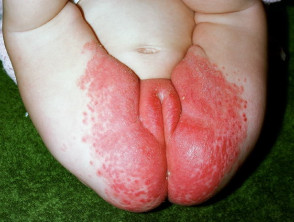
Seborrhoeic dermatitis may affect infants, presenting within the first few months postpartum as cradle cap or napkin dermatitis. It sometimes spreads widely via the flexures. It clears by about twelve months of age.
Seborrhoeic dermatitis appears to be an inflammatory response to malassezia yeasts, which proliferate in oily skin (seborrhoea). In infants it is supposed that maternal androgens are responsible.
Characteristically, the scale is yellowish and greasy or white and bran-like (pityriasiform) associated with variable nummular or annular pale pink to bright red patches. Itching tends to be absent or mild.
Infantile seborrhoeic dermatitis
Adult-pattern seborrhoeic dermatitis
Seborrhoeic dermatitis is a common chronic erythematous scaly dermatosis that may arise in adolescents. It is more prevalent in middle-aged adults.
Seborrhoeic dermatitis affects the following sites:
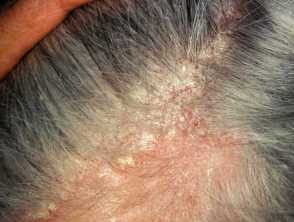
- Scalp: the inflammatory phase of pityriasis capitis (dandruff)
- Other hair bearing areas especially eyebrows, moustache
- Eyelid margins (blepharitis)
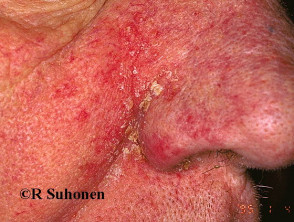
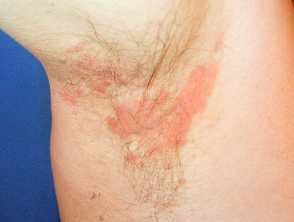
- Skin flexures especially nasolabial fold, postauricular fold, axillae and groin.
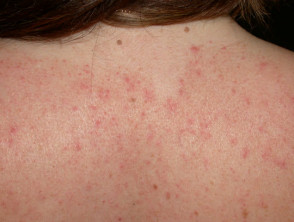
- Upper back and chest
As in infants, seborrhoeic dermatitis appears to be an inflammatory response to malassezia. It sometimes progresses to psoriasis; unusually extensive seborrhoeic dermatitis is sometimes called ‘sebopsoriasis’.
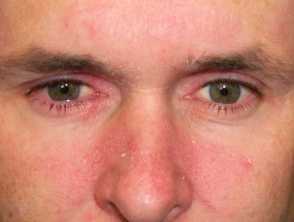
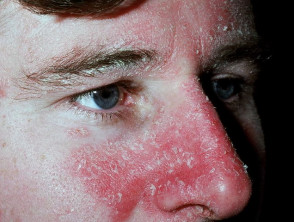
Characteristically, the scale is yellowish and greasy or white and bran-like (pityriasiform) associated with variable nummular or annular pale or salmon pink to bright red patches. Itching tends to be absent or mild.
Excoriation may lead to secondary infection, which is occasionally chronic and difficult to eradicate.
Adult pattern seborrhoeic dermatitis
Investigations
In most cases the diagnosis of seborrhoeic dermatitis is made clinically.
- Microscopy of skin scrapings may be reported as typical for malassezia. Their absence doesn't rule it out.
- Culture and sensitivity of skin swabs may reveal Staphylococcus aureus
- Biopsy shows eczematous and psoriasiform features.
Differential diagnosis
Seborrhoeic dermatitis may be confused with or may coexist with:
- Psoriasis (thicker plaques, larger scales, typical distribution, nail involvement)
- Atopic dermatitis (very itchy, lichenified)
- Rosacea (flushing, scattered dome-shaped papules and pustules); very rare under the age of 25
- Discoid lupus erythematosus (indurated plaques, follicular plugging, scarring); rare in children
- Systemic lupus erythematosus (unwell patient, photosensitivity, arthritis); rare in children
- Perioral dermatitis (clusted flakey papules in typical periorificial distribution )
Management
Management of cradle cap may consist of gently washing with a baby shampoo after a proprietary oil or lotion has been used to soften the scales (e.g. Egocappol, Egozite lotion). More troublesome seborrhoeic dermatitis affecting the scalp can be managed as in an adult:
- Shampoo twice weekly (or if desired, more frequently) with antidandruff shampoo containing:
- Keratolytics such as salicylic acid and sulphur
- Antifungal agents especially ketoconazole and ciclopirox (also miconazole, selenium sulphide and zinc pyrithione)
- Coal tar or pine tar
- Intermittent use of mild potency topical steroid lotion
- Leave-on tar preparation e.g. coconut oil compound ointment, washed off after an hour or so.
Management of seborrhoeic dermatitis affecting non-hair bearing areas:
- Minimal use of emollients (malassezia is lipophilic)
- Cleanse with non-soap cleanser or anti-dandruff shampoo
- Keratolytic cleansers or creams containing salicylic acid and/or sulphur
- Topical antifungal cream especially ketoconazole or ciclopirox
- Intermittent use of mild topical steroid or tar preparations
Activity
Describe the use of coal tar in the management of scalp problems.
Related information
References:
On DermNet NZ:
Information for patients
Other websites:
- Medscape Reference: Seborrhoeic dermatitis
- Medscape: Dandruff and Seborrheic Dermatitis from U.S. Pharmacist
- Clinical evidence (BMJ): Seborrhoeic dermatitis
Books about skin diseases:
See the DermNet NZ bookstore
Sign up to the newsletter
© 2024 DermNet.
DermNet does not provide an online consultation service. If you have any concerns with your skin or its treatment, see a dermatologist for advice.