Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Created 2008.
Dermoscopy (also called dermatoscopy), is an essential tool for dermatologists, plastic surgeons, general practitioners and other health professionals attempting early diagnosis of melanoma. Using dermoscopy to evaluate pigmented lesions, the abnormal structural features of melanoma can be identified, borderline lesions may be closely observed and benign lesions can be confidently diagnosed without the need for biopsy. Dermoscopy is also increasingly useful in diagnosis of non-pigmented skin lesions and inflammatory dermatoses.
Dermoscopy performed by experts results in enhanced accuracy of diagnosis, with increased sensitivity and specificity for the detection of early melanoma. But dermoscopy is hard! Dermoscopy should never override a strong clinical suspicion of melanoma. Beginner dermoscopists are also likely to overdiagnose melanoma.
We recommend progressing slowly through each topic in this course over some weeks, working through the assessments, and reading the online resources. There are several excellent textbooks available.
It is essential to practise dermoscopy at every opportunity. Where possible, use digital dermoscopy (photographic images) to record your own patient's suspicious or atypical skin lesions and review the images on screen, especially those in which you have a pathological diagnosis.
Derm(at)oscopy refers to the examination of the skin using skin surface microscopy, and is also sometimes called ‘epiluminoscopy’ and ‘epiluminescent microscopy’. Dermoscopy is mainly used to evaluate pigmented lesions in order to distinguish malignant skin lesions, such as melanoma and pigmented basal cell carcinoma, from benign melanocytic naevi and seborrhoeic keratoses.
Dermoscopy requirements include a high quality lens for 10 to 14-times magnification and a lighting system (a dermatoscope). This enables visualisation of subsurface structures and patterns. Hand-held devices are usually lightweight and battery-powered.
Fluid immersion and polarised dermatoscopes are available.
Skin examination DermoGenius® Dermlite® Dermlite®II-Pro 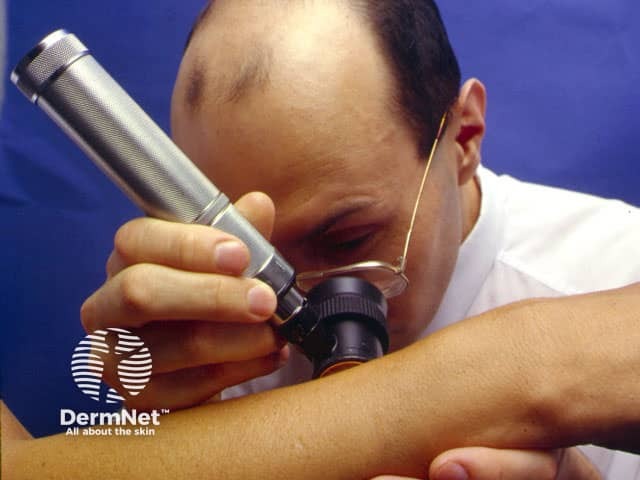



Several studies have demonstrated that dermoscopy is useful in the identification of melanoma, when used by experts.
New users may unfortunately become less accurate at diagnosis at first, paradoxically increasing the number of unnecessary excisions.
Convenient attachments to dermoscopy devices allow high quality video or still digital photography, allowing review on a computer screen and comparison with images taken at follow-up appointments. It is estimated that dermoscopy can detect 92% of melanomas immediately because of typical features. The remaining 8% do not have identifying features and are diagnosed because of change in an atypical lesion. Structural change can be detected in superficial melanomas within 3 to 6 months.
Nikon 995 with DermLite Detecting change over time 


Computer software can be used to archive the images and allow remote diagnosis and reporting by a dermatologist (digital epiluminescence microscopy, teledermoscopy, mole mapping). This is the system used by MoleMap NZ, who have provided many of the images used for this course.
Some systems such as SolarScan® and MelaFind offer smart programs to aid in diagnosis by comparing the new image with stored cases with typical features of benign and malignant pigmented skin lesions. Given good images of the appropriate lesion, they may be as accurate as an expert dermatologist. However, they are not particularly useful for non-pigmented lesions and they can't make the decision which lesions should be imaged.
The SIAscope™ (SIA: Spectrophotometric Intracutaneous Analysis) is an automated dermoscopy device that uses 12 wavebands to evaluate the skin (rather than conventional broadband white light). Patterns of collagen, vascular and melanin distribution are demonstrated within the lesion – the spectrophotometric analysis of a skin lesion.
Surveillance of patients at risk for melanomas is greatly aided by the use of high quality images of the entire integument. It is particularly useful for those with atypical naevi or many moles. Several systems have been described, using about 24 to 30 images as conventional transparency slides, prints, or digital systems. New lesions can be identified by careful comparison with older images. Lesions that are of concern can be kept under review, reducing unnecessary excisions if they are stable. Significant change in size or shape of individual lesions may prompt biopsy. However, close-up and dermoscopic images of the lesion under scrutiny are much more useful for this purpose.
Digital whole body imaging can be used for mole mapping, i.e. precisely locating an individual lesion that has been imaged by macro or dermoscopic photography. It is not necessary to individually photograph every lesion.
Naevi in the same individual tend to resemble one another but melanoma often deviates from the individual's usual naevus pattern. Watch out for the Ugly Duckling, i.e., a pigmented lesion that is different from the patient's other moles. An extension of this idea is the Little Red Riding Hood sign, where a melanoma is observed to differ from naevi only when seen close-up – the sharp teeth of the wolf.
Whole body photography should be supplemented by regular physician examinations. Skin self-examination is also valuable, and the patient may find it helpful to have copies as prints or digital images.
However, new, changed, and regressed nevi are common in younger patients. A new or changed pigmented lesion is more likely to be a melanoma in patients older than 50 years.
Nikon 995 with DermLite Detecting change over time 


Evaluate handheld dermatoscopes (cost, ease of use, photographic application).
See the DermNet bookstore.
The links below take you to Amazon.com. Purchase via this route provides NZ DermNet with a small commission. Select Dermoscopy from the dropdown search menu.