DermNet provides Google Translate, a free machine translation service. Note that this may not provide an exact translation in all languages
Home Dermatological emergencies Blistering skin diseases CME
Dermatological emergencies
Blistering skin diseases
Created 2008.
Learning objectives
- Recognise and classify blistering skin diseases
Introduction
Blisters are accumulations of fluid within or under the epidermis. Diagnosis depends on the site of the intercellular split as shown in the table below.
| Site of blister | Characteristics | Differential diagnosis | Image |
|---|---|---|---|
| Subcorneal | Very thin roof breaks easily | Impetigo, miliaria, SSSS | 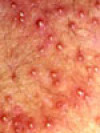 Miliaria |
| Intra-epidermal | Thin roof ruptures to leave denuded surface | Acute eczema, varicella, herpes simplex, pemphigus |  Eczema |
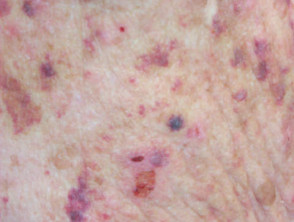
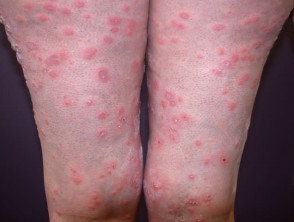
| Subepidermal | Tense roof often remain intact | Bullous pemphigoid, dermatitis herpetiformis, erythema multiforme, TEN, friction blisters | 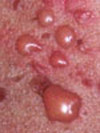 Systemic lupus erythematosus |
SSSS: Staphylococcal scalded skin syndrome
TEN: Toxic epidermal necrolysis
Inherited blistering diseases
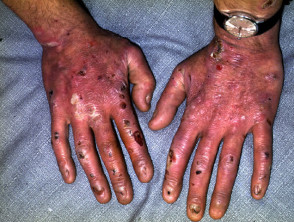
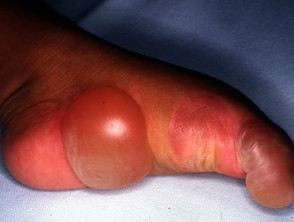
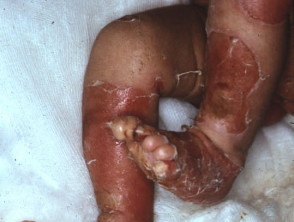
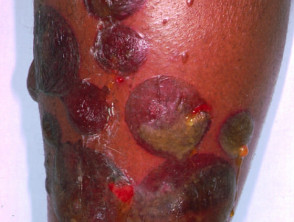
Epidermolysis bullosa (EB) refers to a group of inherited disorders in which there are mutations in specific keratin proteins (EB simplex), hemidesmosomes (junctional EB), anchoring filaments or type VII collagen (dystrophic EB). Minor trauma results in blisters and erosions, the split site and severity depending on the specific defect.
Varying presentations of epidermolysis bullosa
Immunobullous eruptions
There are at least 9 distinct immunobullous diseases due to autoantibodies directed at differing components of the desmosome complex. Skin biopsy and direct immunofluorescence are diagnostic and there may be detectable circulating skin antibodies. High dose corticosteroids and immunosuppressive medication may be required for control.
Bullous pemphigoid
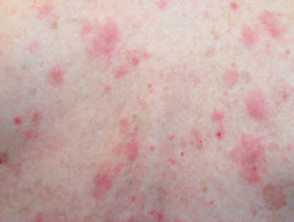
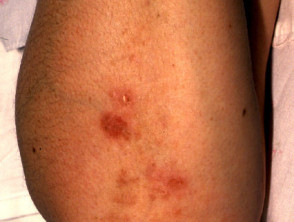
Bullous pemphigoid is the most common immunobullous disease and affects the elderly. Early signs include various subacute itchy rashes on any site, particularly the flexures (submamammary, inguinal):
- Dermatitis-like: dry or exudative discoid eczema
- Urticaria-like: erythematous urticated plaques
- Non-specific: patchy erythema and/or dryness
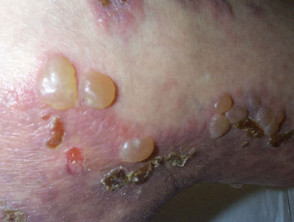
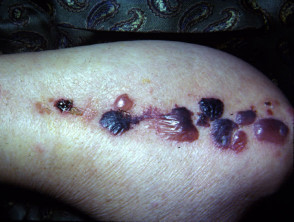
Eventually (days to weeks) the plaques evolve into subepidermal bullae, or these may arise from apparently normal skin.
- Tense fluid-filled clear or haemorrhagic blisters
- Erosions and crusted lesions
- Excoriations and bruising
Purulent lesions may or may not indicate secondary infection (staphylococcal and/or streptococcal), and in such cases spreading erythema may or may not be due to cellulitis.
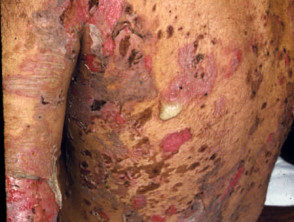
Varying presentations of bullous pemphigoid
Dermatitis herpetiformis
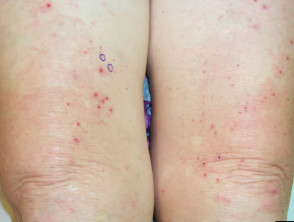
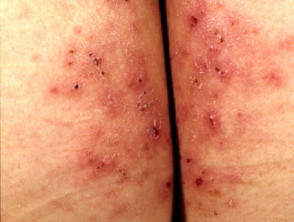
Dermatitis herpetiformis mostly affects young adults but may present at any age as a chronic prurigo. It mainly affects scalp, elbows, buttocks, knees and shoulders. Diagnosis is made by skin biopsy and rapid improvement on dapsone. Signs include:
- Papules
- Vesicles
- Crusted excoriations
Despite distressing itch, signs may be quite subtle (hence few photographs available!).
Dermatitis herpetiformis (DH) is associated with gluten-sensitive enteropathy in most cases (at least 85%) although this may be asymptomatic. Symptoms (in 10%) include:
- Bloating
- Abdominal pain
- Diarrhoea
- Weight loss
- Failure to thrive
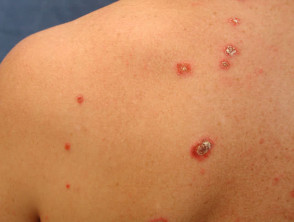
Dermatitis herpetiformis
Pemphigus
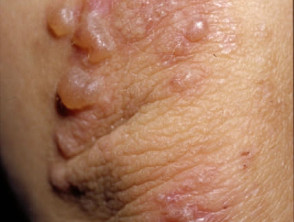
Pemphigus has at least 7 subtypes caused by pathogenic IgG antibodies to intraepidermal cell adhesion molecules. It is diagnosed by clinical presentation and skin biopsy. The most common subtypes are:
- Pemphigus vulgaris
- Pemphigus foliaceus
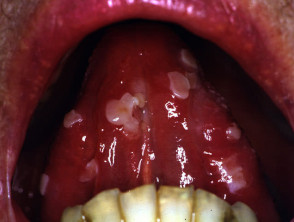
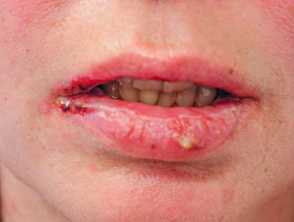
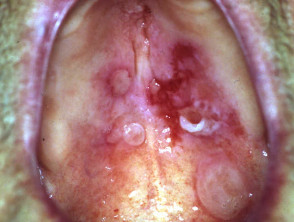
Pemphigus vulgaris is potentially fatal; it usually presents with acute or subacute extensive oral ulceration followed by widespread cutaneous denudation. It appears to be particularly common in middle-aged patients from the Indian subcontinent.
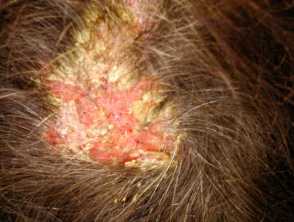
Pemphigus foliaceus affects the elderly and presents with erosions affecting primarily seborrhoeic areas (scalp, face, chest). It is much less severe than pemphigus vulgaris.
Pemphigus may be precipitated by:
- Drugs (with or without antibody formation): penicillamine, captopril, enalapril and others
- Neoplasia: lymphoma, bronchogenic squamous cell carcinoma and others
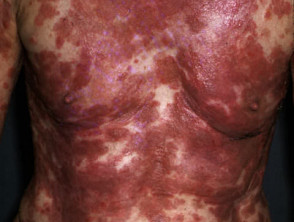
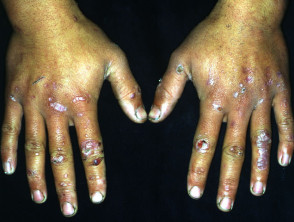
Pemphigus
Other immunobullous diseases
Other rare immunobullous diseases include:
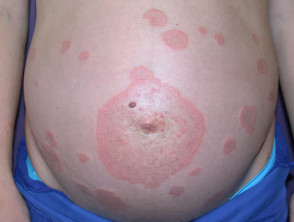
- Pemphigoid gestationis: bullous eruption of pregnancy (autoantibodies directed against BP180 antigen)
- Cicatricial (benign mucosal) pemphigoid: blisters affecting mouth, nose, eyelids and genitocrural sites that form scars (autoantibodies directed against anchoring filaments)
- Epidermolysis bullosa acquisita: blistering following trauma (autoantibodies directed against NC1 domain of type VII collagen)
- Linear IgA dermatosis: annular blistering
Rare immunobullous diseases
Investigations
Skin biopsy and direct immunofluorescence (DIF) are crucial for diagnosis of immunobullous diseases.
| Disease | Biopsy features | DIF |
|---|---|---|
| Bullous pemphigoid |
|
Linear IgG, C3 in BMZ (lamina lucida) |
| Dermatitis herpetiformis |
|
Granular IgA in tips of papillae |
| Pemphigus vulgaris |
|
IgG within suprabasal intercellular spaces |
| Pemphigus foliaceus |
|
IgG within upper epidermal intercellular spaces |
| Paraneoplastic pemphigus |
|
IgG within epidermal intercellular spaces and BMZ |
| Pemphigoid gestationis |
|
Linear C3 in BMZ (lamina lucida) |
| Cicatricial pemphigoid |
|
Linear IgG, C3 in BMZ (lamina lucida) |
| Epidermolysis bullosa acquisita |
|
Linear IgG, C3 in BMZ (upper dermis) |
| Linear IgA dermatosis |
|
Linear IgA, C3 in BMZ |
BMZ: basement membrane zone
EM: electron microscopy
Other tests
Specific immunoreactive proteins detected using histochemistry on skin biopsies are beyond the scope of this article, and they are not evaluated in routine clinical practice.
There may be circulating ‘skin antibodies’ in immunobullous diseases. These are detected by indirect immunofluoresce of serum.
Dermatitis herpetiformis
Additional investigations to detect gluten enteropathy should include:
- Serum IgA autoantibodies to reticulin, gliadin and/or endomysium
- Iron and folate (malabsorption can be detected in 20% patients with DH)
- Refer to gastroenterologist for small bowel endoscopy and biopsy
Management
Dermatitis herpetiformis
- Dapsone: doses of 50-300mg daily rapidly controls itching and blistering
- Gluten-free diet: required long term for control (avoid barley, rye, and wheat)
- Refer to Coeliac Society for help
Other immunobullous diseases
Control of immunobullous diseases can be very challenging and is best left to a dermatologist. Maintenance therapy is usually required for years if not lifelong and is likely to result in significant complications.
- Systemic steroids: prednisone 40 - 100mg daily; pulsed IV methyl prednisolone.
- Bone prophylaxis requires DEXA scan, calcium and biphosphonates
- May precipitate diabetes, hypertension etc
- Ultrapotent topical steroids
- Unsuitable for widespread disease
- Tetracyclines: doxycycline or minocycline 200mg daily
- Niacinamide
- Other antibiotics: dapsone, salazopyrin, erythromycin
- Immunosuppressive agents: azathioprine, methotrexate, chlorambucil, cyclosporin, tacrolimus, mycophenolate mofetil, cyclophosphamide
- Monitor bp and blood (CBC, LFT, Renal function, lipids etc)
- Intravenous immunoglobulin (very expensive)
- Plasma exchange
Activity
Describe the adverse effects of dapsone.
Related information
On DermNet NZ:
Information for patients
Other websites:
- Medscape Reference:
- Manufactured food database
- Cochrane reviews
Books about skin diseases:
See the DermNet NZ bookstore
Sign up to the newsletter
© 2024 DermNet.
DermNet does not provide an online consultation service. If you have any concerns with your skin or its treatment, see a dermatologist for advice.