DermNet provides Google Translate, a free machine translation service. Note that this may not provide an exact translation in all languages
Home Dermatological emergencies Neutrophilic dermatoses CME
Dermatological emergencies
Neutrophilic dermatoses
Created 2008.
Learning objectives
- Recognise neutrophilic dermatoses
Introduction
Dermatoses with dense dermal infiltrates of neutrophils include:
- Acute febrile neutrophilic dermatosis
- Pyoderma gangrenosum (PG)
- Overlap disorders
Neutrophilic dermatoses are probably mediated through helper T cell type 1 cytokines (IL-2, INF-γ) rather than helper T cell type 2 cytokines (IL-4). This results in the stimulation of a cytokine cascade, which might be responsible for the local and systemic activation of neutrophils and histiocytes.
Clinical features
Acute febrile neutrophilic dermatosis
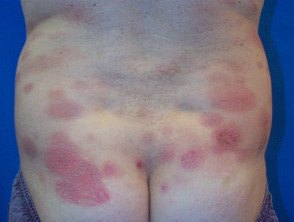
Acute febrile neutrophilic dermatosis or Sweet disease presents acutely as a rash accompanied by systemic symptoms. The skin lesions are rapidly evolving juicy often ‘pseudo-vesicular’ plaques or nodules accompanied by fever, leukocytosis, conjunctivitis and arthralgia. The lesions are most often located asymmetrically on the upper extremities, neck and face and may be painful. There may also be oral ulcers.
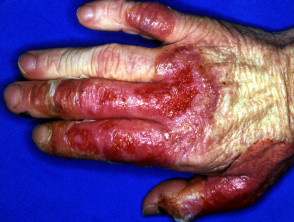
Acute febrile neutrophilic dermatosis arising on the back of the hands is sometimes called pustular vasculitis.
Acute febrile neutrophilic dermatosis may be idiopathic, or arise in association with:
- Infection, most often beta haemolytic streptococcus or other upper respiratory tract infection
- Malignancy, most often acute myeloid leukaemia
- Drugs
Acute febrile neutrophilic dermatosis
Pyoderma gangrenosum
Pyoderma gangrenosum is associated with inflammatory bowel disease, rheumatoid arthritis and haematological malignancies but occasionally arises in otherwise healthy individuals.
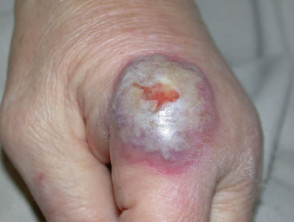
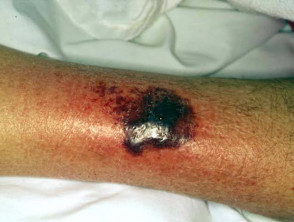
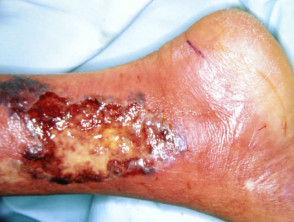
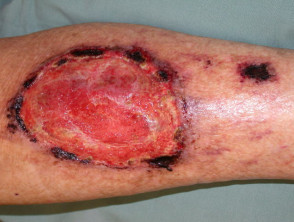
Pyoderma gangrenosum results in acute and often severe ulceration characterised by an overhanging purple or black necrotic edge and severe pain. It most commonly arises on the lower legs but may appear on any site. It heals with cribriform scarring but may be very difficult to control.
Pyoderma gangrenosum (PG)
Investigations
Acute febrile neutrophilic dermatosis
Full blood count shows neutrophilia (and sometimes myelogenous leukaemia). Acute febrile neutrophilic dermatosis may be associated with an acute infection, so other investigations will depend on symptoms.
Skin biopsy characteristically shows:
- Oedema of upper dermis
- Neutrophilic and mixed inflammatory infiltrate
- No true vasculitis (debated)
Pyoderma gangrenosum
Diagnosis is made clinically. A skin biopsy is generally used to rule out other causes of skin ulceration. In pyoderma gangrenosum, the biopsy characteristically shows:
- Epidermal necrosis and ulceration
- Neutrophilic and mixed inflammatory infiltrate
- No true vasculitis (debated)
Direct immunofluorescence is generally negative.
It is important to culture a swab and if necessary, tissue from the ulcer for bacteria including slow growing mycobacteria and fungi.
Management
Acute febrile neutrophilic dermatosis
Acute febrile neutrophilic dermatosis may spontaneously resolve within two or three months, or more promptly with treatment of underlying infection or on withdrawal of the causative drug.
Treatment may also include:
- Systemic corticosteroids
- Topical and/or intralesional corticosteroids
- Oral potassium iodide
- Colchicine
- Dapsone
These medications are usually very effective and only required for a few weeks. Sweet disease may however recur, in which case the treatment may be repeated.
Pyoderma gangrenosum
Pyoderma gangrenosum often requires one or more systemic immune suppressive medications and may recalcitrant to all drugs. Treatment may include:
- Treatment of underlying disease
- A variety of occlusive dressings
- Attention to concomitant venous disease (however compression may be intolerable due to ulcer pain)
- Topical calcineurin inhibitors
- Tetracycline antibiotics
- Oral or pulse intravenous corticosteroids
- Ciclosporin
- Mycophenolate
Activity
Find out which drugs can precipitate acute febrile neutrophilic dermatosis.
Related information
On DermNet NZ:
Information for patients
Other websites:
- Medscape Reference:
Books about skin diseases:
See the DermNet NZ bookstore
Sign up to the newsletter
© 2024 DermNet.
DermNet does not provide an online consultation service. If you have any concerns with your skin or its treatment, see a dermatologist for advice.