DermNet provides Google Translate, a free machine translation service. Note that this may not provide an exact translation in all languages
Home Follicular disorders Oral treatment for acne CME
Follicular disorders
Oral therapy for acne
Created 2009.
Learning objectives
- Prescribe oral antibiotics and hormonal therapy for acne appropriately and safely
- Understand indications for isotretinoin and its common adverse effects
Introduction
Oral treatment is often prescribed for acne. The choice depends on:
- Severity of the acne
- Male or female subject
- Previous response to treatment
- Risks of specific treatment to the individual
Antibacterial agents
Systemic antibacterials for the treatment of moderate-to-severe acne include tetracycline, doxycycline, minocycline, erythromycin and trimethoprim + sulphamethoxazole. They reduce the number of pathogenic organisms and they have anti-inflammatory actions, for example reducing Cutibacterium acnes-induced neutrophil chemotaxis and reactive-oxygen species.
Poor clinical response can be due to:
- Poor compliance
- Too short a course
- Gram-negative folliculitis
- Resistance of P. acnes
- Seborrhoea
The same antibacterial should be prescribed for at least 3 months and usually for an average of 6 months. To prevent the development of resistance, they should be combined with a topical retinoid or benzoyl peroxide rather than a topical antibiotic. Systemic isotretinoin should be considered if one or two antibacterials have been tried without success.
Other chronic skin diseases routinely treated with antibiotics include:
- Folliculitis
- Rosacea
- Immmunobullous diseases
- Granulomatous diseases of infectious and non-infectious origin
- Other diverse inflammatory diseases including urticaria and lichen planus
Antibiotics are used empirically in these conditions. There are very few published randomised blinded trials to support their use, but benefit is generally self-evident in practice. Mostly the mechanism of action is unknown; probably an anti-inflammatory effect in most conditions but antimicrobial action may be important in others.
Tetracyclines are particularly useful as they are well tolerated and generally safe when used long term. In children under 8 and pregnant females it can be replaced by erythromycin, but this is probably less effective and has important interactions with other drugs. Because of a higher risk of serious adverse events, cotrimoxazole is rarely indicated.
Hypersensitivity to tetracyclines may result in:
- Various types of allergic skin rash
- Idiosyncratic hepatitis
- Raised intracranial pressure
- Minocycline has rarely been reported to precipitate systemic lupus erythematosus, vasculitis, autoimmune hepatitis and drug hypersensitivity syndrome (prolonged rash, fever, lymphadenopathy and organ failure). Prolonged courses in adults may also result in bluish pigmentation of nails, skin, teeth and internal organs.
Other adverse effects include:
- Discoloration of growing teeth (avoid in pregnancy and childhood)
- Oesophagitis (take with a full glass of water)
- Photosensitivity, especially doxycycline (take in early evening)
- Candidiasis (prophylaxis may be necessary in adult women)
Hormonal treatment
Hormonal treatment is an alternative regimen in female acne, especially in the presence of polycystic ovarian syndrome or when oral contraception is desired.
Cmbined oral contraceptives containing ethinyl oestrodiol and minimally androgenic progesterones such as desogestrel (Marvelon™, Mercilon™), gestodene (Femodene™, Minulet™) or norgestimate should be tried initially, for a 3 to 6-month course as a minimum. Progestogen-only pills are generally ineffective. Injected medroxyprogesterone (Depo Provera™) tends to aggravate acne.
Specific anti-androgenic contraceptive pills have a combination of ethinyl estradiol and progestins such as cyproterone acetate (Diane 35™, Estelle 35™), drospirenone (Yasmin™, Yaz™) or dienogest. The result is reduced seborrhoea in 80% of users, improvement in acne (up to 70%), in hirsutism (up to 40%) and androgen-related alopecia (up to 80%). They are generally well tolerated (especially those contining drospirenone or dienogest), the main adverse effects of being nonspecific or as expected (headache, breast tenderness and nausea). They have no clinically relevant effects on metabolic or liver functions or on bodyweight. However, those containing cyproterone have been reported to be twice as likely to cause venous thromboembolic disease as second generation pills.
Larger doses of cyproterone are sometimes used to treat hirsutism and polycystic ovarian syndrome but are rarely necessary for acne. Each cycle, 50-200mg is taken for 10 days and is usually combined with an oral contraceptive. Main adverse effects are menstrual irregularities, weight increase and depression.
Spironolactone also has antiandrogenic effects. It is used to treat female acne and hirsutism at a dose of 50 mg twice weekly to 200mg once daily. Main adverse effects are breast pain and menstrual irregularities (combine with oral contraceptive agent).
Isotretinoin
Isotretinoin is an extremely effective treatment for acne and appears to work by reducing sebum production. The indications are:
- Nodulocystic acne
- Severe disfiguring inflammatory acne vulgaris
- Acne which is resulting in scarring
- Moderate acne which has failed to respond to topical agents combined with oral antibiotics, or in women, hormonal treatment
- Acne which relapses rapidly on discontinuing treatment
- Acne which has persisted for several years, or arises in an individual over 25 years old
- Dysmorphophobic acne
- When the acne has a significant adverse occupational, social or psychological effect on the patient's life
It is also used for antibiotic-resistant rosacea, folliculitis and rarely other inflammatory skin diseases. In New Zealand Pharmaceutical Schedule subsidy is restricted and requires Special Authority application.
It has numerous side effects primarily mucocutaneous dryness.
- Teratogenicity (causes major human fetal abnormalities): isotretinoin must not be used by females who are pregnant or who intend to become pregnant during therapy or at any time for at least one month following the discontinuation of therapy;
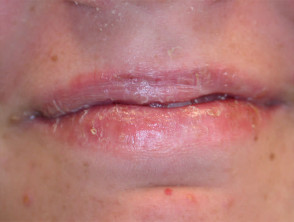
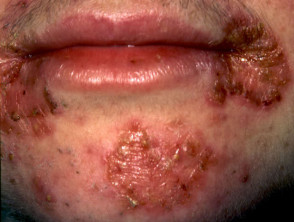
- Mucocutaneous adverse effects: dry fragile lips, skin, nose and eyes, increased chance of skin infections, delayed wound healing;
- Arthralgias, myalgias, raised intracranial pressure (oral retinoids must not be taken with tetracycline or tetracycline derivatives), decreased night vision;
- Hepatotoxicity (rare) and hypertriglyceridaemia (more common);
- Flare of inflammatory acne, including acne fulminans;
- It has been associated with severe depression but it is not known whether the drug is causal as depression and suicide are statistically more common in teenagers with untreated acne.
Adverse effects of isotretinoin
A course of isotretinoin 0.5-1 mg/kg/day ranges from 4 to 12 months (usually 5 to 6 months) and may be repeated if necessary.
Activity
Review the evidence that anti-acne medication improves or aggravates depression in adolescents with acne.
Related information
References:
On DermNet NZ:
Information for patients
Other websites:
- Acne vulgaris – Best Practice (BMJ)
- Acne: a guide to prescribing isotretinoin – BMJ Learning
- Advice on the safe introduction and continued use of isotretinoin in acne in the UK 2010 MJD Goodfield, NH Cox, A Bowser, JC McMillan, LG Millard, NB Simpson, AD Ormerod, BJD, Vol. 162, No. 5, June 2010 (p1172-1179) – British Association of Dermatologists
- Medscape:
- Psychosocial Impact of Acne Vulgaris: Evaluating the Evidence From Skin Therapy Letter, August 19, 2005
- Anxiety, Depression, and Nature of Acne Vulgaris in Adolescents Medline abstracts, September 2000
Books about skin diseases:
See the DermNet NZ bookstore
Sign up to the newsletter
© 2024 DermNet.
DermNet does not provide an online consultation service. If you have any concerns with your skin or its treatment, see a dermatologist for advice.