DermNet provides Google Translate, a free machine translation service. Note that this may not provide an exact translation in all languages
Home Fungal skin infections Mycology CME
Fungal skin infections
Mycology
Created 2009.
Learning objectives
- Describe how to collect samples for mycology and interpret laboratory results
Dermatophyte infections
Fungi are classified according to the appearance of microscopy and in culture, and by the method of reproduction.
Growing fungi have branched filaments called hyphae, which make up the mycelium (like branches are part of a tree). Some fungi are compartmented by cross-walls (called septae). Arthrospores are made up of fragments of the hyphae, breaking off at the septae. Asexual spores (conidia) form on conidiophores. The sexual reproductive phase of many fungi is unknown; these are fungi imperfecta.
Superficial fungal infections affect the outer layers of the skin, the nails and hair. Fungi causing superficial fungal infections are dermatophytes of the genera Trichophyton, Microsporum and Epidermophyton.
Dermatophyte infections (tinea) are named according to the site affected.
Diagnosis of dermatophyte infections
Skin scrapings and nail clippings are taken to establish or confirm the diagnosis of a fungal infection by microscopy and culture (mycology).
Scrapings of scale are best taken from the leading edge of the rash after the skin has been cleaned with alcohol. Gently remove the surface skin using a blade or curette and place in a sterile container or a black paper envelope.
- If it isn't scaly, it isn't a fungal infection!
- Strip off surface skin with adhesive tape, which is then stuck on a glass slide (but your laboratory may not be able to culture the sample).
- Gently pull out infected hair.
- Use a toothbrush to collect scale from infected scalp
- Nail clippings should include debris scraped from under the distal end of an infected nail and scrapings of the surface of the nail plate.
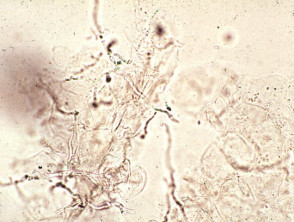
In the mycology laboratory, the material is examined using potassium hydroxide (KOH) to dissolve keratinocytes, then staining the preparation with blue or black ink to identify KOH-resistant mycelium and arthrospores by direct microscopy. Fungal elements are sometimes difficult to find, especially if the tissue is very inflamed, so a negative result does not rule out fungal infection.
Dermatophyte infections
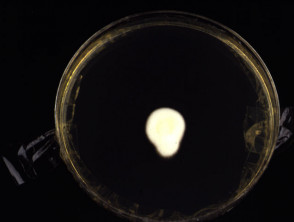
Fungal culture may take several weeks, incubated at 25-30C. The specimen is inoculated into a medium such as Sabouraud's dextrose agar containing cycloheximide and chloramphenicol. A negative culture may arise because:
- The condition is not due to fungal infection.
- The specimen was not collected properly.
- Antifungal treatment had been used prior to collection of the specimen.
- There was a delay before the specimen reached the laboratory.
- The laboratory procedures were incorrect.
- The organism grows very slowly.
Repeat negative scrapings if fungal infection appears likely, preferably prior to treatment. Consider a wide differential diagnosis – there are other reasons for ring-shaped or scaly rashes.
Yeast infections
Yeasts form a subtype of fungus characterised by clusters of round or oval cells. These bud out similar cells from their surface to divide and propagate. The main yeasts causing skin infections are:
- Candida species
- Malassezia species
Yeast infection can be confirmed by swabs and by scrapings.
Activity
Think about the implications of the following results on mycology:
- Positive microscopy and positive culture
- Positive microscopy and negative culture
- Negative microscopy and positive culture
- Negative microscopy and negative culture
Related information
References:
On DermNet NZ:
Information for patients
Other websites:
- Medscape Reference: Fungal infections
- Merck Manual Professional: Fungal skin infections
Books about skin diseases:
See the DermNet NZ bookstore
Sign up to the newsletter
© 2024 DermNet.
DermNet does not provide an online consultation service. If you have any concerns with your skin or its treatment, see a dermatologist for advice.