DermNet provides Google Translate, a free machine translation service. Note that this may not provide an exact translation in all languages
Home Fungal skin infections Pityriasis versicolor CME
Fungal skin infections
Pityriasis versicolor
Created 2009.
Learning objectives
- Identify and manage pityriasis versicolor
Introduction
Although often called tinea versicolor this name is incorrect, as pityriasis versicolor is not due to dermatophyte fungi.
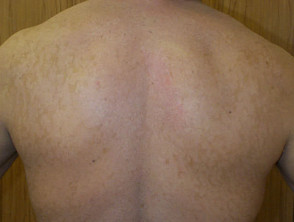
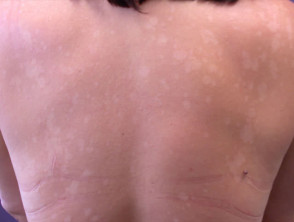
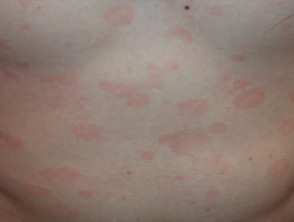
Pityriasis versicolor presents as asymptomatic flaky patches on the trunk, neck, and/or arms, which persist for months or years. It is pink or coppery in pale subjects, but on tanned skin the patches are pale brown, since tanning does not occur in the affected areas. The yeast produces azelaic acid, which diffuses down and impairs the function of the melanocytes.
Pityriasis versicolor is more common in hot, humid climates or in those who sweat heavily, so it may recur each summer.
Pityriasis versicolor
Differential diagnosis
Pityriasis versicolor may be confused with:
- Dry discoid eczema (irritable, generally scattered on trunk and/or limbs)
- Guttate psoriasis (red scaly plaques, look for psoriatic lesions elsewhere)
- Idiopathic guttate hypomelanosis (affects shins and forearms, due to photoageing)
- Pityriasis alba (large patches on face and upper arms)
- Pityriasis rosea (short history and rapid onset)
- Postinflammatory hypo- or hyper-pigmentation (irregular distribution, prior inflammatory episode)
- Seborrhoeic dermatitis (distribution includes scalp and face)
- Tinea corporis (slowly extending annular plaques)
- Vitiligo (completely white or trichrome asymmetrical macules lacking scale)
Investigations
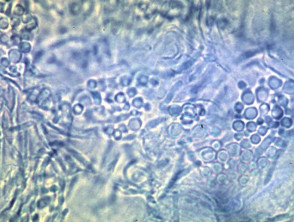
The diagnosis of malassezia infections is generally confirmed by skin scrapings but malassezia may also be identified in apparently normal skin. Microscopy of potassium hydroxide (KOH) preparations from pityriasis versicolor shows clusters of yeast cells and long hyphae. The appearance is said to be like ‘spaghetti and meatballs’.
Malassezia species are difficult to grow in the laboratory so scrapings may be reported as culture negative. The yeast is lipophilic so long-chain fatty acids must be added to the media.
Seven species have been isolated to date – there is some controversy as to whether specific species cause different skin diseases.
- M. furfur
- M. sympodialis
- M. globosa
- M. obtusa
- M. restricta
- M. slooffiae
- M. pachydermatis
- M. ovalis (also known as Pityrosporum ovale)
Pityriasis versicolor fluoresces blue-green on examination using a Wood lamp (long wavelength UVA1).
It is sometimes observed in the stratum corneum of skin biopsies and stains prominently with PAS.
Microscopy of malassezia
Treatment
Available treatments for pityriasis versicolor include topical agents applied for about 2 weeks. Advise the patient that the first aim is to clear up scaling and that it may take some weeks or months for the skin colour to return to normal. Recommend washing affected areas with an anti-dandruff shampoo twice weekly to reduce the chance of relapse. Treatment may be repeated as required.
- Propylene glycol
- Sodium thiosulphate solution
- Selenium sulphide
- Topical/oral azoles including clotrimazole, miconazole, econazole and ketoconazole in various formulations
- Terbinafine gel
- Ciclopirox cream/solution
Patients with extensive or persistent pityriasis versicolor may be prescribed ketoconazole tablets or itraconazole capsules, 200mg daily for 7-10 days and prophylactically once each month. Specialist approval is required for PHARMAC subsidy.
Other conditions due to malassezia
Several other skin conditions are associated with proliferation of malassezia, especially with the predisposing factors of humidity, sweating and seborrhoea. They include:
- Pityrosporum folliculitis (superficial acne-like eruption on upper trunk)
- Pityriasis capitis (dandruff)
- Seborrhoeic dermatitis (non-pruritic scaly red patches on face, scalp and flexures)
- Facial atopic dermatitis, in some cases.
Activity
Find out which species of Malassezia is most likely to be responsible for pityriasis versicolor.
Related information
References:
On DermNet NZ:
Information for patients
Other websites:
- Medscape Reference: Tinea versicolor
- Merck Manual Professional: Tinea versicolor
Books about skin diseases:
See the DermNet NZ bookstore
Sign up to the newsletter
© 2024 DermNet.
DermNet does not provide an online consultation service. If you have any concerns with your skin or its treatment, see a dermatologist for advice.